Chapter 101 Patellofemoral Arthroplasty
Whereas earlier design flaws predisposed to a relatively high rate of failures from patellar maltracking, catching, and anterior knee pain, newer and improved trochlear designs have reduced the incidence of patellofemoral dysfunction.7,24,33,36 These improved outcomes, as well as an interest in single-compartment resurfacing, have led to growing enthusiasm for patellofemoral arthroplasty.
Epidemiology
Chondromalacia patella has been observed in 40% to 60% of patients at autopsy, and in 20% to 50% of patients at the time of arthrotomy for other diagnoses.54 The prevalence of isolated patellofemoral arthritis is high, occurring in as many as 11% of men and 24% of women older than 55 years with symptomatic osteoarthritis of the knee in one study.42 This gender predilection is undoubtedly related to the often subtle patellar malalignment and dysplasia that is common in women. The patellofemoral cartilage is also vulnerable to direct traumatic injury, considering its unprotected location in the body.
Nonsurgical Treatment
Nonsurgical management is the mainstay of treatment for isolated patellofemoral arthritis; to be certain, it is the minority of patients who ultimately require an operation. A directed therapy program emphasizing short arc quadriceps strengthening, stretching of the lateral retinacular structures, and preservation of motion is frequently successful in mitigating symptoms. There is some evidence to suggest that vastus medialis obliquus dysfunction may be associated with patellofemoral pain.55 This serves to reinforce the importance of a directed strengthening program. When the anterior knee pain associated with patellofemoral arthrosis is refractory to months of nonoperative interventions, such as weight reduction, physical therapy, and judicious use of injectable or oral medications, surgery may be considered.
Surgical Alternatives
Arthroscopic Surgery
Federico and Reider16 have analyzed a series of 36 patients who underwent arthroscopic chondroplasty for isolated chondromalacia patella without patellar malalignment. Those patients with traumatic chondromalacia had 60% good or excellent results compared with 41% good or excellent results in all others. Lateral retinacular release, after chondral degeneration has already occurred, is often ineffective in resolving anterior knee pain.46 Schonholtz and Ling50 performed chondroplasty for varying degrees of chondromalacia of the patella to remove loose fibrillation, but not to penetrate through subchondral bone or to débride intact cartilage. At a mean 40-month follow-up, the authors reported good to excellent results in 49% of patients and fair results in 44%. They noted that 78% of patients were satisfied and that the grade of chondromalacia did not correlate with the outcome. Marrow stimulation techniques, such as microfracture, have also fared relatively poorly in treating lesions of the patellofemoral articulation. The reparative fibrocartilage tissue, composed primarily of type I collagen, is incapable of withstanding the excessive shear stresses common to the patellofemoral articulation.
Tibial Tubercle Unloading Procedures
Anteromedialization of the tibial tubercle is a time-tested and well-established procedure for the treatment of patellar maltracking associated with patellofemoral malalignment.18,20 Although anteriorization of the tibial tubercle reduces the patellofemoral joint reaction forces by increasing the angle between the patellar tendon and quadriceps tendon and increases the lever arm for extensor mechanism function, medializing the tibial tubercle improves the Q angle and thereby decreases the strong lateral vectors acting on the patella. Combining these two components can therefore improve patellar tracking and relieve pain associated with subchondral overload of the lateral patellar facet. The obliquity of the tibial tubercle osteotomy allows for adjustment in the extent of anteriorization, and bone graft is not necessary. The angle can be adjusted to accommodate varying degrees of subluxation and articular cartilage damage. Although Fulkerson and colleagues19 have reported excellent to good results in 89% of patients followed up for more than 5 years, no patients achieved excellent results and satisfaction was only 75% in the presence of substantial chondromalacia (Outerbridge grade III or IV).
Direct anteriorization of the tibial tubercle has also been advocated for patients with patellofemoral arthrosis when there is no patellar subluxation or malalignment. Symptom improvement with the classic Maquet osteotomy has ranged from 30% to 90%.17,23,41 Biomechanical studies have demonstrated reductions in contact pressures; however, contact areas may shift proximally, paradoxically overloading the proximal portion of the patella in deep flexion.11 The optimal patient to benefit from a Maquet osteotomy is one with post-traumatic arthrosis or chondromalacia involving the inferior half of the patella. Those patients with proximal arthrosis or diffuse patellofemoral arthrosis, and those with multiple prior patellofemoral surgeries, will have compromised outcomes. Its limited indications, unpredictable results, and risk of complications, such as wound necrosis or osteotomy nonunion, restrict the practical application of this procedure.
Cartilage Grafting
Autologous chondrocyte implantation for isolated patellar cartilage lesions has produced satisfactory results in approximately 75% of patients at 2- to 10-year follow-up.10,44 Proponents advise that residual patellar malalignment is a common reason for failure of this technique and should therefore be addressed prior to or simultaneously with autologous chondrocyte implantation. Autologous osteochondral transplantation has been advocated by its innovator for patellofemoral lesions. Although the duration of follow-up is not clear, Hangody and Fules21 have reported 79% satisfactory results in those with patellar and/or trochlear mosaicplasties.
Patellectomy
Patellectomy has been shown experimentally to reduce extension power by 25% to 60%, with a concomitant requisite increase in quadriceps force of 15% to 30% to achieve adequate extension torque.8,26 Tibiofemoral joint reaction forces may increase by as much as 250%, explaining the propensity for tibiofemoral arthrosis after patellectomy.15,25 Variable pain relief, residual quadriceps weakness, and secondary instability, with failures as high as 45%, relegate this to being a salvage procedure for the rare patient who does poorly with other more successful interventions. Additionally, results of total knee arthroplasty can be compromised after patellectomy.47 Therefore, patellectomy is less desirable than patellofemoral arthroplasty or total knee arthroplasty for the treatment of isolated patellofemoral arthrosis.
Total Knee Arthroplasty
Total knee arthroplasty is generally effective for older patients with isolated patellofemoral arthritis, yielding good and excellent results in 90% to 95% of patients at midterm follow up, although anterior knee pain has been reported in as many as 7% to 19% of patients.29,45,48 In one study comparing total knee arthroplasty for isolated patellofemoral arthrosis to that for tricompartmental arthrosis, Knee Society scores, bipedal stair climbing capacity, and ability to rise from a seated position were all significantly better in the former group.29 Given the predictably good results of total knee arthroplasty, it is preferable to patellofemoral arthroplasty in the older patient with isolated patellofemoral arthrosis. However, in younger patients with isolated patellofemoral arthrosis, patellofemoral arthroplasty may be favorable.
Patellofemoral Arthroplasty
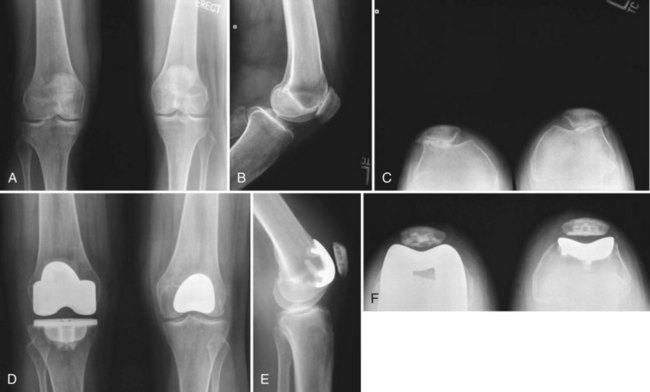
Patellofemoral arthroplasty (PFA) may be considered in the treatment algorithm for patients with localized patellofemoral arthrosis or severe recalcitrant chondromalacia (Fig. 101-1). Early designs resurfaced only the patella, using a metal implant and leaving the trochlea untouched. Although the patella is commonly more degenerated than the trochlea, results have been variable with this technique.2,40 Recognition that residual anterior knee pain may have been related to trochlear chondromalacia, first-generation patellofemoral resurfacing arthroplasties were developed, using a polyethylene patellar component and metallic trochlear component.9
Patient Selection
The outcome of patellofemoral arthroplasty can be optimized by limiting its application to patients with isolated patellofemoral osteoarthrosis, post-traumatic arthrosis, or severe chondrosis (Outerbridge grade IV), and then only after an extended supervised program of nonoperative measures. Additionally, this option is best reserved for patients with isolated retropatellar and/or peripatellar pain and functional limitations, with considerable discomfort with provocative activities such as stair or hill ambulation, squatting, or prolonged sitting. The procedure should not be performed in patients with inflammatory arthritis or chondrocalcinosis involving the menisci or tibiofemoral chondral surfaces, nor should it be offered to patients with inappropriate expectations.30,32,34,35 The presence of medial or lateral joint line pain suggests more diffuse chondral disease and should be considered as potential contraindications to isolated patellofemoral resurfacing. Alternative causes of anterior knee pain, such as patellar tendinitis, synovitis, patellar instability, sympathetic mediated pain, and pain referred from the back or ipsilateral hip, should be excluded, unless it appears that the pain is referred from the patellofermoral compartment.
Although it can be most effective for treating arthritis associated with patellofemoral dysplasia,22 patellofemoral arthroplasty should be avoided in patients with considerable patellar maltracking or malalignment, unless they are corrected. This is not to say, however, that moderate patellar tilt, observed on preoperative tangential radiographs or at the time of arthrotomy, should be considered contraindications for this procedure. In such cases, a lateral retinacular recession or release may be necessary at the time of arthroplasty.32,34,38 Occasionally, for severe maltracking, a proximal realignment may be necessary. Persistent patellar subluxation may cause pain and snapping and potential polyethylene wear of the prosthesis. Patients with excessive Q angles should undergo tibial tubercle realignment before or during patellofemoral arthroplasty, although some trochlear prosthesis shapes may accommodate a slightly increased Q angle. Also, the presence of tibiofemoral arthrosis should discourage isolated patellofemoral arthroplasty. The presence of even focal grade III tibiofemoral chondromalacia can compromise the outcome after patellofemoral arthroplasty, although these patients will often acknowledge resolution of the most prominent component of pain. Combining patellofemoral arthroplasty with medial or lateral unicompartmental knee arthroplasty or autologous osteochondral grafting are sound considerations in these situations.5,38
Clinical Evaluation
Generally, weight-bearing radiographs are ample imaging studies. Standing anteroposterior and midflexion posteroanterior radiographs are critical to determine the presence of tibiofemoral arthritis. Mild squaring-off of the femoral condyles and even small marginal osteophytes may be accepted, provided that the patient is devoid of tibiofemoral pain with functional activities and on physical examination, and that there is minimal chondral degeneration during arthroscopy or arthrotomy. Lateral x-rays will occasionally demonstrate patellofemoral osteophytes, but usually are more useful in identifying whether there is patella alta or baja. Axial radiographs will demonstrate the position of the patella within the trochlear groove and the extent of arthritis, although on occasion there will be relative radiographic patellofemoral joint space preservation with minimal or no osteophytes, despite significant cartilage loss (see Fig. 101-1). Newer MRI sequences may be useful for evaluating patellofemoral arthrosis but, more importantly, can be used to evaluate the medial and lateral compartments for evidence of chondral wear. If committed to performing a PFA, patients should consent to autologous osteochondral grafting for associated focal condylar defects or unicompartmental knee arthroplasty as part of a bicompartmental resurfacing if there is more diffuse degeneration.6,38 Photographs from prior arthroscopic treatment will provide valuable information regarding the extent of anterior compartment arthrosis and status of the tibiofemoral articular cartilage and menisci.
Surgical Technique
The trochlear component should be externally rotated perpendicular to the anteroposterior axis of the femur (Whiteside axis) or parallel to the epicondylar axis to enhance patellar tracking.33,34 Osteophytes bordering the intercondylar notch should be removed. The trochlear component should maximize coverage of the trochlea, without extending beyond the medial-lateral femoral margins anteriorly, encroaching on the weight-bearing surfaces of the tibiofemoral articulations, or overhanging into the intercondylar notch. The medial and lateral transitional edges of the prosthesis should be flush with or recessed approximately 1 mm from the adjacent condylar articular cartilage. The proximal edge should be flush with the anterior femoral cortex and the distal tip should be flush with the articular cartilage and not extend into the intercondylar notch. The patella is resurfaced by the same principles observed in total knee arthroplasty, restoring the original patellar thickness and medializing the component. The exposed cut surface of the lateral patella that is not covered by the patellar prosthesis is removed or beveled to avoid the potentially painful articulation on the trochlear prosthesis.31 This may also enhance patellar tracking by releasing tension on the lateral retinaculum.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree