Initial Evaluation and Management of Complex Traumatic Wounds
Patricia L. McKay
George Nanos
The principles in this chapter are forged from our experience with the treatment of high energy contaminated wounds resulting from recent overseas military conflicts. The soft tissue injuries discussed within this chapter encompass a broad spectrum of clinical presentations, both acute and chronic. These treatment protocols reflect the ever-growing body of scientific knowledge and technological advances contributing to the successful treatment of our patients. In the following illustrations, we hope to point out the common mistakes and potential pitfalls of operative and perioperative wound management and provide surgeons with a framework for successful treatment of all types of wounds.
Initial Evaluation
A thorough initial patient evaluation gives the surgeon the information by which to formulate a treatment plan with the best chance for success. A complete and accurate history must include the circumstances leading to the current wound presentation, the mechanism of injury if associated with trauma, underlying medical conditions, current occupational and socioeconomic status, and patient social habits such as smoking which may have detrimental effects on reconstructive efforts (Table 2-1).
In cases of trauma the energy level, mechanism, location, and the time course from injury to presentation are invaluable in predicting prognosis and planning treatment. Medical comorbidities such as underlying cardiopulmonary or peripheral vascular disease, endocrinopathy, neuropathic disease, immunocompromising conditions, psychiatric illness, nutritional deficits, and allergies can negatively impact the success of treatment if not identified and optimized. Medical consultation and comanagement is recommended in these cases. Tetanus status must be addressed in accordance with Centers for Disease Control guidelines.
Failure to fully recognize the scope of the wound and/or injury can have dreadful consequences to the outcome. A detailed physical examination with critical assessment of vital signs, secondary survey, and multi-system examination is required in all cases to evaluate the wound and exclude other medical conditions or associated injury that may take greater priority in treatment.
In multi-system trauma, the Advanced Trauma Life Support (ATLS) approach, beginning with airway, breathing, and circulation (ABC’s) is recommended. Traumatologists or critical care specialists should be the principle coordinators of all initial medical care to ensure appropriate global management of the patient.
Critical attention should be directed to vascular status. If capillary refill and/or pulses are abnormal or absent, or if the mechanism introduces suspicion for vascular injury, Doppler testing and/or perfusion studies must be obtained. Revascularization or repair of vessels should be completed prior to, or concurrent with, surgical wound treatment. Special attention should also be paid to the neurological examination, and all deficits clearly documented. In cases of extremity trauma, a high index of suspicion for compartment syndrome is essential. Continued reevaluation is required with adjunctive use of compartment pressure monitoring if the diagnosis is in question, emergent compartment release should be performed if clinically indicated, and prophylactic release should be considered in trauma cases with revascularization procedures.
Table 2-1. Wound Treatment Pitfalls | ||
|---|---|---|
|
Ancillary studies aid in full comprehension of the clinical situation. Plain radiographs should be routinely obtained to evaluate for associated fracture, foreign body, exostosis, osteomyelitis, soft tissue emphysema, vascular calcifications such as those associated with Diabetes Mellitus, or other factors contributing to or resulting from the overlying wound. CT scans and MRI may provide additional valuable information. Markers of hematologic and immune status, clotting factors, electrolyte and renal function, and adequacy of resuscitation must all be accounted for based on the clinical situation.
Careful documentation of every aspect of the evaluation and treatment must be made, and generous use of medical photography is helpful not only for documentation, but also for preoperative planning purposes.
Preoperative Planning
Once the evaluation is complete, the surgeon can formulate a treatment plan and determine if surgical intervention is required. The most important question to consider is whether the surgeon and the facility possess the requisite experience, capability, equipment, and consultative and ancillary services to render optimum treatment (Fig. 2-1). The surgeon must have the technical ability and anatomic knowledge for the given location of the injury. The treating hospital and operating room must also be able to furnish the necessary instruments, implants, and wound treatment dressings. When confronted with cases of multi-system trauma, a multidisciplinary team involving traumatologists, intensivists, medical consultants, infectious disease specialists, and wound care support personnel is generally considered to be mandatory. If unable to meet these basic requirements, the clinical situation should be carefully reviewed and the strongest consideration should be given for referral to a higher level of care.
Surgery
Patient positioning varies depending on the site of the wound in question. General or regional anesthesia may be employed, and consideration for peripheral nerve blocks should be considered for perioperative pain control. A sterile or non-sterile tourniquet is indispensable to ensure optimal visualization for meticulous, thorough debridement and protection of vital structures. Appropriate broad-spectrum antibiotics should be given as scheduled throughout the surgical procedure.
Debridement
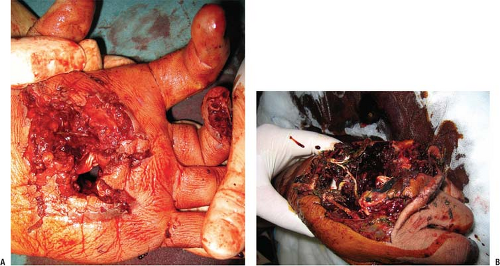
Successful surgical treatment of wounds begins with the meticulous and complete removal of foreign material, infection, and devitalized tissue to create a healthy wound bed (Fig. 2-2). In chronic wounds, we attempt to create an acute wound to promote healing. In acute injury, wounds must be extended past the zone of injury to ensure complete treatment, and failure to do so significantly limits the effectiveness of debridement. Judicious use of lavage may help remove foreign matter, but care must be taken not to extend the zone of contamination by forcing debris into the surrounding tissue. Use of a tourniquet early in the case is important to best visualize all contaminants and devitalized tissue and avoid injury to vital structures such as nerves and blood vessels. The tourniquet should be released prior to closure or dressing application to confirm removal of all devascularized tissue and excellent hemostasis.
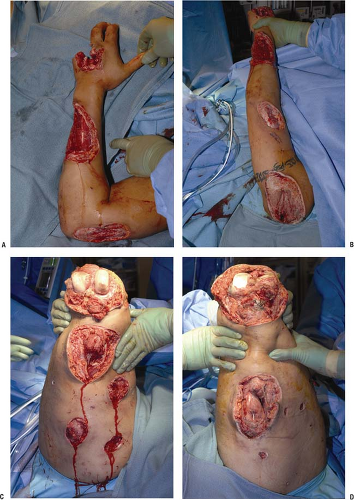
A systematic approach to wound debridement is required and sharp debridement is the cornerstone of this surgical technique. We prefer the centripetal approach working from superficial tissues to deep, from the margins to the center of the wound. Starting at the skin edges, we meticulously work towards the deeper structures within the wound (Fig. 2-3). In general, we prefer excision of all devitalized tissue to a healthy tissue margin instead of a “wait and see” approach to suspect tissue as we feel this limits persistent contamination and infection. All non-viable or suspect tissue is sharply debrided from the wound until a healthy margin of viable tissue achieved. Every effort to preserve nerves and blood vessels crossing the zone of injury is made, and if they are transected these structures are carefully tagged with dyed monofilament suture and documented in the operative records so that they may be more easily visualized during later wound debridements or reconstructive efforts.
Identification of non-viable tissue remains a challenge, and there is no substitute for experience. In general, non-bleeding skin that appears dusky or does not blanch should be excised, creating a smooth wound margin and avoiding the creation of a ragged skin edge that is difficult for subsequent skin grafting or closure. Subcutaneous fat should be soft and yellow; hard, dusky, or gray fat should be excised (Fig. 2-4). It is also important to keep this tissue moist during deeper debridement, as it will easily desiccate. Injured blood vessels or nerves must be carefully assessed for primary or delayed repair or grafting. Smaller sensory nerve branches may not be amenable to salvage, and if so, we like to pull traction on the proximal end, cut sharply, and allow retraction into the soft tissues. If the stump cannot be retracted, we make every effort to bury it in muscle. To the greatest extent possible local soft tissues should be used to cover exposed tendons, nerves, and vessels to prevent desiccation and further injury.
In debridement of muscle, fascia, and tendon, there are several important points to keep in mind. Muscle fascia should be stout, white, and shiny, while non-viable fascia will often appear grey or black, fragile, and stringy. When excising fascia, however, great care should be taken as neurovascular bundles may be in close proximity. Muscle should be red, shiny, of good consistency, contractile, and bleeding (Fig. 2-5). Anything to the contrary should be considered for debridement. Knowledge of anatomy and local blood supply is paramount in this endeavor as overly aggressive
debridement within muscle compartments may devascularize previously viable tissue. Tendon debridement must be carefully considered due to potential loss of function. Tendons are also easily desiccated, especially if overlying paratenon or sheath is missing.
debridement within muscle compartments may devascularize previously viable tissue. Tendon debridement must be carefully considered due to potential loss of function. Tendons are also easily desiccated, especially if overlying paratenon or sheath is missing.
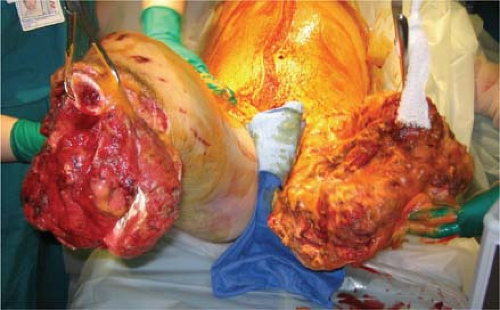
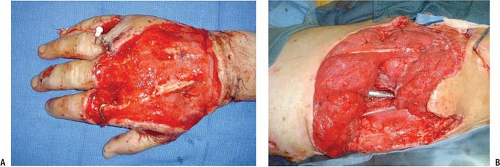 FIGURE 2-5 A: Right hand and (B) left hip open wounds ready for further coverage. Note the healthy, smooth skin margins, clean granulating tissue bed, minimal edema, and skeletal stabilization. |
Devascularized bone fragments must be removed from the wound bed, with the exception of substantial articular fragments, which should be retained in an attempt to preserve the articular surface (Fig. 2-6). Curettes, rongeurs, and burs are useful to check for punctated bleeding indicative of healthy bone that should be preserved. Cultures of any contaminated or osteolytic bone will help guide antibiotic selection.
There are many tools available for mechanical debridement. One tool we find useful for very large wounds is the VersaJet™ Hydrosurgery System (Smith and Nephew). This device uses negative pressure from a high-speed stream of water across a small aperture at the tip to remove softer tissue and surface debris by suction. Additional lavage is not required when using this device. However, great care must be used around neurovascular structures to avoid injury.
Strict hemostasis is critical to prevent hematoma and limit further infection and morbidity due to blood loss. Suture ligatures and surgical clips should be used for larger vessels, and bovie or bipolar cautery for smaller vessels. We avoid use of braided suture when possible to avoid harboring bacteria.




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree