8 Deep dry needling of the arm and hand muscles
Introduction
Arm pain syndromes constitute a complex entity which can arise from a wide range of different conditions. Symptoms in the upper quadrant, including the neck, shoulder, arm, forearm, or hand not related to an acute trauma or underlying systemic diseases, can be provoked by trigger points (TrPs). In fact, there are several neck and shoulder muscles with referred pain pattern being perceived throughout the upper extremity, e.g. the scalenes, subclavius, pectoralis minor, supraspinatus, infraspinatus, subscapularis, pectoralis major, latissimus dorsi, serratus posterior superior and serratus anterior muscles (Simons et al. 1999). For instance, Qerama et al. (2009) demonstrated that 49% of individuals with normal electrophysiological findings in the median nerve, but with symptoms mimicking carpal tunnel syndrome, presented with active TrPs in the infraspinatus muscle with paresthesia and referred pain to the arm and fingers. In the same study, patients with mild electrophysiological signs of carpal tunnel syndrome exhibited a significantly higher occurrence of infraspinatus muscle TrPs in the symptomatic arm as compared with patients with moderate to severe electrophysiological signs (33% vs 20%). Dry needling of these muscles has been covered in Chapters 6 (scalene) and 7 (shoulder).
Additionally, TrP taut bands in the musculature of the upper quadrant can be related to neural or articular dysfunctions. For instance, since the brachial plexus runs anatomically between the anterior and the medial scalene muscles, TrPs in the scalene muscles may be related to entrapment of the brachial plexus (Chen et al. 1998). Similarly, shortening of the scalene muscles induced by TrPs taut bands may be related to first rib dysfunctions (Ferguson & Gerwin 2005), which means that clinicians should integrate TrP dry needling within the overall clinical reasoning process and management. In the current chapter we will cover deep dry needling of TrPs in the arm and hand muscles.
Clinical relevance of TrPs in arm and hand pain syndromes
There are several studies demonstrating the relevance of TrPs in the etiology of different arm pain syndromes. The most accepted muscle pain syndrome in the arm is lateral epicondylalgia (Slater et al. 2003). Fernández-Carnero et al. (2007) found that active TrPs in the extensor wrist musculature reproduced the pain symptoms in subjects with lateral epicondylalgia (65% extensor carpi radialis brevis, 55% extensor carpi radialis longus, 50% brachioradialis, 25% extensor digitorum communis muscle). In a subsequent study, Fernández-Carnero et al. (2008) reported that subjects with unilateral lateral epicondylalgia also exhibited latent TrPs within the unaffected elbow (88% extensor carpi radialis brevis, 80% extensor carpi radialis longus), which may be related to the development of bilateral symptoms in this patient population. A recent study found that active TrPs in the extensor carpi radialis brevis were very prevalent (68% right side; 57% left side) in women with fibromyalgia syndrome (Alonso-Blanco et al. 2011). These studies support the role of TrPs in arm pain syndromes, although further studies are needed. Additionally, when TrPs are present in the brachioradialis (Mekhail et al. 1999) or extensor carpi radialis brevis muscle (Clavert et al. 2009), entrapment of the radial nerve is feasible.
In clinical practice, an association between TrPs in the wrist flexor muscles and medial epicondylalgia is commonly seen, particularly in individuals with high muscular demands in the forearm, i.e., climbers (González-Iglesias et al. 2011), or with low-load but repetitive load, i.e., manual or office workers (Fernández-de-las-Peñas et al. 2012). Again, TrPs in the wrist flexor musculature can be also related to different nerve entrapments. For instance, as the pronator teres muscle is a common place for median nerve entrapment, commonly referred to as pronator syndrome (Lee & LaStayo 2004), tension induced by TrP taut bands may be relevant for symptoms associated with median nerve compression (Simons et al. 1999). Similarly, the median nerve can be entrapped by TrPs in the flexor digitorum profundus and superficialis muscles, whereas the ulnar nerve can be entrapped by TrPs in the flexor carpi ulnaris and flexor digitorum profundus (Chaitow & Delany 2008). Therefore, clinicians should consider muscle-nerve interrelations into their daily practice even though no study has confirmed the clinical observations.
Dry needling of the arm and hand muscles
Coracobrachialis muscle
• Anatomy: The muscle originates from the coracoid process and inserts to the mid-portion of the humerus bone.
• Function: It assists in flexion and adduction of the arm at the glenohumeral joint.
• Innervation: Musculocutaneous nerve, via the lateral cord from the C5 and C6 roots. It should be noted that the musculocutaneous nerve crosses the muscle belly of the coracobrachialis underneath the pectoralis major muscle.
• Referred pain: It is projected over the anterior aspect of the shoulder and also extends down the back of the arm and dorsum of the forearm to the back of the hand.
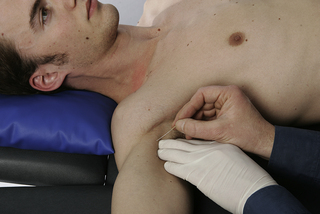
• Needling technique: The patient lies supine with lateral rotation at the shoulder. The muscle is needled via flat palpation. The needle is inserted perpendicular to the skin from medial to lateral side toward the upper third of the humerus bone (Figure 8.1). The muscle can also be needled near the coracoid process just medial to the tendon of the short head of the biceps brachii muscle.
• Precautions: The neurovascular bundle, which includes the median nerve, the musculocutaneous nerve which passes through the muscle, the ulnar nerve, and the brachial artery, is located dorsally and medially to the muscle and must be avoided.
Biceps brachii muscle (short head)
• Anatomy: The long head of the muscle originates from the superior margin of the glenoid cavity, whereas the short head originates from the coracoid process of the scapula. Both heads attach distally to the lesser tuberosity of the radius.
• Function: This muscle flexes the forearm at the elbow, assists flexion of the arm at the shoulder, and assists supination of the forearm when the elbow is not fully extended.
• Innervation: Musculocutaneous nerve, via the lateral cord from the C5 and C6 roots. It should be noted that the median nerve runs anatomically medial to the muscle belly of the biceps brachii (Maeda et al. 2009).
• Referred pain: It is projected mainly upward, over the muscle to the front of the shoulder (mimicking symptoms of long head bicipital tendonitis) and the common tendon of the bicep brachii muscle.
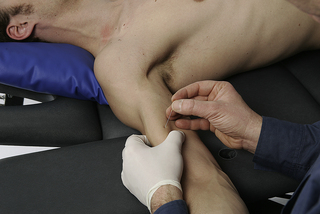
• Needling technique: The patient lies in supine. The muscle is needled via a pincer palpation. The needle is inserted perpendicular to the skin from medial to lateral side of the short head, and directed towards the practitioner’s finger (Figure 8.2). Otherwise, the needle can be also inserted from lateral to medial side of the muscle.
• Precautions: The neurovascular bundle, which includes the median nerve, the musculocutaneous nerve, the ulnar nerve and the brachial artery, is located medially to the biceps brachii muscle and must be avoided.
Triceps brachii muscle (lower portion)
• Anatomy: The long head of the muscle originates from the scapula inferior to the glenoid fossa, the medial head originates from the medial portion of the humerus and the lateral head originates from the lateral side of the humerus. All three heads insert to the olecranon process on the ulna via a common tendon.
• Function: This muscle extends the forearm at the elbow (antagonist of biceps brachii). The long head may extend the arm at the shoulder joint.
• Innervation: Radial nerve, via the posterior cord of the brachial plexus from spinal roots C7 and C8.
• Referred pain: It is projected up and down the posterior aspect of the shoulder, spreading occasionally to the upper trapezius region, and sometimes down the dorsum of the forearm, to the posterior part of the arm, spreading to the dorsum of the forearm or the fourth and fifth digits (lateral head), and to the lateral, sometimes to the medial, epicondyle (medial head).
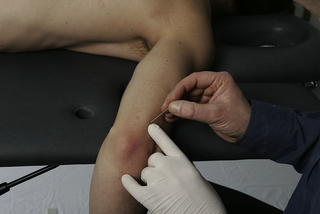
• Needling technique: For the lower portion, the patient lies in prone. The muscle is needled via flat palpation. The needle is inserted perpendicular to the skin from lateral to medial side of the lateral head directed towards the posterior part of the humerus (Figure 8.3). If the muscle belly can be grasped with pincer palpation, the needling procedure can be also conducted with pincer palpation. The upper portion (which is needled via pincer palpation) is covered in Chapter 7.
• Precautions: The radial nerve runs deep to the lateral head of the triceps muscle (Rezzouk et al. 2002) and must be avoided. This is of particular relevance for dry needling of the upper portion of the muscle (see Ch.7).
Anconeus muscle
• Anatomy: The muscle originates from the side of the olecranon process and to the dorsal surface of the ulna, and inserts to the lateral epicondyle.
• Function: It assists the extension movement of the forearm at the elbow (agonist of the triceps brachii).
• Innervation: Radial nerve, via the posterior cord of the brachial plexus from spinal roots C7 and C8.
• Referred pain: It induces pain and tenderness locally to the lateral epicondyle.
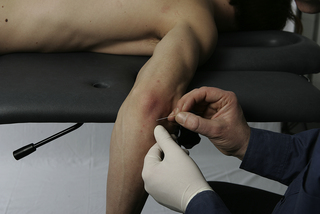
• Needling technique: The patient lies in prone, with the forearm flexed about 45° at the elbow. The muscle is needled via flat palpation. The needle is inserted perpendicular to the skin directed towards the ulna bone (Figure 8.4).
Brachialis muscle
• Anatomy: The muscle originates from the distal two thirds of the humerus and inserts at the coronoid process of the ulnar tuberosity. This muscle extends into the anterior part of the joint capsule of the elbow.
• Function: This muscle flexes the forearm at the elbow.
• Innervation: Musculocutaneous nerve, via the lateral cord and by spinal roots C5 and C6.
• Referred pain: It is projected to the base of the thumb, and often to the ante-cubital region of the elbow.
• Needling technique: The patient lies supine with the elbow relaxed and slightly flexed. The muscle is needled via a flat palpation. The muscle is needled only from the lateral aspect of the arm to avoid hitting the neurovascular bundle. The needle is directed medially between the biceps and triceps brachii (Figure 8.5).
• Precautions: The neurovascular bundle should be avoided over the medial head of the muscle.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree