CHAPTER 25 Midcarpal Instability
The concept of midcarpal instability (MCI) has unfolded over many years. It represents several distinct clinical entities that differ in their cause and direction of subluxation but share the common characteristic of abnormal force transmission at the midcarpal joint. Lichtman and Wroten consolidated the various forms into intrinsic and extrinsic types. The intrinsic types consist of palmar MCI (PMCI), dorsal MCI (DMCI), and combined forms.1 There are no arthroscopic findings that are characteristic of MCI, but wrist arthroscopy allows one to examine the chondral surfaces for abnormal wear and has a role in treatment for milder forms of MCI. Extrinsic MCI, as described by Taleisnik and Watson, is caused by a dorsally malunited distal radius fracture.2 This lesion is typically treated by a distal radius osteotomy to restore the normal palmar tilt and falls outside the scope of this discussion.
ANATOMY
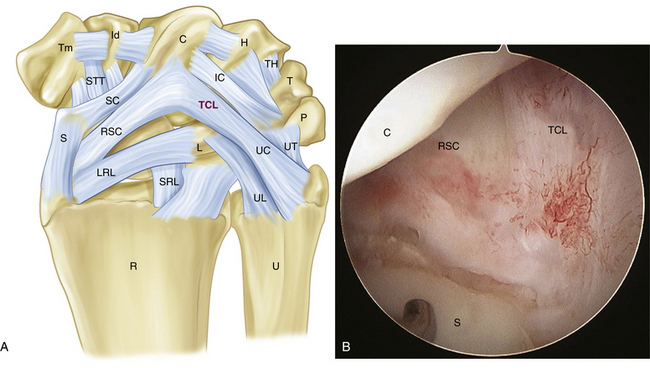
The palmar arcuate ligament complex comprises a radial arm, which is confluent with and distal to the radioscaphocapitate ligament, and an ulnar arm, the triquetrohamate-capitate ligament (TCL) (Fig. 25-1). In the normal situation, the proximal carpal row moves smoothly, from a flexed position when the wrist is in radial deviation to extension when the wrist is in ulnar deviation. This is possible because of the progressive tightening effect of the arcuate ligament as it stretches out to length, incrementally pulling the midcarpal row into extension, and the carpal bone geometry, which causes the triquetrum to translate dorsally along the helicoidal facet of the hamate. If the arcuate ligament is attenuated, this synchronous motion is lost.3
Studies by Trumble and colleagues4 and Viegas and coworkers5 showed that sectioning of the TCL or the dorsal radiocarpal ligament (DRCL), also known as the dorsal radiotriquetral ligament, could produce a volar intercalated segmental instability (VISI) deformity and simulate PMCI. Lichtman and colleagues showed in vivo that tightening the DRCL alone can stabilize the proximal carpal row and eliminate the clunk of PMCI, emphasizing the potential importance of dorsal ligament laxity in the pathogenesis of this disorder.6 Lichtman believed that PMCI is caused by laxity of the TCL and DRCL, which allows an excessive palmar sag of the heads of the capitate and hamate at the midcarpal joint. This produces a VISI pattern of the proximal row in the nonstressed wrist. This sag results in a loss of joint contact across the midcarpal joint, which manifests clinically as a loss of the smooth transition of the proximal row from flexion to extension as the wrist deviates ulnarward. The proximal carpal row stays in a flexed position until the terminal extent of ulnar deviation, when the helicoidal shape of the hamate facet suddenly forces the triquetrum to move dorsally. This snaps the lunate, and subsequently the scaphoid, into extension, causing a sudden reversal of the VISI. This sudden proximal row extension is responsible for the painful and rapid catch-up clunk that occurs. As the wrist moves back to neutral position, the triquetrum translates down the hamate facet, allowing the proximal row to drop back into VISI while the distal row again settles palmarly into its slightly subluxated starting point (Fig. 25-2).
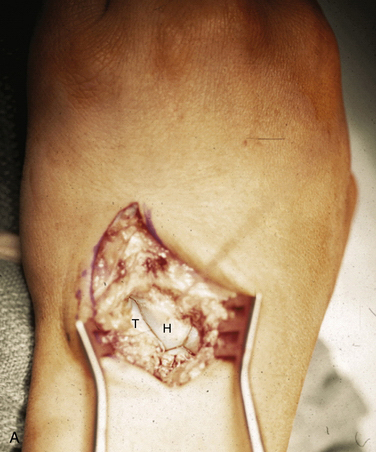
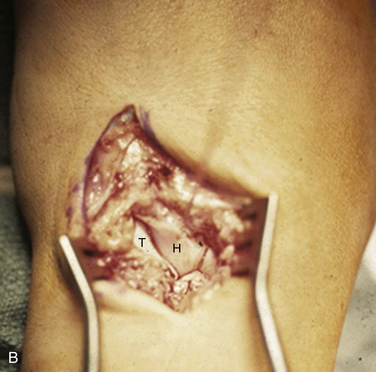
FIGURE 25-2 Dorsal exposure of the midcarpal joint in a left wrist. H, hamate, T, triquetrum. A, Triquetrohamate joint with the proximal row reduced. B, Subluxed triquetrohamate joint with volar sag of the proximal row. H, hamate, T, triquetrum.
(Courtesy of David J. Slutsky, MD, Torrance, California.)
The dorsal pattern of MCI has not been studied as extensively. It appears that laxity of the radial arm of the palmar arcuate ligament permits the capitate and hamate to translate dorsally to an excessive degree, especially with ulnar deviation of the wrist.7,8 In the palmar and dorsal patterns, the proximal row always moves into extension, and the distal row translates dorsally with ulnar deviation. It is the timing and force of this movement that differentiates the two patterns. In PMCI, the distal carpal row starts out in palmar subluxation with the wrist in neutral position. As the wrist moves into ulnar deviation, the subluxation suddenly corrects. In DMCI, the wrist starts out in a reduced position in neutral. Dorsal subluxation of the distal row then occurs with ulnar deviation. In either case, the instability is caused primarily by laxity of the selected extrinsic carpal ligaments that support the proximal row, which prevents them from controlling the complex kinematic relationships among the articular surfaces across the midcarpal joint.
PATIENT EVALUATION
History and Physical Examination
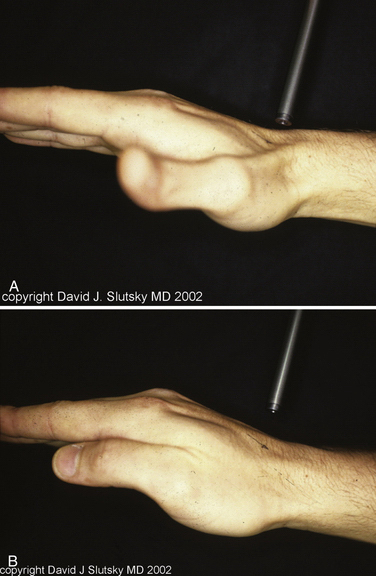
In PMCI, the patient presents with a history of clunking of the wrist. Patients can often reproduce the clunk on both sides, because generalized ligamentous laxity frequently coexists. The patient may have a trivial injury that accentuates this normal laxity, resulting in a painful clunk. On physical examination, close inspection reveals a sag of the midcarpal joint with the wrist in radial deviation, which is reduced with active or passive ulnar deviation (Fig. 25-3). The clunk may be reproduced by performing the midcarpal shift test.3 This test is performed by placing the patient’s wrist in neutral position with the forearm in pronation. A palmar force is then applied to the hand at the level of the distal capitate. The wrist is simultaneously loaded and deviated ulnarly. The test result is positive if a painful clunk occurs that reproduces the patient’s symptoms.