Figure 20.1
AP radiograph of the right shoulder showing cystic change of the greater tuberosity (arrowhead)

Figure 20.2
MRI of right shoulder showing a supraspinatus tear (arrowhead)
Diagnosis
The patient’s imaging findings were consistent with the diagnosis of a small, partial recurrent supraspinatus tear; however, her weakness on physical exam and continued severe pain with overhead activity appeared out of proportion to her MRI findings. Therefore, the patient was sent for electromyography (EMG) /nerve conduction velocity studies (NCV) which demonstrated suprascapular nerve entrapment at the suprascapular notch along with mild cervical radiculopathy (Fig. 20.3). A cervical spine MRI demonstrated minimal pathology and it was felt that the majority of the changes were due to suprascapular nerve compression .


Figure 20.3
EMG results. Red boxes indicate supraspinatus and infraspinatus muscle testing
Given the fact that she had previously undergone nonoperative management and was still experiencing pain and limited function, the patient elected to pursue revision surgery and arthroscopic suprascapular nerve decompression, distal clavicle excision, and intraoperative evaluation of the rotator cuff were recommended. It was felt that the majority of her symptoms were due to traction on the suprascapular nerve in the setting of repetitive overhead activity.
Management
A standard posterior portal was used for initial diagnostic arthroscopy with the patient in the beach-chair position. This revealed multiple loose bodies in the glenohumeral joint, synovitis, and a focal full-thickness re-tear of the supraspinatus tendon (Fig. 20.4). Attention was then turned to release of the suprascapular nerve at the suprascapular notch. While viewing from a posterolateral portal and working from an anterolateral portal, the posterior aspect of the coracoid was identified as was the insertion of the coracoclavicular ligaments. The transverse scapular ligament was carefully identified medial to the conoid ligament and a portal slightly medial to the standard Nevasier accessory superior portal was created to allow an appropriate trajectory for release. The suprascapular artery was identified (running over the ligament) and protected. While the artery is typically not used as a landmark, it can be helpful for orientation. Carefully blunt dissection can prevent injury to the artery and at times branches may need to be cauterized with a radiofrequency device to improve visualization. While protecting the suprascapular nerve (running underneath the ligament), the transverse scapular ligament was resected using a meniscal biter (Fig. 20.5). The nerve was then inspected, which revealed no further compression. The RC repair was then performed arthroscopically using a single-suture anchor and two sutures placed in a simple configuration (Fig. 20.6).




Figure 20.4
Arthroscopic posterior-portal view of full-thickness rotator cuff tear (arrowhead)

Figure 20.5
Arthroscopic view using meniscal biter to resect transverse scapular ligament (arrowheads)

Figure 20.6
Arthroscopic view showing repaired rotator cuff
Immediate postoperative rehabilitation included immobilization in a sling and early pendulums and passive range of motion. Active and active-assisted motions were permitted after 5 weeks with return to sport at 4 months.
Outcome
The 49-year-old patient with suprascapular neuropathy (SSN) recovered successfully. At 5 weeks postoperatively, her strength had recovered to 4+ out of 5 in all ranges. At 4 months she had minimal further pain with restoration of strength and was allowed to return to tennis. At 10 years postoperatively, her SF-12 PCS score was 48.9, ASES score was 73.3, and DASH score was 27.2 (normative scores for age and gender as mean ± standard deviation 49.7 ± 9.9, 92.2 ± 14.5, and 12 ± 16, respectively) [1–3].
Case 2
The patient is a 60-year-old right-hand-dominant retired male with a history of multiple injuries to his left shoulder including a remote humeral and scapular fractures treated nonoperatively. Prior to presentation he sustained two falls on his left shoulder while skiing and reported that pain and weakness in the left shoulder worsened with external rotation and abduction. Through clinical exam and MRI imaging (Fig. 20.7) he was diagnosed with complete tears of the supraspinatus and infraspinatus without atrophy or fatty infiltration. He underwent arthroscopic repair at an outside facility.
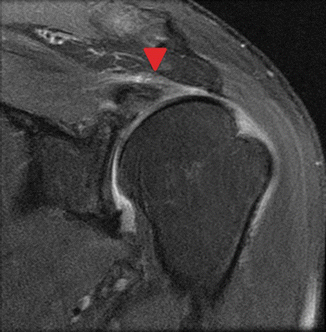

Figure 20.7
MRI of left shoulder demonstrating tear of the infraspinatus and supraspinatus (arrowhead) tendons with retraction
The patient’s rehabilitation went well until approximately 3 months postoperatively when he again fell and hurt his shoulder. At that point, he presented to clinic with increasing shoulder pain. Physical exam of the left shoulder demonstrated a preserved range of motion; strength examination revealed −5/5 strength on external rotation and forward flexion. Radiographs were unchanged from the previous images. A repeat MRI demonstrated a 25% partial bursal tear of the infraspinatus with an intact repair otherwise. There was mild atrophy of the supraspinatus and mild-to-moderate atrophy of the infraspinatus muscles noted on the new imaging (Fig. 20.8). Due to his increasing pain in the setting of a predominately intact RC and some early findings of atrophy, the patient underwent EMG/NCV which demonstrated SSN at the suprascapular notch (Fig. 20.9).










