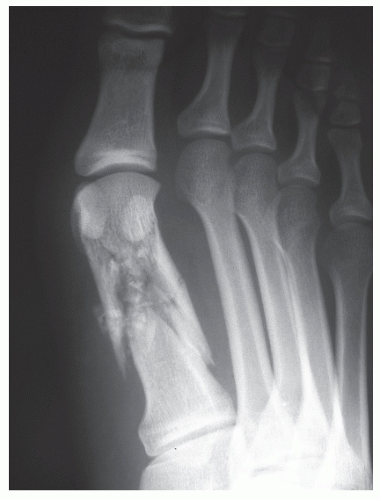
Metatarsal Fractures
Michael S. Lee
Linda Ho
Fractures of the metatarsals are frequently encountered injuries. They account for up to 55% of all foot fractures and may represent nearly 7% of all reported fractures (1,2,3,4 and 5). The fifth metatarsal is the most often injured metatarsal (6). Metatarsal stress fractures represent approximately 2.5% of all metatarsal fractures and most commonly affect the second or third metatarsals (2). Metatarsal fractures are rarely open, and most multiple fracture injuries are contiguous in nature. The mechanism of injury for metatarsal fractures may include crush injuries, blunt trauma, or indirect forces such as inversion or twisting injuries, falls, or sports injuries.
FUNCTIONAL ANATOMY
Each metatarsal is divided into the distal head, neck, diaphysis, and proximal base. The base of each metatarsal is broad and primarily consists of cancellous bone. Each metatarsal is bound to the adjacent metatarsal and the respective midtarsal bone by strong plantar and weaker dorsal ligaments. The first metatarsal is the exception as it is only loosely attached to the second metatarsal bone. Lisfranc ligament secures the medial cuneiform to the base of the second metatarsal. The diaphyseal portion of each metatarsal is concave plantarly and consists of mostly cortical bone. The diaphysis lacks the robust vascularity that the base and head claim (7). The metatarsals are attached to each other distally by the transverse metatarsal ligament (7).
The first metatarsal articulates with two sesamoid bones and bears a considerable portion of the body weight with gait at the first metatarsophalangeal joint. The physeal plate is located at the base of the first metatarsal, while it is located distally in the four lesser metatarsal bones. The styloid process or tuberosity of the fifth metatarsal has a secondary ossification center proximally in addition to the distal physeal plate.
Muscular attachments include the intrinsic interossei muscles, the tendon attachments of the peroneus brevis and peroneus tertius on the fifth metatarsal tuberosity, and the attachments of the peroneus longus and the tibialis anterior tendons on the base of the first metatarsal. The lack of extrinsic muscular attachments to the central second, third, and fourth metatarsals contributes to the relative stability of fractures in this area.
The vascular supply to the metatarsals originates from the dorsal metatarsal arteries off of the dorsalis pedis artery and the plantar metatarsal arteries off the posterior tibial artery. Vascular supply to the metatarsal heads differs from the supply of the respective diaphysis (8). Perforating arteries into the shaft anastomose numerously along each diaphysis and with the surrounding periosteum. Metatarsal heads have extraosseous anastomoses between dorsal and plantar metatarsal arteries that enter the metatarsal head and become terminal end arteries. Contributions of blood supply to the metatarsal head also proceed through collateral ligament insertions around the metatarsophalangeal joint (9). The blood supply to the base of the fifth metatarsal comes from two sources that result in an area of poor vascularity (10). This watershed area is often implicated in poor healing in proximal metaphyseal-diaphyseal fractures of the fifth metatarsal (11,12).
EVALUATION
The evaluation and diagnosis of metatarsal fractures is based on both clinical and radiographic exam. Patients will often present with antalgic gait resulting from pain that is worsened with weight-bearing, diffuse edema restricting movement, increased warmth, and ecchymosis. Pain may be localized at first, but will be less distinct after considerable swelling has developed. Stress fractures often present with less acute symptoms including low-grade swelling and pinpoint tenderness over the involved metatarsal.
Thorough neurovascular assessment is imperative, particularly in cases of crush injuries to the forefoot. While rare, compartment syndrome should be considered, particularly in cases with severe swelling, soft tissue injury, or crush injuries (13,14). Soft tissue damage should be assessed. Open fractures call for prompt management including débridement and irrigation, tetanus, and antibiotic administration according to open fracture protocol (15). Appropriate management of soft tissue defects greatly affects the outcome of open metatarsal fractures (16).
Radiographic evaluation of metatarsal fractures typically demonstrates the type, orientation, and degree of displacement. In cases of severe crush injuries, penetrating trauma (i.e., gunshot wounds), or in suspected cases of stress fractures, advanced imaging may be warranted. Cases of malunion or nonunion may also require advanced imaging such as computed tomography (CT) or magnetic resonance imaging (MRI) to accurately diagnose the condition or aid in preoperative planning (17,18). Technetium bone scans, while highly sensitive for metatarsal stress fractures, are poorly specific and have fewer clinical indications with the availability of MRI (19).
METATARSAL STRESS FRACTURES
Chronic repetitive overloading of the metatarsals results in stress fractures. The measured strain forces during jumping or walking have been shown to be two times higher in the metatarsal than in the tibia (20). Prodromal symptoms are common in cases of metatarsal stress fractures. Individuals particularly prone to metatarsal stress fractures include athletes, ballet dancers, military personnel, and patients with various medical conditions including osteoporosis, diabetes, inflammatory arthritis, and chronic steroid use (21,22,23,24,25 and 26). Second metatarsal base stress fractures are common in ballet dancers due to en pointe dancing (24).
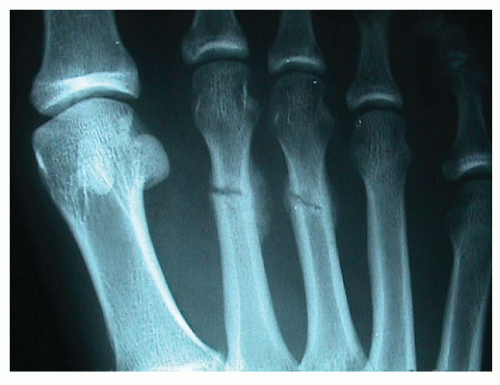 Figure 104.1 Typical second and third metatarsal stress fractures demonstrating early healing with bony exocallus formation. |
Metatarsal stress fractures may also be iatrogenic after procedures such as hallux valgus correction or hindfoot arthrodesis procedures (27,28 and 29). They may also be associated with various deformities of the forefoot, hindfoot, or ankle (26,30,31). Failure to address the underlying deformities either biomechanically or surgically may result in recurrent stress injuries.
Symptoms typically include forefoot swelling, warmth, and localized tenderness to the area directly dorsal to the involved metatarsal. The area of tenderness is typically proximal to the metatarsophalangeal joint. Radiographs typically lag behind the clinical findings and may be negative for 2 to 3 weeks following initial symptoms or clinical presentation (Fig. 104.1) (32). In some cases, advanced imaging with either MRI or a bone scan may be indicated to clearly diagnose the stress fracture, particularly in cases of fourth metatarsal base stress fractures (33).
TREATMENT
The treatment of metatarsal stress fractures typically includes a 3- to 4-week period of protected weight-bearing in a surgical shoe or fracture boot. Crutches may or may not be needed based on the patient’s symptoms. Elevation, ice, and NSAIDs may be warranted to reduce swelling and pain initially. In rare cases of stress fracture nonunion or displacement, surgical management with or without grafting may be warranted. Additionally, stress fractures of the fifth metatarsal diaphyseal-metaphyseal junction typically require internal fixation (see fifth metatarsal fractures).
FIRST METATARSAL FRACTURES
First metatarsal fractures are rare compared with fractures of the lesser metatarsals. Fractures to the first often occur proximally at the junction between the diaphysis and metaphysis. They are often the result of direct trauma such as a crush injury or penetrating injury such as a gunshot wound (Fig. 104.2). In some cases, the peroneus longus tendon may cause an avulsiontype injury from the base of the first metatarsal (34).
The weight-bearing requirements of the first metatarsal during the stance phase of gait make preservation of first metatarsal and first metatarsophalangeal joint function essential. Therefore, delayed union, nonunion, or malunion of the first metatarsal can result in significant morbidity. Changes to the metatarsal length or sagittal plane deformities will affect weightbearing biomechanics of the first ray. Arthritic damage and stiffness to the first metatarsophalangeal joint may occur from dorsal jamming due to sagittal plane malalignment. Plantar pressure lesions under the first metatarsal head may occur as the result of the metatarsal being oriented too plantar. In addition to deformities of the first metatarsal itself, the inability of the first metatarsal to bear weight properly will cause excess loading on the lesser metatarsals, resulting in possible stress fractures and plantar pressure lesions, particularly to the second or third metatarsals (35,36).
Nonoperative treatment for nondisplaced or minimally displaced first metatarsal fractures typically includes cast or boot immobilization and non-weight-bearing for 4 to 6 weeks (34,37,38). Closed reduction via the use of Chinese finger traps and counterweights for first metatarsal fractures has been considered challenging because of the extrinsic pull of the tibialis anterior and peroneus longus tendons and the inherent instability of maintaining alignment of the distal fragment.
Displaced and comminuted fractures require fixation to prevent malalignment of the first metatarsal and prevent malunion morbidity. Percutaneous wire fixation, cerclage wiring, interfragmentary screw fixation, and plate fixation have all been reported as options for fixation, depending on configuration of the fracture at the head, neck, shaft, or base of the first metatarsal. External fixation may also be recommended for comminuted fractures to maintain metatarsal length (39). The primary goal of all of the fixation techniques employed should be anatomical restoration of the first metatarsal (40).
Complications after first metatarsal fractures include first ray shortening or elevation that can often lead to malalignment concerns of the hallux including hallux valgus, hallux rigidus,
or hallux malleus. This may also lead to lesser metatarsalgia or second metatarsophalangeal joint instability. Restoration of proper length and metatarsal declination greatly reduces problems associated with lesser metatarsalgia.
or hallux malleus. This may also lead to lesser metatarsalgia or second metatarsophalangeal joint instability. Restoration of proper length and metatarsal declination greatly reduces problems associated with lesser metatarsalgia.
PERCUTANEOUS FIXATION OF FIRST METATARSAL FRACTURES
Percutaneous fixation is often considered when the first metatarsal fracture is located at the base of the metatarsal or in skeletally immature patients due to the proximal location of the physeal plate. The orientation of fractures in this particular area has a tendency to be transverse in nature and does not lend itself well to screw fixation.
Percutaneous fixation is achieved with or without tourniquet control. Typically, a tourniquet is applied but not inflated unless the procedure is converted to “open.” Distraction of the great toe and first metatarsal head allows the fracture to be reduced into proper alignment. In some cases, a small ancillary incision is required to manipulate the proximal end of the distal fragment into proper alignment. This is achieved using a freer elevator and fluoroscopic assistance to manipulate the fracture fragment. It is also beneficial to drive a 0.062-inch Kirschner wire (K-wire) into the distal fracture fragment that can then be used to manipulate the fragment into proper alignment before advancing the K-wire across the fracture site. Typically, the fracture is fixated with two percutaneous K-wires across the fracture site, with one passing from the medial first metatarsal into the medial cuneiform or intermediate cuneiform (Fig. 104.3). The second K-wire passes from the dorsal aspect of the first metatarsal into the plantar medial aspect of the medial cuneiform.
Postoperatively, the K-wires are left in place for 5 to 6 weeks. The patient is typically placed in a fracture boot and touchdown heel weight-bearing is allowed at around 3 to 4 weeks. Weight-bearing is progressed based on radiographic healing of the first metatarsal fracture.
EXTERNAL FIXATION OF FIRST METATARSAL FRACTURES
External fixation of first metatarsal fractures is reserved for cases of crush injuries or penetrating injuries (i.e., gunshot wounds) when there is high comminution of the metatarsal. The purpose of the external fixator is to maintain length of the first metatarsal and provide stability to the bony structures in the presence of significant soft tissue disruption. In some cases, external fixation is the only option due to the comminuted nature of the metatarsal and the inability to fixate it in any other manner.
A small monorail fixator is often utilized. Ideally, half pins are placed both in the base of the first metatarsal and the medial cuneiform (Fig. 104.4). These are placed through small stab incision with fluoroscopic assistance. The distal half pins are then placed in the first metatarsal head or neck distal to the fracture site through small stab incisions as well. The fracture is then manipulated into proper anatomic reduction and alignment. The fixator is locked down to maintain stability and alignment.
Partial weight-bearing on the heel is allowed while the fixator is intact. Typically, full weight-bearing is not tolerated or advised. Radiographic healing determines the timeframe for the external fixator; in cases of penetrating injuries, the defect may require an extended timeframe or subsequent grafting techniques once the soft tissues have consolidated and there is no further risk of infection.
ORIF OF FIRST METATARSAL FRACTURES
Midshaft first metatarsal fractures and neck fractures lend themselves well to open reduction and internal fixation (ORIF). These cases are often done under tourniquet control. A dorsal or dorsomedial approach is implemented. Dissection is carried through the periosteum and the fracture is identified. The fracture is reduced into proper anatomic alignment and maintained with reduction forceps. If the fracture line runs perpendicular to the long axis of the metatarsal, then a K-wire may be used for temporary fixation. The senior author has found that T and L plates work nicely on the first metatarsal (Fig. 104.5). Mini fragment plates are often utilized. When possible, based on the orientation of the fracture, interfragmentary compression is also achieved with a 2.7-mm cortical screw. A small locking plate may also be utilized.
CENTRAL METATARSALS
Central metatarsal fractures are often the result of direct trauma such as crush injuries. In these cases, care must be taken to rule out compartment syndrome or vascular disruption to the lesser digits (41). In such cases of vascular compromise from crush injuries, it is prudent to avoid surgical intervention until it is completely clear that the vascular status of the lesser digits has not been disrupted. Cases of compartment syndrome mandate aggressive management with decompressive fasciotomy prior to ORIF.
Nondisplaced or minimally displaced fractures may be treated with cast immobilization or protected weight-bearing in a fracture boot for 4 to 8 weeks (26,41,42). In some cases, especially with isolated fractures, early weight-bearing to tolerance in a surgical shoe may be adequate (43). Weight-bearing is progressed according to radiographic healing and clinical symptoms.
Generally, surgical management is warranted for central metatarsal fractures if displacement is more than 3 to 4 mm or angular malalignment is greater than 10 degrees (13,37,44,45 and 46). Options for surgical repair of central metatarsal fractures include percutaneous pinning (retrograde), cerclage wiring, plate fixation, and intramedullary pinning (43,47). Typically, longitudinal incisions over the metatarsal or between two metatarsals are implemented. For metatarsal neck or distal shaft fractures, Ozer and Oznur (48) have suggested a single transverse dorsal incision over the metatarsal necks to treat multimetatarsal fractures instead of multiple longitudinal incisions when fixating more than two fractured metatarsals.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree