CHAPTER 11 Reconstruction of the Medial Patellofemoral Ligament
Recurrent lateral instability of the patella after traumatic patellar dislocation or subluxation usually requires attention to the medial soft tissue restraints for prevention of future pathologic lateral translation. Historically, procedures for addressing medial restraint insufficiency include reefing, vastus medialis obliquus (VMO) advancements, and nonanatomic tendon transfer procedures.1,2 In addition to shortening or imbrication of the medial soft tissue restraints, several authors have described reconstructing or reinforcing the medial patellar structures with fascia lata, nylon, and even preserved skin.3–6 Earlier proximal procedures for patellar instability can be summarized into two categories—advancement from structures above the patella or nonanatomic attachment from tendons anchored below the patella. Numerous earlier techniques of proximal VMO advancement and extensor mechanism equilibration have been summarized best by Ficat,7 who described these proximal muscle transfers as a dynamic means of patellar control. Baker and colleagues8 have summarized some of the early work of Galliazzi, with emphasis on a nonanatomic static semitendinosus tenodesis for the prevention of lateral subluxation.
ANATOMY
The MPFL is a thickened band of retinacular tissue originating in the saddle area between the medial epicondyle and adductor tubercle and inserting on the proximal third of the medial border of the patella. Typically, the MPFL is approximately 55 mm long and is overlaid by the distal part of the VMO, with fibers merging into the deep aspect of the muscle.9 Current techniques for addressing post-traumatic patellar instability have shifted focus to a restoration of the normal anatomy and the importance of the MPFL. The primary restraints against lateral patellar mobility are passive.10 The trochlea is the most important patellar stabilizer in normal knees beyond 20 degrees of flexion. If the patella is dislocating laterally, the medial restraints must be abnormally lax or deficient.
The MPFL has been shown to be the primary soft tissue restraint to lateral translation of the patella; it functions primarily in the first 30 degrees (before patellar engagement in the trochlea) and becomes lax in flexion.6,10–13 Additionally, if the trochlear groove is deficient (dysplastic), the MPFL takes on an even greater role. The MPFL is believed always to sustain some form of injury during traumatic lateral dislocation of the patella. Logically, a repair or reconstruction of this structure should provide the most anatomic reproduction of normal patellar biomechanics. Even though other medial tissues, such as the medial patellotibial ligament, may contribute to patellar stability, addressing the primary static restraint to lateral patellar subluxation provides the most reproducible and reliable outcomes at present.14 Reconstruction of the MPFL restores tracking to near-normal when the medial restraints are deficient. Current techniques for MPFL reconstruction differ from historical models and VMO advancement because of the emphasis on avoiding the creation of increased patellofemoral contact forces. VMO advancements and proximal reefings tend to tighten, therefore increasing the patellar joint contact forces in flexion. By anatomically reconstructing damaged normal anatomy, we attempt to correct patellar pathology without introducing a mechanism that will lead to medial facet overload and subsequent degenerative patellar disease.
PATIENT EVALUATION
History and Physical Examination
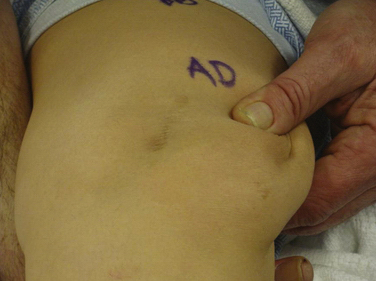
Success, as with any operation, relies mainly on proper patient selection. After an extensive history, the physical examination begins with examining the patient’s standing leg alignment and gait. A standing squat is helpful for demonstrating painful arc of motion and crepitus. We then have the patient flex and extend the knee while seated on the edge of the examination table to assess patellar tracking, specifically checking to see if the patella slides laterally with full extension, a J sign. Palpation of the patella with slight posterior pressure allows us to feel for crepitus and isolate the exact arc of pain better during active range of motion. With the patient supine, we assess lateral patellar translation, looking for abnormal increased glide. Specifically, we examine both knees at full extension and at 30 degrees of flexion (Fig. 11-1). We subdivide the patella into four quadrants and determine the extent (the number of quadrants) that the patella can be shifted laterally over the edge of the trochlea; MPFL patholaxity typically corresponds to 3+ to 4+ lateral glide at 30 degrees of flexion (Fig. 11-2). We also try to determine whether there is a hard or soft end point to translation, which can be helpful in determining whether there is any residual ligament function. Passive patellar tilt is examined to determine tightness of the lateral retinaculum. We have found the Sage sign, passive medial translation of the patella performed at 15 to 20 degrees of flexion, to be helpful in determining the need for lateral release. If the patella can be translated two quadrants or more, lateral release is not necessary, and may lead to debilitating medial instability if performed in this situation. In our practice, we often see patients with previously failed reefing procedures, previous lateral releases, and trochlear dysplasia, which may contribute to a more progressive laxity of medial restraints. In these cases, it is especially important to use the Fulkerson jump test to rule out iatrogenic medial patellar dislocations (postexcessive lateral release), which can present with the patient mistakenly reporting lateral dislocations.
Diagnostic Imaging
Standard imaging includes anteroposterior (AP) weight bearing, posteroanterior (PA) flexed weight bearing, a true lateral at 30 degrees of flexion to assess patellar height and trochlear dysplasia, and axial views (at 30, 60, and 90 degrees of flexion) to look at congruence and patellar rotation or tilt. Assessment of patellar height on the 30-degree lateral is performed using the Blackburn-Peel method, measured off the tibial plateau and articular surface of the patella, rather than the Insall-Salvati method. This eliminates the chance of misreading patella alta or infera, occasionally caused by a long nonarticular “nosed” portion of a patella, such as with a Cyrano-type morphology.15 Trochlear dysplasia is also best assessed on the true lateral view, looking for the crossing sign and presence of a trochlear bump.
We routinely perform a calibrated computed tomography (CT) patellar tracking study with midaxial cuts from 0 to 60 degrees of knee flexion in 10-degree increments to assess patellar tracking from 0 to 60 degrees. This is the range in which stability occurs. The CT study also includes fixed-frame images from the trochlear groove to the tibial tubercle to measure tibial tuberosity-trochlear groove (TTTG) distance. From the CT cuts and Merchant view at 30 degrees, we can determine whether the patella is tilted. Normally, the patella will be centered in the trochlea; however, if the lateral facet is parallel to the anterior trochlea or if the angle formed by the lateral facet and the anterior trochlea is open medially, the patella is tilted. The congruence angle on a standard Merchant view should normally demonstrate that the patellar apex is medial to the bisected trochlea. The sulcus angle can be measured and should be 137 ± 6 degrees.16 A higher measured angle helps us identify a flat, shallow, dysplastic trochlea. Finally, magnetic resonance imaging (MRI) can be helpful in determining the extent of chondral damage in the patellofemoral joint and the status of the soft tissue restraints, as well as ruling out other pathology. We prefer MR arthrography if advanced cartilage sequencing is not available.
This compilation of information is predicated on the understanding that patellofemoral problems are often multifactorial. Factors such as the presence of trochlear dysplasia, poor tissue quality, patellar cartilage damage, hip rotation, alignment, and status of the tibiofemoral joint may influence operative decisions. As a stand-alone procedure, MPFL reconstruction is solely used for instability, whereas distal realignment surgery is better used to address tubercle malalignment with patellofemoral pain and/or instability. It is our experience that a Q angle more than 20 degrees at 30 degrees of flexion or a corresponding TTTG value more than 15 to 20 mm will bring the necessity of a distal osteotomy into serious consideration. In many cases, the presence of both scenarios may require a combined proximal and distal approach. Normal TTTG values, an increased lateral patellar glide, and a history of recurrent patellar dislocations following trauma suggest MPFL incompetence and the need for reconstruction.
TREATMENT
Arthroscopic Technique
Graft Selection
We have used semitendinosus autograft in the past, but it is our current preference to use a semitendinosus allograft. Of note, in petite patients a gracilis tendon is often sufficient. We have found that the allograft performs just as well in this richly vascular, extra-articular environment. If an autograft is used, this is harvested though a separate incision over the pes anserine insertion. This tendon far exceeds the 200 N associated with native MPFL rupture in cadaver models; the doubled graft requires approximately 2000 N for rupture. It is also an order of magnitude stronger (150 N/ mm) than the average stiffness of the MPFL (12 N/mm).10,17
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree