Fig. 4.1
An intra-operative clinical photograph revealing extensive soft-tissue injury on the posterior aspect of the knee with an associated recurvatum deformity
The state of the skin is also quite revealing as to the direction, force and mechanism of injury. Pay particular attention to observe the anterior aspect of the tibia for the presence of bruising; this is a common site for a haematoma in the setting of a PCL injury as a result of direct impact to the anterior aspect of the tibia following a fall on the flexed knee. In addition, be mindful to inspect the posterior aspect of the knee, which is also instructive as to the extent of the injury (Fig. 4.2). The shape of the joint and upper and lower limb segments, their general alignment and any atrophy or swelling (localized or diffuse) should be noted; all of this preceding the ‘laying on of hands’.
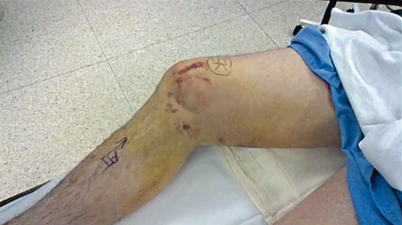

Fig. 4.2
Ecchymosis on the medial aspect of the knee with a positive ‘dimple’ sign (white arrow), indicative of an irreducibly dislocated knee with soft-tissue interposition between the femur and tibia
Feel
Vascular Assessment
The physical examination continues with an evaluation of the vascular status of the lower extremity. Be observant for signs of vascular injury (Table 4.1). Examine the temperature of the distal extremity. Palpate for both the dorsalis pedis and posterior tibial pulses. Hard signs should alert the treating surgeon to the need for emergent vascular imaging and involvement of a vascular surgeon. Soft signs, on the other hand, are less reliable; however, at the very least they should heighten the clinical suspicion and prompt the use of further vascular studies.
Table 4.1
Signs of vascular injury
Hard signs | Active haemorrhage |
Distal ischemia | |
Expanding haematoma | |
Soft signs | Limb colour |
Capillary refill |
Neurological Assessment
Assessment of neurological function in the setting of knee dislocation can be challenging. In the context of a multisystem injury, the compliance of the patient may be compromised by a head injury or intoxication. The peroneal nerve is the most commonly injured nerve, due to its proximity, with less frequent injury to the tibial nerve [20]. Both the sensory and motor function of these nerves must be evaluated and documented, particularly before and after any manoeuvres or intervention.
The Form of the Knee
Palpation of the knee requires a subtle gradient of force application. The examiner should commence with the normal side with sufficient pressure to feel the subtleties of the knee’s form. The process complements the visual inspection.
Increasing pressure may be applied to distinguish induration—the hardness of the different tissue planes. Induration provides insight into the severity and site of the injury. It is often helpful to bend the knee during this process to localize the source of the injury, and identify specific anatomical structures.
The skin, soft tissues and bones should be palpated methodically in an orderly manner to distinguish between normal and altered anatomy. The precise relationship of tender points to the joint line and ligamentous attachments is instructive in identifying the site of the lesion.
The final palpation is conducted with slightly more force to identify tenderness and/or gaps in the underlying soft tissue. It is critical that the patient is aware that you will be probing with increased vigour and can expect a certain degree of discomfort. It is important not to neglect the extensor mechanism of the knee, in particular the inferior pole of the patella, which, if tender, may indicate a concomitant injury to the PCL , which may have resulted from an anteriorly applied force; e.g. a dashboard injury.
Move
Examination of the knee should consist of active and passive motion. It is helpful to ask the patient to move the well leg within the range of motion that is comfortable and possible, which provides the standard for comparison. In an acutely injured knee, this portion of the examination may be painful. The examiner should be confident and decisive and try to avoid excessive force, which can induce pain and cause guarding or even further injury.
Ask the patient to move the injured leg within the limits of comfort. This process is important in demonstrating the range of motion available to position the leg for the ligamentous examination. Passive movement of the joint may be carried out gently to assess any resistance to full extension or further flexion. Focus on the effect of passive movement by looking at the patient’s face.
Limits of Motion
An initial assessment of the limits of motion is very important. First, start by asking the patient to fully extend the knee. An inability to fully extend the knee may indicate meniscal pathology, hamstring spasm or a comprised extensor mechanism. This assessment is very beneficial also in ascertaining the need for acute surgical intervention or the requirement for preoperative physical therapy to improve the range of motion.
Flexion, both active and passive, is tested next. Note the limits of motion with each test and try to identify the location of any discomfort. Knee flexion of at least 90° is required to be able to carry out a conclusive examination of the PCL . If this angle cannot be achieved initially, the patient should be re-examined sequentially following physical therapy until it is reached. Ice may be helpful in reducing swelling and pain and facilitate an improved physical examination. Failing this, an examination under anaesthetic (EUA) may be warranted. Joint line tenderness on maximal flexion may indicate meniscal pathology, which should not be overlooked.
Special Tests
There are a myriad of special tests, which may be carried out to assess the knee. The key factor is to choose a series of tests, which are comprehensive enough to assess the entirety of the knee and are also reproducible to the examiner. Listed below are preferred tests of the authors.
Varus/Valgus Stability
If the patient can reach hyperextension, it is the ideal position to start. Stability in this position infers that the medial and lateral capsuloligamentous structures and the PCL are intact. This finding alone is extremely informative. However, laxity in this position to either varus or valgus angulation is a worrying sign, indicating disruption of key ligamentous structures. If in hyperextension the knee is lax to varus angulation, then the posterolateral corner and the PCL are probably disrupted (Fig. 4.3). Likewise, if in hyperextension the joint is lax to valgus angulation, the medial capsuloligamentous structures and the PCL are probably disturbed (Fig. 4.4).
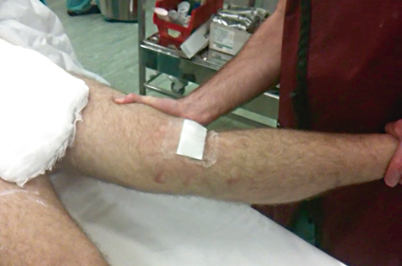
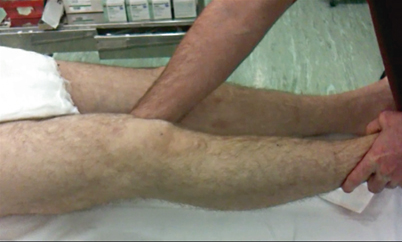

Fig. 4.3
Valgus instability in hyperextension: Valgus opening in full extension with no end point. This finding is indicative of injury to not only the medial structures but also the posteromedial capsule and likely the posterior cruciate ligament

Fig. 4.4
Testing of varus stability in full extension: The knee is tested in full extension to assess if there is lateral and posterolateral corner instability
At 0° flexion, the ACL and PCL are sufficiently slackened to allow diagnostic evaluation of medial or lateral capsular injuries by application of varus and valgus angulation. Further flexion to 30° facilitates examination of the isolated medial and lateral collateral ligaments (LCLs) because, in this position, the posterolateral and posteromedial corners, in addition to the cruciate ligaments, are relaxed.
Anteroposterior Translation
Anteroposterior glide is best determined with the fingers. Prior to performing any dynamic manoeuvres, be confident that you can palpate both the medial and lateral joint line. As the examination of both posterior and anterior drawers is conventionally performed in the same position, one must be able to distinguish between subtle changes in anteroposterior translation.
An anterior drawer is only present when one has proved that the posterior drawer is absent. Werner Müller [21]
The first component to these series of tests is to assess the relationship of the tibial plateau to the femur in the sagittal plane. Position the patient supine with the hips flexed to 45° and the knee at 90° of flexion. Prior to performing any tests, keen surveillance is essential. Flex both knees together, and inspect the silhouette of the knee in the sagittal plane, from each side (Fig. 4.5). Begin with the uninjured side. The key structures to observe are the anterior tibial tubercle and the association with the patellar tendon and the anterior aspect of the patella. In the presence of a disrupted PCL , and more often than not a concomitant posteromedial or posterolateral lesion, the tibial plateau will be translated posteriorly with respect to the femur, which is termed ‘posterior sag’.
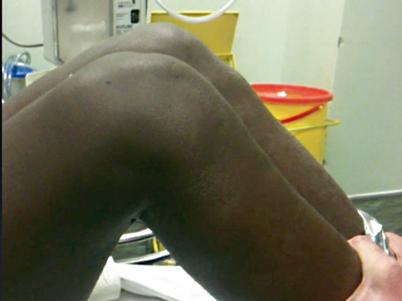

Fig. 4.5
Inspection of relative tibial translation: The patient is placed supine on the table with hips flexed to 45° and knees to 90°. Observe the silhouette of the knees. Note the loss of the contour of the joint line and prominence of the tibial tuberosity on the right knee compared to the opposite side, suggesting posterior subluxation of the tibia
Müller also describes a test where the patient is asked to actively extend the knee from the flexed position [21]. The force of the quadriceps will translate the tibia anteriorly to allow the knee to straighten, which is visible from the sagittal position. This test is also known as the ‘quadriceps active’ test. A modification of this test is performed by holding the foot and asking the patient to contract his/her quadriceps against resistance.
Pure posterior glide involves symmetrical posterior translation of both tibial plateaus with neither internal nor external rotation. This is a rare situation. Posterior drawer alone without any peripheral lesions is due to an isolated PCL lesion, which is not a common finding. Peripheral structures compensate for the absence of a PCL and give rise to a hard end point at the extreme of posterior translation [22]. The accuracy of the interpretation can, therefore, be uncertain. Associated posteromedial or posterolateral lesions also influence the response to posterior translation. A soft end point is typically present in this circumstance. Failure to discriminate between this finding and an anterior drawer is not unusual, as injury to the anterior cruciate ligament (ACL) is a more common finding.
The Posterior and Anterior Drawer Test
The foot is fixed firmly in a neutral position with the knee flexed to 90°. The posterior aspect of the proximal tibia is held with both hands, placing the fingers into the popliteal fossa (Fig. 4.6). The movement for posterior drawer first requires the joint to be reduced to a neutral position. It is, therefore, advisable to place the thumbs of each hand on either side of the patellar tendon so that one can palpate any posterior subluxation and to confirm that the joint is in neutral alignment. Feel the tightness of the hamstrings with the index and middle fingers and ask the patient to relax. The tibia is then pulled forward in order to feel the anterior shift of the tibial plateau. The tibia is then pushed backwards by applying a force with the thumbs on the tibial tuberosity. This manoeuvre is gently repeated, as required. It is important to be conscious of the end point in the anterior and posterior direction. Observe for a change in shape of the joint with each sequential movement. It is possible to increase the force of the anterior pull by placing the thumbs against the femoral condyle and levering the tibia forward. The parallel orientation of the thumbs on either side of the patellar tendon also facilitates detection of any rotatory movement, which may occur in addition to anteroposterior glide. The extent of translation can be quantified according to the International Knee Documentation Committee (IKDC) values (Table 4.2) or based on grading of the step-off (Fig. 4.7) [23].
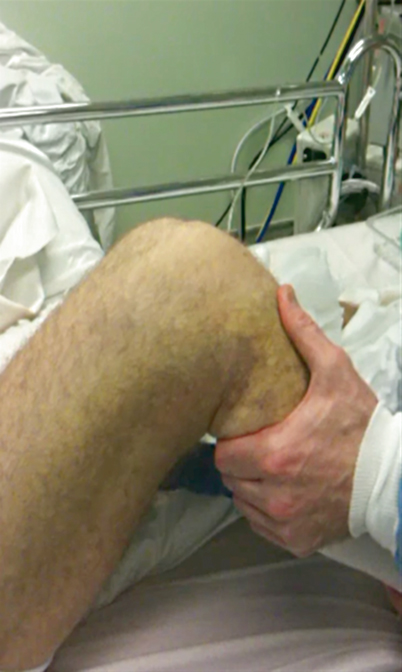
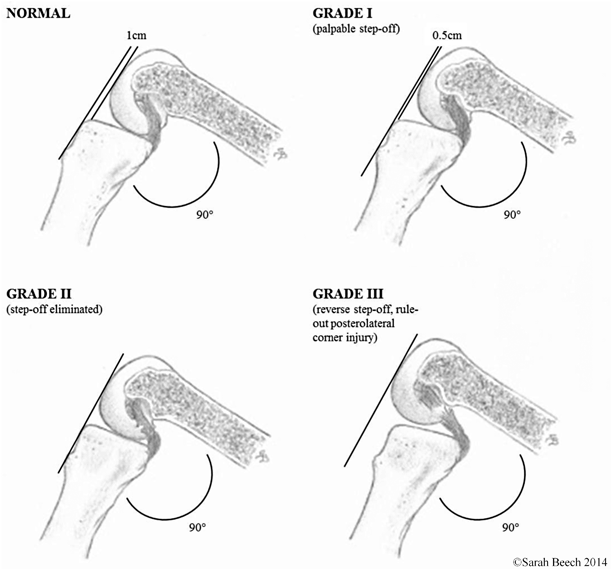

Fig. 4.6
Posterior drawer testing in neutral rotation. The patient is supine with the knees flexed to 90°. A posterior force is exerted anteriorly on the proximal tibia. Translation at the joint line can be appreciated with the thumbs

Fig. 4.7
Assessment of step-off in the PCL-deficient knee as classified by Petrie and Harner [23]. PCL posterior cruciate ligament. (Figure courtesy of Sarah Beech)
Table 4.2
IKDC—Grading of joint translation
Normal | Nearly normal | Abnormal | Sev. abnormal |
|---|---|---|---|
0–2 mm | 3–5 mm | 6–10 mm | > 10 mm |
Rotatory Stability
The appreciation of increased rotatory excursion requires careful attention to detail and can be subtle. Failure to diagnose and rotatory instability may result in failed surgical treatment and a poor prognosis. The pathophysiology of injuries to the posteromedial and posterolateral corners can be difficult to interpret with physical examination, and, therefore, it is advisable to spend some time teasing out abnormalities that are detected.
The Anteromedial Rotatory Drawer
The patient is supine with the hip flexed to 45°, the knee flexed at 90° and the foot fixed on the examining table in 15° of external rotation. In this position, the ACL and collateral ligaments are lax, which permits anterior and lateral displacement of the medial tibial plateau. An anteriorly direct force is applied to pull the tibia directly forward. Depending on the severity of injury to the medial capsule, the medial collateral ligament (MCL) and the ACL, there will be a progressive increase in the pathological external rotation of the tibia with respect to the femur. The medial tibial plateau glides forward while the lateral plateau hardly moves at all. The axis of rotation occurs around the PCL on the lateral wall of the medial femoral condyle. If the ACL is intact, this drawer is purely rotational. Slocum, who was the first to describe this test in 1968, stated that greater than 30° external rotation should be considered pathological [24]. Accordingly, it is very important to rule out the presence of hypermobility of the contralateral limb to avoid false positive results. The quantification of this test, as proposed by Slocum, falls outside the IKDC classification, and is listed in Table 4.3.
Table 4.3
Slocum classification of rotatory instability
1+ | Half a thumb—13 mm |
|---|---|
2+ | Between half and three quarters of a thumb—13–19 mm |
3+ | Greater than three quarters of a thumb—> 19 mm |
The Anterolateral Rotatory Drawer
This test is performed in the same position with the foot internally rotated. A positive drawer in this position is indicative of a deficient ACL, which according to Noyes is the first restraint to anterior shift in internal rotation. This manoeuvre also examines the integrity of the anterolateral femoral tibial ligament [25]. Anterolateral rotation is only possible if these fibres are deficient.
Posterior Rotatory Stability
The addition of rotation to the posterior drawer is used as a further test to assess the integrity of the PCL and posterior corners of the knee. The key determinant in drawing conclusion from these tests is quantifying the ratio of translation to rotation that occurs, which should be compared to posterior drawer in neutral rotation. In internal rotation, the PCL tightens and apposes the surface of the tibia to the femur, preventing any posterior sliding of the medial tibial plateau. If the PCL is ruptured the axis of rotation shifts from a central position to a lateral position, provided the posterolateral structures are intact. This results in the medial tibial plateau translating posteriorly to a greater extent than the lateral tibial plateau. Translation predominates over rotation. This is defined, therefore, as a posteromedial translatory rotatory laxity.
The Posterolateral Rotatory Drawer
The patient is in the same position as for all other drawer tests. The foot is fixed in slight external rotation and posterior directed force is applied to the anterior tibial tuberosity [26]. In this position, the PCL relaxes so that there can be rotatory and translatory posterolateral laxity. The ratio of translation to rotation should be compared to that observed when the posterior drawer is in the neutral position. Pure rotatory laxity occurs with an isolated posterolateral corner injury. There is an increase in external rotation, but posterior translation will not increase with external rotation of the foot, as the PCL is intact. The result is a decrease in the ratio of translation to external rotation. In the case of a PCL rupture without injury to the posterolateral corner, application of a posterior drawer in this position will result in increase in the ratio of posterior translation to external rotation as the centre of rotation is displaced peripherally.
The Posteromedial Translatory Rotatory Drawer
Internally rotating the foot tightens the PCL at 90° of knee flexion , resulting in coaptation of the femur and tibia, which prevents posterior sliding of the medial tibial plateau. Application of a posteriorly directed force to the anterior tibia, in this setting, will result in a hard end point, thereby confirming the presence of an intact PCL. However, if the PCL is deficient, coaptation does not occur and the axis of rotation shift laterally, provided the posterolateral structures are intact, which will result in a greater degree of medial-to-lateral tibial subluxation. In the absence of a PCL and a disrupted posterolateral corner, the axis of rotation is more centrally located, allowing posterior translation of the lateral tibial plateau along with the medial tibial plateau [27]. It is, therefore, necessary to assess the magnitude of the relative translation between the lateral tibial plateau and the medial tibial plateau. The more this ratio increases, the more posterior laxity become global.
The Lachman Test
The Lachman test is one of the most sensitive tests to assess ACL integrity when performed by experienced hands [28]. This test does require practice to master and relies upon having a relaxed and compliant patient. The advantage this test has over the anterior drawer relates to the fact that it is not always possible to flex the patient’s knee to 90° in an acutely injured knee, in the setting of an effusion or haemarthrosis, whereas flexion to 30° is normally attainable. The reflex contraction of the hamstrings can be strong, particularly in an athletic population, and has a greater effect on preventing anterior translation at higher degrees of flexion. Finally, the bony osteology of the medial compartment and the addition of the secondary restraints, provided by the medial meniscus and posterior oblique ligament (POL), are more effective in resisting anterior translation at 90° than 30°.
The examination is performed with the patient supine and the examiner on the side of the knee to be examined. With the patient relaxed, the knee is placed in 30° of flexion. While stabilizing the femur with one hand, place the other hand on the posterior aspect of the upper tibia and apply an anterior force to draw the tibia forward on the femur (Fig. 4.8). When the test is positive, there is an anterior shift of the tibia with respect to the femur with a soft end point. This is in contrast to a hard end point when the ACL is still intact. A soft end point, which occurs with increased anterior excursion, denotes that the ACL is ruptured without doubt. However, a hard end point is more difficult to interpret as it may not indicate that the ACL is intact for two reasons—the ACL may be simply attenuated and stretched and tighten at a greater degree of tibial excursion, or the secondary peripheral structures are compensating to produce the hard end point. In this test, as in any test, it is very important to compare with opposite side to rule out any congenital laxity and quantify the side-to-side difference in translation.
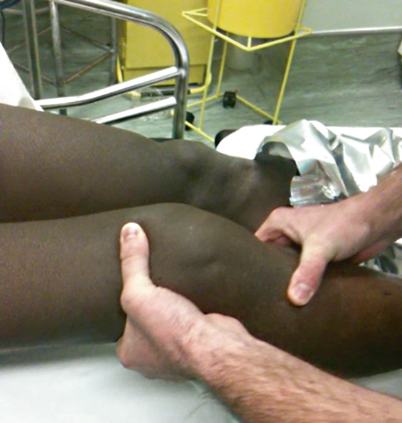

Fig. 4.8
The Lachman test: The knee is flexed to 30°. The proximal tibia is pulled anteriorly with one hand while the femur is held steady with the opposite hand
The Recurvatum Test
Testing in full extension may also reveal a recurvatum deformity, which points to a posterolateral lateral injury or possibly even a posteromedial injury. Classically, the description of this test involves the examiner lifting the patient’s great toe and observing the relative amount of genu recurvatum present [29]. The amount of relative knee hyperextension present should be compared to the contralateral normal knee and may be measured by a goniometer or heel-height differences. In addition to the hyperextension seen, the tibia commonly rotates into external rotation and a varus alignment is often noted at the knee (Fig. 4.9). A positive finding of this test should alert the examiner to the possibility of a posterolateral corner injury, which is typically with an associated cruciate ligament injury [30, 31].
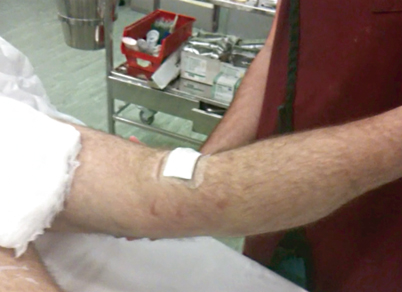

Fig. 4.9
Recurvatum deformity: Holding the leg by the foot or toe, the knee is seen to hyperextend. This finding is indicative of a PCL rupture and suggestive of an injury to the posterolateral corner of posteromedial structures. PCL posterior cruciate ligament
Prone Examination of Knee
The prone examination affords the opportunity of assessing the posterior aspect of the knee. Initial observation is carried out to identify the presence of any scars, swellings, atrophy or bruising on the posterior aspect of the lower leg. Extra-articular bruising is often easier to appreciate posteriorly, as it typically accumulates here, as the lower limb is usually in a supine, dependent position following injury. This position also facilitates further testing of rotational stability through the dial tests.
The Dial Test
The dial test is performed to determine the amount of external rotation of the tibia, which occurs on the femur. Conventionally, it is used to differentiate between isolated posterolateral corner injury and a combined PCL and posterolateral corner injury. The test is performed by flexing both knees to 30° and maximally externally rotating both feet (Fig. 4.10). Compare the uninjured side to the affected side and assess for any increase in rotation. The test is repeated at 90° of flexion. An isolated posterolateral corner is diagnosed if there is a positive dial test at 30° with a normal dial test at 90°. A positive dial test at 90° usually indicates a combined posterolateral corner and cruciate ligament injury, but it may also indicate a severe medial knee injury, which can be isolated or combined with a PCL disruption.
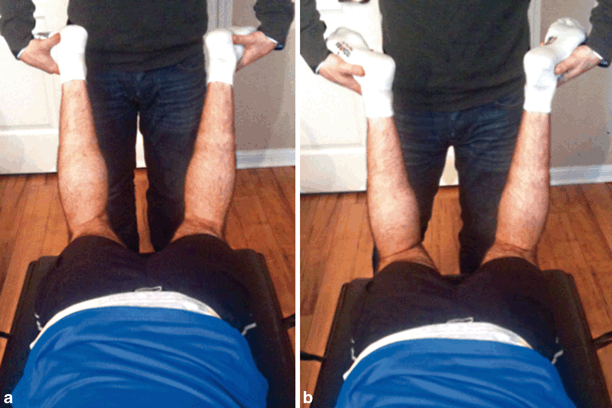

Fig. 4.10
The dial test: The patient is positioned prone. A comparison of external rotation of both feet is made at (a) 30° and (b) 90° of flexion
Functional Tests
Of particular importance, is the use of functional and dynamic examinations, which require the assumption of different positions; standing, walking, or running gives the examiner a keener appreciation of the limitation of function of the joint and the patient. It is vital to recognize mechanical mal-alignment, which may have a significant influence on the outcome of a soft tissue reconstruction and may point to the requirement for bony correction. Pay particular attention to a thrust when the patient is walking. Adequate exposure to appreciate subtle compensatory movement of the lower limb when ambulating is very important. In complex instabilities, it is often beneficial to film functional activities and to examine them in slow motion. A comparison can be made postoperatively to assess any changes with treatment.
Diagnostic Studies
Vascular Studies
Aside from physical examination, additional vascular studies may be warranted in the context of an acute knee dislocation or multi-ligamentous injury. Many surgeons advocate that an ankle-brachial index (ABI) be performed in all patients suspected of having a knee dislocation [32]; however, this is not universal practice. The ABI is a fast and reliable test with relatively no associated morbidity to the patient. The ABI is recorded by means of a Doppler ultrasound probe by measuring the systolic pressure in the affected leg at a level just proximal to the ankle and dividing this value by the systolic pressure in the ipsilateral arm. A value of > 0.9 has been found to be a reliable marker of normal arterial patency. Further investigation by arteriography or imaging with vascular reconstructions is indicated in the presence of abnormal physical findings and an ABI < 0.9.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








