CHAPTER 24 Transtibial Single-Bundle Posterior Cruciate Ligament Reconstruction
Injuries to the posterior cruciate ligament (PCL) are increasingly being recognized in athletes and trauma patients. The past decade has seen an increase in the diagnosis, treatment, and study of these injuries. Depending on the patient population being evaluated, there is a wide range reported for the incidence of PCL injuries. The incidence of PCL injury varies between 3% in an athletic population to 37% in the emergency room trauma setting.1–3 Many of these patients have multiple ligament involvement including anterior cruciate ligament (ACL), posterolateral corner (PLC), and medial-sided injuries. Clinical and cadaveric studies have established that grade 3 PCL injuries usually involve concurrent injury to the posterolateral corner.4
In this chapter, we will describe the anatomy of the posterior cruciate ligament, pertinent aspects of the history and physical examination in evaluating patients with a potential PCL injury, diagnostic imaging, treatment options, and our single-bundle transtibial reconstruction technique. There is much debate surrounding PCL reconstruction, including timing and the optimal technique. This chapter describes our preferred transtibial technique in detail, but we are aware that several successful reconstructive techniques may yield equivalent outcomes.5–12
ANATOMY
Structure
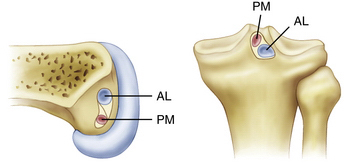
The posterior cruciate ligament is an extra-articular ligament. Although it is clearly visualized arthroscopically, there is a thin layer of synovium that reflects from the posterior capsule and surrounds the PCL. The PCL is between 32 and 38 mm in length and its cross-sectional area at its midsubstance is 32.2 mm2 (approximately 1.5 times larger than the ACL).13 The insertion sites of the PCL are approximately three times larger than the midsubstance cross-sectional area, giving the PCL an hourglass appearance. The fibers of the PCL attach on the tibia approximately 1.0 to 1.5 cm below the joint line in a lateral to medial direction (Fig. 24-1). On the femoral side, the PCL fibers attach to the medial femoral condyle in an anterior to posterior direction, adjacent to the anterior margin of the articular cartilage.
There are three main components of the PCL—the anterolateral bundle (AL), the posteromedial bundle (PM), and the meniscofemoral ligaments.14–17 These components each have unique bony insertions as well as anatomic and biomechanical properties. The anterolateral bundle has a maximum load of 1120 N and a stiffness of 120 N/mm, the posteromedial bundle has a maximum load of 419 N and a stiffness of 57 N/mm, and the meniscofemoral ligaments have a maximum load of 297 N and a stiffness of 49 N/mm.16 The anterior meniscofemoral ligament (ligament of Humphrey) and the posterior meniscofemoral ligament (ligament of Wrisberg) arise from the posterior horn of the lateral meniscus and sandwich the PCL bundles. Because the meniscofemoral ligaments are attached to the mobile lateral meniscus, it is possible for the PCL to be ruptured while the meniscofemoral ligaments remain intact. Their anatomic location and relative strength allow them to provide a scaffold for an injured PCL ligament while it attempts to heal. The AL bundle has twice the cross-sectional area of the PM bundle and 150% of the stiffness and strength, so it is considered the most important component of the PCL and the focus of single-bundle reconstructions.18
The vascular supply to the posterior cruciate ligament is from the popliteal artery via the middle geniculate artery. The synovial sleeve covering the PCL is well vascularized and is a major contributor to the blood supply of the ligament.19,20 The synovial sleeve that provides a rich vascular supply to the PCL, as well as the meniscofemoral ligaments, gives some PCL injuries the potential to heal. Both the PCL and its synovial sleeve are innervated by nerve fibers from the popliteal plexus. The plexus receives contribution from the posterior articular nerve, a prominent branch of the posterior tibial nerve, and from the terminal portions of the obturator nerve.21 Golgi organ–like structures have been observed near ligament origins beneath the synovial sheath and are thought to have a proprioceptive function in the knee.22 Ruffini’s corpuscles (pressure receptors), Vater-Pacini corpuscles (velocity receptors), and free nerve endings (pain receptors) have also been found in the PCL on histologic study.23 Therefore, disruption of the PCL not only alters knee kinematics, but also alters the sensation and, probably, proprioception.24
Injuries to the posterolateral corner are commonly associated with PCL injuries. It is highly unlikely that a patient has a grade 3 PCL injury without a significant injury to the posterolateral corner.4 The structures of the PLC have been studied at length and there remains some debate as to which structures are included. Traditionally, the structures of the posterolateral corner are the popliteus tendon, popliteofibular ligament, and lateral collateral ligament.25–27 However, other structures that have been described as part of the posterolateral corner include the joint capsule, arcuate ligament, and fabellofibular ligaments.
Function
The kinematics of the posterior cruciate ligament reflects the two-bundle anatomy. The larger anterolateral bundle is tight in flexion and slackens with knee extension.14,17 The posteromedial bundle is tight in extension and slackens with knee flexion. With deep knee flexion, the PM bundle moves anterior and away from the tibial plateau so that it becomes taut again in deep knee flexion.28 Midranges of flexion recruit fibers from both bundles so that neither bundle is completely slack. When studied independently, however, neither bundle is completely isometric.
Biomechanical studies have shown that the PCL is the primary restraint to posterior drawer forces and is a secondary restraint to external rotation.25–27 Isolated section of the PCL, without damage to the posterior capsule, results in a small degree of increased posterior laxity in full extension, with more pronounced increases in posterior laxity with flexion to 90 degrees.29,30 In these studies, there were only minimal changes in rotation or varus-valgus laxity from isolated PCL sectioning.
The structures of the posterolateral corner each have an independent kinematic profile that comes together in a complex pattern to provide resistance to tibial external rotation and posterior tibial translation.4,25–27 Individually, the lateral collateral ligament (LCL) is the primary restraint to varus stress and does not significantly contribute to anterior/posterior translational control. The popliteofibular ligament complex, which comprises the popliteus and popliteofibular ligament, is relatively isometric and controls external tibial rotation at all angles of knee flexion.31 It tightens in full extension to provide restraint to posterior tibial translation at full extension. Combined sectioning of the PCL and posterolateral corner results in significantly increased posterior laxity when compared with isolated sectioning of the PCL or the posterolateral corner alone.32 Therefore, injuries to either structure when both are damaged will result in increase stress on the remaining structure or reconstruction.33
PATIENT EVALUATION
History
Physical Examination
Careful evaluation of the ligamentous structures of the knee is crucial. Because isolated PCL injuries are rare, and isolated grade 3 tears perhaps nonexistent, a multiligamentous injury should be suspected whenever a PCL injury is identified. The usual clinical testing of the ACL, medial collateral ligament (MCL), and LCL should be carried out. In an unstable knee, it is critical to perform these tests with the knee starting in a reduced position. If the test is performed from a subluxed position, the examiner may mistake the cause of laxity—for example, reporting a positive anterior drawer in the setting of a PCL tear because the anterior drawer test was initiated from a posteriorly subluxed position.
A posterior drawer test is the most accurate clinical test for PCL injuries.34,35 The patient is placed supine with the knee flexed to 90 degrees and the tibia neutrally rotated. A posteriorly directed force is placed on the proximal tibia. This can also be performed with the tibia in external rotation (posterolateral drawer) and internal rotation (posteromedial drawer) to assist in evaluation of the posterolateral and posteromedial corners, respectively. The extent of posterior translation of the tibia with respect to the femur is measured by evaluating the relationship and change in position of the proximal tibia and medial femoral condyle. Normally, the medial proximal tibia is positioned approximately 1 cm anterior to the medial femoral condyle, but comparison with the contralateral side, if uninjured, can provide an accurate reference point. In addition to degree of translation, the quality of the end point is important in the evaluation of the PCL injury.
Grade I injuries are partial thickness tears that have a palpable but diminished step-off of the tibia with respect to the femur. This corresponds to 0 to 5 mm of posterior tibial translation. Grade II injuries are partial-thickness tears in which patients have lost the normal tibial step-off, but the proximal tibia does not translate posteriorly to the medial femoral condyle. This corresponds to 5 to 10 mm of posterior tibial translation. More than 10 mm of posterior tibial translation corresponds to a grade III injury, which is consistent with a complete PCL rupture.33 The proximal tibia will translate posterior to the medial femoral condyle without a good end point in this setting. Grade III injuries are associated with PLC injury in most, if not all cases.4
The posterior sag test (Godfrey test) is performed with the hip and knee flexed to 90 degrees. The examiner supports the lower extremity by holding the foot and observes the proximal tibia with respect to the femur. In the setting of a complete PCL tear, gravity will pull the proximal tibia posteriorly. By comparing the anterior profile of the injured knee and proximal tibia with the normal side, very subtle posterior translations can be seen. The quadriceps active test is performed with the patient supine and the knee flexed to 60 degrees. While the examiner stabilizes the foot, the patient contracts the quadriceps muscle. With PCL insufficiency, the tibia will initially lie posteriorly subluxed when the knee is relaxed, but with isometric quadriceps contraction, the tibia will translate anteriorly and attempt to reduce relative to the femur. The reverse pivot shift test is performed by passively extending the knee from a flexed position with the foot externally rotated and a valgus force applied to the tibia. The tibia will initially be subluxed posterolaterally if the PCL-PLC is not functional, but will abruptly reduce with respect to the femur at 20 to 30 degrees of knee flexion as the knee comes into extension.36 Additional tests for injury to the PCL and posterolateral corner have been described. See the chapter on the posterolateral corner for an in-depth review of this topic (Chapter ••).
A careful neurovascular examination is critical for evaluating patients with PCL injuries. The structures of the popliteal fossa include the popliteal artery, popliteal vein, tibial nerve, and peroneal nerve. The popliteal artery is tethered proximally at the adductor hiatus and distally at the soleus arch, and therefore vulnerable to injury from dislocation of the knee. The peroneal nerve is at risk for injury because of the course it takes around the fibular head, especially in the setting of associated varus injury. The incidence of neurovascular injury ranges from 14% to 49%.26,29,30 Because many knee dislocations “autoreduce” before they are examined or imaged, the physician must be careful to monitor for injury and to get appropriate studies if injury is suspected.
Diagnostic Imaging
Radiography
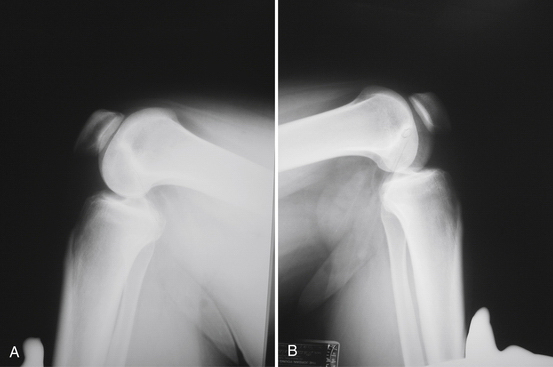
A standard knee series, including bilateral standing anteroposterior (AP), AP flexion 45-degree weight-bearing, lateral, and Merchant patellar radiographs, should be evaluated for evidence of posterior tibial subluxation, avulsion fractures, and associated knee injury. Subtle posterior tibial subluxation may be the only finding on these films. The unopposed pull of the hamstrings causes posterior tibial subluxation, which can become fixed within a short time. Stress lateral radiography performed in neutral rotation and the knee flexed to 90 degrees with and without a posterior drawer force may show increased tibial translation with respect to the femur when compared with the contralateral knee (Fig. 24-2).
Magnetic Resonance Imaging
Magnetic resonance imaging (MRI) has become the diagnostic study of choice for evaluation of the knee with clinical suspicion of a PCL injury (Fig. 24-3). MRI and stress radiography have been shown to corroborate the severity of the PCL injury as identified on physical examination.37
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree