Figure 22.1
Clinical photograph showing the patient’s forward flexion on his injured shoulder prior to physical therapy

Figure 22.2
Clinical photograph showing the patient’s shoulder abduction on his injured shoulder prior to physical therapy

Figure 22.3
Clinic photographs showing the “hand-over-fist” sign

Figure 22.4
Clinical photographs showing the “hallelujah” sign
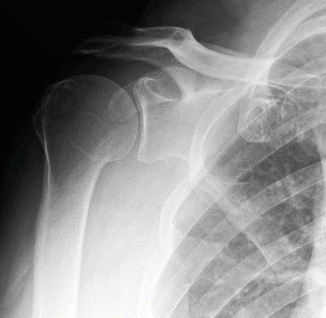
Figure 22.5
AP radiograph of symptomatic shoulder without signs of advanced osteoarthritis

Figure 22.6
MRI of patients’ symptomatic shoulder. (a) Coronal image showing full-thickness supraspinatus tear . (b) Sagittal image showing significant rotator cuff muscle atrophy
Diagnosis/Assessment
The patient’s history, physical exam, and radiographic findings were consistent with a chronic massive rotator cuff tear. Rotator cuff tears are common and become more prevalent as patients age [1]. A systematic review of the many studies assessing prevalence of rotator cuff tears demonstrates that the prevalence of full-thickness tears in the population over 40 years is between 11.8 and 40.8% [2].
It is important to understand that not all rotator cuff tears are the same and there are marked differences among acute traumatic tears, acute-on-chronic tears, and chronic atraumatic tears. Patients with traumatic tears will typically present with an event that caused acute and severe pain in the shoulder with immediate loss of function. Patients with acute-on-chronic tears typically had a history of some mild symptoms prior to a relatively low-energy injury which exacerbated their symptoms. Their pain is significant, but seems to improve over the course of a few days. They may have lost some function, but return of function occurs over a few days. Chronic atraumatic tears are degenerative and are often seen in patients over 60 years old [1–3]. These classically present with insidious onset of shoulder pain with pain at night and loss of function, but typically are related to pain. These tears usually have some degree of muscle atrophy, poor tissue quality, and tendon retraction, making a rotator cuff repair less likely to heal.
Physical examination that employs lag signs can be very helpful to identify large rotator cuff tears [4]. These lag signs can be performed with the arm at the side and externally rotated, the arm held in 90 of abduction and externally rotated, and with the arm behind the back and held away from the spine. When the patient fails to hold this position when the arm is let go, it could be considered a positive test. Lag signs, a drop-arm test, or the inability to raise the arm are the ultimate expression of the weakness associated with massive rotator cuff tears. Interestingly, patients who present with chronic rotator cuff tears and are able to perform either the “hallelujah” sign or the “hand-over-fist” sign will have a high likelihood of successful treatment with physical therapy [5].
Physical examination signs are not particularly useful when patients have small rotator cuff tears [6], and combinations of physical examination tests may be more useful. Murrell et al. found that patients who demonstrated supraspinatus weakness, weakness in external rotation, and positive impingement signs had a 98% chance of having a rotator cuff tear [7]. It must be noted that patients with a rotator cuff tear can present atypically with a full range of motion and good muscle strength due to functional compensation [8]. These patients may require imaging to accurately diagnose the rotator cuff tear.
To evaluate for a suspected rotator cuff tear, multiple imaging modalities can be utilized. Plain radiographs are typically the first imaging modality obtained for shoulder pain. In reviewing plain films, if superior migration of the humeral head is noted on the AP film, a rotator cuff tear is highly suspect. This finding indicates a loss of function of the rotator cuff and appears with long-standing tears. The normal acromiohumeral distance measures from 9 to 10 mm with a range of 7 to 14 mm [9]. An acromiohumeral distance less than 7 mm is consistent with a rotator cuff tear, and a space less than 5 mm indicates a massive rotator cuff tear [10, 11]. Chronic rotator cuff arthropathies can show joint space narrowing, rounding of the greater tuberosity, acetabularization of the undersurface of the acromion, superomedial glenoid wear, and humeral head collapse [12].
Additional imaging modalities include ultrasound and magnetic resonance imaging [MRI]. Ultrasound allows quick and reliable diagnostic imaging for rotator cuff tears; however its accuracy is highly operator dependent [13]. A meta-analysis showed that the sensitivity for ultrasound can range from 66 to 92% and specificity can range from 86 to 94% depending on the size of the tear and the operator [14]. MRI allows for visualization of the tear, as well as muscle atrophy, fatty infiltration, and tendon retraction [15–17]. The sensitivity for MRI ranges from 64 to 92% and specificity ranges from 81 to 93%. MRI arthrography improves the sensitivity range to 91–95% and specificity range to 95–99% [14].
Management
The patient in the case study presented with a chronic rotator cuff tear. At his initial clinic visit he was given an intra-articular steroid injection and a physical therapy prescription specifying the MOON (Multi-center Orthopaedic Outcomes Network ) massive rotator cuff tear protocol. This protocol was based on a systematic review of Level 1 studies that demonstrate effectiveness of exercise for treating rotator cuff disease [18]. This protocol was also used in a large prospective cohort study of patients with symptomatic atraumatic full-thickness rotator cuff tears, with over 75% success [19]. This protocol is available on www.moonshoulder.com.
The protocol begins with supervised physical therapy, two to three times a week with the addition of joint and soft-tissue mobilization. Patients who no longer need joint and soft-tissue mobilization and have developed proficiency with the protocol can be moved to a home-exercise program. Scapular range-of-motion exercises should include shrugs, shoulder retraction, and protraction exercises. Glenohumeral motion should start with pendulum exercises and progress to active-assisted motion and then to active motion as comfort dictates. Active assist exercises can be performed with a cane, suspended with pulleys, or simply with just the uninvolved arm. Stretching should emphasize anterior and posterior shoulder capsule stretching. Strengthening exercises should focus on the rotator cuff and scapular stabilizing muscles. Exercises should focus on internal and external rotation with the arm adducted, as well as scaption provided that the patient does not experience pain with these motions. Scapular exercises should include chair presses, push-ups with a plus, and upright rows [18].
Patients with massive rotator cuff tears and poor function are better served by the protocol described by Levy et al. [5]. This protocol starts with pendulum exercises and active-assist warm-up for the affected shoulder. Once the patient is able to elevate the affected arm in forward flexion with the assistance of the uninjured arm while supine, the patient may then start to try active arm-elevation exercises. After the patient is comfortable with lifting the affected arm alone, resistance training may be initiated using an 8 ounce can progressing to a 1 pound weight. When the patient has become comfortable doing all these exercises while laying supine the bed is then elevated 20 and the steps are repeated until the patient is able to perform all exercises upright.
Importantly, this protocol also calls for strengthening the muscles surrounding the glenohumeral joint, including the deltoid and periscapular muscles. The deltoid muscle is strengthened using resisted exercises involving three motions: shoulder extension, abduction, and forward punches. Lastly, strengthening the periscapular muscles is important so as to control the glenoid during shoulder motion to maximize shoulder function. The two primary exercises the protocol utilizes for periscapular strengthening include serratus punch exercises and upright rows. The serratus punch is performed with the patient lying supine, holding the affected arm at 90 with elbow extended, and then bringing the scapula around the side of the chest wall to “punch” the ceiling, emphasizing scapular protraction. The other exercise is upright rows emphasizing shoulder retraction. The patient is seated in an upright position and then squeezes his shoulder blades together holding for 2 s. Both of these exercises are started with no resistance and then progressed using Theraband resistance bands [5].
Outcome
This 63-year-old male underwent a total of 12 weeks of physical therapy. On the patients’ 6-week follow-up he was able to forward elevate his arm to 140 and his pain had improved by 50%; however, external rotation was still limited to 50 and he still had shoulder weakness with abduction and external rotation. With a positive response in symptoms and motion, therapy was continued for another 6 weeks.
After 12 weeks of physical therapy he subjectively felt 80% better in regard to his pain and function. His shoulder forward elevation as well as abduction had improved to 180 (Fig. 22.7). His external rotation was improved to 70 and internal rotation to L3. He still had weakness in external rotation and abduction; however he was very satisfied with his results.


Figure 22.7
Clinical photograph showing the patients’ range of motion 12 weeks after the physical therapy program. (a) Right-shoulder forward flexion active motion. (b) Right-shoulder abduction active motion
Literature Review
The indications for surgery for rotator cuff tears are not well defined and there is no consensus on who should have surgery. This is demonstrated by the large geographic variation in rotator cuff repair rates [20], and by the great variation in approaches to the same patient as demonstrated by surveys of surgeons [21]. Systematic reviews of the literature demonstrate a paucity of high-level studies, but using the best evidence available (Level 3 and 4), it seems that acute traumatic rotator cuff tears do better if repaired early, age and gender should not affect the decision to have surgery, and strength and/or functional loss will have better outcomes with a successful surgical repair [22, 23].
Pain as an indication for surgery is controversial. The rotator cuff tear severity does not seem to correlate with the patient’s pain, duration of symptoms, or activity level [24–26]. Patient-reported outcomes of failed rotator cuff repair using validated patient-reported outcomes are typically good and cannot be distinguished from successful repairs [27, 28]. Physical therapy for atraumatic tears is successful in over 75% of patients [19, 29, 30]. Finally, while natural history studies of rotator cuff tears demonstrate that some patients will have progression and these patients will statistically have more pain, patients can have progression without pain, or may develop pain without progression making pain a relatively poor predictor of rotator cuff tear progression [31].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








