CHAPTER 3
Wrist
Case Study 3.1: Acute Fracture
Hardeep Singh and Craig M. Rodner
SETTING: ORTHOPEDIC URGENT CARE OR EMERGENCY DEPARTMENT
Definition and Incidence
Wrist fractures are one of the most common orthopedic injuries presenting in two age groups: younger individuals as a result of high-energy trauma, and older individuals as a result of low-energy trauma, classically falls.
Patient
A 65-year-old female presents to the emergency department after a fall onto her right outstretched hand while jogging. She was able to get herself up; however, she had pain, swelling, and a deformity in her right wrist immediately after the fall. Pain is rated at a 9 out of 10, and worse with any movement. The patient reports that she is unable to move her wrist due to the pain and denies any numbness or tingling. The patient denies any loss of consciousness, head trauma, or other musculoskeletal injuries.
Social History
This 65-year-old woman is a retired schoolteacher, and is very active in running. She is currently training for a 10-km race that takes place in 3 months.
Physical Assessment
Upon physical examination, the patient is in mild distress due to her discomfort. Her wrist has visible swelling and deformity. The skin is intact and motor function intact in her extensor pollicis longus (radial nerve), flexor pollicis longus (median nerve), and hand intrinsic muscles (ulnar nerve). Sensation is intact in the median, ulnar, and radial nerve distributions and she has a palpable radial pulse. Elbow range of motion is full.
Diagnostic Evaluations
Radiographs are taken, and include poster anterior (PA) and lateral views of the wrist (Figure 3.1). The wrist is examined for radial inclination (normal 23 degrees), radial height (normal 11–13 mm), and volar tilt (normal 11 degrees) (Lafontaine, 1989). The x-rays reveal that the patient has a right distal radius fracture with loss of radial height, radial inclination, and volar tilt.
Diagnosis
Distal radius fracture, displaced.
Interventions
The patient is given a hematoma block, which was performed at the fracture site using 10 mL of 1% lidocaine without epinephrine to provide adequate anesthesia. The patient’s arm was then subsequently hung onto an intravenous (IV) pole using finger traps to provide traction, also known as “ligamentotaxis.”The fracture was reduced by recreating the mechanism of injury, which included hyperextending the wrist and providing longitudinal traction as used to perform a closed reduction. A sugar-tong splint was applied and molded with a three-point mold to hold the reduction. X-rays were repeated to assess the adequacy of reduction.

FIGURE 3.1 Poster anterior (PA) and lateral views of the right wrist demonstrating a distal radius fracture with dorsal angulation.
Patient Education
In the urgent care setting, it is important that the patient understands the need to follow up within 1 week to assess the wrist fracture and discuss management options. Patient should not bear weight on the affected extremity and should keep it elevated to help with swelling control.
Follow-Up Evaluation
Postreduction x-rays are assessed for radial inclination, radial height, and volar tilt. It is important to also evaluate the neurologic status of the extremity after reduction (Litchman, 2010). As this injury requires surgical consultation, it is possible that the nurse practitioner may not follow up directly with the patient. If the nurse practitioner is in a setting working collaboratively with an orthopedic surgeon, the nurse may perform the preoperative and postoperative care of the patient, and may be in a position to assist in the operating room. For the primary care nurse practitioner, it is likely the patient will return after surgical intervention and rehab has been completed, and the patient has been discharged from the specialist. The patient was referred in consultation with hand surgery. She decided to undergo operative treatment for her right distal radius fracture, which included an open reduction and internal fixation (ORIF) with a volar distal radius locking plate, restoring the radial height, radial inclination, and volar tilt, as shown in Figure 3.2.
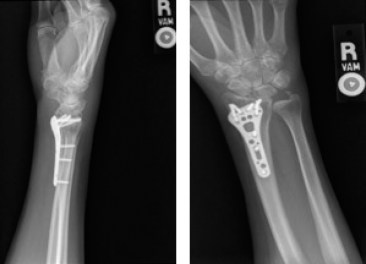
FIGURE 3.2 Posteroanterior (PA) and lateral views of the right wrist after having undergone open reduction and internal fixation with a volar plate. The radial height, radial inclination, and volar tilt are restored.
CLINICAL PEARL
Be sure to evaluate radiographs for radial height, radial inclination, and volar tilt. Acceptable parameters for an adequate reduction include: less than 5 mm of radial shortening, less than 5 degrees of change in radial inclination, less than 2-mm articular step off, and dorsal angulation of less than 5 degrees.
REFERENCES
Lafontaine, M., Hardy, D., & Delince, P. (1989). Stability assessment of distal radius fractures. Injury, 20(4), 208–210.
Lichtman, D. M., Randipsingh, R., Boyer, M. I., Putnam, M. D., Ring, D., Slutsky, D. J., … Raymond, L. (2010). Treatment of distal radius fractures. Journal of the American Academy of Orthopaedic Surgeons, 18(3), 180–189.
Case Study 3.2: Acute DeQuervain’s Tenosynovitis
Hardeep Singh and Craig M. Rodner
SETTING: ACUTE VISIT IN THE ORTHOPEDIC OFFICE
Definition and Incidence
DeQuervain’s disease is a common pathology of the wrist, and often results from overuse. Pain is generated from resisted gliding of the tendons (abductor pollicis longus and extensor pollicis brevis) in the first dorsal compartment of the wrist (Haque et al., 2015).
Patient
A 40-year-old female presents with an insidious onset of right radial-sided wrist pain for 2 months. The pain is localized above the radial styloid and is worse with activity. She rates the pain as a 4 out of 10 at rest, and 7 out of 10 with activity. She denies any history of trauma. She denies having tried anything to relieve her symptoms. She denies any numbness or tingling in the wrist or hand.
Social History
Patient works as a secretary and is unable to continue typing due to the pain in her wrist. She is married and lives with her husband and her 7-year-old daughter.
Physical Assessment
On physical examination, she is in no acute distress. Inspection reveals minimal swelling over the right radial styloid. With palpation, the first dorsal compartment (abductor pollicis longus and extensor pollicis brevis) is tender. She has full, nonpainful range of motion in her fingers and elbow.
Diagnostic Evaluation
A Finkelstein test is performed and found to be positive. Because the diagnosis of acute DeQuervain’s tenosynovitis is a clinical diagnosis, radiographs are not necessary.
Diagnosis
DeQuervain’s tenosynovitis.
CLINICAL PEARL
The Finkelstein test is confirmatory for DeQuervain’s tenosynovitis. The Finkelstein test is performed by making a fist over the thumb and then moving the hand into ulnar deviation, which passively stretches the thumb tendons over the radial styloid (Shehab & Mirabelli, 2013). Pain with this motion is considered a positive test.
Interventions
Treatment options are discussed with the patient. The patient is given a thumb spica splint (see Figure 3.3) to rest her thumb and is given a corticosteroid injection (40-mg Depo-Mederol or Kenalog) into the first dorsal compartment. It is recommended to the patient to rest her wrist, use the thumb spica splint for comfort, and follow up in 4 weeks.
Patient Education
Importantly, teach the patient that she has options for the treatment of her condition. These treatment options range from conservative to operative in nature and are a stepwise process. Rest and modalities to decrease inflammation are the first line of treatment and include oral anti-inflammatory medications such as ibuprofen (800-mg three times a day) or Naprosyn (500-mg two times a day), and splinting. If the patient is very uncomfortable, and desires an injection, then a corticosteroid injection may be given at any time in the treatment.

FIGURE 3.3 A thumb spica splint.
CLINICAL PEARL
DeQuervain’s tenosynovitis is an inflammatory condition affecting the first dorsal compartment of the hand (abductor pollicis longus and extensor pollicis brevis). The condition is more prevalent in females, and oftentimes common with new mothers picking up their children.
Follow-Up Evaluation
The patient returns to the clinic at 3 and 6 months for repeat steroid injection, but has diminishing relief from each subsequent injection. The patient returns to the clinic with worsening symptoms over the first dorsal compartment and elects to undergo operative treatment. The patient is taken to the operating room and has surgical release of the first dorsal compartment. She presents to the office 2 weeks later and reports having complete pain relief.
REFERENCES
Haque, M. M., Datta, N. K., Faisal, M. A., Islam, A., Uddin, M. J., Tarik, M. M., & Hossain, M. A. (2015). Surgical decompression of resistant cases of DeQuervain’s disease. Mymensingh Medical Journal, 24(2), 341–345. PubMed PMID: 26007263.
Shehab, R., & Mirabelli, M. H. (2013). Evaluation and diagnosis of wrist pain: A case-based approach. American Family Physician, 87(8), 568–573.








