Demonstration of Functional Approach in ROM Rehabilitation
This chapter explores the use of functional range of movement (ROM) rehabilitation within a clinical setting. The demonstration will focus on the ROM rehabilitation of the upper limb (shoulder and elbow) and trunk. The management approach described for these areas can be applied elsewhere in the body. The book is accompanied by a video demonstration of the ROM challengers, which can be viewed online at: www.therapeuticstretch.com.
General principles for functional stretching
There are several principles to consider during functional ROM challenges:
Contents of THE demonstration
13.1. Demonstration of principles
13.1.1 Amplifying movement parameters during a dynamic task
13.1.2 Amplifying movement parameters during a static task
13.1.3 Alternating between dynamic and static tasks
13.1.4 Context and localization of amplification
13.1.5 Mixing ranges and planes
13.1.6 Overcoming compensatory movement patterns
13.1.7 Therapist’s stance and patient handling
13.2. Shoulder ROM challenges
13.2.1 ROM challenge during dynamic tasks
13.2.2 ROM challenges during static tasks
13.2.3 Guided challenge within a functional task
13.2.4 Assisted supine ROM challenges
13.3. Elbow ROM challenges
13.3.1 Assisted supine
13.4. Trunk ROM challenges
13.4.1 Standing challenges
13.4.2 Seated challenges
13.1 Demonstration of principles
13.1.1 Amplifying the movement parameters during a dynamic task









Notes on task parameters:
13.1.2 Amplifying movement parameters during a static task
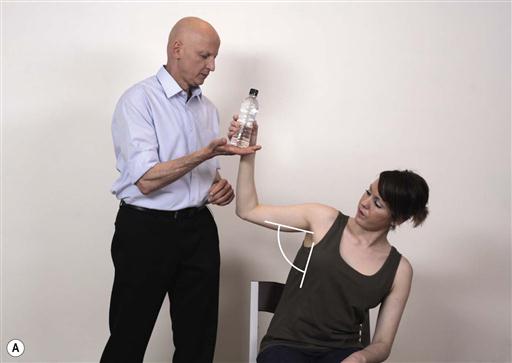
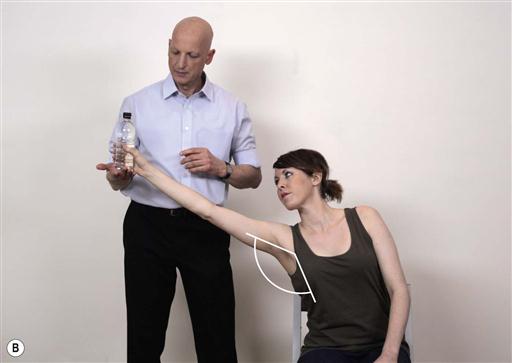
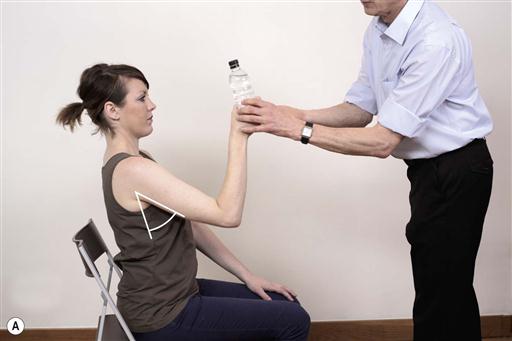
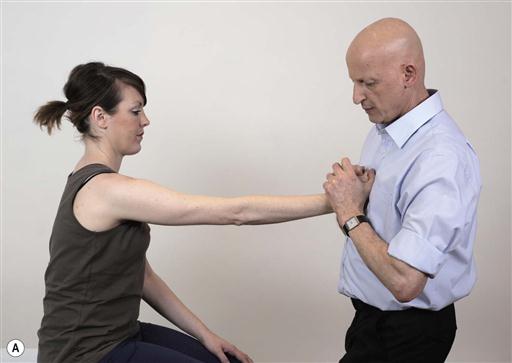
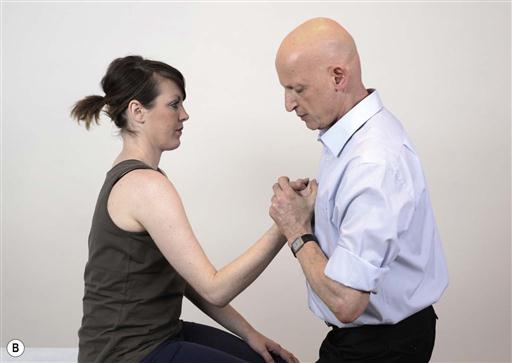
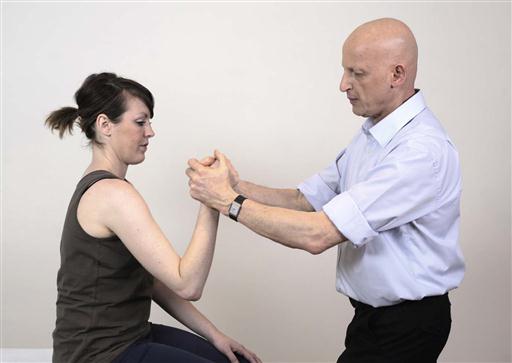
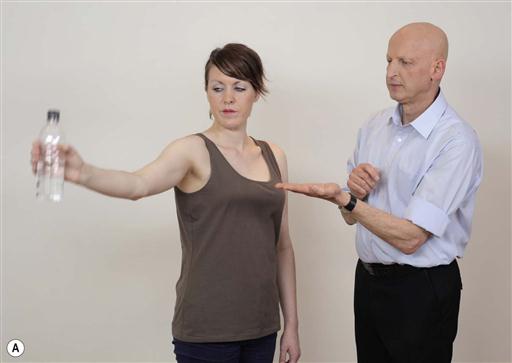
Fig. 13.4A–D. Many functional activities contain static tasks. This is reflected in challenges where the patient is instructed to hold the same position. In the following example the patient is instructed to hold the bottle and maintain it in the same position.
Notes about task parameters during static activities:
13.1.4 Context and localization of amplification
The contex principle suggests that tasks that typify arm movement can be used to challenge all the joints in the upper extremity (and the rest of the body). Some localization to specific areas/joints can be achived by positioning of the limb or changing the nature of the task. However, it should be noted that such localization of movement can be difficult to achieve clinically, in particular when ROM limitation in specific joints is compensated for by excessive movement in adjacent areas. This is further discussed in section 13.1.6 (overcoming compensatory movement patterns).




13.1.5 Mixing ranges and planes
Normal functional movement is highly variable and often involves multiple planes. Generalization of training may occur more readily when end-ranges are mixed with the whole-range challenges, as well as performing the same task in different planes (this is better demonstrated in the accompanying video).
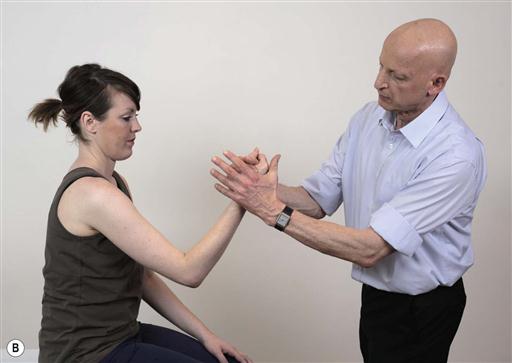
Patients who are unable to perform a movement in a particular range can be still challenged in that range (primary challenge) but with movements in another plane (secondary challenge). This principle of primary and secondary challenges is demonstrated in this section.







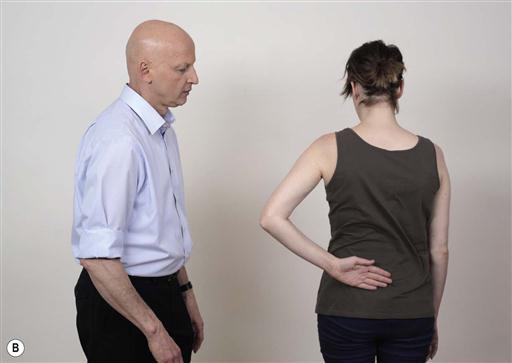
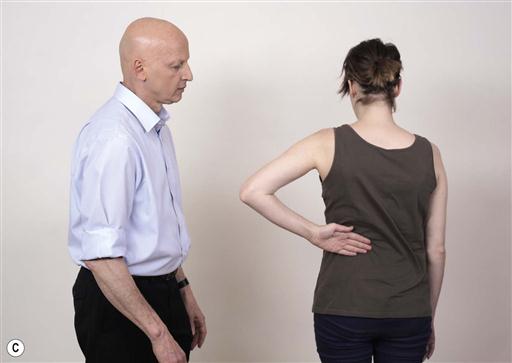
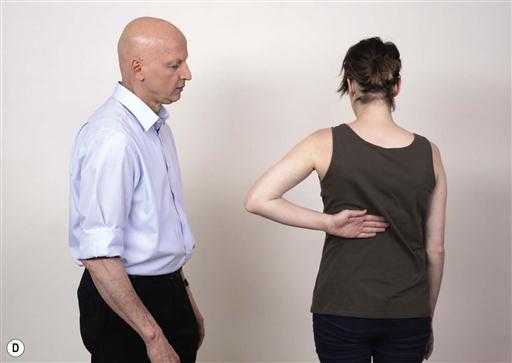


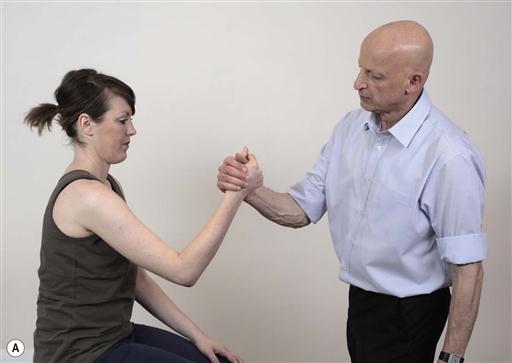
13.1.6 Overcoming compensatory movement patterns
One common problem with ROM loss is compensatory movement patterns elsewhere, which may reduce the efficacy of rehabilitation. Often, these compensatory patterns can be overcome by small modifications of the task, while keeping the focus of attention towards external goals.