Treatment of Vertical Talus
Matthew B. Dobbs
DEFINITION
Congenital vertical talus is a rare foot deformity that presents at birth as a rigid flatfoot deformity.
Although the exact incidence of vertical talus is unknown, it has an estimated prevalence of 1 in 10,000 live births.
It is associated with neuromuscular disorders or genetic syndromes in half of all cases, whereas the remainder occurs as isolated deformities.
Of the 50% of cases of vertical talus that are isolated, almost 20% of these have a positive family history of other members affected with vertical talus.
ANATOMY
The hindfoot is in marked equinus and valgus caused by contracture of the tendo Achilles and the posterolateral ankle and subtalar joint capsules.6, 12
The midfoot and forefoot are dorsiflexed and abducted relative to the hindfoot due to contractures of the tibialis anterior tendon, extensor digitorum longus, extensor hallucis brevis, peroneus tertius, extensor hallucis longus tendons, and the dorsal aspect of the talonavicular capsule.
The navicular is dorsally and laterally dislocated on the head of the talus resulting in the development of a hypoplastic and wedge-shaped navicular.
The talar head and neck are flattened and medially deviated.
The extreme plantarflexion of the talus results in attenuation of the calcaneonavicular or spring ligament and a rocker bottom appearance of the foot where the sole is convex and deep creases are seen in the dorsolateral aspect of the foot.
The calcaneus is plantarflexed, leading often to dorsolateral subluxation or frank dorsal dislocation of the cuboid on the calcaneus.
The posterior tibial tendon is usually subluxed anteriorly over the medial malleolus, whereas the peroneus longus and brevis may be subluxed over the lateral malleolus; the subluxed tendons may then function as ankle dorsiflexors rather than plantarflexors.
PATHOGENESIS
With a host of different genetic and neuromuscular etiologies for vertical talus, it is likely that the pathophysiologic basis for its development is heterogeneous in nature.
Genetic factors play a significant role not only in syndromic cases but in many isolated cases as well.17, 19
The most common gene mutations identified to date for isolated vertical talus are in the HOXD10 gene, encoding a homeobox transcription factor gene expressed in early limb development and the GDF5 (cartilage-derived morphogenetic protein-1) gene.8, 9
Some neurologic cases present with significant muscle imbalances that can explain the resulting clinical deformity.
Congenital muscle abnormalities are responsible in other patients as supported by abnormal skeletal muscle biopsies.
Magnetic resonance angiography in this patient population demonstrates vascular insufficiencies in the lower limb that may be an etiologic factor.
NATURAL HISTORY
Left untreated, the deformities present in vertical talus worsen with weight bearing as secondary adaptive changes occur in the tarsal bones.
Painful callosities develop along the plantar medial border of the foot around the prominent and unreduced talar head.
Heel strike does not occur, shoe wear becomes difficult, and pain develops.
PATIENT HISTORY AND PHYSICAL FINDINGS
Hindfoot equinus, hindfoot valgus, forefoot abduction, and forefoot dorsiflexion are present in all patients with vertical talus in the newborn period, but the deformities vary in severity resulting in many patients not being diagnosed correctly at birth (FIG 1).
In congenital vertical talus, the plantar surface of the foot is convex, creating a rocker bottom appearance.
There are deep creases on the dorsolateral aspect of the foot.
The forefoot dorsiflexion results in a palpable gap dorsally where the navicular and talar head would normally be articulating.
The presence of active dorsiflexion and plantarflexion of the toes is recorded as absent, slight, or definitive. This should be recorded for the great toe alone as well as the lesser toes as a separate group.
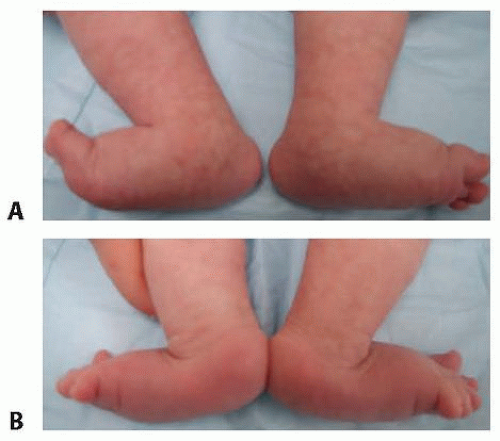
FIG 1 • A. Convex plantar surface of the feet associated with bilateral congenital vertical talus. B. View from behind illustrating the deep creases on the dorsolateral aspect of the feet.
Slight or absent ability to move the toes with stimulation correlates, in our experience, with vertical talus deformities that are more rigid and less responsive to treatment.
In addition to examining the feet, the physician should look for the presence of a sacral dimple which may signify a central nervous system anomaly.
IMAGING AND OTHER DIAGNOSTIC STUDIES
Standard radiographs in evaluation of vertical talus include an anteroposterior radiograph of the foot and three laterals of the foot: maximal dorsiflexion, maximal plantarflexion, and neutral (standing for older children).
The maximal plantarflexion lateral radiograph is the most critical film because a lateral talar axis-first metatarsal base angle (TAMBA) of greater than 35 degrees is pathognomonic for the disorder (FIG 2).
Values below 35 degrees do not rule out a vertical talus, however. In such cases, to differentiate a more flexible vertical talus from an oblique talus, the presence or absence of hindfoot equinus must be documented. If equinus is present, then the deformity is rigid and warrants treatment in the same manner as those vertical tali with a TAMBA angle of more than 35 degrees.
The forced dorsiflexion lateral demonstrates persistent rigid hindfoot equinus.
The anteroposterior radiograph demonstrates an increased talocalcaneal angle indicative of hindfoot valgus.
DIFFERENTIAL DIAGNOSIS
Oblique talus
Calcaneovalgus foot
Posteromedial bow of the tibia
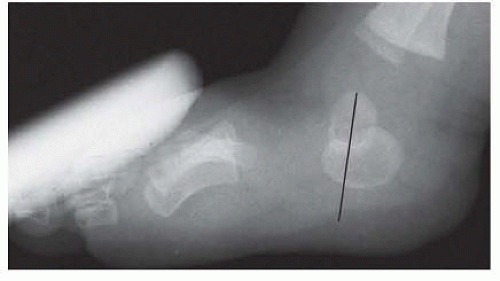
FIG 2 • Plantarflexion lateral radiograph of the left foot of the patient in FIG 1, demonstrating the lack of reduction of the talonavicular joint.
NONOPERATIVE MANAGEMENT
Older casting techniques were not successful in correcting vertical talus deformities.
SURGICAL MANAGEMENT
Correction of all rigid vertical tali should be considered due to the unfavorable natural history.
The use of the Dobbs method of serial manipulation and casting followed by temporary Kirschner wire stabilization of the talonavicular joint and a tendo Achilles tenotomy has provided a new treatment strategy that avoids more extensive soft tissue release surgery while providing excellent correction and preserving ankle and subtalar mobility.1, 2, 3, 4, 5, 7, 10, 13, 14, 15, 20
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








