Abstract
Proximal interphalangeal joint (PIP) arthroplasty is gaining increasing popularity. Besides the optimization of the surgical technique and the rehabilitation, new implants have been developed in order to improve the treatment results. Thus, the options in the treatment modalities have become more differentiated and should be tailored to the individual situation.
This chapter will discuss the anatomical features of the PIP joint related to implant arthroplasty, touch on the conservative treatment of PIP joints affections, and focus mainly on prosthetic joint replacement. Based on a case discussion, a flow chart for the different surgical treatment possibilities is presented. It should act as a possible guideline for the indications and choice of PIP arthroplasty.
Key words
proximal interphalangeal joint – surgical treatment – implant arthroplasty – indication – silicone implants – surface replacement11 The Treatment Strategy in PIP Arthroplasty
11.1 Introduction
11.1.1 Anatomical Considerations for PIP Arthroplasty
Anatomically, the distal (DIP) and the proximal interphalangeal (PIP) joints are very similar; the main difference is the dimension and the reduce mobility at the DIP joint level.
In contrast to the metacarpophalangeal (MCP) joint, the osseous shape of the PIP and DIP plays an important role in joint stability. 1 The head of the phalanx has a trapezoidal shape with an intercondylar groove which increases from dorsal to volar. There are no significant differences between the ulnar and the radial condyles. The counterpart to the head of the proximal phalanx is the base of the middle and the distal phalanges. The joint is not a perfect hinge allowing some degree of freedom for abduction and adduction as well as for joint rotation. There is, therefore, no constant center of rotation but rather an instantaneous rotational axis. 2
There are slightly different radii of curvature between the radial PIP joints and the ulnar joints. The radial joints need greater lateral stability and the ulnar joints more mobility in order to function correctly. These anatomical features are only partially mimicked by the different types of implant arthroplasty available.
11.1.2 Evaluation of PIP Joint Problems
Destruction of a PIP joint is either a result of an inflammatory/degenerative process or is posttraumatic. It is a clinical diagnosis and is confirmed with conventional radiographic examination. Patients classically present with swollen, tender PIP joints, with a diffuse, swollen appearance and a fusiform joint contour. Joint stiffness is almost always present and often correlates with the degree of swelling. In posttraumatic PIP joint arthritis, a CT scan may be useful to determine whether a joint preserving procedure is warranted, such as an intra-articular osteotomy or joint reconstruction.
Most authors, especially in the rheumatology and arthritis literature, use a modification of the Kellgren and Lawrence scale, 3 initially described for patellofemoral arthritis, for radiographic classification:
Grade 1: doubtful narrowing of joint space and possible osteophytic lipping.
Grade 2: definite osteophytes, definite narrowing of joint space.
Grade 3: moderate multiple osteophytes, definite narrowing of joint space, some sclerosis, and possible deformation of bone contour.
Grade 4: large osteophytes, marked narrowing of joint space, severe sclerosis, and definite deformation of bone contour
As always in the evaluation of a joint destruction, the grade of radiographic destruction does not predict the symptoms of an individual joint.
11.1.3 Nonoperative Treatment of PIP Destruction
Nonoperative treatment for advanced destruction of finger joints should be the first line of treatment both for inflammatory disease or osteoarthritis (OA). Treating affected joints with OA does not, to date, alter the appearance of OA in unaffected joints, or delay the progression of OA elsewhere. In the pathophysiology of the disease, catabolic cytokines and anabolic growth factors play key roles in the destruction of the cartilage.
Conventional treatment includes analgesics and nonsteroidal anti-inflammatory drugs. Intra-articular visco-supplementation with hyaluronic acid has been shown to be effective in terms of pain relief and improved disability. In comparison with intra-articular corticosteroids, it seems to have a longer benefit, 4 especially in the knee joint. However, this has not been reproduced in the hand literature and is not supported with personal experience.
Glucosamine and chondroitin are important components of the normal cartilage. Like visco-supplementation, the efficiency of glucosamine and chondroitin in the treatment of OA has been documented best in the knee joint. 5 They seem to reduce the need for anti-inflammatory drugs and improve functionality. 6 Few side effects have been reported. Most authors recommend a combination of the two, at a dosage of 1500 mg glucosamine and 1200 mg chondroitin daily. Since the onset of the effects is slow and takes at least 4 weeks, most authors recommend either 3 months’ therapy twice a year or continuous treatment. 6 There is no literature supporting its efficacy in the hand. Disease modifying drugs, used mainly in patients suffering from rheumatoid arthritis, are good candidates for suppressing the destructive inflammatory process in OA as well. Besides the classic systemic application of this drug, an intra-articular treatment with injection showed a possible disease modifying action of intra-articular Infliximab in erosive OA of the hands in a pilot study. 7
The PIP joint reacts well to intra-articular corticosteroid injections. The most common side effect is atrophy of the skin and subcutaneous tissue, which is more of an aesthetic than a functional problem. No known correlation exists between the radiographic appearance of the joint and the effectiveness of intra-articular steroid administration, and is typically self-limiting. There are different techniques for PIP infiltration: the author finds injecting into the dorsal recess of the joint, similar to a knee joint, is the easiest to perform.
Splints for painful inflamed joints might be effective, but their regular use limits hand function and lowers patient satisfaction. 8 Modification of activity may be beneficial in limiting articular inflammation. Joint protection devices may relieve the joints and help to prevent further irritation of the affected joints.
The effects of ultrasound, laser, and electrotherapy in the treatment of OA in the fingers are not well documented. Experience has shown limited effects, typically only short term, with an often inappropriate cost–efficiency ratio.
11.2 PIP Joint Replacement
11.2.1 General Remarks
PIP joint arthroplasty is a widely accepted procedure in joints with either OA or in posttraumatic arthritis. In inflammatory conditions like rheumatoid arthritis, the indication depends on the disease activity and on the pattern of bone and joint destruction. Prerequisites are intact tendons and at least some residual joint stability. Although no exact degree of instability can be defined, lateral deviation beyond 30 degrees are difficult to treat successfully; they are likely to fail.
PIP arthroplasty has a shorter history than MCP joint replacement. For decades, joint arthrodesis was the standard procedure for painful PIP joint destruction, and the functional results of this procedure were generally reported to be good. 9 Pellegrini and Burton 10 reviewed a number of patients who had undergone different procedures for PIP joint destruction. They observed that arthrodesis in the radial digits brought an improvement in the lateral pinch, while arthroplasty in the ulnar digits gave reasonable functional mobility with good pain relief. Based on this analysis, the authors were not able to make a definitive recommendation on the optimal procedure for destroyed PIP joints. Since that publication, however, several authors have advocated the concept of reserving PIP arthroplasty for ulnar digits and treating the index finger, which is the main partner for pinching with the thumb, with PIP joint fusion.
Contraindications to PIP joint replacement include the classic criteria of insufficient bone stock, missing or dysfunctional tendons, and severe tendon imbalance, especially contracted boutonnière and swan-neck deformities. In severely contracted joints with a long-standing history of immobility, PIP joint fusion in a functional position may be a better choice than implant arthroplasty. Severe joint instability and deformity of more than 30 degrees is extremely difficult to correct with an implant and is a relative contraindication to arthroplasty.
11.2.2 Choice of Implants
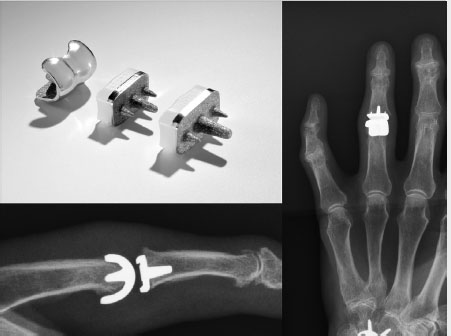
The choice of implant and the surgical approach used are the two most frequently discussed issues in PIP arthroplasty. A variety of implants is available, but only a few series with adequate long-term follow-up have been published. Silicone implants (Fig. 11.1), introduced by Swanson in the early 1960s, are still the gold standard for newer generations of implants with respect to functional performance, revision rate, and long-term outcomes. Silicone joint spacers carry a risk of implant breakage and, much less commonly, silicone synovitis. Overall, the silicone spacer produces fairly consistent results with good pain relief and reasonable function, with an arc of motion of 40 to 60 degrees. Silicone synovitis is not a hallmark of PIP joint arthroplasty as it has been historically with wrist implants. Only a few cases of silicone synovitis have been reported and, although implant failure is seen, it does not necessarily lead to revision. 11 , 12 , 13 , 14 No randomized controlled trials with series of different silicone implants in the PIP joint are available, and analysis of the different case series suggests similar results for most of the Silicone implant designs.

The newer generations of PIP joint implants follow the principles of surface replacement with a two-component concept. 15 , 16 , 17 The proximal component replaces the bi-condylar head of the proximal phalanx and the distal component has a convex surface, which articulates with the head. Most of these implants do not represent a real resurfacing concept, since a significant amount of bone must be resected and long stems for both components are needed to provide adequate bone fixation. However, the newest generation of implants provides a real surface replacement with a very short-stem subchondral bone fixation (CapFlex , KLS Martin Group, Tuttlingen, Germany) (Fig. 11.2 and Fig. 11.4).
Several material combinations are available, from the classic chrome cobalt/polyethylene to ceramic/ceramic and pyrocarbon/pyrocarbon. Although pyrocarbon has excellent biocompatibility and gliding characteristics, problems have been reported, with difficulty achieving osseous stability and reports of joint squeaking. 18 , 19 , 20 , 21 , 22 Similar problems have been observed with ceramics on ceramics. The most frequently used combination is still metal on polyethylene. According to the often-cited recommendation that the polyethylene should be on the concave side, most implants follow that principle. However there are implants on the market which have reversed this principle. The Tactys (Stryker USA) (Fig. 11.3 and Fig. 11.4) implant has the implant head made out of polyethylene and shows no adverse effects in the midterm results. 16 , 23


Most of these implants can be used without cement, although some of them require cementing for primary fixation in the bone. The majority of surgeons prefer noncemented implants, since revision is easier, and removal of the implant causes less damage and bone loss. Overall, the newer generation of PIP implants based on the resurfacing concept seems a logical development in PIP arthroplasty, but most of them have not yet stood the test of time and long-term studies are still lacking for most implant designs.
The concept of resection–interposition arthroplasty, with a volar plate for example, similar to what has been described by Tupper for the MCP joint, is reported only for traumatic or posttraumatic conditions. 24 , 25 Depending on the existing condition and the soft tissue configuration, this technique has an inherent danger of producing an unstable PIP joint, especially in the radial digits.
The choice of implant depends on several factors, including the surgeon’s experience, the local anatomical situation, especially the bone stock, and the surgical approach. Silicone devices, which act as joint spacers, are by far the most forgiving implants. They provide reproducible results even in cases with difficult bone stock and with limited surgical experience. They can be implanted easily using different surgical approaches. More complex, two-component joints need adequate bone stock; no large cystic defects can be allowed to exist with implants, as they must be inserted without cementing. Correct placement, with the goal of restoring the biomechanical center of rotation, needs some experience. Some of these implants are supplied with resection guides, which can be used only with a dorsal approach. In addition, some prostheses need more space for implantation, which also means that a dorsal or lateral approach is required.
11.2.3 Combination of Different Interventions
Since osteoarthritis affects different joints, it is necessary to think about different combined interventions at the same time, according to the patient’s symptoms.
If cases of several painful PIP joints it may be appropriate to operate on multiple joints at a single operation. During rehabilitation the fingers are typically mobilized together, so it is helpful to have neighbor fingers, which tolerate buddy splinting. Every different combination is possible as long as the rehabilitation program is not compromised as this can cause marked adverse outcomes.
The combination of DIP surgery, most often joint fusion, and PIP arthroplasty at the same finger or in the same hand is appropriate. Although the finger will have more postoperative swelling, the immobilization of the DIP and the movement of the PIP joint are complimentary.
Combining thumb base surgery and PIP joint arthroplasty is not so reliable. They are often better treated separately. Typically, the most symptomatic joint needs then to be addressed first.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








