Metacarpophalangeal Joint Synovectomy and Extensor Tendon Centralization in the Inflammatory Arthritis Patient
Andrew L. Terrono
Paul Feldon
Hervey L. Kimbal III
DEFINITION
The finger metacarpophalangeal (MCP) joint is commonly and characteristically involved in inflammatory arthritis.
The MCP joint is often involved early in inflammatory arthritis and usually presents with ulnar extensor tendon subluxation resulting in ulnar deviation of the fingers.
Occasionally in systemic lupus erythematosus (SLE), radial subluxation of the extensor tendon is seen.
ANATOMY
The normal MCP joint is a condylar joint that allows flexion and extension as well as radial and ulnar deviation and a combination of these movements. Normally, there is 90 degrees of flexion, although hyperextension can vary.1,2
The stability of the MCP joint is provided by the radial and ulnar collateral ligaments, the accessory collateral ligaments, the volar plate, the dorsal capsule, and the extensor tendon (FIG 1).
The metacarpal head diameter increases in both the transverse and sagittal planes and therefore has a cam effect, making the collateral ligaments tight in flexion and lax in extension. This allows more radial and ulnar deviation of the MCP joint in extension.
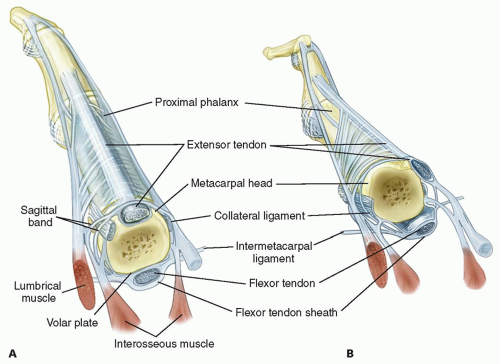
FIG 1 • A. Normal anatomy of the MCP joint. B. Abnormal anatomy seen in inflammatory arthritis. The extensor tendon is subluxated ulnarly.
The MCP joint collateral ligaments are asymmetric.
The ulnar collateral ligament is more parallel to the long axis of the fingers.
The radial collateral ligament is more oblique.
This causes supination of the MCP joint with MCP joint flexion.
The collateral ligament also resists volar-directed forces.
The volar plate is fibrocartilaginous distally and has a membranous portion proximally. It limits MCP joint extension.
The transverse intermetacarpal ligament connects the volar plates to each other.
The accessory collateral ligament connects the collateral ligament and volar plate and keeps the volar plate close to the volar aspect of the MCP joint throughout motion.
The A1 pulley of the flexor tendon sheath is attached to the volar plate.
The extensor digitorum tendon is maintained centrally over the MCP joint by the transverse fibers of the sagittal band that attach volarly to the volar plate and the intermetacarpal ligament. This forms a sling mechanism. The ulnar sagittal band is felt to be stronger and denser than the radial sagittal band.
There is usually no direct extensor tendon insertion into the proximal phalanx. The proximal phalanx is extended through the sling mechanism.
The lumbrical muscle originates from the tendon of the flexor digitorum profundus and is volar to the intermetacarpal ligament. It inserts into the lateral band.
There are three volar (which adduct) and four dorsal (which abduct) interossei that have tendons that all pass dorsal to the transverse intermetacarpal ligament. They have variable insertions into the proximal phalanx and extensor mechanism.
The first dorsal interosseous almost always inserts completely into the radial side of the proximal phalanx of the index finger.
PATHOGENESIS
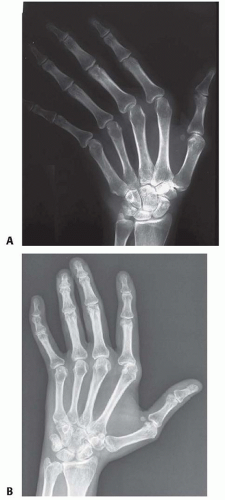
Selective changes in static and dynamic stabilizers of the MCP joint occur, resulting in alteration in the equilibrium of the joint. The most common deformity produced is ulnar deviation of the fingers (FIG 2A).
Which comes first, the changes to the dynamic or static stabilizers, is unclear and may vary.
The capsule, radial collateral ligament, and radial sagittal band are stretched by the synovitis and allow the equilibrium to move toward ulnar deviation.
The accessory collateral ligament and the membranous portion of the volar plate become lax.
The joint capsule becomes thinned and a defect in the dorsal capsule may occur.
With increasing ulnar deviation, the ulnar intrinsic muscle tendon unit shortens.
The intrinsic muscle contribution to the deformity is unclear. It may be a primary or secondary change. There is a cycle that is set up as the MCP joint ulnarly deviates and the extensor tendon acts as an ulnar deviator and may even act as a flexor of the MCP joint.
The laxity of the volar plate and accessory collateral ligament causes the flexor tendons to be further away from the center of rotation of the MCP joint. Therefore, the flexor tendon develops a mechanical advantage and increased flexion force. This results in an increase in the deformity.
The combination of changes to the capsule, radial collateral ligament, radial sagittal band, accessory collateral ligament, and the membranous portion of the volar plate and the increased mechanical advantage of the flexor tendon is magnified by the normal ulnar and volar slope of the metacarpal condyles and allows ulnar deviation and volar displacement of the proximal phalanx (FIG 2B).
The wrist may be a contributing factor to the development of the MCP joint deformity, and this must be considered in each case before correcting the MCP joint.
Radial deviation of the wrist can be a compensatory position to the ulnar deviation of the MCP joints to allow the fingers to line up with the forearm.
Ulnar deviation of the digit is more common in patients with radial deviation of the wrist.
At first, the deformity is correctable passively, but gradually, this mobility is lost and the deformity becomes fixed.
Articular cartilage changes progress from softening of the cartilage to erosion with significant loss of cartilage and bone. This contributes to the deformity.
Once there are significant cartilage and bone changes, extensor tendon realignment alone, without joint resurfacing, is not indicated.
The changes seen in SLE are secondary not to synovitis but rather to alteration in the collagen that results in a change in the equilibrium of the MCP joint and subsequent deformity.
The finger deformity in SLE is often ulnar deviation, but radial deviation is not uncommon.
In SLE, it is easy to change one deformity to another (ie, ulnar drift into a radial deviation deformity after surgery) because of the global changes to the supporting structures.
Despite the MCP deformity becoming fixed, the articular cartilage is usually preserved.
NATURAL HISTORY
The natural history of the MCP joint changes in inflammatory arthritis is not known and is probably highly variable and influenced by the new disease-modifying medications.
Mild ulnar deviation of the fingers is normal and increases with MCP joint flexion.
In inflammatory arthritis, such as rheumatoid arthritis, deformity is initially passively correctable.
Mild ulnar deviation of the fingers is seen in less than 10% of the patients in the first 5 years of having rheumatoid arthritis.3
Ulnar deviation has been reported in 30% of patients with rheumatoid arthritis, with palmar subluxation in 20%.3
Palmar subluxation almost always occurs with ulnar deviation.3
PATIENT HISTORY AND PHYSICAL FINDINGS
In a patient with inflammatory arthritis who is being considered for MCP joint surgery, the entire upper extremity is evaluated. Involvement of the lower extremities must also be considered, given that the upper extremities may need to assist in ambulation.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree