Digital and Sesamoid Fractures
Michael S. Downey
Gretchen A. Lawrence
Digital and sesamoid fractures are common injuries affecting patients in all age groups and activity levels, including those who are sedentary. In most circumstances, the fractures are amenable to conservative treatment and generally do not pose a problem. However, many patients who have sustained a digital or sesamoid fracture do not seek timely care for their injury. Inadvertently, these patients convert what would otherwise be a simple, inconvenient setback into a more difficult to treat and complex problem, often prolonging or impairing their full recovery. A certain mindset or misconception exists among many lay people that there is really no specific treatment for digital fractures or “if the toe can move it is not broken,” and this attitude likely contributes to the delay between injury and seeking treatment.
Significant fractures can affect the toes and sesamoids, and may require more prompt attention, particularly if dislocation or displacement occurs or if the fracture is intra-articular or open. In most injuries of this nature, deformity is obvious, and patients tend to seek treatment quickly.
DIGITAL FRACTURES
Fractures of the toes are the most common injury of the forefoot seen in emergency rooms, with a reported incidence of 140 cases per 100,000 population per year and with a male to female ratio of 1.6:1 (1,2 and 3). As with any injury, the pathologic forces that cause digital fractures may be directed in any one or a combination of the cardinal body planes. Although most injuries involve a combination of these forces, a predominant plane of force can often be identified. Certain fracture patterns are more frequently observed and can be related to these injury mechanisms. Understanding the predominant plane of injury facilitates the closed or open reduction, realignment, and treatment of digital fractures.
SAGITTAL PLANE
Injury occurring in the sagittal plane and resulting from direct trauma, hyperextension, or hyperflexion of the involved digit is the cause of most digital fractures. Sagittal plane crushing is the most frequent mechanism of injury associated with a fractured hallux. Crush injuries are most often caused by a heavy object, which may be dropped or may fall, or by industrial or motor vehicle accidents. A subungual hematoma is often a component of the injury, and these can require evacuation ranging from dorsal drainage through a pinhole created in the nail plate to total nail avulsion. Protocols for care of the nail injury can be found in Chapter 99. The digital fractures seen in direct traumatic injuries are frequently comminuted and most commonly involve the phalanges of the hallux and the middle and distal phalanges of the lesser digits (4,5 and 6).
TRANSVERSE PLANE
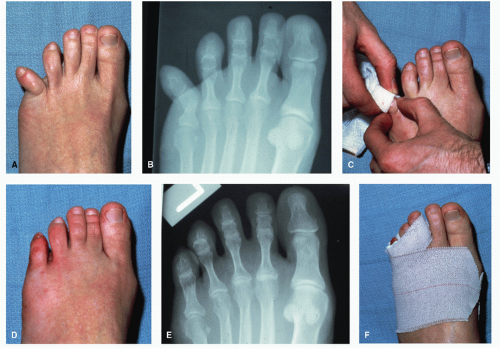
Abduction-adduction forces are also common and generally result in transverse or short oblique fractures of the proximal phalanges. The most notorious example of this injury has been termed the bedroom fracture or night-walker fracture because it often results from striking the fifth digit against a bedpost while the patient is walking in the dark (Fig. 103.1). At times, the injury may consist of a dislocation of the interphalangeal joint or the lesser metatarsophalangeal joint (MTPJ). Even though the proximal phalanx of the fifth digit is the most commonly involved, other digits may be injured through abduction or adduction forces. A transverse fracture free from the articular surfaces may be treated with closed reduction, whereas comminuted or open fractures may require surgical intervention.
FRONTAL PLANE
Rotational or inversion-eversion injuries occurring predominantly in the frontal plane are less frequent and generally are secondary components of transverse or sagittal plane fractures. When spiral fractures of the phalanges occur, closed reduction is more difficult, as is maintaining the reduction once it has been achieved, because of the more unstable nature of the fracture pattern.
CLINICAL PRESENTATION
The signs and symptoms of digital fractures consist of pain, ecchymosis, and edema that develop within a few hours after injury. The patient experiences acute pain, has difficulties with weight-bearing, and finds wearing shoes that compress the area uncomfortable. In some instances, an obvious clinical deformity is seen in the digit as a result of displacement of the fracture. Occasionally, patients may relate that they relocated the deformed toe themselves after the injury.
TREATMENT
Closed Injuries
The initial evaluation is directed toward assessing the neurovascular status of the toe or toes and evaluating the degree of tissue compromise and clinical deformity. Two to three radiographic views are adequate to demonstrate the injury in most cases.
The treatment methods of closed digital fractures range from simple protection of the toe to surgical reduction or excision of all or some of the fracture fragments. Treatment of closed digital fractures may be divided into criteria based on several factors, including the following: (a) alignment of the fracture fragments; (b) if malaligned, the possibility that the fragments can be adequately realigned with closed reduction; and (c) the possibility that alignment can be maintained
once the fragments are reduced. Reduction of the fracture is performed in an attempt to prevent shortening, angulation, and rotational malalignment.
once the fragments are reduced. Reduction of the fracture is performed in an attempt to prevent shortening, angulation, and rotational malalignment.
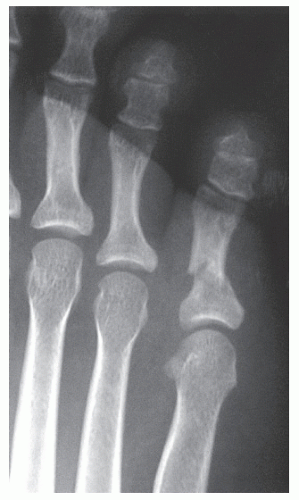 Figure 103.1 A short oblique fracture of the fifth digit that is potentially stable and may be treated with splinting. |
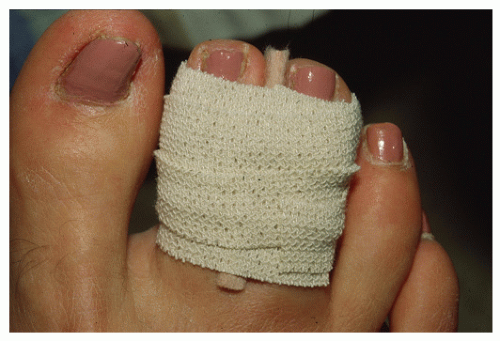
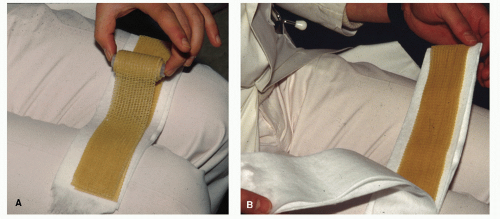
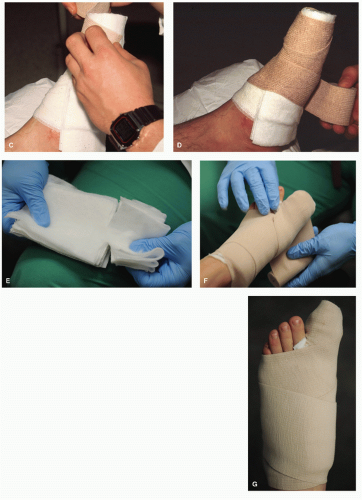
Protection alone consists of maintaining stability to the injured region with splintage and immobilization. Comfort and stability may be enhanced by splinting the injured digits to the uninjured neighboring toes with tape, felt, silicone molds, urethane molds, prefabricated digital splints, or other similar materials. This method of splintage is termed buddy splinting (Fig. 103.2). For fractures of the hallux, a gutter splint or toe spica can be formed around the hallux, first MTPJ, and medial aspect of the foot by fashioning a splint made of moldable, rigid material (e.g., cast material) and secured along the medial aspect of the foot with an ACE bandage or other soft dressing (7,8 and 9) (Fig. 103.3). After splintage, the injured foot can be additionally protected with immobilization in a surgical shoe, cast boot, cast, or in a non-weight-bearing position if necessary. Most phalangeal fractures are immobilized in the position of function, and the duration of immobilization is determined by clinical and radiographic evidence of healing. In most cases, consolidation of the osseous fragments develops in 4 to 8 weeks. During this period, the clinician must correlate the clinical findings with radiographic evidence
because fracture lines will remain radiographically visible for several months.
because fracture lines will remain radiographically visible for several months.
The alignment of the fracture fragments is the key in determining whether reduction is necessary. It is important to understand the principles of closed and open reduction as well as the anatomy and the mechanism of injury if malalignment exists. Bone injury is less significant than the soft tissue disruptions that occur on the convex side of the fracture site. Generally, the soft tissues on the concave side of the injury remain intact. These soft tissue structures guide the fracture fragments into a more normal position and tend to prevent overcorrection during closed reduction by acting as a hinge on the concave surface. Manipulative closed reduction is achieved by exaggerating the plane of deformity, followed by distraction and then reduction. After completion of the reduction, radiographs are taken to assess alignment (Fig. 103.4). The configuration of the fracture may be described as stable, potentially stable, or unstable. Stable, reduced fractures are able to withstand telescoping forces with protection and immobilization and are generally transverse in orientation to the longitudinal axis of the bone or short oblique phalangeal fractures. Stable transverse and short oblique fracture types are usually treated with closed reduction and immobilization and typically respond well and heal without adverse sequelae, unless the injury has an intraarticular component. In this circumstance, the patient may later develop stiffness or painful arthrosis even if healing progresses uneventfully.
Unstable fractures possess minimal intrinsic ability to withstand shortening and consist of long oblique, spiral, and some comminuted fractures. Creating adequate stability may require additional support from external fixation or open reduction with fixation. Kirschner wires (K-wires) can be inserted percutaneously to maintain a fracture that has been realigned with closed reduction. Serial postreduction radiographs or fluoroscopy may be used to ascertain proper placement and reduction. Direct open reduction with K-wire fixation may prove necessary in some instances.
Fractures that are unstable, nonreducible, intra-articular, or associated with coexisting neurovascular compromise need
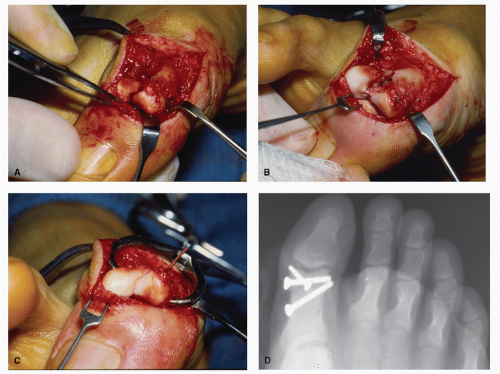
immediate attention and may require open reduction with fixation for proper alignment and stability. Surgical intervention with open reduction is performed with standard sterile technique and insertion of appropriate hardware as deemed necessary (Fig. 103.5). Achieving proper fixation is required, especially with intra-articular fractures that have a significant potential to develop posttraumatic arthritis, as seen in fractures of the hallux interphalangeal joint or first MTPJ (10,11 and 12) (Fig. 103.6).
immediate attention and may require open reduction with fixation for proper alignment and stability. Surgical intervention with open reduction is performed with standard sterile technique and insertion of appropriate hardware as deemed necessary (Fig. 103.5). Achieving proper fixation is required, especially with intra-articular fractures that have a significant potential to develop posttraumatic arthritis, as seen in fractures of the hallux interphalangeal joint or first MTPJ (10,11 and 12) (Fig. 103.6).
In the lesser digits, the concern for complete reduction of the intra-articular components of the fracture is not as great.
Stiffness or arthrosis is generally not as disabling as in the hallux interphalangeal joint, the lesser toes are not subjected to the same degree of weight-bearing stress, and surgical options for repair of these digits are generally easily accomplished. Infrequently, comminuted fractures of the hallux or lesser digits may require excision of the fragments because of the number, smaller size, or nonhealing of the fracture fragments. Excision may be carried out immediately in patients with traumatic open fractures or later with closed fractures if fragments become symptomatic after conservative treatment has failed. If painful arthrosis or malunion of the bone
persists, resectional arthroplasty of the involved joint may be necessary (13).
persists, resectional arthroplasty of the involved joint may be necessary (13).
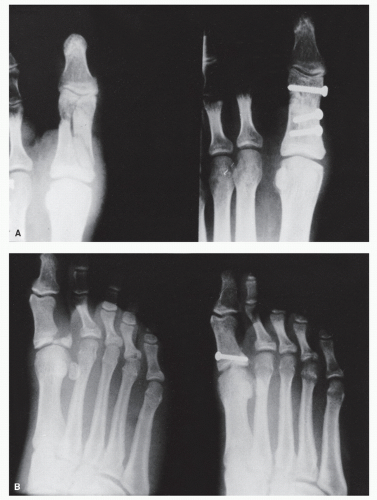 Figure 103.5 A,B: Two examples of open reduction and internal fixation of hallux fractures with screws. |
Even with proper immobilization and fixation, posttraumatic sequelae may occur with digital fractures. Included in the potential long-term problems are delayed union or nonunion of the fractured segments, malunion, chronic pain, and posttraumatic intra-articular arthrosis. In these instances, surgical intervention, possibly including arthroplasty or arthrodesis, may be necessary to obtain pain relief for the patient (10,13,14 and 15).
Open Injuries
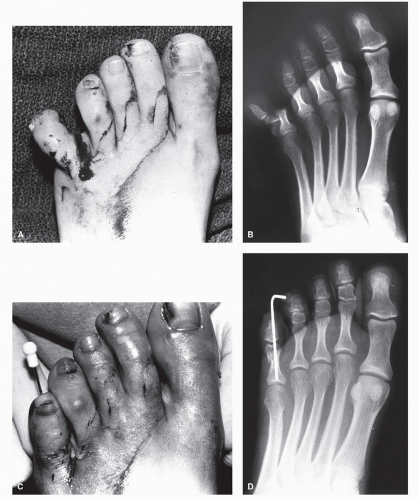
Open injuries frequently represent a surgical emergency. One should initially evaluate the neurovascular status of the injured part as well as the extent of any soft tissue loss (Fig. 103.7). Bacterial cultures should be taken from the wound and appropriate antibiotic therapy initiated. Multiple radiographs aid in assessing the bone disruption. Thorough irrigation is then necessary to reduce the risk of infection. The wounds may then be evaluated relative to the repair of the osseous injury and soft tissues.
SESAMOID FRACTURES
The sesamoids are vitally important structures to the normal function and weight-bearing mechanics of the first MTPJ. The sesamoid complex normally transmits up to 50% of body weight and during push-off can transmit loads greater than 300%. These high stresses can lead to both acute and chronic pathologies. Sesamoidal problems may occur in almost anyone from one beginning an exercise program, to the weekend warrior, to the elite-level athlete (16).
ANATOMY
The sesamoid bones of the hallux are located at the plantar aspect of the first MPTJ and are embedded within a fibrous tendoligamentous network. No periosteum surrounds the sesamoid, but rather an aponeurosis surrounds the plantar cortex (17,18). A cartilaginous dorsal surface articulates with the first metatarsal head. This is believed to increase the mechanical leverage of the great toe by acting as a fulcrum for the flexor tendons (19).
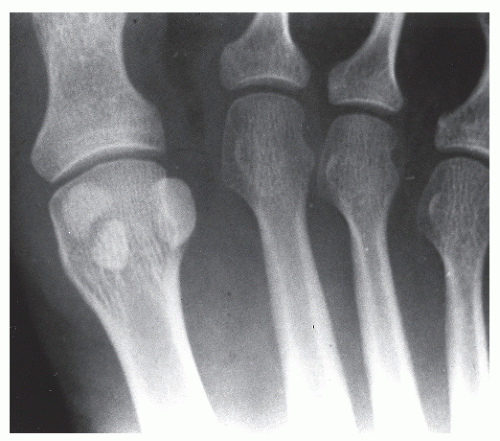
Initially, the sesamoids become identifiable as undifferentiated connective tissue within the tendon of the flexor hallucis brevis by the 8th week of embryonic life, and chondrification arises during the 12th week of gestation. Ossification usually occurs between 6 and 12 years of age. The multiple foci of ossification may or may not coalesce, leading to bipartite, tripartite, or quadripartite sesamoid bones. The incidence of bipartite sesamoids varies widely. In a large series, Kewenter reported a 35.5% incidence in 1,588 feet, and Inge and Ferguson stated a 10.7% incidence in 1,025 feet, with 75% of cases being unilateral. Both studies described numerous variations in partite sesamoids (20,21) (Fig. 103.8).
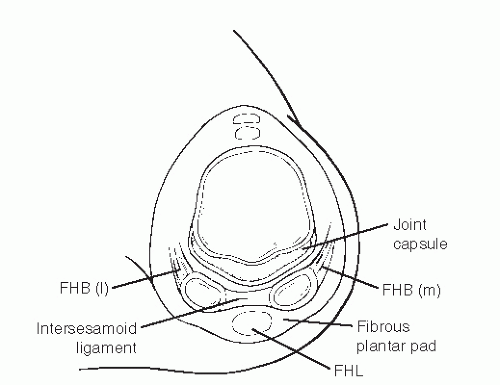
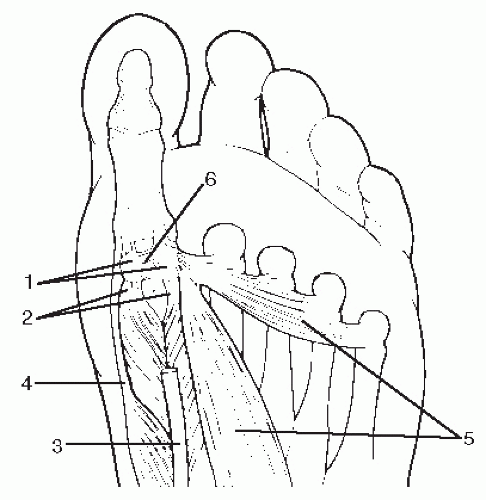
The medial (tibial) and lateral (fibular) hallux sesamoids are enclosed within the medial and lateral tendon slips of the flexor hallucis brevis muscle, with the abductor and conjoined adductor hallucis tendons inserting into the medial and lateral sesamoid complex, respectively. The sesamoids are held in place in their grooves beneath the first metatarsal head by the fibrous plantar plate, which consists of the intersesamoidal ligament, medial and lateral collateral ligaments, medial and lateral metatarsal sesamoidal ligaments (aka tibial and fibular sesamoidal ligaments), and phalangeal sesamoidal ligaments. The plantar fascia blends into the plantar surface of both sesamoids (17). The lateral (fibular) sesamoid is also attached on its plantar surface to the intermetatarsal ligament (Figs. 103.9 and 103.10).
The arterial supply of the hallux sesamoids is variable. Pretterklieber and Wanivenhaus found the number of vessels supplying the sesamoids ranging between one (55%), two (35%), and three (10%) (18) (Fig. 103.11). Rath et al (22) found the first plantar metatarsal artery to be the main source of arterial supply for the sesamoid bones and that more than 90% of feet had both sesamoids supplied by two or three arteries. The supplying arteries penetrated the sesamoid bones on the proximal, plantar, and distal sides (18,22,23).
ETIOLOGY
Traumatic injury to the sesamoid bone may result from falls, forced dorsiflexion, or repetitive stress. These injuries have become more common with the rise in sports such as aerobics, yoga, jogging, long-distance running, and speed or power walking. Athletes competing in acceleration-deceleration sports such as football, soccer, tennis, baseball, softball, or jumping activities also often present with sesamoid injuries (24). Sesamoid fractures are usually transverse or comminuted, and one or both of the sesamoids may be involved. They are frequently created from direct force in the sagittal plane, with the tibial sesamoid injured more often because of the increased weight-bearing at the medial aspect of the joint. Sagittal plane injuries tend to crush the sesamoid between the first metatarsal head and the supporting surface.
Many other sesamoid injuries are insidious in onset, and the patient is unable to recall any single, acute traumatic event. Because the sesamoids of the first MTPJ receive the weightbearing forces carried by the first metatarsal head, they have a supportive role comparable to that of the lesser metatarsal heads (20,23,25). Certain biomechanical derangements and foot types (e.g., the cavus foot or the foot with metatarsus primus equinus) are predisposed to chronic repetitive sesamoid trauma and possible fracture (26,27 and 28).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree