The skin and its appendages constitute a complicated and highly regulated organ known as the integumentary system. Its functions are diverse and include protecting the body from an array of external insults by means of physical and immunologic mechanisms, regulating temperature homeostasis, providing sensory receptors for interactions with the environment, preventing water loss, and initiating vitamin D synthesis. As such, optimal athletic performance relies on the proper health and function of the integumentary system. It is therefore crucial that health care providers be able to recognize and effectively treat dermatologic disorders affecting the athlete. This chapter introduces disorders affecting athletes and focuses on providing a framework to evaluate the skin and effectively establish a diagnosis.
Cutaneous Infections
Cutaneous infections are among the most common dermatologic disorders that affect athletes. Making an accurate diagnosis is critical because infections may result in morbidity and lead to missed practices or game ineligibility. Familiarity with return-to-play guidelines is essential. Readers are encouraged to consult published guidelines, such as the 2013-2014 NCAA Sports Medicine Handbook, which is emphasized in this chapter. Guidelines for skin infections are primarily for athletes in contact sports, particularly wrestlers, because they are at highest risk for acquisition and transmission of cutaneous infections.
Bacterial Infections
Folliculocentric Infections: Bacterial Folliculitis, Furuncles, and Carbuncles
Bacterial folliculitis, furuncles, and carbuncles are infections that begin within hair follicles and can be conceptualized as a disease continuum. All of these infections are common among athletes, and one study documented that 25% of a high school’s varsity athletes experienced an episode of furunculosis over 1 year. Bacterial folliculitis presents as tender, follicular-based pustules, whereas a furuncle is a deeper inflammatory nodule. Furuncles often, but not invariably, arise from folliculitis ( Fig. 26-1 ). Carbuncles are more extensive, deeper, communicating masses that arise when multiple, closely set furuncles coalesce ( Fig. 26-2 ). Patients with carbuncles often are ill and present with fever and malaise. All are most commonly caused by Staphylococcus aureus and can evolve into an abscess or a pus-filled cavity. These infections typically arise in hair-bearing sites, particularly in areas subject to friction, occlusion, and perspiration, such as the neck, face, scalp, axillae, groin, extremities, and buttocks. Shaving of hair may promote infection, and any injury that disrupts skin integrity may lead to increased risk of infection. Diagnosis is made clinically, and if pus is obtainable, a bacterial culture should be submitted for organism identification and antibiotic sensitivity.


The initial therapy for bacterial folliculitis includes washing the affected area daily with an antibacterial soap (e.g., a chlorhexidine gluconate 2% to 4% solution or a benzoyl peroxide 10% wash) and applying a topical antibiotic such as mupirocin 2% ointment two to three times daily. In resistant cases, short courses of oral antibiotics can be used as directed by culture results. Simple furuncles can be treated with warm compresses to promote drainage. Fluctuant furuncles and carbuncles that have evolved into abscesses require incision and drainage, with oral antibiotic therapy considered on a case-by-case basis (e.g., severe or extensive disease, rapid progression, associated cellulitis, systemic illness, and/or the presence of comorbidities or immunosuppression).
Patients with recurrent disease should be evaluated for chronic nasal carriage of S. aureus, which may serve as a reservoir for infection. Eradication measures include intranasal application of mupirocin 2% ointment twice daily for 5 to 10 days, washing the skin and in particular the axillae and groin daily with chlorhexidine gluconate 2% to 4% solution, and use of dilute sodium hypochlorite (i.e., bleach) baths ( ![]() cup per
cup per ![]() tub or 13 gallons of water). Oral antibiotic therapy is not routinely recommended for decolonization.
tub or 13 gallons of water). Oral antibiotic therapy is not routinely recommended for decolonization.
National Collegiate Athletic Association (NCAA) wrestling guidelines require that wrestlers must be without any new skin lesions for 48 hours before competition, must have completed 72 hours of antibiotic therapy, must have no moist, exudative, or purulent lesions, and must not cover active purulent lesions to allow for participation.
Impetigo
Impetigo is a superficial bacterial infection of the skin. Both S. aureus and Group A Streptococcus can produce impetigo, but S. aureus is the more common etiology in industrialized nations. Athletes who engage in contact sports are at higher risk for acquisition of disease via trauma and disruption of skin integrity.
Two presentations are recognized: bullous and nonbullous impetigo. Nonbullous impetigo typically begins as a transient vesicle or pustule that evolves into a honey-colored crusted plaque with surrounding erythema ( Fig. 26-3 ). Infection is most common on the central face. The differential diagnosis includes herpes simplex, contact dermatitis, and atopic dermatitis. Bullous impetigo is characterized by superficial vesicles and bullae that rupture after 1 to 2 days, leading to weeping erosions that eventually heal over. Contact dermatitis, herpes simplex, bullous arthropod bites, drug rash, burns, and erythema multiforme should be ruled out.

Diagnosis is usually suspected based on the clinical appearance, but bacterial culture is recommended for diagnostic confirmation and antibiotic sensitivity, given the increasing prevalence of methicillin-resistant S. aureus (MRSA) infections. Initial treatment should include local wound care with soap and water and use of topical mupirocin 2% ointment three times daily. For widespread infections, penicillinase-resistant antistaphylococcal antibiotics (cephalexin or dicloxacillin) can be considered, pending antibiotic sensitivity results. Empiric MRSA coverage can be considered in areas with high prevalence of infection. Return-to-play guidelines are identical to those for bacterial folliculitis (described in the previous section).
Cellulitis/Erysipelas
Cellulitis and erysipelas are common infections of the skin, usually caused by S. aureus and Group A Streptococcus . Cellulitis is defined as an infection of the dermis and subcutaneous fat, whereas erysipelas is a more superficial variant affecting the upper dermis and lymphatic vessels. Less common causative organisms include Haemophilus influenzae , groups B and G Streptococcus , enteric gram-negative rods, coagulase-negative Staphylococcus , and Streptococcus pneumoniae .
Cellulitis classically presents as a unilateral erythematous, warm, tender, indurated, and edematous plaque with indistinct margins. Erysipelas is similar in appearance but tends to be more sharply defined with a bright red color ( Fig. 26-4 ). Occasionally cellulitis may undergo bullae formation with necrosis, resulting in localized skin sloughing and ulcer formation. Systemic symptoms are variable, with fever, chills, malaise, and regional lymphadenopathy most common. The absence of pain or pain out of proportion to the clinical appearance should prompt consideration of a deeper infection, such as necrotizing fasciitis or myonecrosis.

Diagnosis is primarily clinical, based on the history and clinical presentation. Culture studies of the leading edge of cellulitic plaques are not indicated in routine, uncomplicated cellulitis or erysipelas because of their low yield but should be obtained in the presence of open, fluctuant, or bullous lesions. The differential diagnosis is extensive and includes deep venous thrombosis, superficial thrombophlebitis, Sweet syndrome, contact dermatitis, stasis dermatitis, arthropod bites, panniculitides, necrotizing soft tissue infections, and erythema migrans.
Treatment depends on the severity of infection, with more severe cases necessitating hospitalization and parenteral antibiotics. Routine, uncomplicated infections can be treated in the outpatient setting, with β-lactam antibiotics (e.g., dicloxacillin and cephalexin) remaining empiric first-choice therapy. Simple measures including bed rest and elevation of the involved site should be routinely emphasized, but warm compresses should be avoided because they predispose the skin to vesicle formation. Empiric MRSA coverage (e.g., clindamycin, trimethoprim-sulfamethoxazole, and tetracyclines) should be considered on a case-by-case basis, because studies have shown that empiric β-lactam antibiotics continue to be the most cost-effective choice with fewer adverse events in the treatment of uncomplicated cellulitis, even in areas of high rates of MRSA prevalence. Return-to-play guidelines are identical to those for bacterial folliculitis (described in the section Folliculocentric Infections: Bacterial Folliculitis, Furuncles, and Carbuncles).
Pitted Keratolysis
Pitted keratolysis is a superficial bacterial infection of the feet caused by bacteria of the Corynebacterium genus, particularly Kytococcus sedentarius . Numerous small crateriform punched-out pits are seen predominantly on the thickest areas of the plantar surface and may coalesce to form large, irregular, scalloped lesions ( Fig. 26-5 ). Less commonly the toe web spaces are affected. Infection usually occurs in younger males with sweaty feet, but it can affect all ages and sexes. Patients note a distinctive malodor, and some may describe a slimy sensation. Moisture, occlusion, and tropical climates are predisposing factors. The clinical appearance is distinctive, but the differential diagnosis of interdigital involvement includes tinea pedis and erythrasma. Therapeutic options include thorough cleansing combined with use of a clindamycin 1% solution or a benzoyl peroxide 10% wash or 5% gel. Dilute sodium hypochlorite (bleach) soaks may speed resolution. Adjunctive and preventative measures aim at reducing moisture and include keeping feet dry by changing socks frequently, using absorptive foot powders (e.g., microporous cellulose and talc powder), and applying antiperspirants topically (e.g., aluminum chloride 20% solution nightly). Footwear should be replaced as indicated.

Erythrasma
Erythrasma is an underdiagnosed superficial bacterial skin infection caused by Corynebacterium minutissimum that is commonly confused with dermatophyte infections. The condition is most common in warm, temperate climates and leads to clinical disease, particularly in folds of the skin, such as the inguinal creases, axillae, or interdigital toe web spaces. Lesions are often pinkish-tan, scaly patches, and unlike dermatophyte infections, they do not demonstrate an active, raised advancing border ( Fig. 26-6 ). Erythrasma can be asymptomatic or mildly pruritic.

The diagnosis can be confirmed by demonstrating coral-red fluorescence with Wood’s lamp (ultraviolet A [UVA]) examination. Of note, this finding may be absent in patients who have recently washed the involved area. Potassium hydroxide (KOH) preparations of skin scrapings will be negative. The differential diagnosis often includes other intertriginous eruptions, such as dermatophytoses (e.g., tinea cruris or tinea pedis), candidiasis, seborrheic dermatitis, contact dermatitis, and inverse psoriasis. First-line treatment is with topical erythromycin 2% solution, clindamycin 1% solution, or benzoyl peroxide 5% gel. Oral doses of clindamycin and erythromycin are also effective.
Pseudomonal Folliculitis (Hot Tub Folliculitis)
Use of hot tubs, whirlpools, or swimming pools can lead to development of a self-limited folliculitis caused by Pseudomonas aeruginosa . Lesions present as pruritic, follicular-based papules and pustules that develop 1 to 5 days after use of bathing facilities ( Fig. 26-7 ). Occasionally patients may experience fever, chills, and lymphadenopathy. Lesions may be generalized over the body, may appear underneath clothing, or may be localized if only a certain body site is immersed. The differential diagnosis includes staphylococcal folliculitis, Pityrosporum folliculitis, and arthropod bites. Bacterial culture of pustule contents can be performed to confirm the diagnosis. In immunocompetent persons without systemic involvement, the infection is self-limited and no treatment is necessary. For athletes who require treatment, ciprofloxacin, 250 mg by mouth twice daily for 7 days, is recommended. Suspected water sources should be inspected for adequate pH levels and chlorine content. Return-to-play guidelines are identical to those for bacterial folliculitis (described in the section Folliculocentric Infections: Bacterial Folliculitis, Furuncles, and Carbuncles).

Fungal Infections
Dermatophytoses
The three fungal genera Trichophyton , Microsporum , and Epidermophyton comprise more than 40 species and are collectively referred to as “dermatophytes.” These fungi can be found living in soil and on the skin of animals and humans. Common infections in humans are colloquially referred to as “jock itch” (tinea cruris), “athlete’s foot” (tinea pedis), and “ringworm” (tinea corporis). Dermatophytes can infect any superficial skin surface, including appendageal structures such as hair follicles and nails, but they cannot penetrate into the dermis or infect mucous membranes. Athletes are at higher risk for infection, because perspiration and trauma facilitate growth and penetration of dermatophytes on the skin. Additionally, fungi are transmitted via skin-to-skin contact and use of shared facilities and items (such as locker rooms and towels). Wrestlers in particular are at risk for tinea corporis.
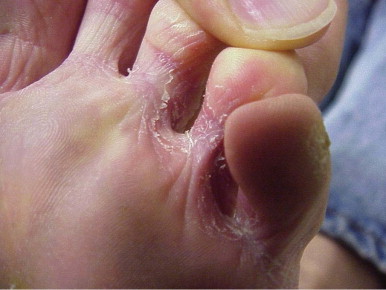
Dermatophyte infections of the skin, no matter the location, typically demonstrate a red, scaly, raised, advancing border, which is the most useful diagnostic clue on physical examination. Lesions on the body variably show an annular or ring-shaped appearance. Tinea cruris favors the inguinal folds and advances onto the thighs ( Fig. 26-8 ). As opposed to candidiasis, tinea cruris almost never involves the scrotum. Tinea pedis classically presents with scaling, maceration, and erythema in the interdigital toe web spaces (particularly the fourth) but can involve the entire foot ( Fig. 26-9 ). Tinea capitis is most common in children and presents as red, scaly patches of alopecia.

The differential diagnosis is location dependent and extensive but most commonly includes seborrheic dermatitis, eczema, or alopecia areata in the scalp; contact dermatitis, atopic dermatitis, psoriasis, tinea versicolor, pityriasis rosea, or subacute cutaneous lupus erythematosus on the body; candidiasis, erythrasma, seborrheic dermatitis, psoriasis, or contact dermatitis in the groin; and dyshidrotic eczema, contact dermatitis, psoriasis, candidiasis, and scabies on the feet. Diagnosis can be suspected on clinical examination but should be confirmed with a diagnostic test. Scraping the advancing edge of a lesion for microscopic examination with 10% KOH is an in-office procedure that is easy to perform. The presence of septate, branching hyphae is diagnostic. Alternatively, hair shafts, skin scrapings, or swabs taken from the scalp can be submitted for fungal culture.
Multiple systemic and topical antifungal agents are available to treat dermatophyte infections of skin, hair, and nails. Most cases of tinea corporis, cruris, and pedis can be successfully treated with topical therapy alone. Terbinafine 1% cream or ketoconazole 2% cream applied twice daily for several weeks are good first-line treatments. Consideration of an oral antifungal agent such as fluconazole, 200 mg by mouth weekly for 2 to 4 weeks or terbinafine, 250 mg by mouth daily for 1 to 2 weeks can be considered in widespread, inflammatory, or refractory cases. Treatment of tinea capitis always requires systemic therapy, with griseofulvin ultramicrosized capsules, 15 mg/kg/day in divided doses for 8 weeks, remaining first-line treatment. Consultation with a dermatologist is recommended in severe cases, after treatment failure, and when the diagnosis is unclear.
NCAA guidelines mandate that for wrestlers to return to competition, a minimum of 72 hours of topical therapy is required for skin lesions and two weeks of oral antifungal therapy is required for scalp lesions. Wrestlers with extensive and active lesions may be disqualified, with infection determined by KOH preparation or a review of the therapeutic regimen.
Malassezia
The fungal genus Malassezia (formerly Pityrosporum ) includes several species of lipophilic yeasts that form part of the normal skin flora and flourish in warm, moist, sebum-rich body areas. Under certain circumstances, proliferation of the yeast can produce the skin conditions tinea versicolor and Pityrosporum folliculitis. By the nature of their physical activity, young athletes are at higher risk for the development of these infections.
Tinea versicolor presents as finely scaling macules that coalesce, forming irregularly shaped patches of pigment alteration. Lesions may be tan to brown or white to pink in color and are most commonly located on the back, chest, abdomen, proximal upper extremities, and neck ( Fig. 26-10 ). A clue to the diagnosis includes the extensive dustlike scaling that can be produced by scratching the lesions. On microscopic examination with 10% KOH, the scale will show clusters of oval, budding yeast cells and short, septate hyphae. The differential diagnosis usually includes tinea corporis, pityriasis rosea, and progressive macular hypomelanosis. Pityrosporum folliculitis presents as follicular, erythematous, 2- to 3-mm papules and pustules on the chest and back and is due to Malassezia yeast proliferating within the hair follicle ( Fig. 26-11 ). The diagnosis is often confused with bacterial folliculitis and acne vulgaris.


Both conditions are treated with topical antifungal agents such as ketoconazole 2% shampoo and selenium sulfide 2.5% lotion, which are lathered onto the skin for 10 minutes and rinsed off. Patients should perform this treatment daily for at least 10 days, with tapering of frequency to weekly use thereafter for 1 to 2 months for prevention. Occasionally, oral antifungal drugs are used in persons with resistant disease.
Viral Infections
Herpes Simplex
Infection by human herpesvirus 1 (HSV-1) and human herpesvirus 2 (HSV-2) is common in both the general population and among athletes, with herpes labialis and genital herpes being the most familiar clinical presentations. After primary acquisition of the virus from direct skin contact, the virus replicates at the site of inoculation, with variable production of a primary skin lesion. The virus spreads to infect sensory nerve terminals and travels by retrograde axonal transport to neuronal nuclei in regional sensory ganglia, where it establishes latent, lifelong infection. The virus will subsequently reactivate with anterograde axonal transport to the original site of primary infection.
Contact sports place athletes at higher risk for both acquisition and transmission of the virus, whereas excessive UV radiation exposure (e.g., among skiers) may place certain athletes at risk for reactivation. HSV outbreaks are well described among wrestlers (“herpes gladiatorum”) and rugby players (“scrum pox”). HSV lesions are divided into primary and recurrent infection. Either may begin with a prodromal phase (marked by pain, burning, stinging, and itching), before development of erythema and edematous red papules, which subsequently become vesicles. Systemic symptoms (e.g., fever and malaise) are most common in primary infections. Classic skin lesions are small (2 to 5 mm) grouped vesicles on an erythematous base. Confluent vesicles may produce a scalloped border. Lesions soon ulcerate, develop an adherent crust, and eventually resolve within 5 to 14 days. Among wrestlers, the most common locations are the head and neck ( Fig. 26-12 ), but they can occur anywhere, including the trunk and extremities. It is critical to note that the majority of patients with HSV are asymptomatic but can transmit the virus via asymptomatic shedding.











