Pantalar Arthrodesis
Travis A. Motley
Brian B. Carpenter
Historically, pantalar arthrodesis has been used to describe arthrodesis of the ankle and subtalar joint (now termed tibiotalocalcaneal arthrodesis). In modern literature and for the purpose of this chapter, pantalar arthrodesis includes fusion of the ankle, subtalar, talonavicular, and calcaneocuboid joints.
At the time of the description of pantalar arthrodesis, the overwhelming majority of patients were due to complications of polio, and the goal was to provide patients the ability to ambulate with minimal or no bracing. Most current literature focuses on pantalar arthrodesis for posttraumatic arthritis and other joint destructive diseases such as rheumatoid arthritis and Charcot neuroarthropathy. Pantalar arthrodesis is considered a limb salvage procedure in patients with severe deformity and/or intractable pain and is an alternative to below-the-knee amputation in certain cases.
EVALUATION, DIAGNOSIS, AND FUNCTIONAL ANATOMY
Careful attention to the preoperative evaluation is critical to postoperative success. Nutritional status, metabolic disorders, neurovascular status, nutritional status, and history of wounds, infections, or osteomyelitis are established and addressed by the medical team. Bone quality from disuse, extended bracing, metabolic disorders, and previous trauma must also be considered. Once the ankle, subtalar, talonavicular, and calcaneocuboid joints no longer provide any motion, preexisting deformities will be accentuated. The considerations for pantalar arthrodesis must start proximally, and consideration must be given to limb-length discrepancy, ipsilateral knee alignment, or history of proximal ipsilateral lower extremity pain. Previous studies have shown that pantalar arthrodesis can result in ipsilateral knee degeneration and pain (1).
Plain films that demonstrate varus, valgus, and equinus deformity of the ankle must be examined so that appropriately based wedges can be planned. Deformities of the calcaneus must be considered so that minimal adjustments to shoe gear will be necessary postoperatively. Midfoot equinus or forefoot varus/valgus must be evaluated so that the best arthrodesis procedure is not thwarted long-term by painful callosities. Soft tissue contractures including equinus, posterior ankle capsule, plantar soft tissues, peroneal tendons, and long flexor tendons must be incorporated into the surgical plan to assist in reduction of rearfoot and ankle deformities and prevent abnormal influences on the forefoot and knee after fusion.
Isolated diagnostic injections with local anesthetic agents will provide the surgeon invaluable data regarding pain relief and which specific joints are involved. It is critical to spare any joint from arthrodesis if it does not generate pain unless that joint shows degenerative changes that will be multiplied by arthrodesis of an adjacent joint. Computed tomography can also aid the surgeon in determining the extent of arthrosis in joints that are to undergo fusion as well as adjacent joints, while magnetic resonance imaging may be helpful in identifying avascular changes (2). For neuropathic patients, better indicators are joint instability and primary areas of deformity. In these patients, arthrodesis can remove the deformity but will produce a rigid rearfoot and ankle that may not accommodate a typical neuropathic gait that a previously supple Charcot deformity may have allowed.
SURGICAL CRITERIA, SELECTION OF PROCEDURE, AND CONTRAINDICATIONS
Prior to consideration for surgery, conservative treatment modalities are attempted to relieve pain and/or allow the patient a better quality of life. This includes nonsteroidal antiinflammatory drugs, physical therapy, and bracing. Shoe gear accommodations such as a rocker sole also have a role in conservative treatment.
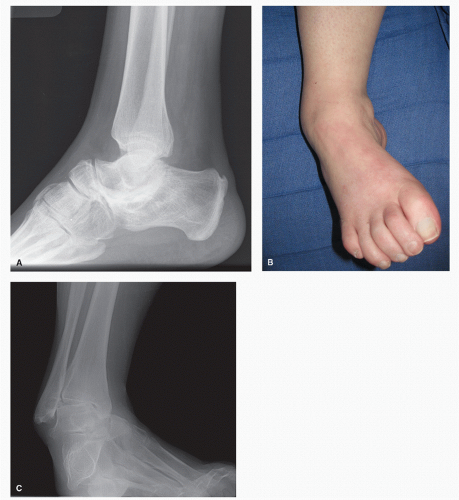
The indications for pantalar arthrodesis include severe pain, instability, and deformity (2). This can include posttraumatic arthritis, posttraumatic malalignment, and neuromuscular or congenital deformities (Fig. 61.1). Patients need to understand that extended arthrodesis procedures are an alternative to extensive bracing or limb amputation. Some authors require patients to spend time in a rigid ankle-foot orthosis or below-knee cast to provide an example of anticipated mobility after pantalar arthrodesis. Consideration must be given if there has been a prior arthrodesis or arthroplasty performed on the contralateral limb before proceeding with a pantalar arthrodesis.
TECHNIQUE
Multiple techniques have been described for pantalar arthrodesis. For all techniques, the fundamental concepts are of removing articular cartilage, exposing bleeding cancellous bone, plantigrade position, and stable fixation. This technique has evolved as first described by Lorthioir (3) in 1911 for equinovarus foot in which the talus was excised, denuded of cartilage, and utilized as a bone graft. Lorthioir’s procedure included fusion of the tibiotalar, subtalar, and tibionavicular joints. Liebolt (4) and Patterson (5) reported on a staged procedure, triple first then ankle a few weeks later, to decrease complications. Hunt and Thompson (6) preferred a single-stage procedure but still extirpated the talus. Hamsa (7) also recommended a single-stage procedure. Steindler (8) and Waugh et al (9) also recommended a single-stage procedure but did not extirpate the talus to decrease the risk of avascular necrosis.
Recent literature fails to demonstrate a difference in arthrodesis rates between one- and two-stage procedure although available techniques and implants direct the surgeon to a single-stage procedure (2,10).
Recent literature fails to demonstrate a difference in arthrodesis rates between one- and two-stage procedure although available techniques and implants direct the surgeon to a single-stage procedure (2,10).
Multiple approaches have been described that provide access to the involved joints. Beginning 4 to 5 cm above the ankle joint, an incision from the lateral border of the fibula to the tip of the fibula then extending distally across the sinus tarsi to the fourth metatarsal base provides excellent exposure after osteotomy of the fibula above the ankle joint. This lateral incision can also be divided into two incisions: the proximal one for exposure to the ankle joint and the distal one for exposure to the subtalar joint and calcaneocuboid joint (Fig. 61.2). The fibula is obliquely osteotomized from anterior-inferior to posterior-superior (creating a posterior spike). After division of the anterior talofibular ligament and calcaneofibular ligament, the fibula is then reflected posteriorly, and direct visualization and access to the joint are possible. The extensor digitorum brevis muscle is elevated from the dorsum of the anterior process of the calcaneus and reflected superiorly to allow access and visualization of the subtalar joint and calcaneocuboid joint.
An anteromedial ankle incision is also utilized and extended dorsally over the navicular to allow access to the medial ankle
joint and the talonavicular joint (Fig. 61.3). These incisions allow a wide skin bridge and easily accept standard operative tools for appropriate joint preparations. If minimal alignment correction is needed, incisions may be smaller. However, it is more likely based on this procedure that there are significant deformities present that will require corrective arthrodesis planes. When substantial deformities are present, closing wedges are preferred to distraction arthrodesis procedures if possible to prevent skin tension at the time of wound closure.
joint and the talonavicular joint (Fig. 61.3). These incisions allow a wide skin bridge and easily accept standard operative tools for appropriate joint preparations. If minimal alignment correction is needed, incisions may be smaller. However, it is more likely based on this procedure that there are significant deformities present that will require corrective arthrodesis planes. When substantial deformities are present, closing wedges are preferred to distraction arthrodesis procedures if possible to prevent skin tension at the time of wound closure.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree