Fig. 11.1
Smith-Petersen transiliac approach for sacroiliac arthrodesis. (a) Incision and window in original description. (b) Exposure of lateral ilium and subsequent modification of transiliac bone window into synovial portion of sacroiliac joint
The gluteal musculature was detached and subperiosteal dissection carried out until the posterior and lateral portions of the ilium were exposed (Fig. 11.1b).
The anatomic projection of the articular portion of the SIJ on the ilium was visualized using the sciatic notch and the “medial gluteal line”, what anatomists refer to as the anterior gluteal line [3], as landmarks. A rectangular “window” was then cut through the ilium through which the articular surface of the sacral side of the joint was visualized. Cartilage and subchondral bone was removed from the sacral side of the joint as well as from the removed block of bone. The block was then countersunk across the defect, which allowed for opposition of cancellous surfaces with the bone block spanning the joint. In his original publication Smith-Petersen made passing reference to seven cases of sacroiliac tuberculosis and three cases of “relaxation” of the joint that had undergone the procedure with successful results though, as was common at the time, no specific data were reported. In the same year Gaenslen reported on a transiliac approach in which a similar window was made after reflecting a partial thickness flap of bone from the posterior ilium (Fig. 11.2) [4].
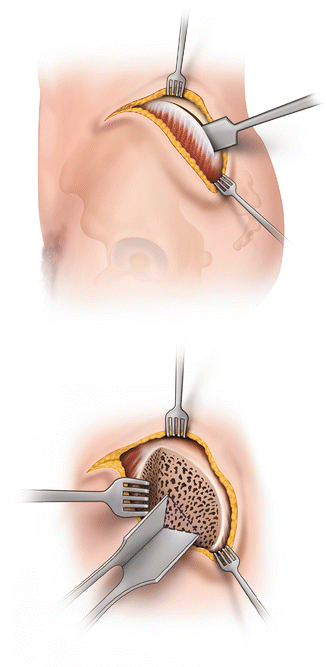

Fig. 11.2
Gaenslen’s transiliac approach for sacroiliac arthrodesis. The outer table of the ilium is osteotomized and a flap reflected with attached gluteal musculature. A triangular window is made to access the sacroiliac joint. After decortication and grafting, the flap was reapproximated with sutures
A triangular window was then made into the synovial portion of the joint through the exposed cancellous surface of the ilium. Decortication of the sacral side of the joint was carried out and local bone graft was placed. The reflected flap of bone and attached musculature were approximated back to the crest using sutures. Blood loss was not reported, but it could be expected that with the exposure of a large area of cancellous bone, blood loss would be higher than with the Smith-Petersen technique.
Smith-Petersen later reported on end results of his technique for patients with tuberculosis of the SIJ [5] and patients with non-tuberculous disorders of the SIJ [6]. Twelve of thirteen (12/13 = 92 %) of patients operated on for tuberculosis had complete resolution of pain following surgery and eight of thirteen (8/13 = 69 %) returned to their prior occupation. It was noted, however, that four patients eventually died from tuberculosis, three from distant involvement due to meningitis or peritonitis and one from a secondary infection and abscess who left the hospital against advice and died 3 months after surgery. In patients with non-tubercular arthritis of the SIJ, 23/26 (88 %) had complete relief of pain. In a follow-up report on his technique, Gaenslen reported on nine patients undergoing surgery either for tuberculosis of the SIJ or sacroiliac “strain” [7]. One patient was considered a failure on the basis of a probable incorrect diagnosis. One patient developed a severe deep infection but ultimately had a good result.
Harris reported on a series of 67 consecutive cases of sacroiliac disease treated with arthrodesis using a transiliac approach similar to that described by Smith-Petersen [8]. He reported 68 % had excellent results, 18 % partially improved, and 3 % had no relief and 1 patient died. Nine percent were lost to follow-up.
Bloom should be credited with the first attempt to perform a minimally invasive sacroiliac arthrodesis [9]. He described a much smaller straight-line incision based on landmarks relating to a line drawn from the (PSIS) to the anterior superior iliac spine (ASIS) (Fig. 11.3a).
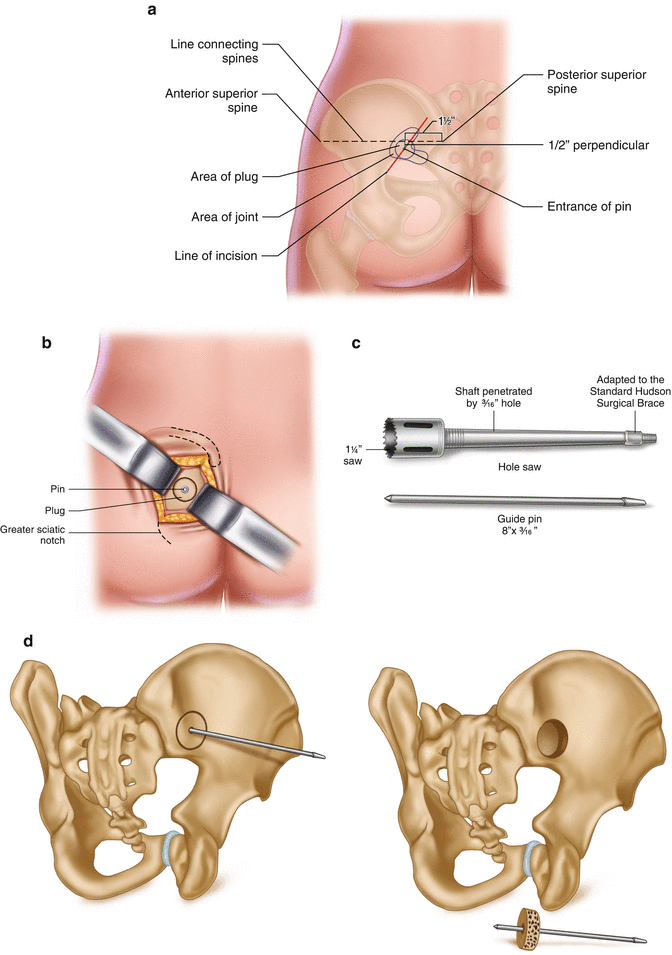

Fig. 11.3
Bloom’s description of novel technique for sacroiliac arthrodesis with minimal soft tissue disruption. (a) Landmarks and planning for incision. (b) Exposed outer surface of ilium and planned bone plug cut. (c) “Hole saw” used for removal of bone plug accessing the sacroiliac joint. (d) Cadaver pelvis showing location of graft [9]
A perpendicular to this line was drawn inferior to a point 1.5 in. anterior to the PSIS along the first line. A point ½ inch from the original line along the perpendicular was selected as the center of a 3-in. incision that was made in the direction of the gluteus maximus muscle fibers. Blunt dissection was utilized to separate muscle fibers and palpate the ilium and the sciatic notch (Fig. 11.3b).
The central point of this incision overlies the synovial portion of the SIJ. A Steinman pin was then driven across the joint perpendicular to the surface of the ilium. A 1.25 in. diameter hole saw (Fig. 11.3c) was then used to cut a cylindrical core of bone through the ilium and across the joint into the sacrum.
The plug was removed, the opposing cartilage surfaces were excised, and the plug was then reinserted and countersunk providing a cancellous plug spanning the joint (Fig. 11.3d).
Per Bloom, the operation could be accomplished bilaterally in “…fifteen to twenty-five minutes, including closure of skin, without any undo haste.” Bloom noted that patients felt well the day following surgery and did not require pain medication. He allowed them to be mobilized early in contrast to other postoperative regimens at the time that prescribed plaster beds and spica casts for up to 5 months [10]. He allowed them to “sit up as soon as they desire” and to be without restrictions in 14 days.
Unfortunately, Bloom only reported on the procedure in four patients and never published any further information on his technique. In the same year, Key also reported on a variation of the Smith-Petersen technique intended to reduce the exposure and soft tissue trauma [11]. Key described a straight-line incision parallel to the fibers of the gluteus maximus just below the PSIS. Blunt dissection was used to separate the gluteus maximus from the gluteus medius, and the ilium was exposed. The standard Smith-Petersen window was then made with much less exposure than in the original description. The author described having used the procedure in eight patients with good results, but, as was common at the time, no specific data were given.
There is a marked absence of mention of sacroiliac arthrodesis in general in the literature for most of the next 50 years. Hodgson reported on 11 cases of pyogenic SIJ infection, which were drained by a Smith-Petersen transiliac approach with 100 % satisfactory results but did not describe the surgical procedure as an arthrodesis per se [12]. Waisbrod et al. [13] reported on arthrodesis of the SIJ for chronic low back pain in 1987 with a very limited description of their technique. It is clear from CT scans included in the article, however, that they used a direct posterior open approach rather than a transiliac approach. Moore first reported on results from a modified Smith-Petersen approach using a smaller incision and incorporating internal fixation in 1992 [14]. Thirteen patients were presented in his initial report who had been diagnosed by CT scan or fluoroscopically guided injections and who had failed conservative treatment. All 13 patients underwent fusion by a modified Smith-Petersen approach with internal fixation. Results were reported as excellent in ten patients, fair in one, and poor in two patients. The only complication reported was a pseudarthrosis in two patients. Subsequent reports by the same author [15–21] using the same transiliac approach documented favorable results with few approach-related complications. In the final review of 120 operations in 110 patients, there was one superficial wound infection, one incidence of over-penetration of a fixation screw causing temporary neuritic pain requiring screw removal, and one case where an intraoperative fracture into the sciatic notch occurred when creating the bone window using an osteotome. The fracture was fixed with a single screw during the index procedure without subsequent morbidity. A symptomatic pseudarthrosis rate of 8.9 % (10/110 cases) was reported, seven of which were reoperated with five going on to radiographic union and a good clinical result. Eight of ten patients with pseudarthrosis were smokers. In patients with isolated sacroiliac pathology, 90 % were classified as clinical successes. Operative time averaged 1 h and 15 min and blood loss averaged 200 cc.
Kurica reported on 32 patients who underwent open sacroiliac arthrodesis by a modified Smith-Petersen transiliac approach without instrumentation and reported a fusion rate of 94 % (30/32) but did not detail clinical results [22]. Giannikas et al. reported on five patients operated on using two Cloward-type grafts placed across the SIJ without any associated instrumentation [23]. Four of five operated patients reported complete relief of symptoms at a mean follow-up of 29 months (range 25–41 months) with one patient reporting partial improvement. Residual symptoms in the fifth patient were ascribed to coexistent lumbar osteoarthropathy.
Buchowski et al. [24] reported on functional and radiographic outcomes of 20 patients who had undergone sacroiliac arthrodesis using a modified Smith-Petersen technique with screw and plate fixation. Solid arthrodesis was found in 17/20 patients (85 %) though only plain radiographic criteria were used. Only 15/20 (75 %) of patients completed preoperative and postoperative SF-36 forms, but of those completing forms, significant improvements were seen in physical functioning, role physical, bodily pain, vitality, social functioning, role emotional, and pain indices. Complications included pseudarthrosis (15 %), deep wound infection (10 %), and painful hardware (5 %).
One frequently cited but seldom critiqued report is the article by Schutz and Grob that describes poor outcomes from sacroiliac arthrodesis [25]. This article stands in distinction from virtually every other article on sacroiliac arthrodesis in that satisfactory results are generally reported in the literature and this article reports negative results in the experience at a single center using a novel technique. Critics of sacroiliac arthrodesis often cite this reference as being evidence that SIJ arthrodesis has been associated with poor outcomes [26, 27]. Examination of the study, however, reveals multiple factors that limit any generalization of their observed results to the subject of sacroiliac arthrodesis.
The authors reported on 17 patients thought to have SIJ-mediated pain who underwent surgical treatment, though diagnostic criteria varied from image-guided diagnostic injection to positive bone scans to pain relief from a trial of external fixation. By their own report, only 30 % of the patients were considered to have “definite” indications for a sacroiliac fusion. Additionally, 10/17 (59 %) had an average of 2.7 prior surgeries on the lumbar spine and/or SIJs. Of the group of patients who had prior surgery, only two patients reported significant improvement from prior surgical interventions with the remainder reporting limited, transient, or no improvement. As the absence of a symptom-free interval following prior surgery is well known to be correlated with an unsatisfactory outcome from a subsequent surgical intervention [28], the study group was likely predisposed to negative outcomes regardless of the intervention. The authors instrumented and fused both SIJs routinely utilizing a technique that involved bilateral exposure of both lateral and medial surfaces of the ilium, direct decortication of (presumably) the articular portion of the joint, and compression instrumentation that spanned both ilia and included screws placed through the ilium into the sacral ala (Fig. 11.4)
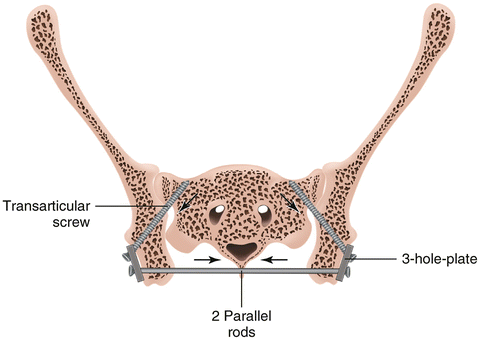

Fig. 11.4
Drawing from Schutz and Grobs article showing technique of novel bilateral sacroiliac arthrodesis and fixation spanning both ilia. Extensive bilateral exposure is necessary involving access to both lateral and medical aspects of ilium for posterior decortication of joint and lateral placement of plate and screws. Posterior sacroiliac ligaments were removed inferiorly
They do not cite a rationale or literature support for routinely fusing both joints, nor do they indicate if any of the patients in the series were experiencing bilateral pain. Operative time was 121.3 min and mean blood loss was 794 cc
Clinical results were reported as satisfactory in 3/17 (18 %) and unsatisfactory in the remaining 14 patients (82 %). They reported their nonunion rate however to be between 41 % (definite nonunion and instability) and possibly 65 % (including those with questionable union). Furthermore, there was a statistically significant association between nonunion and poor clinical result. These data would seem to lead to a conclusion that this particular technique was not effective in achieving the surgical goal. The reported blood loss of 794 cc exceeds that of other reports by nearly a factor of 4, which, even allowing for the fact that bilateral fusions were done, suggests that the technique utilized in this study is associated with greater tissue damage than other techniques [15, 17]. Based on a critical review of the article, the poor results were likely due to variable patient selection criteria, a high percentage of failed low back surgery patients, and a surgical technique that resulted in a very high rate of nonunions. The frequent use of this study as a reference purporting to documenting poor results from sacroiliac fusion represents a lack of familiarity with the details of the report.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







