Chapter 26 Classification of Knee Dislocations
INTRODUCTION
The concept of a dislocated knee has changed markedly over the past few decades. In 1971, Meyers and Harvey10 predicted that most orthopaedists would not see more than one knee dislocation in their entire career. However, evidence indicates that knee dislocations are being seen with increasing frequency for a variety of reasons. Increasing trauma, changes in automotive design, and recognition of spontaneously reduced knee dislocations have all added to the increased incidence. The increasing number of knee dislocations has created the need for a classification system that will help guide the management of these complex injuries. Classification systems should be simple and reproducible; they should give information to the clinician that will be helpful in making treatment decisions and aid in the communication of like injuries as well as in developing prognoses for injuries. This chapter reviews the shortcomings of the older classification systems of knee dislocations and presents the anatomic classification system that is simple, accurate, reproducible, and useful.18–20,28
DEFINITION OF KNEE DISLOCATION
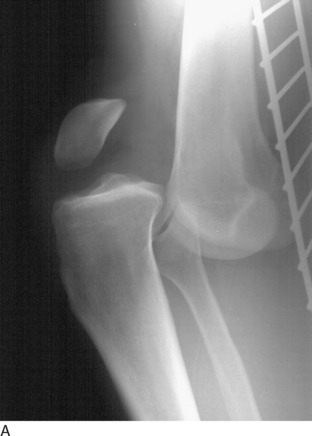
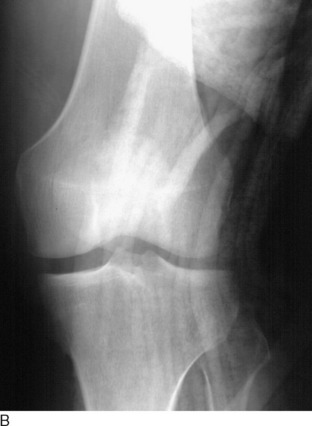
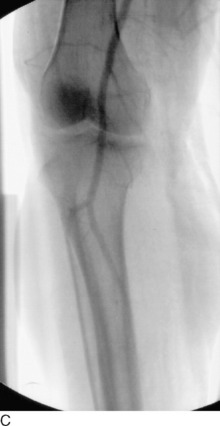
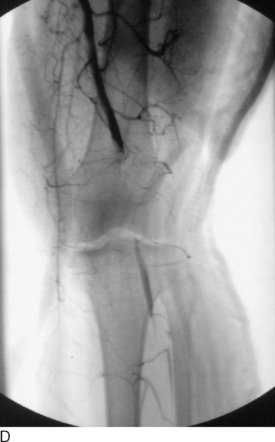
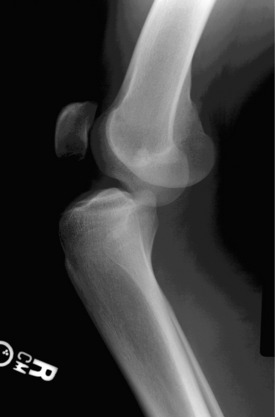
Classically, a knee dislocation was defined as greater than 100% displacement of the tibiofemoral articulation. This displacement had to be present on either physical examination or radiographic imaging. Since the 1990s, several authors have recognized the existence of “reduced” knee dislocations. These are knees that present to the treating physician reduced but have multiple injured ligaments (usually including both cruciates) and gross instability on stress testing. Some of these injuries represent a spontaneous reduction of a knee dislocation, and others are dislocated knees that are reduced in the field before transport to a medical facility. The incidence of this type of reduced knee dislocation may be as high as 50% of all knee injuries classified as a dislocation.3,28,32 A study from our institution showed that the incidence of vascular injury in the reduced dislocations was equal to that of knees that presented dislocated (Fig. 26-1).32 In general, more recent studies have shown that the risk of arterial injury is approximately 7% to 12% with a diagnosis of a dislocated knee.26 Clinicians must be alert to the presence of reduced dislocations in order not to miss a limb-threatening arterial injury, as shown in Figure 26-1. A multiligament-injured knee with gross instability must be treated the same as a knee that presents dislocated.
Critical Points ASSESSMENT OF KNEE DISLOCATIONS
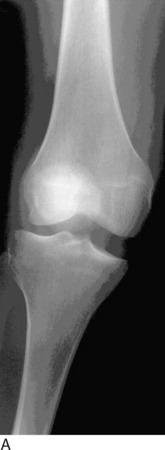
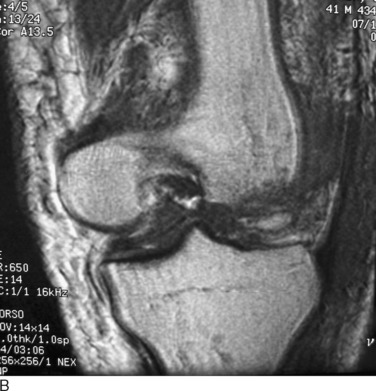
Although most knee dislocations involve tears of both cruciate ligaments (posterior cruciate ligament [PCL] and anterior cruciate ligament [ACL]), case reports of cruciate-intact knee dislocations do exist. A PCL-intact knee dislocation was first described in 1975.11 Several authors2,23 have reported on patients with a radiographically documented knee dislocation that, upon reduction or operative exploration, demonstrated a functioning PCL or ACL. Although some of these patients were noted to have suffered partial PCL tears, the presence of a functioning PCL provides increased stability and changes the management of these PCL-intact dislocations. In most PCL-intact knee dislocations, the tibia is perched anterior on the distal femur (Fig. 26-2). In addition to an ACL tear, there is often complete rupture of either the medial collateral ligament (MCL) or the posterolateral structures.
POSITION CLASSIFICATION SYSTEM
In 1963, Kennedy9 was the first to classify knee dislocations. He proposed a classification system based on the tibial position with respect to the femur. For example, an anterior knee dislocation implies that the tibia is positioned anterior to the femoral condyles. He identified five types of knee dislocation: anterior, posterior, lateral, medial, and rotatory. Rotatory dislocations were further subdivided into four groups: anteromedial, anterolateral, posteromedial, and posterolateral, with posterolateral being the most frequently described type of rotatory knee dislocation.5,6,14,15 This classification system has been widely utilized in the literature.*
The position classification system can help the physician plan a reduction maneuver for the dislocated knee. However, most knee dislocations can be easily reduced with longitudinal traction. The position classification system can also be useful to alert the clinician to the possibility of coexisting injuries. For example, several studies have shown a higher incidence of popliteal artery injury in anterior dislocations.5,8–10 However, vascular injury can occur with any position of knee dislocation; one must have a high index of suspicion for associated neurovascular injuries in any dislocated knee, regardless of position. Although knowing that an anterior dislocation carries an increased risk of vascular injury is helpful to the clinician, it does not give any information about what structures (ligamentous, neurovascular) have been injured and what treatment is required.
Critical Points POSITION CLASSIFICATION SYSTEM
The position classification system is based on the tibial position with respect to the femur.
Uses
One example of the utility of the position classification system is the rare but important posterolateral dislocation (Fig. 26-3). The mechanism of injury is an abduction force to a flexed knee coupled with internal rotation of the tibia. This force causes the medial femoral condyle to “buttonhole” through the medial capsule and the MCL invaginates into the knee joint. The trapped condyle and MCL prevent closed reduction. The clinical hallmark of the posterolateral dislocation and irreducibility by closed means is a transverse furrow seen on the medial aspect of the knee.6,15 Peroneal nerve palsy, theoretically resulting from a traction injury to the nerve over the lateral femoral condyle, is frequently associated with this type of dislocation. Skin necrosis secondary to pressure from the medially displaced femur has also been reported. For a posterolateral knee dislocation, the position classification system alerts the clinician to the injured structures and the means of treating the injury.