Chapter 39 Operative Options for Extensor Mechanism Malalignment and Patellar Dislocation
INDICATIONS
Many surgical procedures have been described for realignment of the patellofemoral mechanism including proximal realignment procedures, distal realignment procedures, or a combination of both. Proximal realignment procedures alter the medial-lateral position of the patella through balancing of soft tissue restraints proximal to its inferior pole. Included in this category are lateral retinacular release, medial retinacular capsular and medial patellomeniscal ligament (MPML) plication, vastus medialis obliquus (VMO) advancement, and medial patellofemoral ligament (MPFL) repair or reconstruction. Distal realignment procedures modify the medial-lateral, anterior-posterior, and proximal-distal positions of the patella by transfer of the tibial tubercle. Included in this category are anterior (Maquet55), medial (Elmslie-Trillat93), and anteromedial (Fulkerson33) transfer of the tibial tubercle. Literally hundreds of articles have been written on these operative procedures regarding their indications, technique, and clinical outcome and the reader is referred to recent review articles for further information.2–4,27,31,32,36,61
 Modification of Elmslie-Trillat procedure: arthroscopic lateral release if a contracted lateral retinaculum is present, a modified VMO advancement, and a modified medial transfer of the tibial tubercle.
Modification of Elmslie-Trillat procedure: arthroscopic lateral release if a contracted lateral retinaculum is present, a modified VMO advancement, and a modified medial transfer of the tibial tubercle. MPFL reconstruction using the quadriceps tendon based on the proximal patella, combined with a distal realignment procedure when indicated.
MPFL reconstruction using the quadriceps tendon based on the proximal patella, combined with a distal realignment procedure when indicated. Diffuse anterior knee pain without distinct anatomic abnormalities in alignment, subluxation, or joint damage: treated conservatively.
Diffuse anterior knee pain without distinct anatomic abnormalities in alignment, subluxation, or joint damage: treated conservatively. Anatomic abnormalities, congenital laxity MPFL, increased Q-angle, trochlear dysplasia: treated conservatively, candidates for surgery if symptomatic.
Anatomic abnormalities, congenital laxity MPFL, increased Q-angle, trochlear dysplasia: treated conservatively, candidates for surgery if symptomatic. ± underlying anatomic abnormalities, major joint hemarthrosis, MRI evidence of patellar or femoral osteochondral fracture: surgery, fixation fracture, MPFL repair.
± underlying anatomic abnormalities, major joint hemarthrosis, MRI evidence of patellar or femoral osteochondral fracture: surgery, fixation fracture, MPFL repair.The second operative procedure described in detail is an MPFL reconstruction using the quadriceps tendon (QT) based on the proximal patella. This procedure is performed through a limited cosmetic incision and avoids harvesting the semitendinosus tendon or bony fixation at the patella or medial femur. This procedure has proved to be useful in revision cases that failed after a prior proximal realignment in which an inadequate MPFL was not addressed. The operative procedure is combined with a distal realignment when indicated, as is discussed. Other operative procedures the senior author has found useful for correcting patella alta and ITB lengthening are also described. Surgical procedures for rotational malalignment of excessive femoral anteversion and external tibial torsion are discussed in Chapter 40, Patellofemoral Disorders: Correction of Rotational Malalignment of the Lower Extremity, and not repeated here.
The majority of patients with patellofemoral malalignment respond favorably to conservative treatment programs, covered in detail in other publications.17,18,96 In general, three types of extensor mechanism problems present for treatment. The first group of patients have diffuse anterior knee pain without distinct anatomic abnormalities in alignment, subluxation, or joint damage that can be identified. Commonly, these are younger athletes who are involved in multiple sports, and frequently, the only finding is the presence of tenderness of peripatellar soft tissues and the anterior fat pad tissues. On occasion, a mild joint effusion may be present. Authors have stressed that these symptoms frequently represent an overuse condition from excessive participation in athletics.45,91 Treatment consists of allowing the soft tissues time to heal and inflammation to recede by modification of athletics, followed by appropriate strengthening and stretching of the muscle groups. Specific factors that may contribute to the symptomatic state include excessive conditioning, type of sport, and duration and frequency of athletic participation. Recurrence of symptoms is not an indication for surgical treatment, because distinct anatomic abnormalities of the extensor mechanism are not present. A cartilage-sensitive magnetic resonance imaging (MRI) may be helpful in recurrent symptomatic knees to determine the status of the patellofemoral joint and the presence of early articular cartilage damage that is aggravated by vigorous athletic activities.
Nonoperative treatment of first-time patella dislocations has a re-dislocation rate that ranges from 14% to 57% in adult populations15,30,40,50,52,53,92 and from 36% to 71% in pediatric populations.12,72 Stefancin and Parker87 conducted a systematic review of 70 articles that focused on the management of traumatic first-time patellar dislocations and concluded that conservative treatment was indicated initially except in specific circumstances. These included the finding of an osteochondral fracture, a substantial disruption of the MPFL, a laterally subluxated patella with normal alignment of the contralateral knee, or after failed conservative treatment or recurrent dislocations.
Patients with an acute lateral first-time dislocation are separated into three categories:
CONTRAINDICATIONS
The primary contraindication for extensor mechanism malalignment surgery is the absence of a distinct anatomic defect, because the goal of surgery is to restore normal anatomy of the extensor mechanism. The presence of chronic recurrent anterior knee pain is not an indication for surgery when the specific etiology of the pain symptoms cannot be determined. This point is worthy of emphasis, because many patients present with anterior knee pain in which the specific diagnosis is not apparent despite a thorough and careful examination and evaluation. It is probable that there are pain generation factors related to early patellofemoral cartilage deterioration that is still early in the disease course. Alternatively, peripatellar and intra-articular soft tissues may be an explainable source of pain.24,32 A common cause of unexplained pain is a subtle infrapatellar neuroma or neuritis of the sensory nerves about the knee joint, discussed in Chapters 42, Knee Pain of Neural Origin, and 43, Diagnosis and Treatment of Complex Regional Pain Syndrome.
Critical Points CONTRAINDICATIONS
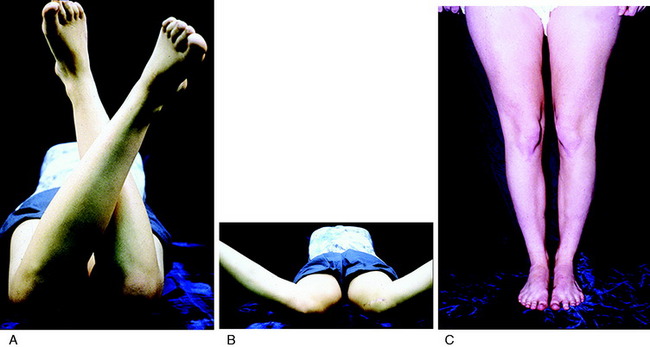
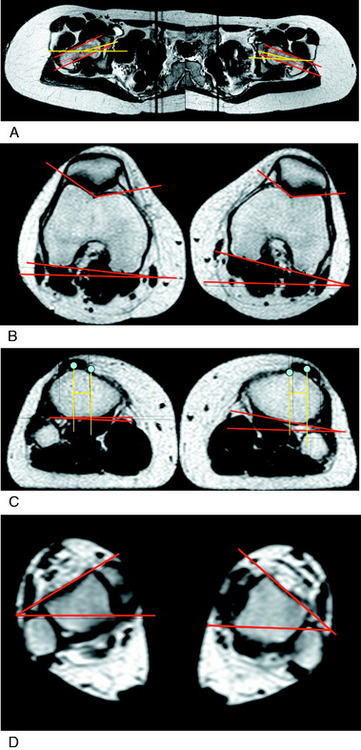
A specific contraindication to extensor mechanism surgery is the presence of excessive hip anteversion or abnormal external tibial torsion as discussed in Chapter 40, Patellofemoral Disorders: Correction of Rotational Malalignment of the Lower Extremity. An MRI or computed tomography (CT) scan for axial rotation of the lower extremity from the hip to the ankle is required. The measurements obtained include femoral anteversion, trochlear groove–tibial tubercle offset, and external tibial torsion as are described. The anterior knee pain is due to excessive lateral patellofemoral forces induced by external tibial torsion or increased femoral anteversion (Fig. 39-1). In these patients, a femoral or tibial derotation osteotomy may be indicated and not a proximal or distal patellofemoral procedure.58,89
A relative contraindication is the presence of patellofemoral arthritis; however, in select knees, a realignment procedure may be performed with a cartilage restoration procedure.9,10,38,43,54,64,74,76
BIOMECHANICS OF MEDIAL AND LATERAL PATELLOFEMORAL RESTRAINTS
Three factors influence patellar stability: articular geometry, dynamic muscle actions, and passive soft tissue restraints.2,27 The geometry of the trochlear groove,2 the height and slope of the lateral femoral condyle, and the angle of knee flexion all affect lateral patellar translation. Amis2 described objective patellar stability in terms of two factors: the amount of force required to displace the patella a given linear distance from its equilibrium position (translation) and the turning moment required to induce a rotation, such as a lateral tilt. Methods used to determine patellar mobility include manual measurement, instrumented quantitative measurement, and radiographic measurement. Kolowich and coworkers47 measured patellar glide by dividing the patella into four quadrants and describing medial and lateral mobility as a fraction of patellar width. Normal subjects had less than two quadrants of translation with the knee flexed 30°. Teitge and associates90 developed a stress radiographic method to measure patellar medial-lateral stability. Knees of normal subjects and symptomatic patients were tested between 30° and 40° of flexion with 71 N of force applied. Wide variation was noted in the normal knees, because lateral displacement ranged from 1 to 32 mm, and medial displacement ranged from 2 to 22 mm. The mean difference in lateral displacement between right and left knees was 1.3 ± 1.1 mm, and the mean difference in medial displacement was 1.2 ± 1.08 mm. The investigators determined that a difference between knees in lateral displacement of 3.7 mm, or a difference in medial displacement of 3.46 mm, was abnormal.
Critical Points BIOMECHANICS OF MEDIAL AND LATERAL PATELLOFEMORAL RESTRAINTS
Hautamaa and colleagues39 developed an instrumented measurement device to determine patella medial-lateral translation in the coronal plane. In 17 cadaver knees, with the knee flexed 30 ± 5°, 5 pounds of laterally directed force produced an average of 9.3 ± 0.9 mm of lateral translation. Instrumented measurement of medial-lateral patellar translation was also conducted by Fithian and coworkers29 in normal and symptomatic patients. Right versus left knee comparisons revealed small mean differences in the control subjects for medial and lateral patellar translation (30° flexion, 2.5-lb force, 0.1 ± 1.9 mm and 0.2 ± 1.0 mm, respectively). Significant differences were found between the control and the symptomatic subjects in the mean differences in lateral translation (P < .01), with the patients demonstrating 1.6 ± 2.5 mm difference under a 2.5-pound force at 30° of flexion.
It is well appreciated that the patella is most unstable in the range of 0° to 30° of flexion. When the knee is near full extension, the Q-angle is maximized owing to the external rotation of the tibia. In addition, with the quadriceps muscle relaxed, the patella is not engaged in the trochlear groove and thus is easily mobilized in a medial-lateral direction. As the knee is flexed, patellar stability is increased owing to the combined tensions of the quadriceps muscles and the patellar tendon that pull the patella into the trochlear groove. A shallow or dysplastic trochlear groove allows the patella to displace more easily.81 A patella alta condition results in a loss of the trochlea geometric restraint until 30° to 40° of flexion when patellotrochlear contact finally occurs.
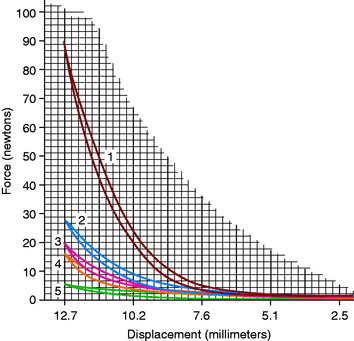
In regard to passive soft tissue restraints, the MPFL is the primary restraint to lateral patellar translation, providing 53% to 67% restraint up to 30° of flexion.4,11,16,23,39,73 Desio and associates23 examined nine cadaver knees (mean age, 57 yr; range, 43–70 yr) at 20° of flexion and reported that the MPFL provided a mean of 60% of the restraining force to lateral patellar translation. The MPML provided a mean of 13% of the restraining force; the lateral retinaculum, 10%, and the medial retinaculum and medial patellotibial ligament, 3% each. Conlan and colleagues16 reported similar findings from 25 cadaver specimens (Fig. 39-2); the MPFL provided an average of 53% of the total restraining force, followed by the MPML (22% contribution), the medial retinaculum (11% contribution), and the medial patellotibial ligament (5% contribution). Sectioning of the MPFL decreased the restraining force significantly; the average stiffness decreased from 225 N/cm in the intact specimens to 104.6 N/cm (P = .001).
Nomura and coworkers68 measured the lateral patellar translation in 10 cadaver knees (aged 45–60 yr) with the quadriceps tensed to 10 N and a lateral force of 10 N applied before and after sectioning of the MPFL. Isolated sectioning of the MPFL significantly increased the lateral patellar translation from 20° to 90° of flexion (P < .05).
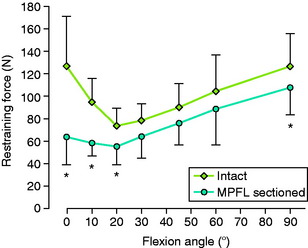
Amis and associates3 reported a mean failure load of the MPFL of 208 N from 10 cadaveric specimens (mean age, 70 yr) and interpreted these findings as “surprisingly strong for such an insubstantial appearance.” These investigators also reported that the contribution of the MPFL in restraining lateral patellar translation was greatest with the knee at 0° extension. Significant increases in lateral translation occurred from 0° to 20° after the MPFL was sectioned (P value not provided; Fig. 39-3).
PREOPERATIVE PLANNING
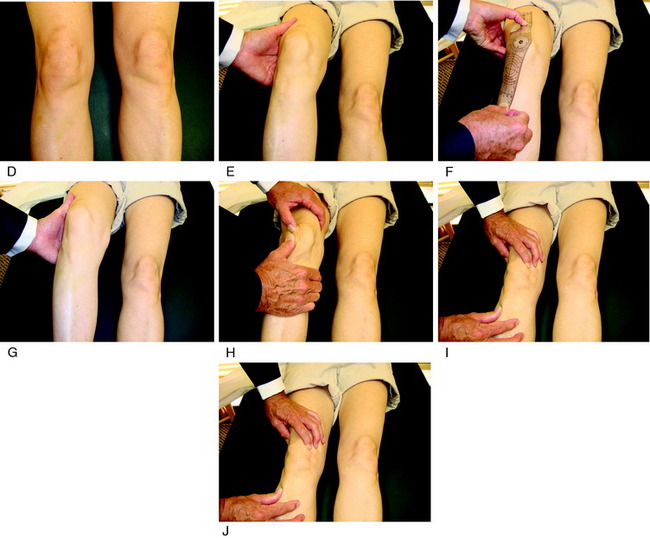
The physical examination is crucial in preoperative planning for patellar realignment surgery. The examination should be performed with the patient in the standing, sitting, and supine positions (see Fig. 39-1D-J). Palpation of parapatellar soft tissues and the fat pad is performed for swelling and elicitation of pain. The examiner should look for evidence of lateralization of the extensor mechanism and tilt. The patellar compression test should be performed with flexion and extension of the knee to evaluate for articular crepitus or pain. Passive patellar tilt and tightness of the lateral retinaculum should be noted. Patellar subluxation tests (patellar glide at 0° and 30° flexion) should be performed in medial and lateral directions, and patellar mobility noted. Other sources of pain such as neuroma, patellar tendinitis, synovial plica, synovitis, meniscus tears, osteochondritis dissecans, complex regional pain syndrome, and advanced tibiofemoral arthritis should be excluded.
Critical Points PREOPERATIVE PLANNING
CT, computed tomography; MRI, magnetic resonance imaging; TT/TG, tibial tubercle/trochlear groove.
CT and MRI have been used to assess lower limb rotational alignment and are important tests for a complete diagnosis of the anatomic abnormalities that may be present. These studies obtain axial images of the patellofemoral joint at or near full extension to evaluate trochlear dysplasia and the tibial tubercle/trochlear groove (TT/TG) distance. Various investigators have studied this distance and found that it is increased in patients with patellofemoral pain and instability.21,46,82
Femoral anteversion has been measured by a variety of techniques by many authors. Yoshioka and Cooke97 measured anteversion from the bone in 32 femora and reported a mean of 13.1° ± 8° (range, –11°–+22°) in both males and females when the distal measurement was the tangent across the femoral condyles, and a mean of 7.4° when measured across the epicondyles. These authors conducted a review of the literature on this measurement and found reported normal values were between 8° and 16° in twelve different investigations. Teitge and associates90 arbitrarily selected 13° as the goal for correction (see Chapter 40, Patellofemoral Disorders: Correction of Rotational Malalignment of the Lower Extremity).
The technique for measuring tibial torsion by CT has not been standardized and wide variation exists in the literature regarding normal values. Yoshioka and colleagues98 reported a mean lateral tibial torsion of 21° ± 4.9° in males and 27° ± 11.0° in females, a significant difference (P < .05). Eckhoff and coworkers25 reported mean tibial “version” of 37.0° ± 1.7° in control knees and 32.8° ± 1.7° in a group of symptomatic knees. Turner94 measured a mean of 19° ± 4.8° in a control group compared with a mean of 24.5° ± 6.3° in a group with unstable patella. Sayli and associates79 reported an average of tibial torsion in females of 31.07° for the right side and 30.02° for the left. For males, the averages were 32.7° and 35.26° for the right and left sides, respectively. Tamari and colleagues88 conducted a reliability study that examined different methods of measuring tibial torsion. The results showed that clinical methods currently available do not accurately measure true torsion of the femur and tibia. The authors stressed that even so, these methods may be useful for screening and descriptive purposes as indices of true torsion and use of different reference axes could improve their reliability.
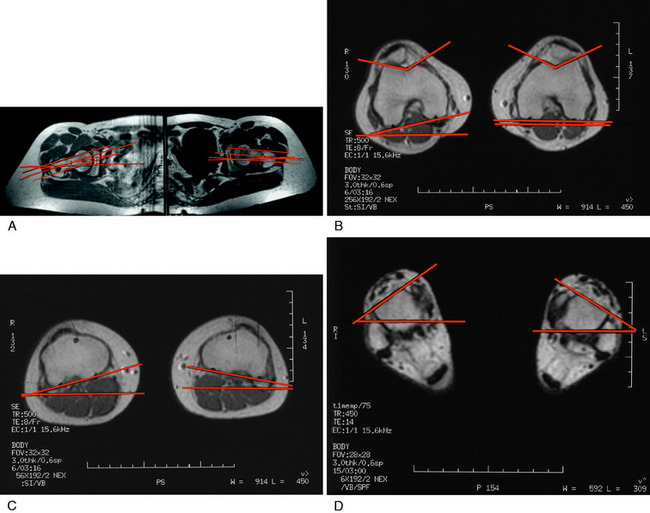
MRI has some advantages over CT, including improved ability to image cartilaginous structures, better anatomic approximation of the trochlear articular cartilage groove, and avoidance of radiation exposure. MRI also provides meaningful information about all of the soft tissue structures about the knee joint. The MRI is obtained in standard fashion, with images obtained of the hip parallel to the femoral neck and axial images obtained of the knee and ankle (Fig. 39-4). These individual images are then measured based on the techniques described by Murphy and coworkers65 and Guenther and associates37 (Figs. 39-5 and 39-6).
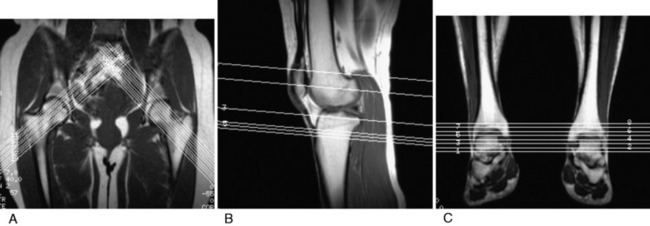
FIGURE 39-5 MRI T1 images are obtained at the hip (A), knee (B), and ankle (C). This allows selection of the proper images for the measurements shown in Figure 39-6.
(A–C, From Parikh, S. N.; Noyes, F. R.; Albright, J.: Proximal and distal extensor mechanism realignment: the surgical technique. Tech Knee Surg 5:27–38, 2006.)
TT/TG is measured using the trochlear groove–patellar tendon insertion distance. TT/TG is measured in millimeters and is the difference from the center of the deepest point of the femoral groove to the center of the patellar tendon attachment to the tibial tubercle. This is done by superimposing the line perpendicular to these points and measuring the distance between the two lines, adjusting for magnification. Dejour and Walch22 reported a mean TT/TG distance of 12.7 ± 3.4 mm in a group of asymptomatic knees. In a group of knees with patellar instability, the mean TT/TG distance significantly increased to 19.8 ± 1.6 mm (P < .001). The authors concluded that the pathologic threshold is 20 mm, which has been agreed upon by others.89 In some knees with trochlear dysplasia, it is difficult to determine the true center point for the measurement, rendering the TT/TG offset to be inaccurate. In these knees, this measurement cannot be used as an evaluation measurement of the desired operative correction.
SURGICAL TECHNIQUES
The patient is positioned supine on the operating table. Under anesthesia, the peripatellar retinaculum, patellofemoral crepitation, patellar tilt, passive medial-lateral patellar glide (0°, 30° flexion), and Q-angle are assessed and compared with preoperative measurements. A sterile thigh tourniquet is applied as proximal as possible, so that an intraoperative assessment of the Q-angle can be made. Routine diagnostic arthroscopy is performed, and any intra-articular pathology is evaluated and treated. Particular attention is paid to patellar position, mobility, tracking, and articular surface. Approximately one fourth of the patella should establish trochlear contact at 0° to 5° of knee flexion. The medial and lateral translation of the patella is assessed at 0° and 30° of knee flexion (Fig. 39-7). This is an important test, because a lateral translation of the patella greater than 50% of its width indicates incompetency of the MPFL. The medial translation of the patella tests for lateral retinacular tightness, and a normal lateral translation of 10 to 12 mm should be obtained with the knee at 30° of flexion. The patella and femoral groove are assessed for articular cartilage pathology or dysplasia. Articular cartilage lesions are evaluated for nature, location, and depth. The finding of loose flaps of articular cartilage requires a careful débridement; otherwise, fibrillated cartilage is left alone because it is possible to produce further damage by the débridement procedure. Radiofrequency cartilage débridement devices are never used, because excessive cartilage damage may occur. Most important at the time of arthroscopy is the critical assessment of whether the realignment procedure will transfer the loading from soft or fragmented articular surface to an intact or less involved cartilage surface. The articular cartilage is graded by the classification system described in Chapter 47, Articular Cartilage Rating Systems.70
Lateral Retinacular Release
Critical Points SURGICAL TECHNIQUE
 Performed only if patellar medial subluxation test is abnormal (patellar medial subluxation ≤ 5 mm on the manual medial translation test, knee at 30° flexion).
Performed only if patellar medial subluxation test is abnormal (patellar medial subluxation ≤ 5 mm on the manual medial translation test, knee at 30° flexion). Arthroscopic retinacular release performed with commercial radiofrequency wand through anterolateral portal.
Arthroscopic retinacular release performed with commercial radiofrequency wand through anterolateral portal. Initiated from 9 o’clock position (right knee), continued distally to 1 cm below inferior pole of patella with the knee in full extension.
Initiated from 9 o’clock position (right knee), continued distally to 1 cm below inferior pole of patella with the knee in full extension.Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree