Chapter 95 Glutamine
 Introduction
Introduction
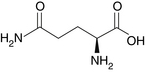
Glutamine (Figure 95-1) is the most abundant amino acid in blood and muscle tissue. It comprises approximately 6% of mixed whole body protein and is unique among amino acids in that it is a preferred fuel of rapidly dividing cells, such as intestinal and immune cells, and is important in maintaining pancreatic function.1–3 Glutamine is involved in the transport of circulating amino nitrogen and is an important intermediary that allows for accelerated gluconeogenesis from amino acids that are released by the skeletal muscle during stress states.4 In addition, glutamine is used as a precursor for DNA and glutathione synthesis.5 As one of the principal fuels used by the cells of the intestinal lining, it accounts for 35% of enterocyte energy production.
Although readily available in the diet and synthesized in the body from glutamate and ammonia, supplementation is known to enhance the energy metabolism of the gastrointestinal mucosa, thus stimulating regeneration.6 Although glutamine is not considered essential in healthy people, there is evidence that the increased need for glutamine in stressed states such as burns, septicemia, endotoxemia, intestinal failure, and critical illness may result in it being “conditionally essential.”3,7,8
Forms
The nomenclature of L-glutamine and glutamine are used interchangeably. D-glutamine is the stereoisomer of L-glutamine and does not have any known biological activity. L-glutamine is not soluble in water, and aqueous solutions are unstable at temperatures of 22° C to 24° C. As a result, the more soluble and more stable dipeptides such as alanyl-glutamine are used as delivery forms of L-glutamine in total parenteral nutrition solutions.9,10
Physiologic Effects
Intestinal Repair and Protection
Animal and human studies suggest that glutamine stimulates intestinal mucosal growth11 and protects from mucosal atrophy. Glutamine prevents intestinal mucosal damage and was shown to decrease bacterial leakage across the intestines after they are damaged, presumably by stimulating repair.12 Glutamine is thought to accomplish this by strengthening epithelial tight junctions and also by preventing paracellular permeabilities through an epidermal growth factor receptor–dependent mechanism.
In one tissue culture experiment, intestinal epithelium cells were treated with acetaldehyde to compromise barrier function. These cells were treated with L-glutamine, D-glutamine, L-asparagine, L-arginine, L-lysine, or L-alanine. Only the L-glutamine demonstrated a benefit by decreasing aldehyde effects on transepithelial resistance. Furthermore, L-glutamine–treated cells decreased permeability that was dose dependent. L-glutamine reduced the acetaldehyde-induced disturbance of transmembrane structures, such as occludin, zonula occludens-1, E-cadherin, and β-catenin from the intercellular junctions. Lastly, L-glutamine induced a rapid increase in the tyrosine phosphorylation of the epidermal growth factor receptor. No other amino acids demonstrated this effect.13
Acid Base Balance
Glutamine plays an important role in acid-base homeostasis.14 Glutamine is synthesized from glutamate and the toxic alkaline waste product ammonia by the enzyme glutamine synthetase, which requires magnesium and adenosine triphosphate. When ammonia levels are elevated, the body effectively removes ammonia from the blood by synthesizing glutamine. Conversely, if the blood is too acidic, the glutamine can be broken down into glutamate and ammonia, which increases blood pH. Ammonia can bind hydrogen ions to produce ammonium cations, which are excreted in the urine along with chloride anions. Bicarbonate ions are simultaneously released into the bloodstream. Clinical studies showed that relatively small oral doses of glutamine can elevate plasma bicarbonate concentrations in healthy adults.
In one study, 2 g of glutamine were dissolved in a cola drink and ingested over a 20-minute period 45 minutes after a light breakfast. Control subjects were given soda only. Blood samples were taken 1 week before, at baseline, and subsequently at three separate 30-minute intervals after ingestion of the glutamine drink or placebo. Eight of nine subjects responded to the oral glutamine load with a significant increase in plasma glutamine at 30 and 60 minutes before returning to the baseline value at 90 minutes. Ninety minutes after the glutamine was administered, plasma bicarbonate concentration was found to be increased. Circulating plasma growth hormone concentration was elevated as well. Concomitant with enhanced renal acid secretion, glutamine ingestion also caused an increase in the glomerular filtration rate.15
The authors of this study explained that their results showed that it was unlikely L-glutamine was a direct precursor of bicarbonate. Instead, L-glutamine appeared to play an indirect role in accelerating acid secretion through mechanistic changes in the kidneys. Human studies showed that urinary ammonium excretion is altered by changes in glutamine intake.16
Chronic metabolic acidosis is a common clinical problem encountered in catabolic states such as sepsis, shock, and diabetes, and is a major factor in many biological derangements.17 Because glutamine becomes an essential amino acid in catabolic states when the increased demand exceeds the body’s capability to synthesize it,18 glutamine supplementation may be quite useful to maintain pH homeostasis in patients with acidotic conditions.
Glutathione Repletion
Glutathione is a tripeptide consisting of glutamate, cysteine, and glycine. As a reservoir source for glutamate in the body, the availability of glutamine appears crucial for the regeneration of glutathione stores in the liver during hepatic injury; in skeletal muscle after major trauma, sepsis, or surgery; and in chemotherapy-injured heart muscle.19–21 Glutamine can enhance intracellular repletion of glutathione, an important scavenger of reactive oxygen species.22 Rat studies demonstrated that during 5-fluorouracil–induced free radical–mediated hepatic injury, glutamine increased glutathione biosynthesis and preserved the glutathione stores in hepatic tissue.19 Seventeen patients who underwent a standardized surgical procedure were prospectively given 0.56 g/kg body weight/day of glutamine or a placebo. Using percutaneous muscle biopsies and blood samples, there were no significant decreases in total or reduced glutathione in the glutamine-supplemented group 24 and 72 hours after the operation. In contrast, the placebo group experienced total muscle glutathione losses of 47 ± 8% and 37 ± 11%, as well as reduced glutathione decreases of 53 ± 10% and 45 ± 16% at 24 and 72 hours, respectively.
Protein Sparing
Glutamine is a regulator of muscle proteolysis,23 and supplementation can attenuate loss of protein in the muscle. Experiments using animal cancer models demonstrated decreased protein loss and simultaneous protection of immune and gut-barrier function during radiation therapy in patients with advanced cancer.5 In children with severe muscle wasting, 5 hours of oral glutamine was shown to have protein-sparing effect (see later discussion on “Cachexia”).24
Immune Support
Although poorly understood, it appears that glutamine has an immune-modulating effect by enhancing interleukin (IL)-6 levels25 and lymphocyte function.26 IL-6 plays an essential role in the final differentiation of β-cells into immunoglobulin-secreting cells, nerve cell differentiation, and acute phase reactants in hepatocytes. Exercise by itself is known to induce an eleven-fold increase in plasma IL-6. Glutamine supplementation further enhances IL-6 levels.25 The ability of lymphocytes to proliferate and generate lymphokine-activated killer cell activity in vitro was found to be glutamine dependent.27 Additionally, glutamine-enriched parental nutrition demonstrated enhanced lymphocyte activity in patients who received high doses of chemotherapy after stem cell transplantation for hematologous malignancy.
 Clinical Applications
Clinical Applications
Intestinal Permeability–Related Conditions
A number of conditions are linked to intestinal permeabilities, including chronic urticaria,28 inflammatory bowel disease (Crohn’s disease),29–31 celiac disease,32 liver and biliary cirrhosis and cases of portal hypertension,33,34 systemic sclerosis,35 diabetes,36 rheumatologic disorders,37,38 cystic fibrosis,39 alcohol overuse,40 adult and child asthma,41 human immunodeficiency virus (HIV)/acquired immune deficiency syndrome,42 nonsteroidal antiinflammatory drug–treated arthritis patients,43 moderate to major burn injuries,44 corticosteroid use,45 cardiopulmonary bypass patients,46,47 and acute metal toxicities.48 To evaluate these permeabilities, sucrose serves as a marker for gastroduodenal permeability and the urinary lactulose/mannitol ratio for intestinal permeability, after administration of these sugars.28 From a naturopathic perspective, the underlying cause of many of these conditions may stem from food allergies that contribute first to chronic inflammation in the intestinal tract28 and then to systemic endotoxemia. Certain conditions such as cardiopulmonary bypass can cause intestinal ischemia,49 which is then the primary insult that causes permeabilities in these patients. The use of glutamine can help heal these permeabilities, thus removing a mode of pathogenesis in these variegated conditions.
Infectious Diarrhea
Animal models showed the usefulness of glutamine in diarrhea to augment sodium and water absorption and to enhance blood glucose and body weight.50 A rat model of cholera toxin–induced diarrhea showed that glutamine was able to improve water and electrolyte intestinal absorption even better than traditional glucose solutions.10 One placebo-controlled, double-blind, randomized trial human study evaluated glutamine to treat acute diarrhea in 128 otherwise healthy children. Of these 6- to 24-month-olds, 63 received 0.3 g/kg per day of glutamine and 65 controls received a placebo for 7 days. The average duration of diarrhea in the glutamine-treated group was significantly shorter than that of the placebo group (3.40 ± 1.96 vs 4.57 ± 2.48 days, respectively). However, no differences in serum IL-8 and secretory immunoglobulin-A were found between groups at the beginning of treatment or 1 week later.51
Clearly, glutamine holds promise for enhancing repair of mucosal injury caused by a wide range of infections or toxic agents and thus has great potential as a nutritional therapeutic for patients with enteric infection.52
Postsurgical Complications of the Gastrointestinal Tract
Patients undergoing abdominal surgeries such as gastrectomies, sigmoidectomies, cholecystectomies, colectomies, and rectal resections are at risk for the development of intestinal failure or short bowel syndrome (SBS). In SBS, a serious malabsorption of fluid, electrolytes, and other nutrients can occur, placing the patient at higher morbidity and mortality risk.53 Trauma from abdominal surgery may also compromise the intestinal mucosa to the point where bacteria and endotoxins can easily transfer through the intestinal wall and invade tissue and blood in an event called bacterial translocation. Through inflammatory mechanisms, bacteria, and endotoxic septic conditions, the intestinal mucosal barrier can be adversely affected and cause further damage, thus forming a vicious circle. Severe cases result in systemic inflammatory response syndrome and multiple organ dysfunction syndrome.54
In a regimen that includes growth hormone and diet changes, glutamine can help difficult cases to enhance bowel adaptation. In one study of 10 patients with SBS who previously failed to adapt to enteral nutrients, 8 subjects received exogenous growth hormone, supplemental glutamine, and a modified high-carbohydrate, high-fiber diet. Two patients were treated with the modified diet alone. Three weeks of treatment with growth hormone, glutamine, and a modified diet significantly increased total caloric absorption from approximately 60% to 75%, protein absorption from 49% to 63%, and carbohydrate absorption from 60% to 82%. Water absorption increased from 46% to 65%, and sodium from 49% to 69%. Fat absorption did not change. Diet alone did not influence nutrient absorption or stool output. After 28 days of therapy, the patients were discharged and instructed to continue the diet and glutamine treatment.55 It is unknown whether glutamine and diet changes alone, without concomitant growth hormone administration, would have the same positive effect.
In a second study, 20 patients who underwent abdominal surgery were randomized into two groups receiving oral administration of 30 g of glutamine or a placebo in divided doses for 7 days. Serum glutamine concentration was significantly decreased in the placebo group and increased in the glutamine group after 7 days. Markers of intestinal permeability were significantly increased in the placebo group and decreased in the glutamine group. Additionally, the serum markers of endotoxin, diamine oxidase, and malondialdehyde concentrations were significantly decreased in the glutamine group compared with those in the placebo group. Temperatures, heart rates, and white blood cell counts were also significantly lower in the glutamine group.54
Ischemia reperfusion of the gut is also a common event in various clinical conditions, such as trauma, burn, septic shock, cardiac or aortic surgery, and liver or small bowel transplantation, and is associated with a high death rate. Intestinal ischemia reperfusion can cause edema and disruption of the structural integrity and function of the intestinal mucosa and associated vascular tissue. It may set the stage for endotoxemic translocation of a number of bacterium, including Escherichia coli, Enterococcus, Pseudomonas, Proteus, and Staphylococcus. Studies of animal models demonstrated that glutamine, when supplemented as total parenteral nutrition, protected the intestines from morphologic and functional mucosal injury after intestinal ischemia reperfusion. Furthermore, intestinal permeabilities and the incidence of bacterial translocation in intestinal ischemia reperfusion animals were also prevented in a dose-dependent manner by glutamine supplementation.56,57
Chemotherapy and Radiation Side Effects
Standard cancer therapies often include the use of chemotherapy and radiation, which can injure rapidly dividing intestinal cells. It was shown that during chemotherapeutic and radiotherapy insult, glutamine reduced degeneration of intestinal mucosa in rats, prevented intestinal mucosal injury,56 protected liver function through enhanced glutathione biosynthesis and storage in hepatic tissue, increased immune function, and reduced permeability of the gut.19,26
In one investigation, 70 patients with colorectal cancer were randomly assigned to oral glutamine at 18 g/day or placebo before the first regimen of 5-fluorouracil and folinic acid administered intravenously for 5 days. Glutamine was given 5 days before, during, and after chemotherapy. Using D-xylose urinary excretion and cellobiose/mannitol evaluation, damage to the intestines was assessed at baseline, as well as 4 and 5 days after the end of the first cycle of chemotherapy. After one cycle of chemotherapy, the reduction in D-xylose absorption and reduction of mannitol was significantly greater in the placebo group (7.1% vs 3.8% and 9.2% vs 4.5%, respectively). Urinary recovery of cellobiose was not different between the study arms. Accordingly, the cellobiose/mannitol ratio increased more in the placebo treatment group. Furthermore, diarrhea parameters, as well as the average number of antidiarrheal opiate loperamide tablets needed, were reduced in the glutamine arm, thus supporting the positive clinical effect of this low-cost supplement.11
Oropharyngeal mucositis, or mouth sores, and accompanying swallowing difficulty are other untoward results of radiotherapy and can be a major source of suffering in patients with head and neck cancer. Glutamine during and after chemotherapy appears to be an excellent way to safely decrease the incidence of mouth sores. One investigation of 17 patients with head and neck cancer who received primary or adjuvant mouth irradiation for 5 days a week were randomized to either adjunctive glutamine suspension of 16 g in 240 mL normal saline or a saline placebo. Patients were instructed to swish the test solutions (30 mL) four times daily. The duration of objective oral mucositis was significantly shorter in the glutamine arm.58 A second randomized, double-blind crossover trial observed 24 patients who were given a glutamine or placebo suspension to swish and swallow on days of chemotherapy administration and for at least 14 days after therapy. Significant improvement was observed in the glutamine group. Additionally, the duration of mouth pain was 4.5 days less in chemotherapy courses with concomitant glutamine supplementation. The severity of oral pain was reduced so significantly when glutamine was used that a patient could venture past soft foods 4 days sooner compared with placebo.59
Glutamine studies validating its use are also beginning to emerge in other areas of oncology. In a study of esophageal cancer patients, 13 patients were randomized into two groups, controls and a group that received oral glutamine supplemented at a dosage of 30 g/day for 4 weeks. It was observed that supplementation of glutamine enhanced lymphocyte mitogenic function and reduced permeability of the gut during radiochemotherapy.5 Patients who underwent bone marrow transplant and myelosuppressive chemotherapy for acute myeloid leukemia also found that parenteral glutamine therapy could improve neutrophil recovery, although no change in neutropenic fever was shown.60 Given that glutamine improves the structure and function of the gut, it is understandable that multiple parameters and markers of healthy physiologic function will improve with its use.
It should be noted that glutamine’s efficacy may depend on a number of other factors, including the specific chemotherapeutic prescribed and dosage. A study of 65 patients with advanced breast cancer receiving doxifluridine were prescribed 30 g/day of glutamine in three divided doses of 10 g each or a placebo for 8 consecutive days during each interval between chemotherapy, which was administered from days 1 to 4. In this case, there was no statistical difference with regard to diarrhea morbidity, nor did glutamine affect the severity and duration of tumor growth.61 Interestingly, a study of bone marrow transplantation patients found that allogeneic transplantation patients (those receiving bone marrow from another individual) did not have the same beneficial mouth pain reduction that autologous transplantation patients (those who donated their own marrow) experienced when receiving glutamine support. However, in the work mentioned previously, the amounts of glutamine were less than those used in other studies.
It was also theorized that methotrexate use in the allogeneic patients might have been responsible for the decreased protection. Nevertheless, in the allogeneic patients, the 28-day survival was still increased.62 A third multicenter study of 129 patients found no protection against diarrhea when used adjunctively with pelvic radiation therapy. These patients received 4 g of glutamine or a placebo by mouth, which was also a significantly lower dose than the more successful studies employed.63
Although intestinal function is greatly compromised with chemotherapy and radiation treatment, cardiac function is commonly affected as well. The use of doxorubicin therapy for breast cancer is often limited by cardiomyopathic heart changes that often result in congestive heart failure. One rat study simulated doxorubicin treatment with and without glutamine support and found that oxidative damage to the heart was diminished in the glutamine-treated group, probably as a result of glutamine’s ability to maintain cardiac tissue glutathione levels (see later discussion on “Cardiac Disease”).21
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree