Towards a Functional Approach
This chapter will explore how to integrate the various principles discussed in previous chapters into a unified, functional range of movement (ROM) rehabilitation approach.
The principal aim in ROM rehabilitation is to plan a management that takes into account various patient-related processes. They include the processes underlying the ROM loss, such as the dimension in which the ROM loss occurs – are they related to adaptive tissue changes (tissue dimension), motor control losses or sensitization (neurological dimension), or are they related to fear of movement (psychological dimension)? We also need to consider the patient’s ability to execute the recovery behaviour. This will determine the level at which the management is pitched – managed, assisted, functional or extra-functional.
This chapter will explore the following topics:
 How is ROM management matched to the patient’s condition?
How is ROM management matched to the patient’s condition?
 When do we use functional or traditional stretching?
When do we use functional or traditional stretching?
 When do we use managed or assisted approaches?
When do we use managed or assisted approaches?
 Do different conditions need specific ROM rehabilitation?
Do different conditions need specific ROM rehabilitation?
 How can we create a recovery environment beyond the session?
How can we create a recovery environment beyond the session?
The Potency of ROM Challenge
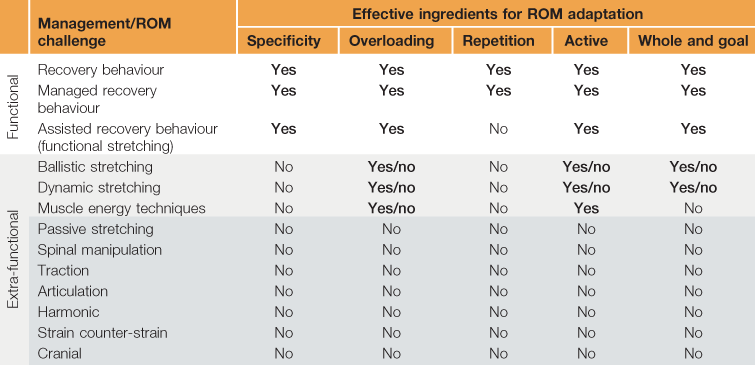
Imagine for a moment that ROM rehabilitation is some form of medication rather than a physical procedure. As such, its potency depends of several ingredients which have been identified in the previous chapters: specificity of the challenge (Ch. 5), overloading or amplifying activity at end-range (Ch. 6) and the need for frequent repetition of the ROM challenge (Ch. 7). Added to these is the importance of active versus passive ROM challenges, use of whole rather than fragmented movement and the importance of goal-orientated movement (Ch. 8). ROM management is likely to be more successful when it contains the maximum number of these ingredients and less so as their number declines (Table 12.1).
Using this table, ROM challenges can be grouped into functional and extra-functional approaches and their therapeutic efficacy can be evaluated. The recovery behaviour is at the top of this table as it contains the maximum number of ingredients, providing the ideal conditions required for ROM recovery; it is natural, free and works for most people most of the time. It is followed by managed and assisted recovery behaviour (functional stretching). Below the functional approaches are all the traditional stretching techniques. At this point there is also a drop in the number of the effective ingredients, suggesting a decline in therapeutic potential.
This hierarchy of effectiveness can be exemplified in the active stretching approaches, such as muscle energy techniques. They contain only some of the effective ingredients (overloading and active) and are missing others, such as specificity and repetition. The absence of these ingredients is likely to reduce their therapeutic effectiveness in assisting ROM recovery (see Ch. 1). However, more research is required to explore the relationship between the effective ingredients and therapeutic success. In the meantime, this can be resolved by striving to provide the functional ROM management which contains the full set of effective ingredients.
Determining the Level and Form of ROM Rehabilitation
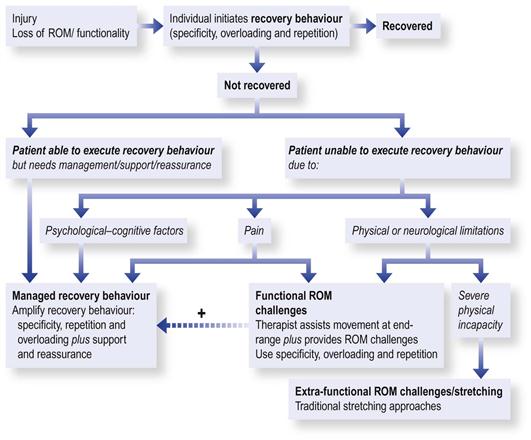
Assuming that the patient has a condition which is likely to respond to ROM rehabilitation, the next clinical task is to determine the level of ROM rehabilitation: whether it should be functional (managed or assisted) or extra-functional using traditional stretching methods (Fig. 12.1).
Recovery behaviour
All patients should be made aware of the benefits of a functional approach, highlighting the importance of specificity, overloading and repetition, i.e. “whatever you do, do more, to the end-limit and more often”. Patients who have the capacity to engage in this behaviour, who are autonomous and who have high self-efficacy and who are already challenging their movement ranges may need only this general advice.
Managed recovery behaviour
At a managed level the primary task is to identify daily tasks that provide effective ROM challenges, e.g. for a patient with restricted hip – “do more walking”. It may include focusing and amplifying specific task parameters within these daily activities (force, speed, range and endurance) – “do more walking taking wider steps” (range parameter). It could also include rectifying compensatory patterns that result in underloading of the affected joints, e.g. “avoid swinging the leg to the side when walking”. Within a managed level we also provide psychological–cognitive reassurance, in particular if the patient’s recovery behaviour is impeded by movement-related anxieties – “it might be uncomfortable as you walk but its not causing any damage”.
Assisted recovery behaviour
This level is important if the patient is capable of performing whole movement, but unable to provide sufficient overloading to effectively challenge their ROM losses. This level of management would be suitable in the early stages after immobilization or when multiple injuries or co-morbidities impede the recovery behaviour. Under these circumstances the end-range can be reached with assistance by the therapist. Once in this position, the patient is encouraged to “take over” and performs different functional tasks (see graded challenge and the task parameters, Ch. 6, and the accompanying video).
Management at the assisted level can result in the patient becoming dependent on the therapist. Since self-care is essential for ROM rehabilitation such attitudes may impede their recovery. Therefore, once the patient demonstrates an ability to perform the ROM challenge effectively they should rapidly progress to a managed approach. This progression may be difficult for patients who have a tendency for low autonomy or low self-efficacy or who have an external locus of health. They will often steer the treatment towards or wish to remain within an assisted approach. Sometimes this attitude of dependency can be difficult to modify. However, it does not represent a significant drawback in minor and short-term ROM losses. At worst the patient may need a few extra treatments. However, dependency becomes a problem in conditions that require longer treatment durations.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree