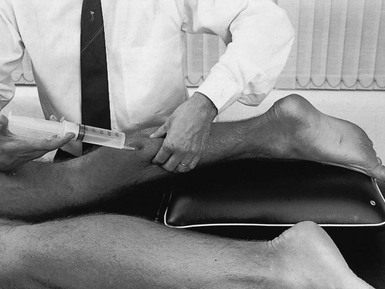
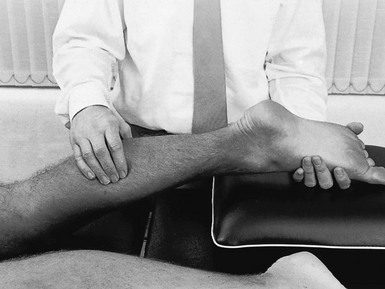
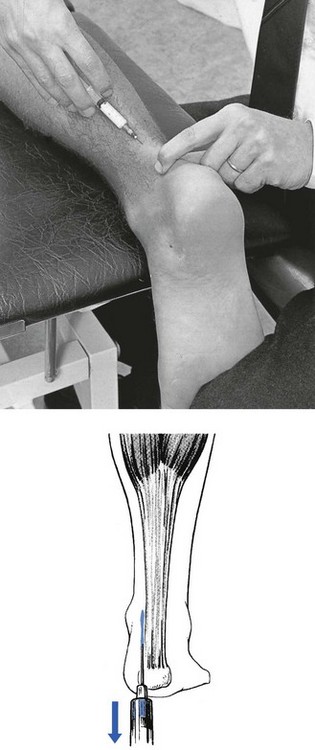
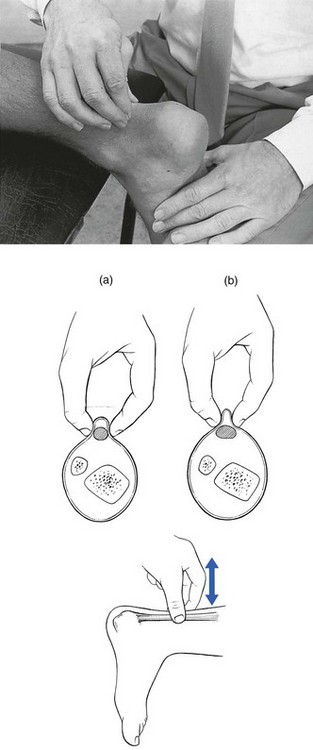
57 Children between the ages of 6 and 11 years who complain of diffuse pain in the legs but have a normal clinical examination are very often regarded as suffering from ‘growing pains’. Paediatricians’ estimates of the frequency of this diagnosis vary from 4%1 to 20%2 of all children. During recent decades, several hypotheses have been put forward but none gives a good explanation for the symptoms. As it occurs between the ages of 6 and 12, which is not the period of maximum rate of growth, ‘growing’ cannot be the real reason for the pain. Whatever the origin of the pain, it disappears spontaneously and completely after the age of 12 years.3,4 This is the common term to describe a tear in the triceps. It occurs most often in the medial belly of the gastrocnemius muscle, usually some 5 cm above the musculotendinous junction.5 The disorder was first described by Hood in 1884.6 For decades it has been regarded as a ruptured plantaris tendon,7,8 but careful clinical examination of patients suffering from this disorder shows this to be false.9 Examination reveals pain during resisted plantiflexion but no weakness. In the supine-lying position, dorsiflexion at the ankle is found to be markedly limited when the knee is in the extended position but becomes normal when the knee is flexed. This implicates the gastrocnemius muscle, part of which is in spasm around the tear. The difference in range between a flexed and an extended knee in a disorder of the gastrocnemius muscle is another example of the constant-length phenomenon. Palpation of the calf reveals the tender area in the medial gastrocnemius, with either swelling and haematoma if the lesion is recent, or induration around the tear if it is old. After a severe rupture, it is possible to palpate the gap in the medial gastrocnemius. Ultrasonography is the imaging technique of choice to demonstrate size and grade of the lesion.10,11 Although the diagnosis is obvious, it is as well to bear in mind some other possibilities. Although the similar onset and localization of the pain can cause diagnostic confusion, this condition should hardly be a problem if a proper clinical examination is done. Weak resisted plantiflexion and no spasm during passive dorsiflexion in a ruptured Achilles tendon contrast with the findings in tennis leg.12,13 If there is any doubt, a simple test can be done as follows.14 The patient lies prone, the foot hanging over the edge of the couch. The examiner squeezes the calf muscles. If the Achilles tendon is intact, the foot moves into plantar flexion. When there is total rupture, no movement results. Differential diagnosis from this condition is very important. Instances have been described of patients with tennis leg receiving anticoagulants, which aggravated their condition.15 The main historical difference is in the onset. In deep venous thrombosis, pain appears after immobilization or after sitting for a couple of hours,16 and not during vigorous contraction of the calf muscles. Clinical examination does not show limited passive dorsiflexion, although passive dorsiflexion and resisted plantiflexion can be painful. The calf muscle and leg are swollen and the foot becomes oedematous because of obstruction to venous return. Palpation of the tender spot shows other differences: in thrombosis the whole calf muscle is painful to the touch and sometimes a painful ‘string’ can be palpated deep within it.17,18 In long-standing rheumatoid arthritis of the knee, chronic distension with fluid can weaken the posterior ligaments and during exertion these can rupture. Sudden pain in the knee, followed by swelling of the leg and oedema of the ankle, strongly suggests venous thrombosis.19 Here, the long-standing rheumatoid arthritis and the absence of injury suggest the diagnosis, which can be confirmed by arthrography. The patient, usually a young man, reports an ache and swelling in the calf some hours after unaccustomed exercise. Walking is uncomfortable and increases the swelling. Examination shows that rising on tiptoe is not difficult and not really uncomfortable. The calf is diffusely swollen and the skin is red and warm to the touch. Passive dorsiflexion of the foot is severely limited by loss of elasticity of the calf muscles. Palpation reveals uniform tenderness of the whole calf muscle without any localized tender area.20 The symptoms result from muscle ischaemia, produced by increased tissue fluid pressure in the closed fascial compartment. The difference from tennis leg lies in the discrepancy between marked restriction of passive dorsiflexion and almost painless tiptoe rising. Treatment is surgical division of the deep fascia. Different types of treatment have been advocated for tennis leg. Most authorities advise partial or total immobilization for small tears21 and surgical suture for serious ruptures.22,23 In our opinion, surgery for this condition is scarcely ever necessary and partial or total immobilization by plaster cast or strapping is obsolete. When such treatment is instituted, the formation of a chronic adherent scar is promoted, which results in disability lasting several months. The aim of treatment in muscle tears is to allow the torn fibres to heal in such a way that mobile and functional scar tissue is formed. If normal enlargement of the muscle is impaired by adhesions, self-perpetuating inflammation will be the result. Muscle belly lesions (tennis leg is an excellent example) therefore need a different and more functional approach. The aim must be to restore normal movement in the damaged muscle as quickly as possible. This can be achieved with combined treatment: early compression to decrease the amount of haemorrhage; aspiration and infiltration with local anaesthetic as soon as the patient is seen; and deep transverse friction and electrically stimulated or active contractions of the muscle during the next few days.24 During the recovery period, the muscle must be protected by a raised heel pad, which enables the patient to use the unaffected parts of the gastrocnemius without strain on the line of healing. As soon as the patient is seen – whether on the day of the accident or some weeks or months later – local anaesthesia is induced at the site of the partial rupture. The patient lies prone, the knee slightly bent and the foot plantiflexed, to allow maximal relaxation of the muscle. The tender spot is located and gripped between thumb and index finger (Fig. 57.1). If there is any fluctuation, an attempt is made to aspirate the haematoma. Once that has been done, 30–50 mL of procaine 0.5% is injected using the usual infiltration techniques. As the spot is never precisely localized (gentle pressure does not reveal tenderness in the deeper part of the muscle, whereas strong pressure is apt to hurt throughout the belly) and the gastrocnemius muscle is a large structure, up to 50 mL of a 0.5% solution may be required. The patient lies prone with the foot fully plantiflexed. The therapist sits at the level of the patient’s leg. The fingers are placed at one side of the affected area and the thumb is positioned at the opposite side of the leg so as to apply counterpressure. The other hand may reinforce the palpating one (Fig. 57.2). Transverse friction starts deeply. By drawing the fingers upwards over the affected area, the therapist feels the muscle fibres escape from the grip until only skin and subcutaneous tissue remain. In the second stage, the fingers are slightly relaxed and moved backwards into the previous deep position, where the same movement starts again. The procedure is continued for about 15 minutes. During friction, the fingers do not move in relation to the skin – fingers and skin move as a unit over the muscle fibres. The diagnosis and treatment of tennis leg is summarized in Box 57.1. The terminology used to describe this painful condition of the Achilles tendon is very confusing and terms such as Achilles tendinitis, tendonitis and tendinopathy have been widely used. In this book we use the term tendinopathy as the general clinical label for the combination of tendon pain, swelling and impaired performance. Peritendinitis and tendinosis are the histopathological entities of the disease.25 Achilles tendon problems are very common among athletes as well as the general population.1,2 Tendinitis of the Achilles tendon is chiefly a runner’s problem.26 Non-sporting people can also suffer from this condition and it then starts after unaccustomed exertion or a long walk in inappropriate shoes. Nevertheless, it most often occurs in long-distance runners, and it comes as no surprise that the increase in the number of people running during the past few decades has been paralleled by an increase in the number of cases of inflamed Achilles tendon.27,28 In a survey of 2002 running injuries seen over a 10-year period at a sports medicine referral clinic, overuse injury to the Achilles tendon was the sixth most common injury.29 The lifetime cumulative incidence of Achilles tendinosis is 5.9% among sedentary people and 50% among elite endurance athletes.30 The site of the lesion lies usually at mid-tendon. Occasionally, the strain occurs level with the upper border of the calcaneus or, very rarely, at the musculotendinous junction. Achilles tendinitis is multifactorial and usually the outcome of a combination of anatomical and biomechanical characteristics, along with poor training technique.31 The most important aetiological factors are short triceps (decreased touchdown angle), poor stretching habits and increased plantar flexion peak torque.32,33 Some authors suggest that there might also be a vascular factor furthering the condition.34,35 This would explain the usual location of the lesion at mid-tendon, which is the junction of its two vascular systems.36,37 During the last decade, fluoroquinolone antibiotics have been implicated in the aetiology of Achilles tendinitis and subsequent tendon rupture.38–41 The history in Achilles tendinitis is quite simple.42 The patient states that the heel aches during or after walking or running (stage I). Sometimes there is pain at the beginning of exertion, improving after a while and reappearing on fatigue (stage II). Alternatively, there is continuous and worsening pain during exercise (stage III). Sometimes the pain does not cease after exertion but continues at rest (stage IV). As a rule, however, pain eases at rest and increases on running or walking. Nocturnal pain is absent. Because we advocate deep transverse friction as the most effective conservative treatment for this disorder and massage only acts where it is applied, the tendon should be palpated very carefully to discover all the tender areas because there may be more than one. The lesion nearly always lies at the inner or outer aspect, or both, of the tendon. Very often, the anterior surface is affected but almost never the posterior.43 Most of the lesions lie 2–6 cm above the tenoperiosteal junction.44 The morphological and macroscopic changes in the condition are not always the same. Observations during surgery have led to the description of two separate histopathological types: • Peritendinitis: the inflammatory changes are confined to the peritenon, which is thickened and shows inflammatory changes, with considerable connective tissue proliferation and adhesions between peritendineum and tendon.45,46 • Tendinosis: this is characterized by inflammatory and degenerative changes in the tendon tissue itself.47,48 Sometimes partial ruptures of deeply situated fibres can be seen, with the superficial parts of the tendon remaining intact. Here there is a visible and palpable enlargement at the tendon from the structural changes of chronic fibrosis.49 Ultrasonography has been used increasingly to examine Achilles tendon injuries. It is a quick, safe and inexpensive method to verify the existence and location of intratendinous lesions but is operator-dependent.50,51 Magnetic resonance imaging (MRI) is useful in visualizing pathological conditions of the tendon but is expensive and time-consuming. It is unwise, however, to rely solely on the results of these imaging techniques. First of all, the normal anatomy of an asymptomatic Achilles tendon may vary, which causes diagnostic misinterpretation.52 Secondly, several studies have reported intratendinous changes in up to 34% of cadaver specimens, in ultrasound and MRI images of patients without symptoms.53–55 There are a number of approaches. Initial conservative treatment should be directed towards preventing adhesion formation between tendon and paratenon. Cold packs and stretching comprise most of the treatments proposed in the recent literature and may produce some benefit. Cold therapy is able to control pain and oedema, as well as to reduce regional blood flow and the metabolic demands of the tissue, and thereby helps to prevent further tissue damage at the site of injury. Passive stretching of the Achilles tendon has been advocated as restoring normal ankle joint mobility and decreasing the strain of the Achilles tendon with normal motion.56 The role of corticosteroid injections in the treatment of Achilles tendinopathy is controversial.57–61 Several reports demonstrate disappointing results and injections have also been blamed for causing spontaneous rupture of the Achilles tendon.62 However, localized paratendinous infiltrations with small doses of triamcinolone (10–20 mg) still have a place in the treatment of Achilles tendinopathy, provided the correct technique is used. The injection is never made into the body of the tendon but along the surface, between tendon and peritendineum. After the injection, the patient should avoid all exercise during the first 10 days, after which a training programme can gradually be resumed. The injection can be repeated once if there is no cure after 2 weeks. If this procedure is followed and the correct technique is used, as set out below, postinfiltration ruptures are not to be feared.63 The patient lies prone on the couch. The foot is forced into dorsiflexion over the edge of the couch. This stretches the tendon, which facilitates palpation of the affected area. A 2 mL syringe is filled with 20 mg triamcinolone. A 5 cm needle is fitted and introduced some 3 cm away from the lesion. It is pushed through the skin and moved either upwards or downwards, parallel to the tendon, until the tip reaches the distal edge of the lesion. A small injection is given while the needle is drawn back along the surface of the tendon (Fig. 57.3); the manœuvre is repeated four or five times, each time a little to one side of the previous infiltration line. If the tip of the needle stays superficial to the tendon, no particular resistance to the plunger will be felt during the injection. Recently, promising results have been described in studies of patients with Achilles tendinopathy who were treated with paratendinous injections of a sclerosing agent. On ultrasonography, neovascularization and tendon inhomogeneity decreased significantly as the clinical parameters improved.64–66 In simple peritendinitis, the crural fascia and the paratenon are split longitudinally from the musculotendinous junction to the insertion on the calcaneus, and adhesions between the tendon and the sheath are released.67 In cases with focal tendinosis and partial rupture of the tendon, the diseased area of the tendon is excised and the tendon repaired by side-to-side suture of the remaining tendinous fibres.68 Where excision of the degenerated tissue disrupts the continuity of the tendon, the tendon is reconstructed and reinforced with the fascia of the gastrocnemius.69 If there is extensive tendinitis, excessive scar tissue is excised.70 Some authors claim better results if carbon fibres are implanted between the tendinous straps.71 This was introduced more than 40 years ago by Cyriax74 and is, in our opinion, the best conservative treatment for the condition, provided it is given correctly: (a) at the right point, (b) with a good friction technique, (c) 20 minutes per session and (d) at regular intervals (three times a week). During the period of treatment, the patient must take relative rest. Technique: friction to the medial and lateral edge of the tendon The patient lies face downwards on a low couch, with the foot projecting just beyond the edge of the couch. The therapist sits at the foot and pushes the sole into dorsiflexion through a slight pressure of the contralateral knee. At the correct point the tendon is grasped between finger and thumb, or two fingers and thumb, depending on the extent of the lesion (‘a’ in Fig. 57.4). Slight pressure under the tendon is exerted and the hand is drawn upwards until the fingers slip towards the posterior aspect of the tendon (‘b’ in Fig. 57.4). In the final stage of this manœuvre, only skin remains between the two grasping fingers. The pressure is now released slightly and the fingers are pushed downwards until they lie at the starting position (‘a’) and the whole procedure can be repeated. The cycle is repeated for about 15 minutes. Technique: friction to the anterior part of the tendon This localization should always be sought in addition to other tender spots. Once again, friction is given in two phases. First, the fingertip is placed deeply under the tendon with the forearm in a slightly pronated position (‘a’ in Fig. 57.5). Pressure is exerted in a dorsal and medial direction; meanwhile, the arm moves in full supination, until the lateral fibres escape under the fingertip (‘b’ in Fig. 57.5). Caution is taken not to move the finger on the skin but rather to move the skin and the fingertip as a whole. Now pressure is slightly released and the fingertips replaced in the former position (‘a’), so that the whole procedure can be repeated. The to-and-fro movements are performed for 15 minutes. The fingers must not be allowed to glide on the skin, to avoid the formation of a blister. Technique: friction to the tenoperiosteal insertion of the tendon The tendon is compressed between the therapist’s fingers and the upper surface of the calcaneus. Using both hands, a circle is made round the heel with one index finger, reinforced by the other, at the lesion. Both thumbs cross at the plantar surface. Pressing downwards squeezes the tendon between the fingers and the calcaneus. Deep friction is performed by moving the forearms in opposite directions. The amplitude of the movement must be large enough to reach the whole width of the tendon (Fig. 57.6). Recently, there has been increasing interest in the use of eccentric loading in treatment of chronic Achilles tendinopathy. (In an eccentric contraction, the muscle–tendon unit lengthens as a load is applied to it.) In 1986 Stanish et al75 reported that a once-daily, 6-week eccentric loading programme led to complete relief of pain in 44% and a marked improvement in symptoms in a further 43% of patients. More recently, others have confirmed the efficacy of eccentric loading for mid-substance lesions of the Achilles tendon,76,77 and high success rates (at least 60% either good or excellent) have also been reported in prospective randomized trials.78–80 However, the mechanism for the efficacy of eccentric loading remains unknown.81 Raised heels, shock-absorbing heels and correction of a valgus deformity are usually prescribed.82 As the triceps is also a slight invertor, a valgus deformity must always be corrected to relieve excessive strain on the tendon.83 Although these measures are certainly beneficial, it is important to remember that they are prescribed for prevention only because they do not lead to substantial and histological changes at the site of adhesions. Many authors pay a great deal of attention to the preventive value of stretching exercises before running.84,85 Although they may have such value, the worth of stretching techniques alone should not be overestimated when they are used as therapy in actual lesions. Stretching is a good method of prevention but, in our experience, has no therapeutic value. In these conditions, the contrast between the mild symptoms and the marked signs is striking. It is also important to remember that gout can sometimes affect the Achilles tendon. The main complaint is not, as in tendinitis, pain during contraction of the triceps but pain during local pressure, e.g. catching the heel against the edge of the shoe. Examination shows that rising on tiptoe is indeed just uncomfortable rather than painful but the tendon is warm, swollen and very tender to the touch.86,87 Local treatment consists of infiltration with 20 mg of triamcinolone between the sheath and the tendon. The technique is the same as described for Achilles tendinitis. Apophysitis of the calcaneus (Sever’s disease, Osgood’s disease) occurs in boys between 6 and 12 years of age and is often bilateral. The disorder has been classified among the general osteochondrosis syndromes, such as Legg–Calvé–Perthes disease at the hip or Osgood–Schlatter disease at the tibial tuberosity. The child complains of sharp pain in the heel, occurring during contraction of the triceps. The pain starts suddenly, can last a couple of hours or days, and may disappear and reappear. Rising on tiptoe can be negative but the bone is usually tender to the touch. The radiological appearances are characteristic – ‘slight fragmentation of the apophysis’ – and confirm the diagnosis. Spontaneous recovery occurs in a year or two, often with the development of a slight permanent prominence on the posterior aspect of the calcaneus.88 There is no treatment except relative rest, slightly raising the heel and inserting shock-absorbing heel pads in the shoe.89 Weakness of the plantiflexor mechanism is detected by an inability to rise on tiptoe. Apart from neurological lesions, which are discussed at the end of this chapter, the commonest cause of weakness is a rupture of the Achilles tendon, most frequent in athletes over 30 years of age.90 The tear lies in the ‘critical zone of poor vascularization’, which is 2–6 cm above the calcaneal insertion.91 It is surprising that this simple and easy-to-detect condition very often remains undiagnosed for a time. Between 30 and 41% of Achilles tendon ruptures remain undiagnosed for more than 2 weeks.35,92,93 When the patient lies on the couch, the clinical examination reveals little. There is usually no haematoma or visible thickening. Passive movements are painless. An alert examiner will probably detect an excessive range of dorsiflexion. In the supine, non-weight-bearing position, resisted plantiflexion remains possible because the plantaris, flexor hallucis longus and flexor digitorum muscles still contract. Rising on tiptoe, however, immediately reveals the diagnosis. The squeeze test is also positive: the patient lies prone, with both feet suspended over the edge of the couch; compressing the triceps surae causes plantiflexion of the foot when the tendon is intact but not when it is ruptured.14 There is still controversy concerning the best treatment for Achilles tendon ruptures. It appears that a satisfactory outcome may be achieved with either non-operative or operative treatment but surgical repair appears to provide better functional capacity94 with better scores of strength, power and endurance95–97 and lower re-rupture rates. The advantages of the conservative approach are that there are no risks of anaesthesia, infection, skin adhesions and sural nerve injury.98,99 Reports in the literature indicate that in active, young, very demanding individuals, surgical repair should be considered, with non-surgical treatment reserved for elderly or sedentary patients.100–102 However, conservative treatment can also be considered in athletically active patients, as treatment should always be individualized to the concerns and health of the patient.103,104
Disorders of the lower leg
Bone disorders
Lesions of the plantiflexors
Pain
Tennis leg
Differential diagnosis
High rupture of the Achilles tendon
Deep venous thrombosis in the calf muscles
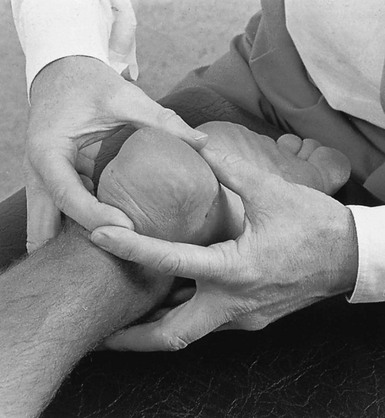
Rupture of a Baker’s cyst
Posterior compartment syndrome
Treatment
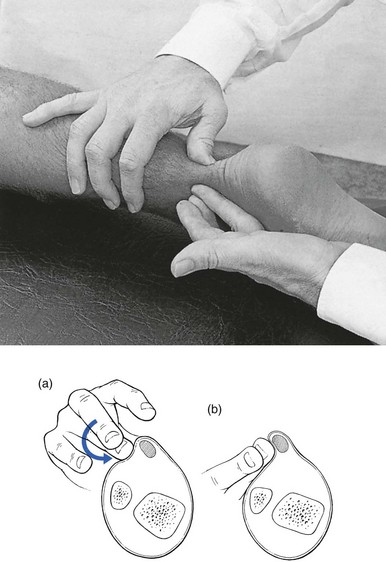
Technique: infiltration
Technique: friction and electrical contractions
Achilles tendinopathy
Imaging methods
Treatment
Steroid injection
Prolotherapy
Surgery
Deep friction to the Achilles tendon
![]()
![]()
![]()
Eccentric training
Prevention
Achilles tenovaginitis
Rheumatoid arthritis and ankylosing spondylitis
Calcaneus apophysitis
Weakness
Treatment
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Disorders of the lower leg