Chapter 29 Meniscus Transplantation
Diagnosis, Operative Techniques, and Clinical Outcomes
INDICATIONS
The meniscus provides important functions in the human knee, including load bearing, shock absorption, stability, and joint nutrition, that are vital for the integrity of the articular cartilage. Although many meniscus tears can be successfully repaired, including complex tears that extend into the central avascular region,52,53 not all are salvageable, especially if considerable tissue damage has occurred. Transplantation of human menisci is hypothesized to restore partial load-bearing meniscus function, decrease patient symptoms, and provide some chondroprotective effects.10,25,37,63,70 However, the procedure remains in an evolving state, as investigations of tissue-processing, secondary sterilization, and long-term function continue to evaluate its effectiveness. Clinical studies have shown that meniscus transplantation decreases tibiofemoral joint pain in the short term. However, long-term investigations report that most transplants gradually deteriorate, tear, or shrink in size, thereby losing the ability to provide function, as is described later. Accordingly, the goal is to provide short-term benefits until a more suitable meniscus transplant is clinically available. At best, the transplant provides only partial function, and therefore, strenuous sports and high-impact activities are not advised postoperatively even though many younger patients have the desire to return to unrestricted athletics. Education of the patient and family is required so that all understand and accept these current limitations of the procedure.
The optimal candidate is a patient under the age of 50 who has had a total meniscectomy, has pain that limits daily activities, and demonstrates early articular cartilage deterioration in the involved tibiofemoral compartment. There should be no radiographic evidence of advanced tibiofemoral joint arthritis. At least 2 mm of tibiofemoral joint space should be visible on 45° weight-bearing posteroanterior (PA) radiographs.50 Arthroscopic examination performed prior to meniscus transplantation confirms that the patient is a suitable candidate. In the most advanced cases, there should be no or only minimal bone exposed on tibiofemoral surfaces. Few treatment options are available for these individuals, especially those younger than 30 years of age, and the goal in the short-term is to decrease pain, increase knee function, allow pain-free activities of daily living, and delay the onset of tibiofemoral arthritis. Normal axial alignment and a stable joint are required. The body mass index (BMI) must be within normal range.
CONTRAINDICATIONS
Patients who have had a meniscectomy are evaluated with 45° PA weight-bearing radiographs and magnetic resonance imaging (MRI)45,46 to determine the status of the joint, articular cartilage, and subchondral bone edema. Advanced knee joint arthritis with flattening of the femoral condyle, concavity of the tibial plateau, and osteophytes that prevent anatomic seating of the meniscus transplant are contraindications. Clinical studies have shown poor results and high failure rates in knees with this amount of joint damage.19,35,46,60
Untreated lower limb malalignment is associated with failed meniscus transplantation8,12,64,65; therefore, the patient must be willing to first undergo a corrective osteotomy. Axial correction is recommended in knees in which the weight-bearing line is less than 45% (varus) or greater than 55% (valgus), representing a 2° to 3° change from normal alignment. Uncorrected knee joint instability, especially anterior cruciate ligament (ACL) deficiency, is also associated with poor outcomes after meniscus transplantation.64 Patients must undergo concurrent or staged ACL reconstruction to restore normal stability to protect the meniscus transplant.
The clinical problem is often encountered involving patients younger than 30 years of age who have undergone meniscectomy years ago, do not have articular cartilage damage, and are asymptomatic. Clinical studies show that eventual deterioration of the meniscectomized tibiofemoral compartment will most likely occur. These patients are advised that there is no optimal or predictable operative procedure to replace meniscus function and that they should decrease or refrain from participating in high-impact, strenuous activities. There are sensitive and accurate MRI cartilage techniques to determine the status of the articular cartilage in the meniscectomized compartment.44,45 When early but definite articular cartilage damage is detected, it can be logically assumed that the joint deterioration will continue over time and the opportunity exists to perform meniscus transplantation. This still represents a difficult choice for the patient in terms of undergoing surgery before the onset of major joint symptoms. In addition, the transplant may not function and further arthroscopic surgery may be required to remove the tissue. Most patients who develop early cartilage damage in the meniscectomized compartment complain of pain with strenuous athletic activities, but not with recreational or daily activities. These patients are not truly asymptomatic and desire to lessen the risk of further joint deterioration to the level at which it will affect lower intensity activities. Patient education and a conservative approach to recommendation of transplantation are important until a more dependable transplant is available.
Critical Points CONTRAINDICATIONS
The presence of a full-thickness femoral condylar defect with bone exposure is a relative contraindication to meniscus transplantation. Concurrent articular cartilage restorative procedures (such as osteochondral grafts or autologous chondrocyte implantation) can be successfully performed with meniscus transplantation18,38 and expand the indications to include knees with these lesions.
CLINICAL BIOMECHANICS
Chondroprotective Effects
The deleterious effects of meniscectomy on knee joint contact pressures and tibiofemoral articular cartilage have been demonstrated in multiple experimental studies.7,25,28,42,63,72,74 Bylski-Austrow and coworkers7 reported that medial meniscectomy caused a decrease in medial compartment contact pressures compared with intact joints of 70% by 4 months postoperatively and 42% by 8 months postoperatively in the goat model. The overall goal of meniscus transplantation is to protect the articular cartilage from subsequent deterioration.
Critical Points CLINICAL BIOMECHANICS
Chondroprotective Effects
Knee Joint Contact Mechanics after Meniscus Transplantation
Effect Fixation and Location of Meniscus Transplants
Szomor and associates63 conducted a study to determine the chondroprotective effects of meniscus allografts and autografts in a large animal model. Medial meniscectomy, medial meniscus autografts, and medial meniscus allografts were performed in 24 sheep. The grafts were placed into the anatomic anterior and posterior horn attachment sites and secured to the tibial plateau with three suture anchors. At 16 weeks postoperative, both the allograft and the autograft knees demonstrated a 34% to 40% reduction in the score for macroscopic damage to the articular cartilage and an approximate 50% reduction in the area of damage to the articular cartilage compared with the meniscectomized knees. However, neither graft provided complete protection, which the investigators hypothesized could have been due to nonisometric positioning and tensioning and graft fixation. Histologic analysis revealed that the allografts had fibrinoid degeneration, areas of hypocellularity, and cloning of meniscus cells.
Kelly and colleagues25 developed a meniscus allograft surgical technique that attempted to restore the anatomic anterior tibial and posterior femoral meniscal attachments in a sheep model. Fixation of the allografts was accomplished through bone tunnels. Lateral meniscus allografts were implanted into 17 animals, and lateral meniscectomies were performed in 24 animals. Gross inspection, histologic analysis, biomechanical testing, MRI, and T2 mapping of the central weight-bearing portion of the lateral tibial plateau performed 2 and 4 months postoperatively demonstrated protective effects of the allografts. Significantly decreased cartilage wear and increased cartilage stiffness were found in the allografted joints compared with the meniscectomized knees. However, at 4 months postoperative, the allografted knees had significantly worse values for these outcome measures than the intact knees. The authors noted the successful utilization of MRI with T2 mapping to detect early articular cartilage degeneration. In summary, experimental studies published to date are short term and show only partial function of the meniscus transplant in terms of contact area measurements.
Knee Joint Contact Mechanics after Meniscus Transplantation
Alhalki and coworkers2 measured the maximum pressure, mean pressure, and contact area of the medial tibial articular surface after medial meniscectomy and implantation of ipsilateral medial meniscus autografts and cryopreserved allografts in 10 cadaveric knees (mean age, 70 yr). The autografts and allografts were implanted using the same technique of bone plug fixation through anterior and posterior horn transtibial tunnels.
The allografts significantly reduced normalized maximum and mean contact pressures by 75% compared with meniscectomized knees. In addition, the maximum pressure was restricted to a small region of the contact area. The authors hypothesized that the reduction of this magnitude could reduce the rate of cartilage wear compared with that in a meniscectomized knee. However, the allografts did not restore normal contact mechanics and demonstrated greater variability in normalized maximum and mean contact pressures than the autografts. The authors concluded that the variability in contact mechanics could have been due to poor matching of the three-dimensional geometry of the allograft to the recipient knee. Dimensions for the allograft were matched from standard anteroposterior (AP) and lateral radiographs in the transverse plane. Studies by Paletta and associates41 and Haut and colleagues21 revealed that measurements made in the transverse plane only weakly predict the cross-sectional shape of the meniscus.
The effect of the size of lateral meniscus allografts (in comparison with native menisci) on tibial plateau contact mechanics was investigated by Dienst and coworkers.14 Allografts that were 17.5% larger than native menisci showed significantly higher contact pressures across the articular cartilage. Although allografts sized 10.5% smaller than native menisci had normal contact forces, increased forces in the meniscal tissue were detected that the authors hypothesized could cause early transplant failure. Allografts sized 10% larger or smaller than native menisci restored contact mechanics close to normal. The authors concluded that the surgeon should select lateral meniscus transplants (LMTs) that are slightly larger than native menisci (rather than smaller) to reduce the risk of early failure.
Paletta and associates41 investigated the effects of lateral meniscectomy, cryopreserved lateral meniscus transplantation with bone plug fixation, and lateral meniscus transplantation without fixation of the anterior and posterior horn attachments. The study involved 10 cadaver knees less than 48 years of age. The lateral meniscal transplants increased total contact area by 42% to 65% compared with meniscectomized knees at all flexion angles (0°, 30°, and 60°). However, there remained a residual 17% to 23% decrease in contact area compared with intact knees. Release of the horn attachments resulted in contact area that was identical to meniscectomized specimens. McDermott and associates28 assessed the effects of lateral meniscal transplantation with and without bone block fixation in eight cadaver knees. These investigators reported no difference between the two methods in peak contact pressures compared with intact knees. The cadaver specimens used in the study were aged 81 to 98 years, and all had moderate to severe degenerative changes. In addition, no formal size matching was performed with the allografts and recipient knees.
Effect Fixation and Location of Meniscus Transplants
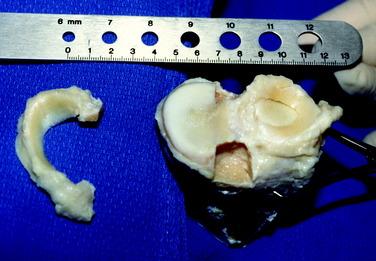
The method of fixation of meniscus transplants to the surrounding tissues is believed to be paramount in subsequent load-bearing function and chondroprotective effects. The goal is to reproduce the normal attachment sites, allowing lateral and medial transplants to remain in their anatomic location and move normally throughout knee motion.47,68 The use of a transplant with bone for fixation incorporated with either a central bone bridge or a two-tunnel technique (as described later in this chapter) is, in the authors’ opinion, required to obtain these goals. Soft tissue meniscus transplants, without bone fixation, are not recommended. Although soft tissue transplants are far easier to prepare and implant surgically, scientific data are inadequate to support that the soft tissue ends of the meniscus implant will heal and provide the circumferential tension in the meniscus that is required for function (Fig. 29-1).
The importance of securing the anterior and posterior horns of an LMT was documented by Chen and colleagues,9 who investigated a variety of surgical methods for meniscus implantation. Using an autograft cadaver model, the study revealed that a transplant that had either a bony bridge or bone plug fixation of both horns produced contact area, peak contact pressure, and average central pressure results similar to those of an intact meniscus. Procedures in which either only one horn was secured or neither horn was secured demonstrated a loss of mechanical function and subsequent expected benefit of the transplant.
Alhalki and coworkers1 compared three fixation methods of medial meniscus autografts in cadaver knees to determine which method restored tibial contact mechanics closest to normal. The experimental design tested bone plug fixation alone, bone plug fixation combined with peripheral suturing of the transplant to the native rim, and suturing of the horns through bone tunnels combined with peripheral suturing of the transplant to the native rim. The study revealed that bone plug fixation produced contact mechanics closest to normal; however, the maximum pressure was significantly greater than that in the intact knee. There was no benefit in adding peripheral sutures to the bone plug fixation model. Importantly, fixation with sutures only did not restore normal contact mechanics and was not recommended by the investigators.
Verma and associates72 measured medial compartment peak pressure, mean pressure, and contact area in eight cadaver knees to determine whether a difference existed between medial meniscus transplants (MMTs) implanted with a bone plug technique and those with a bone trough technique. The data indicated no difference between the two techniques for all three variables, which were restored to values similar to those measured in the intact knees. The authors cited clinical advantages with the trough technique for both medial and lateral meniscus transplantation.
The effect of variations in placement of the posterior horn attachment of an MMT were investigated by Sekaran and colleagues.56 Using a cadaver autograft model, the posterior horn tunnel was placed either in its anatomic position or 5 mm medial or 5 mm posterior to the anatomic location. The study showed that placing the posterior horn tunnel 5 mm medial to its anatomic position caused an increase in normalized maximum pressure, a posterior shift in the location of the centroid of the contact area, and an increase in the normalized mean pressure. Placing the posterior horn tunnel 5 mm posterior was not as detrimental; however, this location resulted in a significant shift in the centroid of contact area. The authors concluded that surgeons should place the posterior horn tunnel as close to its anatomic position as possible, with a tolerance limit of less than 5 mm medial and 5 mm posterior to this location.
CLINICAL EVALUATION
MRI is obtained using proton-density–weighted, high-resolution, fast-spin-echo sequences45,46 to determine the status of the articular cartilage and prior meniscectomized tibiofemoral compartment. Radiographs include AP, lateral at 30° of knee flexion, weight-bearing PA at 45° of knee flexion, and patellofemoral axial views. Axial lower limb alignment is measured using double-limb standing hip-knee-ankle weight-bearing radiographs16 in knees that demonstrate varus or valgus alignment.
Patients complete questionnaires and are interviewed for the assessment of symptoms, functional limitations, sports and occupational activity levels, and patient perception of the overall knee condition according to the Cincinnati Knee Rating System (CKRS).4
PREOPERATIVE PLANNING
Meniscus transplants are obtained from tissue banks accredited by the American Association of Tissue Banks (AATB) and inspected by the U.S. Food and Drug Administration (FDA), in which serologic testing meets or exceeds the standards of these organizations.67 Importantly, donor selection criteria may vary between tissue banks and the surgeon should understand the specific criteria used by the bank chosen to supply the transplant.
A variety of sterilization techniques have been described for meniscus transplants, including none (fresh-frozen), irradiated, cryopreserved, and proprietary chemical techniques. To date, no scientific data exist to select one type of graft processing method over another. Some authors8 advocate combined secondary sterilization using low-dose irradiation (1–2 Mrads) and chemical agents.
Surgeons should be aware that so-called sterilization processes may not prevent contamination and do not guarantee a sterile graft. The authors recommend that grafts be selected that have undergone some form of sterilization to decrease the risk of bacterial infection. Prophylactic antibiotics are administered intravenously before surgery, and patients are carefully monitored postoperatively for any signs of infection. The implications of different processing techniques on graft sterility and donor selection issues, allograft harvesting techniques, and disease testing are beyond the scope of this chapter and have been discussed in detail by others.5,10,67
Although there is no standard protocol at present, AP and lateral radiographs are used to obtain approximate width and length measurements for the meniscus transplant.43 A number of studies have been performed to determine the appropriate sizing method for meniscus transplants.15,21,58,61 Shaffer and coworkers58 found no difference between AP radiographs and MRI in terms of accuracy in measuring actual meniscus width and length. With accuracy defined as no more than a 2-mm difference between actual meniscus dimensions in cadaver specimens and that measured on the films, the accuracy rates were 33% for AP radiographs and 37% for MRI. Stone and associates61 suggested that recipient height, weight, and gender be considered as important matching criteria when selecting meniscus transplants. These investigators measured meniscus and tibial plateau dimensions in 111 patients using MRI and correlated the dimensions with the patients’ height, weight, BMI, and gender. Height correlated well with total tibial plateau width (R = 0.7194), and females generally had smaller meniscus dimensions than males. In addition, patients with a BMI greater than 25 had larger meniscus dimensions than patients with a lower BMI at any given height.
Critical Points PREOPERATIVE PLANNING
Donahue and colleagues15 developed an algorithm for meniscus transplant sizing based on MRI measurements. The authors recommended that tissue banks follow the algorithm, which involves a series of six steps. These include making four transverse and six cross-sectional measurements for each transplant in the bank’s inventory using a three-dimensional coordinate digitizing system, obtaining MRI of the recipient’s uninjured knee and measuring nine parameters for the medial or lateral meniscus, and performing a series of calculations to determine the best match.
The problem still exists that even though an approximate size can be determined preoperatively, in many knees the tibiofemoral joint has undergone degenerative changes that produce subtle alterations in joint geometry leading to permanent alterations in the normal surface stress distribution of the joint surface.7 A meniscus transplant does not have the ability to restore the native or normal state of the meniscectomized compartment. Future studies are required to determine the effect of subtle size and shape mismatch of the transplant on retaining articular cartilage functional properties. A chondroprotective effect of meniscus transplants has yet to be proved. This involves sophisticated questions regarding the chondrocyte function, cartilage collagen, and glycosaminoglycan homeostasis and resultant biomechanical properties.
It is preferred that the tissue bank provides a digital photograph of the transplant selected for the patient before surgery. A metric ruler is placed adjacent to the transplant in the photograph to ensure that the specimen is of adequate size and width. Certain medial menisci may have a hypoplastic anterior horn that is narrow, inserting distal to the medial tibial surface (type III6), and are not acceptable for implantation. The middle third of a medial or lateral meniscus may be 8 to 10 mm in width and suitable only for small patients. The lateral meniscus may have reduced anterior-to-posterior length, less than that calculated on the sagittal radiograph, and not be suitable for implantation.
Knees with associated varus osseous malalignment require a staged corrective osteotomy prior to the meniscus transplant procedure. Knees with ligament deficiency require a staged ligament reconstruction. Some studies have advocated concurrent ACL reconstruction and meniscus transplantation.20,57,77 The normal ACL tibial attachment site and the ACL tibial graft tunnel may compromise meniscus transplant tibial fixation. This may occur when the slot technique to be described is selected in patients whose central tibial intercondylar region is not wide enough to accommodate both the meniscus transplant slot and the ACL tibial graft tunnel. Because it is not possible in these knees to use the central slot technique, a two-tunnel procedure is selected for the MMT.
INTRAOPERATIVE EVALUATION
All knee ligament subluxation tests should be performed after the induction of anesthesia in both the injured and the contralateral limbs. The amounts of increased anterior tibial translation, posterior tibial translation, lateral and medial joint opening, and external tibial rotation should be documented. A thorough arthroscopic examination should be conducted, documenting articular cartilage surface abnormalities39 and the condition of the menisci.
OPERATIVE TECHNIQUE: LMT
Critical Points INTRAOPERATIVE EVALUATION
Critical Points OPERATIVE TECHNIQUE: LATERAL MENISCUS TRANSPLANT
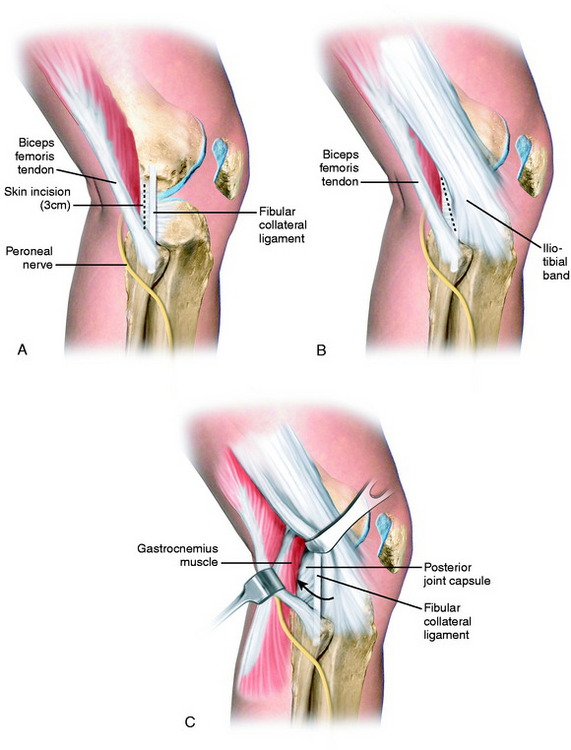
A second 3-cm posterolateral incision is made just behind the fibular collateral ligament (FCL; Fig. 29-2), similar to that described in Chapter 28, Meniscus Tears: Diagnosis, Repair Techniques, and Clinical Outcomes, for inside-out lateral meniscus repairs.29,53 The interval between the short head of the biceps muscle and the iliotibial band is identified and incised. The lateral head of the gastrocnemius is gently dissected with Metzenbaum scissors off the posterior capsule at the joint line just above the fibular head. Care is taken at this point because dissection that extends too far proximal to the joint line would enter the joint capsule. If this occurs, a capsular repair is required to maintain joint integrity during the inside-out meniscal repair procedure.
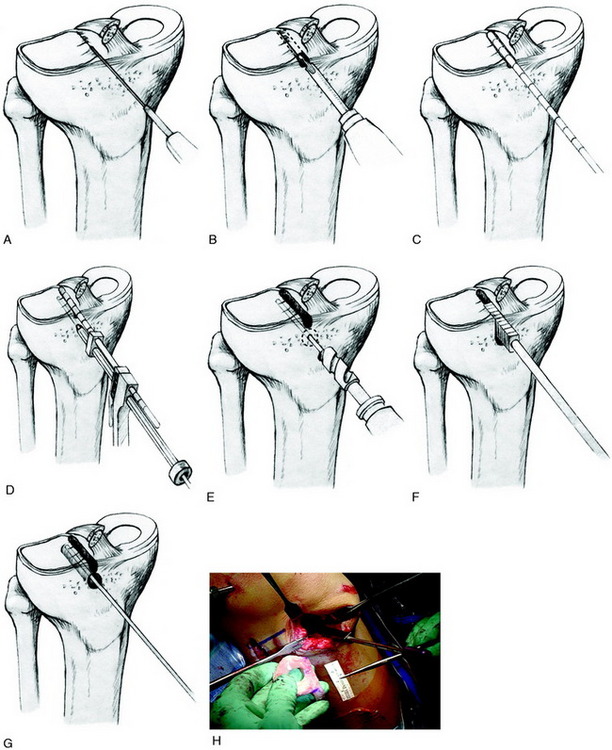
The sequence of steps to prepare the lateral tibial slot is shown in Figure 29-3. The tibial bone slot is 1 to 2 mm wider than the transplant to facilitate implantation. The anterior and posterior horns of the transplant are placed into their normal attachment locations, adjacent to the ACL. It is important to note that a prior ACL reconstruction in which the tibial tunnel was placed in a lateral position may produce a technical problem in creating the tibial slot.
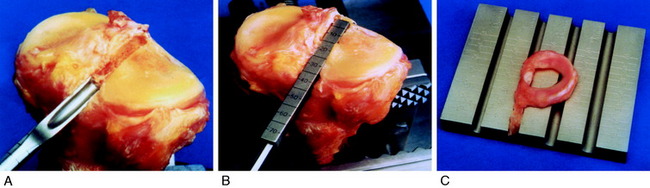
A starter chisel and finishing chisels provide an alternative technique to create and fashion the tibial slot to its final depth and width (Fig. 29-4A). A tibial slot sizing guide is used to check the length and depth (see Fig. 29-4B). A sizing block (see Fig. 29-4C) confirms that the transplant bone bridge is of the correct width and depth.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree