Rehabilitating the Active ROM
Neuromuscular Consideration
Imagine a common clinical scenario in which a treatment is about to commence for the stiff, non-painful frozen shoulder. Several questions come to mind as we plan the management. Should we begin treatment with passive stretching and later add the active challenges; start both simultaneously; or not bother with passive stretching? When using an active approach, should the movement be broken up to focus on specific shoulder or scapular muscles or focus on whole arm movements? What kind of active movement should be used, functional, extra-functional? Above all, what exactly is being rehabilitated in the active range and is there a way of making the process more effective?
This chapter will explore the active component of range of movement (ROM) rehabilitation and will aim to provide answers to these commonly raised questions:
 What is being rehabilitated in the active ROM?
What is being rehabilitated in the active ROM?
 Which elements of motor control are the targets of ROM rehabilitation?
Which elements of motor control are the targets of ROM rehabilitation?
 Should rehabilitation be of part or whole movement?
Should rehabilitation be of part or whole movement?
 Can passive approaches help recover motor control?
Can passive approaches help recover motor control?
 How does focus of attention influence recovery of active ROM?
How does focus of attention influence recovery of active ROM?
Goals and Focus of Attention
Curiously, what we focus on while we train or move can influence learning and the efficiency and effectiveness of our movements. When we observe human movement, a large selection of this repertoire is directed towards external goals: to reach for a cup, hit a ball or walk across a room. Movement goals are rarely internal to specific body parts; we do not set out to move our limbs, joints or contract specific muscles.1 Whether the focus of attention is external or internal has important implications for ROM rehabilitation.
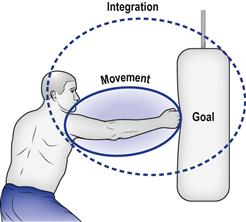
For an outsider observing a person performing a task, say lifting a cup, the action can be broken into two components (Fig. 8.1): the movement that typifies the task (unique arm movement) and the goal of this movement (to lift the cup). However, this separation is artificial. In most activities the movement and its goals are a unified response and not separate entities.2 When we are learning a new task the movement and its goal are integrated and represented internally as images of the goal. The intention to attain the goal triggers the execution of the associated movement, including all the anticipatory postural adjustments that precede it.3–6
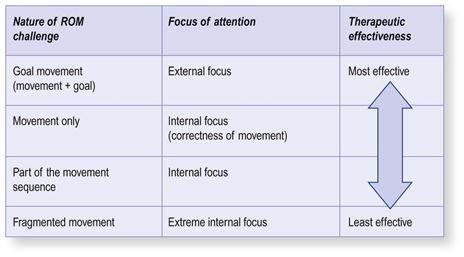
The integration of the movement with its goals and the direction of focus create an order of effect in ROM management (Fig. 8.2). Movement, motor learning and recovery are most effective when the focus of attention is directed towards external goals, i.e. training or rehabilitation that engages this natural integration.7–14 Less effective is rehabilitation in which the focus is internal, on movement itself and separated from its goals. Below this level is the “extreme” internal focus in which movement itself is fragmented into smaller units to become the focus and goal of rehabilitation. Here, the focus of attention is directed towards specific muscles or joints that make up the movement.
Internal focus is often represented in rehabilitation as “correctness of movement”, where faults in movement are identified and corrected. It can have a negative or positive influence on movement depending on the the skill level of the individual. It tends to degrade task performance if the person is already skilled in the task. It has a positive effect when the individual is learning a novel task. However, in ROM rehabilitation the individual is often experienced in the task but is unable to perform it because of physical/motor constraints. Hence, external focus is more effective, whereas internal focus is mostly superfluous and may even be detrimental in ROM rehabilitation. Extreme internal focus is often represented in ROM rehabilitation by contract–relax methods or by muscle-by-muscle or muscle chain rehabilitation. From a motor control perspective it is considered to be the least effective form of training and rehabilitation.
The evidence to support the use of goal-orientated movement in rehabilitation is derived from focus-of-attention studies.7–14 In these studies individuals are instructed to focus either on the goal/outcome of the movement (external focus) or on a particular part of the body (internal focus). It was demonstrated that even simple tasks such as biceps curls are executed more effectively and efficiently under external focus (concentrating on the curl bar) rather than internal focus (concentrating on the biceps muscle or movement of the arm). The group using internal focus had lower electromyography (EMG) activity than the external focus group, although both groups were lifting the same weight.15,16 In a study of force production in the leg, subjects were instructed to either “push your foot against the plate” (external focus) or “push with the muscle of the calf” (internal focus).17 Using external focus resulted in less error in force production, more efficient co-contraction and optimized EMG activity. Similarly, in studies on jump height, subjects were instructed to focus externally on the goal, “concentrate on the highest rungs”, or internally, “concentrate on your fingers”. The external focus group demonstrated increased jump height and greater force production while exhibiting lower EMG activity.18,19 The effects of focus of attention have also been observed in trunk muscle activation during sudden load change. In this study, a load was applied to the subject’s back and then suddenly removed. Throughout that task subjects were instructed to resist the load either by their naturally chosen manner (external focus) or by abdominal bracing (internal focus).20 The naturally selected manner resulted in more effective muscle recruitment patterns of the spine. Conscious, voluntary overdriving of this natural pattern resulted in unbalanced muscular activation patterns and increased the loading on the spine to dangerously high levels.
Overall, the studies on focus of attention demonstrate that focusing on the outcome of the movement rather than on the body and its workings enables the individual to produce greater peak forces, execute faster movement, and increase joint movement accuracy with less muscular activity.14,15,18,19 External, goal-focused training engages the individual in whole movement patterns that promote movement economy.17 It also optimizes motor learning by promoting movement automatism earlier in the training as well as facilitating transfer of learning to novel situations (Ch. 5).18,21 These studies suggest that an external focus of attention is a more effective strategy for rehabilitating the active ROM.
External–internal focus in ROM rehabilitation
The difference between external and internal focus approaches has important practical manifestations in shaping the ROM challenges. This can be exemplified by flexion rehabilitation of the shoulder. In the internal focus approach, the patient is instructed to contract their anterior deltoid, elongate the pectorals, stabilize the scapula and so on. In the external goal approach, the patient is instructed simply to reach with their hand to the ceiling. The outcome is likely to be the same for both approaches – a full flexion range. However, in the goal approach the individual is training in more efficient movement patterns which are within task. This raises the potential for transfer of training gains from the rehabilitation to functional activities (Ch. 5).7–14 Furthermore, external focus is clinically more economical. Minimum instruction is producing a maximum effect. The patient is not required to have any knowledge of anatomy or movement physiology; more importantly, they do not have to learn anything new. The rehabilitation is using what the patient already knows. In the external focus/goal approach, the patient needs only a modest training investment to recover control of the shoulder. In the internal approach the patient is required to learn a new complex movement pattern, which is less effective and efficient and which often demands greater therapist involvement and additional treatments.
Regression from goal to movement level
There are occasions when attention could regress from an external to an internal focus. Imagine a patient who has flexion contractures of the elbow. When attempting a goal movement, such as reaching, rather than extending their elbow the patient may compensate by twisting and bending forward. In this situation it could be useful to instruct the patient to focus internally, on the elbow, and attempt to straighten the arm while reaching. However, even when the rehabilitation regresses to a movement level (“keep the elbow straight”) it should aim to be within the context of the overall goal (“keep you elbow straight while reaching for the cup”).
There are clinical solutions to limit postural compensations and minimize the need for internal focus. In the elbow scenario above, the forward trunk movement can be restrained by instructing the patient to hold the back of the chair with the opposite arm while performing the reaching movement (Ch. 13). Another strategy is to let the patient “cheat” and bend forward, but, then, place the target even further away until forward bending is no longer possible. In both of these examples the patient will be forced to extend the elbow maximally to reach the target. A similar tactic can be used to recover flexion and abduction range in a frozen shoulder (Ch. 13). Often, a seated patient will use trunk side-bending to compensate for abduction restriction, and trunk extension to compensate for flexion restrictions. This can be overcome by placing the target further away from the body, laterally or in front, forcing the patient to execute greater shoulder abduction and flexion movements.
Task-specific Muscle Recruitment
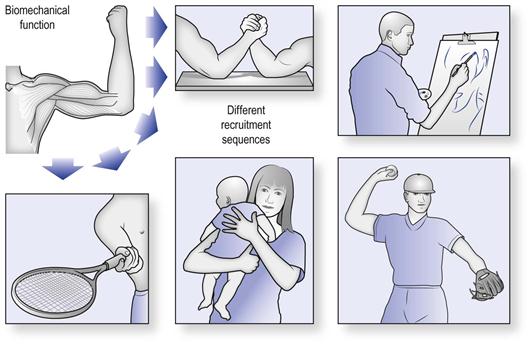
The organization of movement around its goals means that any given muscle will participate in many different tasks, rather than a specific one (Fig. 8.3). This means that muscle recruitment is task specific.22–27 Task-specific recruitment can be likened to a speaker (the muscle) through which different music tracks (motor programmes) can be played. For example, there is a completely different recruitment pattern of the trunk muscles during standing, walking, reaching to the sides, forward bending or lifting or any other imaginable movement.26–30 We cannot claim that the spinal multifidus muscle is exclusively designed for any one of these activities (as is often claimed in many physical therapy approaches). However, we could state that its anatomical location and mechanical function mean that it has a varying role in all these movements, and many more.
Integrate or fragment?
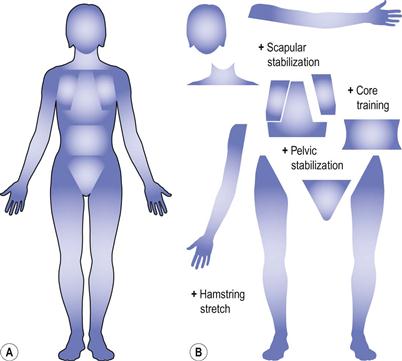
Task-dependent muscle recruitment determines whether a movement should be rehabilitated as a whole or fragmented to smaller anatomical units (Fig. 8.4). Rehabilitating a specific muscle or muscle chain is unlikely to improve the performance or recover the control of the whole task. This is because the task determines the muscle’s activation pattern and not the other way round. It would be like trying to learn a tennis serve by practising biceps activation, triceps and then forearm control, and so on. The only way to recover normal function is to practise the task itself, during which the whole recruitment sequence is rehearsed simultaneously.
Single muscle or muscle-chain activation simply does not exist in motor organization or in the physiology of movement. ROM rehabilitation that favours movement fragmentation is more likely to improve the specific fragmented activity but not the whole movement (Fig. 8.5).31 For example, training that improves the local power at the ankle or at the ankle and knee fails to transfer to gains in vertical jumping, although this task depends on these neuromuscular components.31 Likewise, exercises that isolate parts of the kicking action are not recommended because they do not appear to transfer well to kicking performance; training should be of the whole kicking action.32 It has also been demonstrated that training in isolated tasks, such as hip flexibility or trunk-strengthening activities, does not improve the economy of walking or running.33
Further support for whole movement training comes from the focus-of-attention studies described above. Training that promotes external focus is essentially engaging the individual in whole movement training, whereas internal focus is closely related to movement fragmentation. As discussed, external focus, goal-orientated movement provides more effective and efficient movement patterns. By normalizing the task, adaptation occurs simultaneously throughout the neuromuscular axis: centrally as motor control changes and peripherally as muscle adaptation.
If Aristotle was alive now he would have pointed out that “The task is different from the sum of its muscles and joints”.
Synergy in pathology
Take a task such as a high kick. It requires an explosive shortening contraction of the hip flexors. But the success of this movement also relies on the simultaneous “explosive relaxation” and elongation of the hip extensors.34 So muscles do not work alone but in complex synergies.
Movement synergy means that when a muscle is affected it will inevitably alter the control of all its synergists. It has been demonstrated that induced fatigue in the hamstrings will influence the control of non-exercised quadriceps. Similarly, induced fatigue in the biceps influences triceps control.35–37 This effect was shown to spread even to more distant synergists. For example, fatigue in quadriceps will also influence the control of the non-exercised gastrocnemius muscle.38 So, even in pathology, muscles do not work alone but are controlled in complex synergies.
The interplay between synergists suggests that, if one muscle group is pathologically shorter, the control of all the synergists is likely to change. Imagine a clinical situation in which a patient with reduced hip ROM tries to recover the ability to perform a high kick. There are two potential therapeutic approaches: traditional fragmentation of movement, treating each loss separately, or using task-specific whole movement approaches. In the traditional approach the patient might be given hip flexor resistance exercises to improve active hip flexion and hamstring exercises to increase antagonists’ extensibility. However, such fragmentation cannot capture the complex intermuscular coordination of the synergists. The pattern of recruitment during this procedure is highly dissimilar and therefore non-transferable to a high kick (see specificity and transfer of training, Ch. 5). The complexity of intermuscular coordination and its specificity to particular exercise can be resolved by simply challenging the whole movement, in the context of the goal task, i.e. practising high kicks will challenge and normalize that task.
Focus of ROM Rehabilitation
We have so far identified that ROM rehabilitation should be of whole movement and practised within the context of the goal task. However, we are still left with the question of what is being rehabilitated within the task. To answer this question we need to explore what happens to the task parameters in the presence of injury and pain.
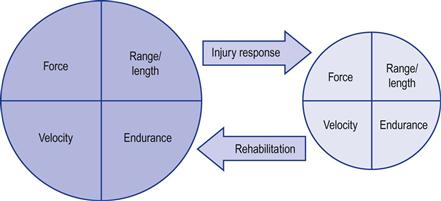
The task parameters are controlled centrally as part of normal movement organization. In the presence of injury, pain or even fear of movement the task parameters are attenuated as a protection strategy (Fig. 8.6).39–61 This movement reorganization serves to reduce the physical stresses imposed on the injured areas. The outcome is the experience of force loss, slower movements, limitation in movement range and early onset of fatigue, which serves to reduce iteration of potentially damaging movements. This strategy is universal and can be seen throughout the body in various musculoskeletal conditions. It is a normal and advantageous motor control response; it does not represent a central pathology. The capacity for central adaptation and motor reorganization is preserved and therefore the likelihood for active ROM recovery remains high. The task parameters can also be affected by central nervous system (CNS) damage.62–65 In these conditions central adaptive capacity is reduced and therefore the potential for ROM recovery is more limited (Ch. 3).
The production of force, velocity, length and endurance are also peripheral phenomena of the muscle’s structure and physiology. Fortunately, by challenging the task parameter there is concurrent stimulation and adaptation of the whole neuromuscular axis, central and peripheral, motor control and muscle. They cannot be targeted individually as is sometimes believed. This means that, in ROM rehabilitation, we do not have to focus specifically on the shortened muscle. Performing a task at end-range will drive simultaneously the central and the peripheral recuperative processes.
There are other movement components that can be the focus of ROM rehabilitation such as coordination and balance. These are outside the scope of this book and can be found in Lederman.42
Importance of Cognition
Cognition is a broad term to describe mental processes such as attention, understanding, remembering, thinking, rationalizing, memorizing, imagination, planning, decision-making and problem-solving. It has been demonstrated that these play an important role in motor learning and recovery of movement control in various musculoskeletal conditions and following CNS damage.66–70
Cognitive factors play an important role in ROM rehabilitation. Learning a movement pattern or recovering control requires conscious attention to particular aspects of the movement, being aware of the ranges affected and the daily tasks that could be used to challenge them.71,72 Cognitive management also includes the patient’s involvement in problem-solving, decision-making, goal-setting, planning and scheduling of practice/rehabilitation.18,69,70,73–76 It has been shown that treatment can be more effective if these factors are an integral part of the management.18,69,70,73–76
The successful integration of cognitive elements in the treatment depends on the cognitive state of the patient, the therapist’s awareness of their importance and effective communication but also on the therapeutic relationship between the practitioner and patient (see psychological consideration, Ch. 11). For example, patients who have cognitive losses as a result of CNS damage may have difficulties in understanding instructions or making choices. Under these circumstances, movement rehabilitation may be prolonged or impeded.
Cognition and feedback
Imagine you are learning a new task, such as a golf swing. The rate of learning and your skill of performance will partly depend on feedback from your own body and the instructor. In a similar manner, the recovery of active ROM can be enhanced or impeded by provision or withdrawal of feedback.77–86 In ROM rehabilitation, feedback can take different forms: sensory feedback, task feedback and feedback on recovery progress.
Sensory feedback is the intrinsic, ongoing information provided from proprioceptors and other sensory modalities such as vision, auditory and vestibular (again, for full discussion, see Lederman42). It is a subconscious form of feedback, but it can be raised to a cognitive, conscious level by drawing attention to the body or to a particular sensory modality.87–89 It is often used during stretching to raise awareness of tension or to promote relaxation in particular parts of the body. Although there is much interest in physical therapies in this form of feedback, it is fairly immutable to modification by physical means – you can become more aware of it but cannot change it..42
Task feedback is often provided by the therapist and contains information about the “correctness” of the movement (“hold the racket this way”), the movement sequences (“swing it like this”) or the quality in performance (“good shot”). Sensory and task feedback are often provided as verbal instructions, visual demonstration and physical correction of movement by the therapist/trainer.44,90
Generally, feedback is more effective if it promotes an active gathering of information and problem-solving by the patient.91 For optimum learning, guidance should be kept to a minimum and rapidly reduced or fully withdrawn at the earliest opportunity.9,68,86,92–95 Furthermore, training is found to be more effective when the feedback emphasizes successful performance and ignores less successful attempts.19,96
Tracking recovery progress is another important form of feedback which is usually set against specific treatment goals. Tracking can be of various treatment outcomes such as changes in ROM, pain and functional improvements.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree