Chapter 190 Migraine Headache
 Diagnostic Summary
Diagnostic Summary
• Recurrent paroxysmal attacks of headache.
• Headache is typically pounding and unilateral but may become generalized.
• Attacks often preceded by psychological or visual disturbances (auras); accompanied by anorexia, nausea, and gastrointestinal upset; and followed by drowsiness.
• Physical examination typically reveals no focal neurologic deficit.
 General Considerations
General Considerations
The lifetime prevalence of migraine headache is at least 18%.1 Women are more frequently affected than men, and more than half of affected patients have a family history of migraine. Prevalence is highest in North America and lowest in Africa and Asia.2 Although many migraines come on spontaneously, 10% to 20% of migraineurs may have warning symptoms (auras) before the onset of pain.3 Typical auras last a few minutes and may include the following:
Pathophysiology
The sequence of events producing migraine headache is unclear, but migraine headache is no longer believed to be a primary vascular event.1,4,5 Considerable evidence supports an association between migraine headache and vasomotor instability, but vasomotor changes are now believed to be epiphenomena, and a singular pathophysiologic mechanism has not been identified. Despite the awareness of multiple pathways involved in migraine, a clear understanding of its pathogenesis is at present not within reach. However, many of the key elements involved are worth discussing, because they relate to prevention and treatment.
Vasomotor Activity
It has been clinically observed that superficial temporal vessels are visibly dilated during migraine, and local compression of these vessels or the carotid artery temporarily relieves migraine pain.6 However, other types of extracranial vasodilation (e.g., heat- or exercise-induced) are not associated with migraine. Despite the extracranial vasodilation, the patient appears pale during the headache, suggesting constriction of the small vessels. This observation is supported by the presence of a lower skin temperature on the affected side. The clinical manifestations of focal or diffuse cerebral or brainstem dysfunction have been attributed to intracranial vasoconstriction. Some studies measuring cerebral blood flow have demonstrated a reduction in flow, sometimes to very low and critical levels, during the prodromal stage. The aura of migraine is apparently caused by cortical spreading depression (CSD),7–10 a process that produces transient depression of spontaneous and evoked neuronal activity. During this time, the brain fails to maintain normal ionic homeostasis and efflux of excitatory amino acids from neurons.7 CSD may represent a significant link to the decrease in cerebral blood flow observed during a migraine aura.11,12 This stage may be followed by a phase of increased blood flow, which can persist for more than 48 hours.
We are seeing increasing evidence that CSD may play a role in migraine pathophysiology and overall cerebral hyperexcitability. In addition, triggering CSD can require activation of the N-methyl-D-aspartate (NMDA) receptor, which augments depolarization.13 In one study, CSD was prevented in the presence of ifenprodil, a selective NMDA receptor antagonist.14 NMDA receptor antagonist therapy is suggested to be a potentially novel therapeutic approach.15 The anticonvulsant topiramate has become a first-line treatment for migraine; its efficacy as a GABA-agonist and glutamate antagonist supports the concept of excessive cerebral excitability as related to NMDA receptor activation.16 Calcitonin gene–related peptide (CGRP), among the most potent vasodilators known, is found to be elevated after migraine. CGRP antagonists have been demonstrated to be effective in relieving migraine pain without causing vasoconstriction and are being investigated for their therapeutic efficacy and safety.17
Evidence indicates that migraine patients have a functional abnormality of vasomotor control. Migraineurs suffer from syncope and orthostatic intolerance more often than patients who do not have migraine (who are without clear interictal signs of autonomic nervous system dysfunction)18; they also seem to be abnormally sensitive to the vasodilatory effects of physical and chemical agents.
Migraine also has complex relations with disorders of the cerebrovasculature, the cardiovascular system, and the heart. Right-to-left shunt, patent foramen ovale, and mitral valve prolapse are all associated with a higher prevalence of migraine headache. Migraine has also been shown to be associated with an increase in cardiovascular risk factors (ratio of total cholesterol to high-density-lipoprotein cholesterol >5), hypertension, and history of early-onset coronary heart disease or stroke). Although the risk for stroke is highest among young women who have migraine with aura, particularly if they smoke or use oral contraceptives, studies suggest that male and female migraineurs are at increased risk for ischemic stroke regardless of age.20 It is additionally worth noting that migraine and epilepsy are comorbid disorders that share common physiologic mechanisms and treatments.19
Platelets and Serotonin
Serotonin is normally stored in platelets and released by platelet aggregation and in response to various stimuli, such as catecholamines. There is no difference in total serotonin content between normal platelets and the platelets of migraine patients. However, the quantity of serotonin released by the platelets of the migraine patient in response to serotonin stimulation, although normal or even subnormal immediately after an attack, becomes progressively higher as the next attack approaches.21 The rise of plasma serotonin may not be causative in migraine but could represent a self-defense mechanism.7 Platelet activation has been observed in electron micrographs during migraine, which may be a result of the neurogenic inflammation.8 It is worth noting, on the other hand, that platelet deactivating agents—such as aspirin, feverfew, and essential fatty acids—appear to be effective in migraine prevention. Biochemical studies have shown that serotonin is a stress-response system that involves increased turnover during both acute and longer-term stress.22
The connection between serotonin and headaches began in the 1960s when researchers found that there was an increase in the serotonin metabolite 5-hydroxyindoleacetic acid (5-HIAA) in the urine during a migraine.23 Initially, serotonin excess was implicated; however, newer information indicates that the factor responsible for the increase in 5-HIAA is more likely the increased breakdown of serotonin as a result of increased activity of monoamine oxidase (MAO).24,25 Because migraineurs appear to have low levels of serotonin in their tissues, researchers began to refer to migraine as a “low-serotonin syndrome.”25 Low serotonin levels are thought to lead to a decrease in the pain threshold in patients with chronic headaches. This contention is strongly supported by over 35 years of research, including positive clinical results in double-blind studies with the serotonin precursor 5-hydroxytryptophan (5-HTP). Current understanding indicates that a low-serotonin state facilitates activation of the trigeminovascular nociceptive pathway, as induced by CSD.26 For more information on the clinical studies with 5-HTP in migraine headaches, see Chapter 98.
The triptan family of drugs are the 5HT1b and 5HT1d receptor agonists. These agents constrict blood vessels, block neurogenic inflammation and neural peptide release, and may also inhibit neuronal activity within the trigeminovascular system.27–29 The safety of these agents has been questioned, because the triptans activate serotonin receptors on cerebral vessels and, to a lesser extent, coronary arteries. The chest pain that is reported by 3% to 5% of patients taking oral triptans has generally not been associated with electrocardiographic changes and does not appear to be due to cardiac ischemia.30 However, triptans should be avoided in patients with ischemic heart disease, uncontrolled hypertension, or cerebrovascular disease.1 It is generally advisable to avoid the use of triptans, ergotamine-based drugs, and selective serotonin reuptake inhibitors (SSRIs) simultaneously, although the risk of serotonin syndrome appears to be low.30 Extreme caution is advised in considering the use of an SSRI along with 5-HTP. Although SSRIs are sometimes used for migraine prophylaxis, the scientific effect is unknown, the quality of evidence poor, and the impression of clinical impact low.22,31,32
Neuronal Disorder
It has been suggested that the trigeminovascular neurons, which innervate the pial arteries, release calcitonin gene–related peptide and the peptide substance P, either directly from various cellular signals or secondarily to CNS activation.33 Substance P is a key pain mediator and its release into the arteries is associated with vasodilation, mast cell degranulation, and increased vascular permeability. It is believed that the endothelial cells of the arteries respond to substance P and CGRP by releasing vasoactive substances such as arachidonic acid metabolites, purine compounds, or molecules containing carbonyl groups. This theory suggests that functional changes within the noradrenergic system constitute the threshold for migraine activation, and it is through modulation of sympathetic activity that potentiators exert their effects.33 Chronic stress is a chief potentiator in this model.
Unified Hypothesis
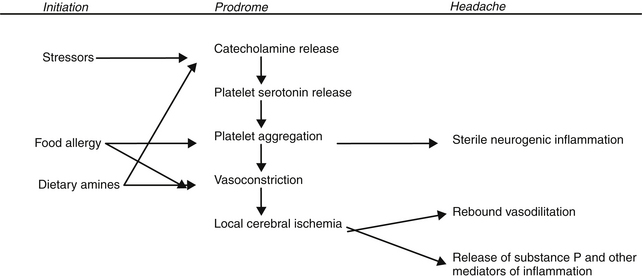
The mechanism of migraine can be described as a three-stage process: initiation, prodrome, and headache. Although a particular stressor may be associated with the onset of a specific attack, it appears that initiation is dependent on the accumulation over time of several stressors. These stressors ultimately affect serotonin metabolism (Box 190-1). Once a critical threshold of susceptibility is reached, a cascade of events is initiated. This susceptibility is probably based on a combination of decreased tissue serotonin levels, platelet modulation, alteration in the responsiveness of key cerebrovascular end organs, increased sensitivity of the intrinsic noradrenergic system of the brain, and the accumulation of histamine, arachidonic acid metabolites, or other mediators of inflammation. The platelet changes include increased adhesiveness, enhanced tendency to release serotonin, and increased levels of arachidonic acid in the membranes. Once platelets are stimulated to secrete serotonin, sequelae including platelet aggregation, vasospasm, and inflammatory processes lead to local cerebral ischemia. This is followed by rebound vasodilation and the release of peptide substance P and other mediators of pain. These events are summarized in Figure 190-1.
BOX 190-1 Factors that can Trigger Migraine Headaches
• Alcohol, especially red wine
• Withdrawal from caffeine or other drugs that constrict blood vessels
• Emotional changes, especially letdown after stress, and intense emotions such as anger
• Hormonal changes—e.g., menstruation, ovulation, birth control pills
• Too little or too much sleep
• Weather changes—e.g., changes in barometric pressure, exposure to sun
 Therapeutic Considerations
Therapeutic Considerations
Pharmacologic treatment of migraine headache tends to be inadequate because it fails to address the underlying cause. Modern first-line pharmaceuticals for prophylaxis in adults include propranolol, valproic acid, and topiramate, but a host of other drugs are helpful for migraine prevention. Despite their effectiveness, some preventive drugs can exacerbate other conditions. Flunarizine (unavailable in the United States), valproate, and amitriptyline, for example, should be used with caution or avoided in obese patients because they tend to cause weight gain. Amitriptyline and pizotifen can worsen glaucoma and urinary retention. Beta blockers can exacerbate asthma and diabetes a and topiramate can enhance the risk of renal calculi.34 Most guidelines from European countries include a nondrug treatment section, which also includes behavioral and psychological techniques.35 Medications are considered efficacious if they reduce migraine frequency by at least 50%.36 This is an important consideration where nonpharmacologic treatment options are concerned. The first step in treating migraine headache is to identify the precipitating factor or factors. Although food intolerance/allergy is important, many other factors must be considered as either primary causes or contributors to the migraine process. In particular, it is very important to assess the role that headache medications may be playing, particularly in chronic headaches.
Drug Reaction
Medication-overuse headache (MOH), also known as analgesic rebound headache, drug-induced headache, and medication-misuse headache, deserves mention because it frequently precludes the successful treatment of the underlying primary headache disorder, most often migraine or tension-type headache. In some cases, MOH may be associated with the development or maintenance of a chronic daily headache syndrome.37 After successful MOH treatment, preventive medications for the underlying primary headache disorder have a greater chance of success. Patients who were able to discontinue their daily use of symptom-modifying medications experienced improvement in their chronic headaches in addition to greater efficacy of their prophylactic medications.38 All drugs used for symptomatic relief on a regular basis can produce MOH, although the precise mechanism of action is unknown.39 Central sensitization, changes in trigeminal pain processing, receptor downregulation, and biobehavioral factors have all been proposed as possibly leading to MOH. Drugs that carry the highest potential for causing MOH include opioids, butalbital-containing analgesics, and aspirin/acetaminophen/caffeine combinations. Triptans carry intermediate to high potential for causing MOH when used frequently, and nonsteroidal antiinflammatory drugs (NSAIDs) carry the lowest risk.40 Ergotamine can cause MOH in addition to other symptoms when taken regularly. Regular use of ergotamine in migraine can result in a dependency cycle in which headaches escalate in severity on cessation of the medication. Ergotamine withdrawal predictably causes debilitating headaches, often accompanied by nausea and vomiting, generally resulting in an improved status by 72 hours. Ginger preparations can be helpful during ergotamine withdrawal.
Diet
Food Allergy/Intolerance
Food allergy/intolerance can play an important role in many cases of migraine headache. Double-blind placebo-controlled studies have demonstrated that the detection and removal of antigenic/intolerable foods will eliminate or greatly reduce migraine symptoms in the majority of patients. What is unclear is the percentage of migraine patients for whom food control is the most important factor. Table 190-1 summarizes the results of several clinical studies. Success ranges from 30% to 93%, with the majority of studies showing a remarkably high degree of success.41–48
TABLE 190-1 Food Allergy/Intolerance and Migraine Headache
| STUDY | PERCENTAGE RESPONDING | METHOD |
|---|---|---|
| Mansfield et al.41 | 30 | Elimination |
| Carter et al.42 | 93 | Oligoantigenic diet |
| Hughes et al.43 | 80 | Fasting, rotation, elimination |
| Egger et al.44 | 93 | Elimination |
| Monro et al.45 | 70 | RAST*, elimination, sodium |
| Grant46 | 85 | Elimination |
* Radioallergosorbent Test (blood test for IgE mediated allergy)
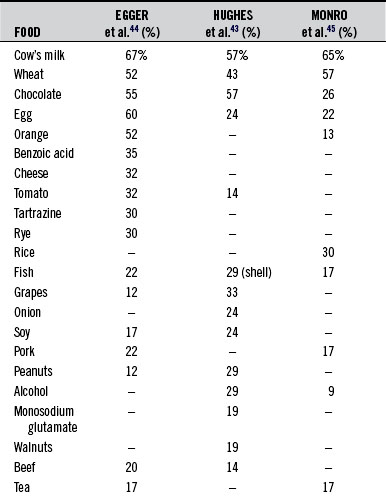
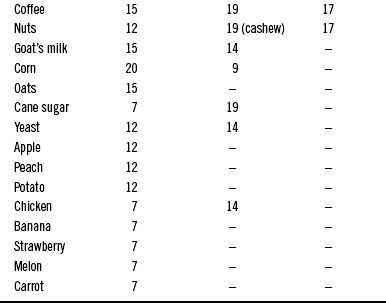
A plausible explanation for the large difference between the results of Mansfield et al41 and the others42–48 is that the Mansfield design was carefully selected for food allergy only, whereas the others included food intolerance. These studies found the incidence of food allergy to be similar among the major types of migraine. Few studies have been performed since the 1980s, when much of the groundwork regarding the relationship between food intolerance and migraine was laid. The foods most commonly found to induce migraine headaches are listed in Table 190-2.
• Idiopathic response to a pharmacologically active substance, such as tyramine
• Monoamine oxidase deficiency
• Platelet phenolsulfotransferase deficiency; immunologically mediated food allergy
Egger et al44 suggested that migraine headache may occur through chronic activation of the nonspecific responsiveness of cerebrovascular end organs as a result of long-term antigenic stimulation. This mechanism would be analogous to the bronchiolar response in asthma to exercise or cold after antigen contact. Allergic reactions to foods are known to cause platelet degranulation, with resultant serotonin release.47
In children, common migraine triggers include cheese, chocolate, citrus fruits, hot dogs, monosodium glutamate, aspartame, fatty foods, ice cream, caffeine withdrawal, and alcoholic drinks, especially red wine and beer. Tyramine, phenylethylamine, histamine, nitrites, and sulfites are involved in the mechanism of food intolerance headache, whereas immunoglobulin E–mediated food allergy is an infrequent cause.49
Several methods may be used to detect food allergies; most of these are described in Chapter 15. Laboratory testing can be convenient, but one major drawback of food intolerance testing with IgG antibodies can be a lack of reproducible findings with split blood samples among various laboratories. However, a study published in Mexico in 2007 found that when migraineurs removed foods to which they had mounted IgG responses, they experienced a robust improvement in their migraines, with 43 of 65 patients showing complete remission after 1 month of specific food elimination.50 Elimination diets/challenge testing are reliable and experiential methods for detecting food intolerance, but they also have limitations: some foods evoke a delayed response, so that it may require several days of repeated challenge to elicit recognizable symptoms. Food triggers can also be inconsistent. Ingestion of large amounts of several foods may be necessary to detect those that are marginally reactive. The recommended procedure for the diagnosis and management of food allergy/intolerance is described in the section on “Therapeutic Approach.”
Dietary Amines
Foods such as chocolate, aged cheese, pickled herring, sausages, sour cream, fermented foods, beer, and wine may precipitate migraine attacks because they contain histamine and/or other vasoactive compounds such as phenylethylamine that have a vasodilatory effect (Box 190-2).48,51,52 Tyramine is a component of many of these foods and has long been regarded as an important migraine trigger, but controlled studies have yielded conflicting findings.53 Red wine is more likely than white wine to trigger a headache because it contains 20 to 200 times the amount of histamine and also stimulates the release of vasoactive compounds by platelets.21,51,54
BOX 190-2 Factors Involved with Histamine-Induced Headaches
Red wine is additionally much higher in flavonoids, the antioxidant components shown to help prevent heart disease. These compounds can also inhibit the enzyme phenol sulfotransferase, which normally breaks down serotonin and other vasoactive amines in platelets. Many migraineurs have been found to have significantly lower levels of this enzyme,53 although the implications are confusing. Because red wine contains substances that are potent inhibitors of this enzyme, it often triggers migraines in these individuals, especially if consumed along with foods high in high vasoactive amine content, like cheese or chocolate. A standard treatment for histamine-induced headaches is to use a histamine-free diet along with vitamin B6 supplementation.54,55
The activity of the enzyme diamine oxidase, which breaks down histamine in the lining of the small intestine before it is absorbed into the circulation, appears to play a key role in determining reactivity to dietary histamine. Individuals sensitive to dietary histamine have lower levels (about 50%) of this enzyme in their tissues compared with control subjects.51 Diamine oxidase is a vitamin B6–dependent enzyme. Not surprisingly, compounds that antagonize vitamin B6 also inhibit diamine oxidase.51 These inhibitory factors include food coloring agents (specifically the hydrazine dyes, such as FD&C yellow #5), some drugs (isoniazid, hydralazine, dopamine, and penicillamine), oral contraceptives, alcohol, and excessive protein intake.
Vitamin B6 supplementation (usually 1 mg/kg) has been shown to improve histamine tolerance, presumably by increasing diamine oxidase activity.51,55 Women have lower levels of diamine oxidase, which may explain the higher incidence of histamine-induced headaches among them. Women are also much more frequently unable to tolerate red wine. Interestingly, the level of diamine oxidase in a woman increases by over 500 times during pregnancy.56,57 It is very common for women with histamine-induced headaches to experience complete remission of their headaches during pregnancy.
Miscellaneous Diet-Related Triggers
Hypoglycemia can be a trigger for migraine headache58,59 and is modifiable by dietary manipulation. Glycemic dysregulation is common in the setting of the standard American diet, given a tendency to consume unregulated quantities of high-glycemic-index carbohydrates. Hypoglycemia may be a result of inappropriate carbohydrate intake, especially when insulin levels become elevated. Excessive sodium intake may also represent a migraine trigger,60 perhaps as a consequence of increasing angiotensin levels in response to sodium ingestion. For individuals who are lactose-intolerant, avoidance of dairy products may afford improvement in the experience of migraine headache.61 Aspartame, a common sweetener, may be associated with an increased likelihood of migraine incidence62,63 and is easily avoided. Sucralose has become another commonly used artificial sweetener, and may be a migraine trigger.64 Monosodium glutamate is a well-recognized migraine trigger that can directly activate the NMDA receptor.
Helicobacter pylori
Gasbarrini et al65 demonstrated that migraine headaches improved dramatically in 100% of patients for whom H. pylori was identified and treated through standard measures. Further research has shown that the prevalence of H. pylori infection is significantly higher in migraineurs without aura compared with controls, indicating that H. pylori infection is a probable independent environmental risk factor for migraine without aura, especially in patients not genetically or hormonally susceptible.66 It appears that incidental H. pylori positivity is more relevant in migraineurs compared with controls, because a high percentage experienced relief from migraines when the infection was eradicated.67
Nutritional Supplements
5-Hydroxytryptophan (5-HTP)
5-HTP, the molecular intermediate between tryptophan and serotonin, is readily absorbed when taken orally and easily crosses the blood-brain barrier. In addition to augmenting serotonin levels, it may also increase endorphin levels. The use of 5-HTP in the prevention of migraine headache offers considerable advantages over drug therapy. Although a number of drugs have been shown to be useful in the prevention of migraine headache, all of the currently used drugs carry with them a risk of significant adverse effects. 5-HTP is at least as effective as other pharmacologic agents used in the prevention of migraine headaches and is safer and better tolerated. Although some studies have employed a dosage of 600 mg/day or more,68 5-HTP can be effective at a dosage as low as 200 mg/day.69 The clinical studies with 5-HTP in migraine headaches are discussed in Chapter 98.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree