CHAPTER 8 General and Regional Anesthesia and Postoperative Pain Control
INTRODUCTION
Orthopaedic procedures for the elbow are well suited to regional anesthetic techniques. Continuous catheter techniques provide postoperative analgesia and allow early limb mobilization. In addition to intraoperative anesthesia, brachial plexus and peripheral nerve blocks may also be used in the treatment and prevention of reflex sympathetic dystrophy. Conversely, although the benefits of regional anesthesia in this patient population are well established, the operative site may be adjacent to neural structures, as with total elbow arthroplasty or supracondylar fractures. For example, ulnar nerve dysfunction may occur in up to 10% of patients undergoing elbow arthroplasty.17 Early diagnosis and intervention are paramount in reducing the severity of nerve injury; assessment of neurologic function would not be possible in the presence of a regional block. Thus, the anesthetic and analgesic management are based on the patient’s evolving neurologic status (including the need for serial neurologic examinations, the anticipated rehabilitative goals, and history of side effects or interactions to systemic analgesics). Meticulous regional anesthetic technique, careful patient positioning, and serial postoperative neurologic examinations are required to reduce the incidence of neurologic dysfunction while optimizing surgical outcome.
INTRAOPERATIVE ANESTHETIC MANAGEMENT
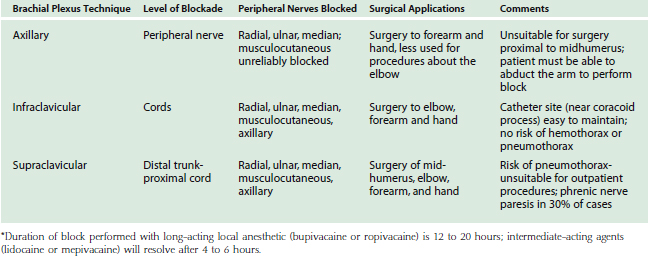
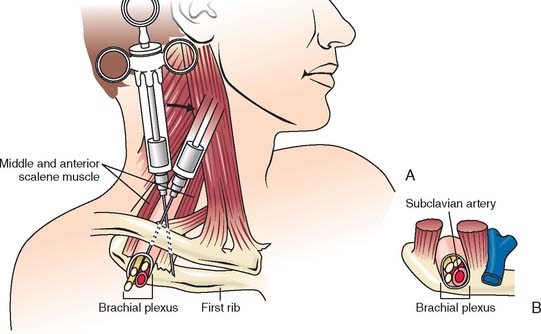
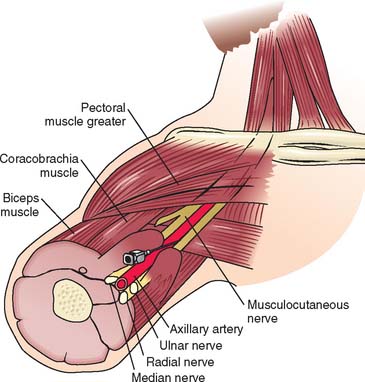
Surgical procedures for the distal humerus, elbow, and proximal radius, and ulna are commonly performed with regional anesthetic techniques.4 The brachial plexus may be blocked using four distinct approaches. Advances in needles, catheters, and nerve stimulator technology have facilitated the localization of neural structures and improved success rates. Selection of regional technique is dependent on the surgical site (Table 8-1). For surgery on the elbow, the supraclavicular (Fig. 8-1), infraclavicular, or axillary (Fig. 8-2) approaches are ideal because these approaches provide adequate blockade of the lower trunk, which remains unblocked with the more proximal interscalene technique. Supraclavicular, infraclavicular, and axillary approaches to the brachial plexus are reliable and provide consistent anesthesia to the four major nerves of the brachial plexus: median, ulnar, radial, and musculocutaneous.19 However, the small but definite risk of pneumothorax associated with supraclavicular blocks makes this approach unsuitable for outpatient procedures. Typically, pneumothorax occurs 6 to 12 hours after hospital discharge; therefore, a postoperative chest radiograph is not helpful. Although chest tube placement is advised for pneumothorax greater than 20% of lung volume, the lung may also be re-expanded with a small Teflon catheter under fluoroscopic guidance, eliminating the need for hospital admission. The infraclavicular and axillary approaches to the brachial plexus eliminate the risk of pneumothorax and reliably provide adequate anesthesia for surgery near the elbow.14,19 The infraclavicular approach has the added advantage of not requiring abduction during regional block, which would be painful in the presence of arm/forearm fracture.6 The various approaches to the brachial plexus blockade may be performed before surgical incision or after postoperative upper extremity neurologic function has been determined.
Although preoperative brachial plexus block reduces the intraoperative requirement of volatile anesthetic and opioids, and in theory provides pre-emptive analgesia, postoperative evaluation of neurologic function is not possible until block resolution. In addition, few outcome studies exist comparing regional and general anesthesia specifically for surgery about the elbow. However extrapolating the results of forearm and hand procedures under single-injection brachial plexus block versus general anesthesia, a regional technique is associated with improved analgesia, reduced opioid consumption and postoperative nausea and vomiting, and early hospital dismissal.15 Overall, there are early but no long-term benefits with a single-injection regional anesthetic technique compared with a general anesthetic. However, placement of an indwelling perineural catheter results in more substantial and lasting benefits, including avoidance of hospital admission/readmission, decreased opioid-related side effects and sleep disturbance, and improved rehabilitation.11,13,20 Thus, anesthetic management of patients undergoing elbow surgery is focused on postoperative analgesia, rather than intraoperative anesthesia to improve perioperative outcomes.
POSTOPERATIVE ANALGESIA
Patients undergoing major upper extremity surgery experience substantial postoperative pain. Indeed, 30% of patients undergoing ambulatory hand and elbow surgery reported moderate to severe pain at 24 hours postoperatively.16 Failure to provide adequate analgesia impedes early physical therapy and rapid rehabilitation, which are important for maintaining joint range of motion, facilitating hospital dismissal and preventing readmission. Traditionally, postoperative analgesia following major upper extremity surgery was provided by intravenous patient-controlled analgesia (PCA). However, opioids do not consistently provide adequate pain relief and often cause sedation, constipation, nausea/vomiting, and pruritus. Recently, clinical series have consistently reported that continuous brachial plexus block provided a superior quality of analgesia and surgical outcomes compared with systemic opioids but with fewer side effects.4,11 These reports suggest that continuous peripheral techniques may be the optimal analgesic method following elbow surgery. Appreciation of the indications, benefits, and side effects associated with both conventional and novel analgesic approaches is paramount to maximizing rehabilitative efforts and improving patient satisfaction.
MULTIMODAL ANALGESIA AND PERIPHERAL BLOCKADE
Multimodal analgesia is a multidisciplinary approach to pain management, with the aim of maximizing the positive aspects of the treatment while limiting the associated side effects. Because many of the negative side effects of analgesic therapy are opioid related (and dose dependent), limiting perioperative opioid use is a major principle of multimodal analgesia. Not surprisingly, the efficacy and side effects of analgesic therapy are major determinants of patient satisfaction. In a prospective survey of 10,811 patients, after adjusting for patient and surgical factors, moderate or severe post-operative pain and severe nausea and vomiting were associated with patient dissatisfaction.18 The use of single-injection and continuous brachial plexus techniques and a combination of opioid and nonopioid analgesic agents for breakthrough pain results in superior pain control, attenuation of the stress response, and decreases opioid requirements.
CONVENTIONAL ANALGESIC METHODS
Parenteral Opioid Analgesics
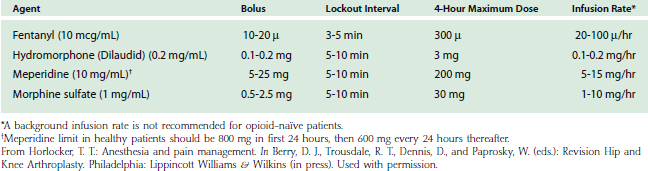
When adequate analgesia is achieved with systemic opioids, side effects, including sedation, nausea, and pruritus, are common. However, despite these well-defined side effects, opioid analgesics remain widely used for postoperative pain relief. Systemic opioids may be administered by intravenous, intramuscular, and oral routes. Current analgesic regimens typically employ intravenous PCA for 24 to 48 hours postoperatively, with subsequent conversion to oral agents. The PCA device may be programmed for several variables including bolus dose, lockout interval, and background infusion. The optimal bolus dose is determined by the relative potency of the opioid; insufficient dosing results in inadequate analgesia, whereas excessive dosing increases the potential for side effects, including respiratory depression. Likewise, the lockout interval is based on the onset of analgesic effects; too short of a lockout interval allows the patient to self-administer additional medication before achieving the full analgesic effect (and may result in accumulation/overdose of the opioid). A prolonged lockout interval will not allow adequate analgesia. The optimal bolus dose and lockout interval are not known, but ranges have been determined (Table 8-2). Varying the settings within these ranges appears to have little effect on analgesia or side effects. Although most PCA devices allow the addition of a background infusion, routine use in adult opioid-naïve patients is not recommended. There may be a role for a background opioid infusion in opioid-tolerant patients, however. Owing to the variation in patient pain tolerance, PCA dosing regimens may need to be adjusted in order to maximize the benefits and minimize the incidence of side effects. Despite the ease of administration and titratability, parenteral opioids may not provide adequate analgesia for major upper extremity surgery, particularly with movement, as evidenced by pain scores in the moderate to severe range in the first 2 days postoperatively.16
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree