Abstract
Arthroplasty of the proximal interphalangeal (PIP) joint of the finger remains an established surgical treatment option for the arthritic and painful PIP joint. Various materials and surgical approaches have been used. The first generation arthroplasty consisted of silicone spacers. Outcomes of this type of PIP joint arthroplasty generally showed very good pain relief. Several complications were reported though, including implant fracture or loosening. This led to the concept of resurface replacement arthroplasty (second generation), which aims to relieve pain, restore range of motion and maintain stability of the PIP joint. Understanding of current biomaterials and the complex PIP joint anatomy and biomechanics resulted in introducing new implants, which could achieve very good pain relief and good range of motion of the PIP joint, compared to arthrodesis. In this chapter these second generation implants are introduced.
Key words
arthroplasty – resurfacing – proximal interphalangeal joint – pyrocarbon – titanium – ceramic12 Second-Generation Surface Gliding Proximal Interphalangeal Joint Implants (Metal, Pyrocarbon, and Ceramic)
12.1 Introduction
Osteoarthritis of the proximal interphalangeal (PIP) joint is a frequent cause of pain and loss of function of the hand. Pain relief and preservation of a satisfactory range of motion (ROM) are the goals of arthroplasty of the PIP joint as an alternative to arthrodesis. Over the past four decades silicone implant arthroplasty has become a standard procedure in the surgical treatment of PIP joint osteoarthritis. 1 , 2 , 3 The main complications of silicone implants, such as poor long-term ROM and implant fractures (Fig. 12.1a, b), can, in theory, be avoided using new resurfacing implants. 5 , 16 , 19

12.2 Characteristic of Implant or Technique
High rates of loosening, implant breakage, and restricted ROM with silicone and semiconstrained implants have led to new treatment strategies. 8 The development of the new PIP joint implant by Avanta (San Diego, USA) with its first clinical application at the Mayo Clinic (Rochester, USA) in the early 1980s signaled the birth of second-generation surface gliding PIP joint implants. 18
12.2.1 SR-PIP Prosthesis
The surface replacement PIP (SR-PIP) joint arthroplasty implant consists of a distal titanium shaft with biconcave joint surface made of ultrahigh-molecular-weight polyethylene (UHMWPE) and a matching proximal component consisting of a titanium shaft and core, as well as a joint surface made of a cobalt chrome alloy (Fig. 12.2). The matched opposing joint surfaces help create lateral stability and congruity. The shape of the shaft is similar to the shape of the medullary cavity and has a slight dorsal convexity. The implant can be cemented (polymethylmethacrylate; PMMA) or inserted using a press-fit technique. The implant system is available in five different sizes.

12.2.2 Pyrocarbon Prosthesis
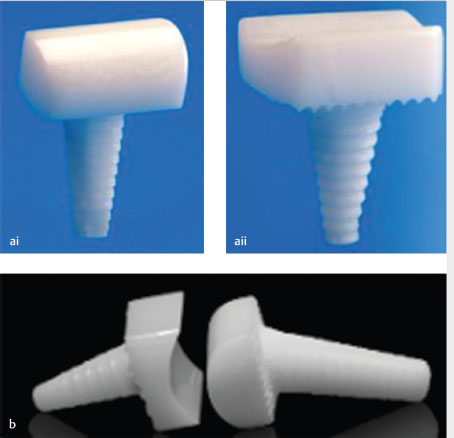
This implant (Ascension, Plainsboro/New Jersey, USA) is made of pyrocarbon, a wear-resistant graphite alloy created from hydrolysis of hydrocarbon gas (Fig. 12.3). It has a similar bicondylar design as the SR-PIP implant. The key advantages of pyrocarbon implant include its biocompatibility, due to its inert properties, and the material’s high level of resistance and high load-bearing capacity. The implant consists of separate proximal and distal components, which are available in five different sizes. It is implanted exclusively using a press-fit technique.

12.2.3 Ceramic Prosthesis
An unconstrained, ceramic prosthesis (Fig. 12.4) PIP arthroplasty has been manufactured by the MOJE company (Petersberg/Germany); it is now being offered in its third generation. It has a similar bicondylar design. It has a volar tilt of 8 degree of the proximal and distal components, longer conical stems as well as a slope of 2 degree in the proximal and 6 degree in the distal component. The purpose of this new prosthesis was to more closely imitate the normal anatomy and physiology of the PIP joint as it preserves the collateral ligaments. The components are made of zirconium oxide ceramic with an additional bioceramic hydroxyapatite coating. The conical implant shafts have grooves to increase surface area for an optimal osseous integration. It is implanted using a press-fit technique.
12.3 Indication and Contraindication
The indication for PIP joint arthroplasty is joint destruction as a result of osteoarthritis, posttraumatic arthritis, or rheumatoid arthritis. 6 If pain persists after appropriate conservative management or if joint instability leads to functional impairment, operative treatment is indicated. The main treatment options are arthrodesis, arthroplasty, or vascularized joint transfer. 4 While both arthrodesis and arthroplasty typically give good pain relief and improvement in stability, the benefits of an arthrodesis are achieved at the cost of lost motion. This is a significant drawback especially for active patients. In contrast, the arthroplasty aims to maintain or improve the range of PIP joint motion while reducing pain, thus improving the hand function. In the published literature, the total ROM in the PIP joint after successful arthroplasty is expected to be around 50 to 60 degrees. 8 , 9 The ROM is dependent in part on the preoperative ROM; the greater the ROM preoperatively, the greater it will be postoperatively. The choice of the surgical treatment will also depend upon which finger is affected. PIP arthroplasty is mainly performed in the middle, ring, and small finger in order to improve grip function. In the index finger, lateral stability of the PIP joint is essential for the key pinch strength. In cases of severe deformity and instability, some hand surgeons may prefer joint fusion for the index finger, as the capacity to correct these through arthroplasty is limited.
The contraindications to arthroplasty are severe chronic boutonniere or swan-neck deformities, insufficient bone stock for example after infection, insufficiency of the collateral ligaments, or long-lasting advanced joint contracture. However, there is a clear trend in favor of arthroplasty in recent years as even limited mobility of the PIP joint may improve overall hand function. Generally, the second-generation implants show promising results in short-term follow-up data. The definitive role of each individual implant, however, is yet to be established.
12.4 Results in the Literature
12.4.1 Results for SR-PIP
One of the first studies to investigate long-term outcomes after arthroplasty with the SR-PIP implant was by Sauerbier et al. 2 , 18 They reported on 82 implants in 60 patients with a mean follow-up of 64 months. The PIP joint ROM increased from 31 to 47 degrees postoperatively; over 70% of patients were pain-free. Similar results were reported by Vogt et al. They reviewed 66 implants in 53 patients. Surgery could improve ROM at approximately 20 degrees and led to a substantial reduction in pain. 7 Murray et al reported similar results in 67 implants in 47 patients at a mean follow-up at 8.8 (range 0.1–31.8) years. They reported significant improvement in ROM and pain. Their mean ROM increased to a mean of 40 degrees (range 0–160) and the mean VAS (visual analog scale) pain score was 3 out of a maximum of 100. 8 Of note, they reported that the rate of complications was significantly higher for the volar as opposed to the dorsal approach. The reported revision rate for SR-PIP implants due to loosening, dysfunction of the extension apparatus, or insufficiency of collateral ligaments was around 26% at a mean of 9.3 years in a study of 39 implants in 21 patients (Fig. 12.5). 9

A successful SR-PIP implant gives good pain relief and ROM but with a high failure rate.
12.4.2 Results for Pyrocarbon PIP Arthroplasties
Several studies on the results of arthroplasty using the pyrocarbon implant have been published since its introduction in 2001 (Fig. 12.6). 10 , 11 , 12 , 13 , 14 , 17 Most authors presented the outcomes in short- or medium-term follow-up studies. The vast majority of the studies have shown good pain relief and maintained or slightly improved ROM. However, reduced ROM compared to preoperatively was demonstrated over a longer follow-up of 10 years. 10 The rates of complications and revision surgery are very variable in the literature with some studies suggesting relatively low complications, satisfactory implant survival rates, and overall good patient satisfaction while others demonstrated unfavorable results. 12 , 13 , 17 The most frequently encountered problem was migration of the implant due to instability at the bone–implant interface as the implant stem does not osseointegrate; at best, the bone will grow up to the stem achieving a stable interface. The high rate of implant loosening and malalignment led some hand surgeons to abandon the use of pyrocarbon PIP arthroplasties. In a large study, Wagner et al analyzed the outcome of 170 PIP arthroplasties with a mean follow-up of 6 (range 2–14) years. 14 The study confirmed the previous series that in cases not requiring revision surgery, pain relief was good and ROM satisfactory.

Overall when successful the pyrocarbon PIP arthroplasties give good outcomes but the concerns over failure of stability of the stems and secondary problems has led to hand surgeons moving away from their use.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








