Femoral Revision
Impaction Bone Grafting
Graham A. Gie
Key Points
• Provides restoration of bone stock loss
• Indicated in patients of any age, but particularly the younger group
Introduction
Impaction allografting for reconstruction of bone loss in revision total hip arthroplasty was initially developed for acetabular reconstruction. Experience from Professor Slooff and colleagues from Nijmegen, The Netherlands, who developed impaction bone grafting in the acetabulum in 1979,1 subsequently contributed toward the application of this technique on the femoral side.
Professor Robin Ling had initially impacted a femoral canal with milled bone (1985) and inserted a femoral component without cement that subsided significantly. To address this shortcoming, this technique was revised by using cemented femoral fixation, and the senior author performed the first case of a contemporary femoral revision with impaction bone grafting in Exeter in 1987. With the goal of achieving a stable reconstruction while restoring proximal femoral bone stock loss, this first case of cemented revision with impaction grafting was carried out using canal sizers as distal impactors and an oversized trial stem as the proximal impactor.
Ling and associates2 examined the quality of bone from a retrieved specimen 3.5 years post femoral impaction grafting, clearly showing cortical healing and a histologically regenerated cortical zone. As a result, in Exeter, this technique has become the procedure of choice in femoral revision surgery (Fig. 95-1).
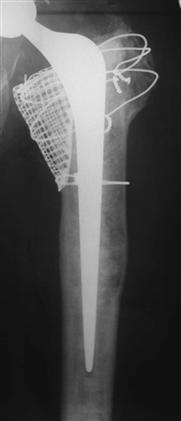
Figure 95-1 Femoral impaction grafting.
Indications/Contraindications
Preoperative Planning
Description of the Technique
Insertion of Intramedullary Plug
After removal of all debris, the femoral component, and cement, the femoral canal diameter is determined by the largest reamer used during débridement and is checked with a canal sizer (Fig. 95-3). An appropriately sized plug is then fixed to a threaded guide wire (Fig. 95-4) and is inserted down the canal using the revision plug introducer while the plug is positioned to the templated depth. This should be 2 cm distal to the tip of the stem, allowing for a short column of well-impacted graft chips distal to the prosthesis.
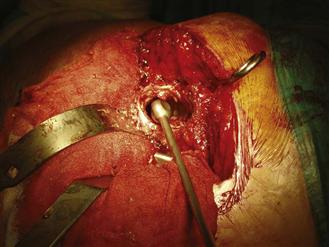
Figure 95-3 Checking femoral canal diameter with a canal sizer.
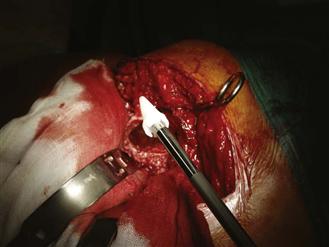
Figure 95-4 Intramedullary plug fixed to threaded guide wire with plug introducer attached.
Sizing of the Femoral Canal
A proximal femoral impactor (phantom) of the templated size, offset, and length is passed over the guide wire. Its shape is that of the definitive prosthesis, but it is oversized to allow for the cement mantle and centralizer (Fig. 95-5). If any resistance is felt, a smaller size should be selected. Before the distal impactors are used, it is important to determine the distance down the canal that each sizer can be passed without jamming in the canal. Driving an impactor distal to this level would cause a femoral fracture. Select a distal impactor one size smaller than the diameter of the plug used. This should pass easily down to the plug without resistance (Fig. 95-6). Withdraw the impactor 2 cm from this position, and mark the level against the tip of the greater trochanter with the plastic clip marker. This will allow for the 2-cm column of bone graft distal to the implant and will reduce the risk that the plug may be driven distally during vigorous impaction. Impactors of larger diameter are sequentially introduced over the guide wire as far down the canal as they will pass (Fig. 95-7) and are marked with a clip. In this way, the maximum depth of insertion allowed for each distal impactor is determined. With impacting bone graft, the impactors must not be driven beyond the marked depth.
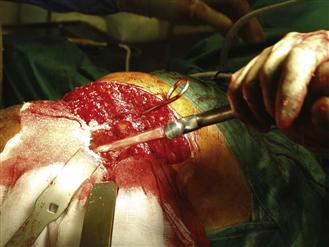
Figure 95-5 Proximal impactor (phantom) is passed over the guide wire, confirming adequate sizing.
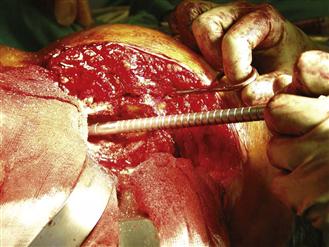
Figure 95-6 Canal sizer one size smaller than the plug diameter used was passed down the guide wire to the plug, and then was retrieved 2 cm for marking.
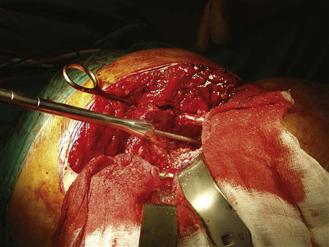
Figure 95-7 Distal impactor of larger diameter introduced over the guide wire as far down the canal as it will pass, and then marked.
Distal Impaction
Small cancellous bone chips (4 mm) are introduced into the canal using an open-ended syringe (Fig. 95-8). Before impaction is started, diaphyseal defects must be repaired with an appropriate wire mesh. Chips are then driven and compacted distally using distal impactors (Fig. 95-9) to the pre-rehearsed depth of the plastic markers. Progressively larger impactors are used as the canal is filled. More chips are firmly compacted until the impactors cannot be driven beyond the distal impaction line. For standard length stems, this line is the transition between polished and ridged sections of the impactors (Fig. 95-10). For longer stems, the distal impaction line is marked accordingly.
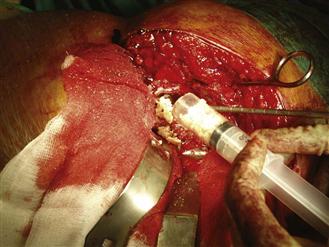
Figure 95-8 Small cancellous bone chips (4 mm) introduced into the canal using an open-ended syringe.
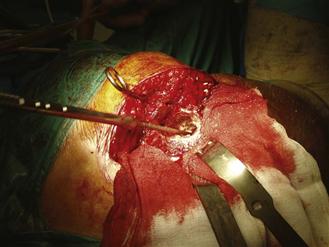
Figure 95-9 Chips driven distally using a distal impactor.
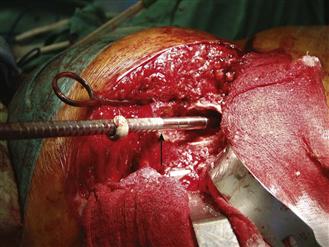
Figure 95-10 Distal impaction line for standard length stems (arrow) demonstrating the transition between polished and ridged sections of the impactors.
Proximal Impaction
The phantom is driven into the distally impacted bone (Fig. 95-11) and then is removed. More graft is pushed down the canal with handheld distal impactors and the phantom reinserted. The procedure is repeated until the phantom is stable enough to allow performance of a trial reduction, when hip stability and leg length can be assessed. The position of the phantom in relation to the proximal femur is marked with diathermy and methylene blue for reference at the time of cementing the stem (Fig. 95-12). The need for reconstruction of a calcar defect is reassessed at this stage, and it is indicated whether less than 1 cm of medial femoral neck is present above the level of the lesser trochanter, or if the most distal leg length mark of the phantom is seen well above cortical bone. The metal mesh is then fixed in position with cables or cerclage wires, avoiding multifilament cables for the most proximal section that will lie within the joint, to minimize the risk of fretting and release of metal debris. The impaction process is repeated until graft is firmly compacted up to within 1 or 2 cm of the top. At this stage, it should be impossible to withdraw the phantom by hand; it can be removed only with the use of the sliding hammer. It should also be impossible to produce any rotational movement of the phantom within the impacted graft. The following steps are the most important part of the procedure and determine the stability of the reconstruction, allowing for transmission of load into the proximal femur and ensuring that subsidence of the stem within the cement mantle is similar to that observed in primary hip arthroplasty. Using dedicated handheld block impactors and large cancellous chips (8 to 10 mm in size), the level of impacted graft is brought up to the top after firm impaction around the phantom (Fig. 95-13). To optimize proximal impaction, the phantom at this final stage should be backed out 1 or 2 cm so that more bone chips can be added; these are firmly impacted and the phantom driven to the correct depth, providing sound stability of the reconstruction. Calcar wires can be further tightened if necessary. The final consistency of the impacted chips should be that of cortical bone. Running out of bone graft material before completing proximal impaction will seriously affect the stability of the reconstruction.
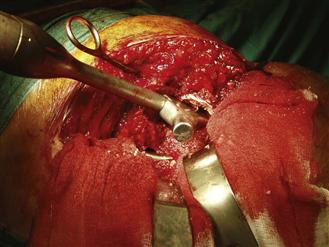
Figure 95-11 The phantom being sequentially driven into the distally impacted bone as more graft is pushed down the canal with handheld impactors.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree