Fig. 6.1
Friction bullae frequently occur on the heel
These bullae, which result from splits in the epidermis at the level of the stratum granulosum, occur most frequently on the feet and hands, but can occur at any site wherein the skin becomes rubbed repeatedly. Once a split in the epidermis develops, the space fills with fluid and a tense blister forms. These bullae can cause discomfort and may hinder further activity [1].
While the diagnosis is often straightforward, the management and prevention of these lesions present challenges. Research reveals that a blister, which is repeatedly lanced and drained three times in 1 day, heals more rapidly and less likely develops secondary infection [2]. The clinician should lance the blister in a focal spot and take great care to keep the blister roof intact. No commercially available dressing possesses the ideal coverage of the wound base as well as the athlete’s own skin.
Once lanced, the athlete should apply petroleum jelly and cover the area with an adherent dressing. Only rarely do these blisters become infected and require topical or oral antibiotics. Athletes can prevent bullae by essentially decreasing the friction between their skin and the sporting environment.
Simply wearing synthetic moisture-wicking clothing keeps the skin relatively dry and cool and minimizes the production of bullae. Athletes who are particularly prone to blisters may need to wear protective gloves or double layer of socks. Applying petroleum jelly to areas of the skin prior to athletic activity further minimizes the bullae production. Athletes must also ensure that their footwear fits well as ill-fitting equipment produces loose or tight spots that create friction bullae [1].
6.1.2 Athlete’s Toenail
Extreme athletes’ nails experience enormous pressure and tension as a result of their activities. Abrupt and intense forces can completely remove a finger or toenail. More commonly, athletes develop nail changes related to chronic, low-grade pressure, and tugging. The changes related to these physical forces include longitudinal and transverse ridging, onycholysis (separation of the nail plate from the nail bed), discoloration around the periungual area, and calluses periungually (Fig. 6.2) [1, 3].
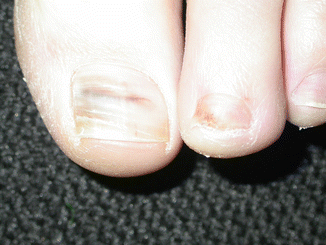

Fig. 6.2
Athlete’s nail demonstrates periungual change and transverse ridging and hemorrhage
Extreme athletes must employ several techniques to prevent athlete’s nail. All nails should be closely cut in a straight-across fashion that allows an equal distribution of the force created during the athlete’s physical activity. Cutting nails in a curved manner places increase pressure on the middle portion of the nail. As the sport allows, wearing gloves also helps to reduce the friction and pressure experienced by fingernails. Extreme athletes need to ensure that their footwear has an adequate toe box [1]. Unique lacing techniques can also redistribute the physical forces away from the toenails and onto the ankle which is better suited to experience the forces that create long-term nail changes. To employ this lacing method, the athlete undoes both laces from the last eyelet; instead of crossing the lace into the opposite side’s eyelet, one enters the eyelet on the same side such that two loops are generated. The free lace ends then are crossed and thread through the opposite loop. Then the athlete can tie the ends as usual [4].
6.1.3 Talon Noire
The significance of talon noire resides in the fact that this condition can confuse the clinician to believe that the athlete has warts or melanoma. Talon noire, otherwise known as black heel, occurs most commonly in younger athletes on the posterior lateral or medial heel (Fig. 6.3) [1]. Caused by friction with subsequent hemorrhage into the skin, talon noire is asymptomatic and requires no therapy [5].
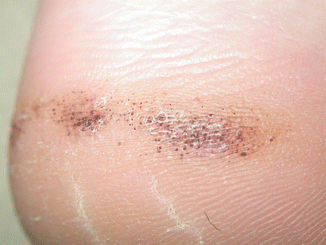

Fig. 6.3
This heel illustrates talon noire which can easily be confused with verruca (warts)
6.1.4 Piezogenic Pedal Papules
In addition to friction, pressure can also create havoc in an extreme athlete’s skin. Piezogenic pedal papules primarily affect the feet of young women, and while most often not painful, the discomfort associated with the condition can prevent the endeavors on the extreme athlete. The subcutaneous fat and associated nerves and microvasculature protrude up into the dermis that can cause strangulation and subsequent pain [1]. Clinicians may misdiagnose the foot pain and embark on an extensive musculoskeletal work-up without having the athlete stand on only the affected extremity that then readily reveals the skin colored to yellow papules most often on the sides of the heel. Multiple therapies exist including intralesional steroids [6], compression [7], and acupuncture [8]. Susceptible athletes sometimes find heel pads prevent piezogenic pedal papules.
6.1.5 Athlete’s Nodules
A combination of pressure and friction, particularly along the lower extremities, can cause a skin condition called athlete’ nodules. Two mechanisms exist by which athletes can develop these lesions. First, surfers get “surfer’s knots or nodules” on their legs as a result of pressure, friction, and rough board surface (along with sand) [9]. As surfers paddle out to catch waves (especially those in colder waters), they kneel on the board, and the combination of these factors and forces creates a foreign-body reaction in the skin. Second, these nodules can develop as a reaction to constant pressure in one particular location that most often related to protective equipment or shoewear. As a result, the dermis hypertrophies creating a collagenoma.
Regardless of the exact etiology, the differential diagnosis of these firms, skin colored to erythematous nodules can be vast. Atypical mycobacterial and deep fungal skin infections have this appearance, as do inflammatory conditions such as granuloma annulare and rheumatoid nodules. Primary and secondary malignancies can also share a similar morphology. While a biopsy will differentiate among these various cutaneous ailments, linking the lesion to one’s athletic pursuits facilitates early accurate diagnosis.
Athlete’s nodules may require excision, while others respond to intralesional steroids. Occasionally changing the equipment or footwear results in clearance. To prevent athlete’s nodules, extreme athletes can wear padding between their skin and the offending piece of equipment [10]. In the case of surfer’s knots, surfers may lie prone on the board to equally distribute forces along the board. Surfers, in colder waters, may wear a wet suit to comfortably allow a prone position.
6.1.6 Sunburns and Actinic Damage
Extreme athletes experience an enormously high level of ultraviolet radiation (UVR). As a result, these athletes ultimately risk acquiring skin cancer and actinic damage (wrinkles and dyspigmentation) (Figs. 6.4 and 6.5).
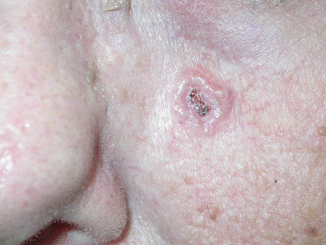
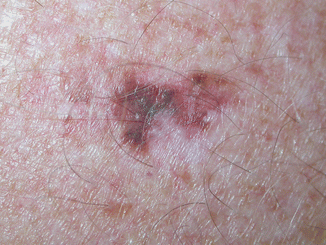

Fig. 6.4
Long-term, extreme athletes risk developing basal cell carcinoma. This photo depicts the characteristic pearly border and telangiectasias

Fig. 6.5
Extreme athletes’ skin endures enormous ultraviolet light that ultimately can create malignant melanoma
Several factors result in this intense UVR exposure. Athletes practice and compete during the time of peak UVR that is between 10 am and 4 pm. Additionally, they train for long periods of time and started this training often early in their life resulting in an immense total lifetime exposure. Sweating, inherent to most extreme sports, enhances the potency of the UVR such that it takes 40 % less UVR to burn athletes if they did not sweat [11]. Several extreme sports exist at very high altitudes. At high altitudes, the atmosphere has not had a chance to filter a significant portion of UVR. For example, the UVR experienced high in the mountains is comparable to the UVR affecting an individual at sea level [12]. Lastly, extreme athletes who compete in snow and water environments must also contend with the significant reflection of UVR off the surfaces. Wearing hats that shade the face will provide no protection against UVR reflecting up to the athletes’ face from the environment.
To prevent sunburns and long-term actinic damage, athletes must apply water- and sweat-resistant sunscreen and reapply the lotion or spray after practicing or competing. They should take care to apply areas that athletes often forget which include the ears and any part created by hairstyles. If possible, athletes should avoid the peak hours of UVR exposure and practice early morning or evening. Tightly woven and dark clothing provides ideal sunblocking properties. While athletes traditionally prefer light-colored clothing to keep them relatively cool, the myriad commercially available synthetic moisture-wicking clothing allows the athlete to wear a sporting garment with both excellent UVR-blocking capabilities and good cooling qualities [1].
6.1.7 Miliaria Crystallina
Exposure to extraordinary heat and UVR plays a major role in many extreme sports. One relatively rare cutaneous condition that may occur more often in this population is miliaria crystallina. An affected athlete will develop delicate, crystal-like, small vesicles on their skin; unsuspecting clinicians may misdiagnose the lesions as herpes or another skin infection (Fig. 6.6).
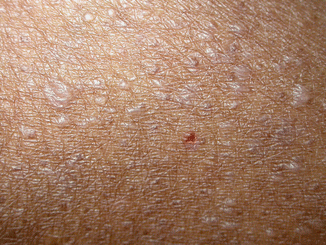

Fig. 6.6
The tiny blisters of miliaria crystallina are extremely fragile and rupture easily
Miliaria crystallina, which results from superficial obstruction of the eccrine duct, highlights the fierce heat that challenges the athlete. Wearing moisture-wicking, dark-colored synthetic clothing will assuage some of the affect of the heat [1].
6.1.8 Frostbite
While heat can cause many ailments in an athlete’s skin, cold exposure poses its own challenges. Prolonged exposure to cold can cause significant damage to the cutaneous structures. Wind and moisture can exacerbate the issue. An extreme athlete with frostbite will initially complain of pain and develop erythema on the toes and fingers; as the condition progresses, necrosis ensues. To treat frostbite, clinicians should rapidly rewarm the area by dunking in 40 °C water [13]. This treatment should only occur if no chance of subsequent exposure to prolonged cold remains. Rewarming frostbitten skin and subsequently refreezing that skin result in maximal tissue damage. Extreme athletes whose environment includes freezing temperatures must use thermal clothing and gloves and chemical heating packets [1, 13].
6.1.9 Jellyfish Envenomations
While uncommon overall, extreme athletes risk encounters with water creatures that can affect their skin. Water-based extreme athletes may experience painful jellyfish stings from their long tentacles. Once the tentacles contact the skin, nematocysts fire and cause a linear, erythematous, and edematous eruption. Treatment includes removing the tentacles with tweezers and applying vinegar solution. Athletes and clinicians should avoid applying freshwater that can activate the nematocysts [1]. Extreme athletes who wish to enter seawater with jellyfish should minimize skin exposure by wearing wet suits as their sport allows.
6.2 Allergic Skin Reactions
Among the most common cutaneous ailments in extreme athletes, after traumatic skin events result from allergies. The main categories of allergy include allergic contact dermatitis, exercise-induced anaphylaxis, and urticaria.
6.2.1 Allergic Contact Dermatitis
In their sporting pursuits, extreme athletes can develop allergies to the various pieces of equipment necessary for their activity. Protective equipment commonly causes allergic contact dermatitis. Shin pads may contain urea formaldehyde and helmets may possess epoxy resins. Extreme athletes who contact tape containing formaldehyde resins or analgesic creams containing eucalyptus can also develop contact dermatitis [14]. Injured or pruritic athletes often reach for Benadryl spray which can create an allergic contact dermatitis.
Sensitized athletes will develop well-defined, erythematous, scaling eruption in a distribution corresponding to the area of equipment contact (Fig. 6.7).
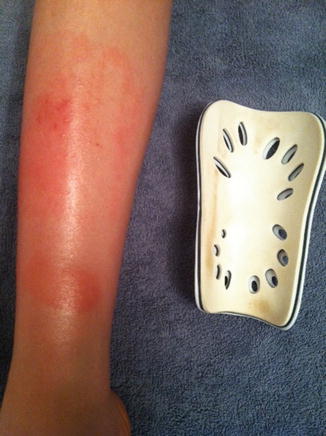

Fig. 6.7
Eruptions with a linear arrangement strongly suggest an allergic contact dermatitis
Acute dermatitis will demonstrate small blisters (vesicles), whereas subacute dermatitis will lack vesicles and instead often display more scale and less erythema.
Allergic contact dermatitis responds well to topical steroids. Affected areas on the trunk, extremities, and scalp respond well to potent (class I) topical steroids. Athletes should use caution with topical steroids on the face (especially the eyelids), groin, and axilla. The latter two areas will experience occlusion, which enhance the potency of topical steroids. In this instance, potent topical steroids may more readily cause side effects that include hypopigmentation, skin thinning, erosions, and acquisition of telangiectasias. Sensitive areas such as these require no more than medium-potency topical steroids such as triamcinolone 0.1 % twice daily; low-potency topical steroids such as hydrocortisone 2.5 % twice daily most often will be effective. When athletes need to chronically use topical steroids for their dermatitis in the groin, axilla, or face, the clinician should consider using topical pimecrolimus or tacrolimus. These agents do not possess the potential to cause the side effects aforementioned [1].
To help prevent contact dermatitis, susceptible extreme athletes can use silicone helmets (instead of those containing epoxy resins). Placing a moisture-wicking barrier between the protective pads and the skin not only will provide a barrier between the pad and the skin but also will wick away moisture that would otherwise enhance leaching of the offending allergen from the equipment. Allergic athletes may use acrylate tape to help avoid dermatitis (Table 6.1).
Table 6.1
Cutaneous allergy in athletes
Sports equipment | Offending agent | Location of eruption | Nonallergenic options |
|---|---|---|---|
Analgesic cream | Eucalyptus | Focal | Hot/cold packs |
Athletic tape | Formaldehyde resins | Focal | Acrylate tape |
Helmets | Epoxy resins | Forehead, scalp | Silicone |
Sailing wishbone | Thiorams | Hands | Aluminum |
Shin pads | Urea formaldehyde | Shins | Synthetic padding at interface |
6.2.2 Urticaria
Another somewhat common allergic skin reaction in athletes is the general entity of urticaria. Extreme athletes risk developing three types of urticaria: cholinergic, solar, and cold. While each condition culminates in pruritic, edematous, well-defined, effervescent papules and plaques, the etiologies and morphology differ among the three ailments. Cholinergic urticarias present as small wheals and result from an increase in an athlete’s core body temperature; runners seem particularly prone. Cold urticaria occurs in athletes participating in winter or cold-water activities, and solar urticaria abruptly occurs (within minutes) after exposure to ultraviolet radiation. The ice cube test confirms the diagnosis of cold urticaria. An ice cube is placed on the athlete’s skin, and after removal and the skin warms, a welt develops where the ice cube rested. Phototesting confirms the diagnosis of solar urticarial [1].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








