Atypical femoral fractures have attracted a great deal of attention and controversy in the osteoporosis community because of their association with prolonged bisphosphonate therapy. The purpose of this article is to review the epidemiologic evidence linking bisphosphonates to atypical fractures and to highlight the potential pathologic mechanisms involved in such fractures. A management plan is provided based on the available evidence.
Key points
- •
Bisphosphonate therapy is safe and effective for the management of osteoporosis when used for the duration measured in the original trials (<5 years).
- •
Atypical fractures constitute a rare subset of subtrochanteric and femoral shaft fractures.
- •
Careful identification and evaluation of these fractures demonstrated an association with prolonged bisphosphonate therapy (>5 years).
- •
Prolonged bisphosphonate therapy may contribute to atypical fractures by oversuppressing bone remodeling, leading to alterations in bone mineral and organic properties.
- •
Once atypical fractures are identified, bisphosphonates must be stopped and teriparatide therapy should be considered to enhance fracture healing.
Introduction
Bisphosphonates are a mainstay of therapy for osteoporosis. Several studies have documented their efficacy in preventing both vertebral and nonvertebral fractures. With its continued success in improving bone mineral density and reducing the incidence of some fractures associated with low bone mass, longer-term data regarding bisphosphonate use have become available. Although described before the Food and Drug Administration’s (FDA) approval and widespread clinical use of bisphosphonates, an uncommon variant of subtrochanteric and femoral shaft fractures thought to be associated with prolonged bisphosphonate therapy has captured the attention of the osteoporosis community. These so-called atypical femoral fractures occur after minimal trauma and have a distinct configuration and radiographic appearance compared with typical osteoporotic fractures. Although there is no evidence to suggest a cause-and-effect relationship, several studies have established an association between long-term bisphosphonate therapy and atypical femoral fractures. Yet, several other clinical studies have provided data to counter this association. This article highlights the reported incidence of atypical femoral fractures and their association with prolonged bisphosphonate therapy. The potential pathogenic mechanisms are discussed to identify gaps in our knowledge that warrant further research. A management approach is also provided to help guide orthopedic surgeons in the treatment of these fractures.
Introduction
Bisphosphonates are a mainstay of therapy for osteoporosis. Several studies have documented their efficacy in preventing both vertebral and nonvertebral fractures. With its continued success in improving bone mineral density and reducing the incidence of some fractures associated with low bone mass, longer-term data regarding bisphosphonate use have become available. Although described before the Food and Drug Administration’s (FDA) approval and widespread clinical use of bisphosphonates, an uncommon variant of subtrochanteric and femoral shaft fractures thought to be associated with prolonged bisphosphonate therapy has captured the attention of the osteoporosis community. These so-called atypical femoral fractures occur after minimal trauma and have a distinct configuration and radiographic appearance compared with typical osteoporotic fractures. Although there is no evidence to suggest a cause-and-effect relationship, several studies have established an association between long-term bisphosphonate therapy and atypical femoral fractures. Yet, several other clinical studies have provided data to counter this association. This article highlights the reported incidence of atypical femoral fractures and their association with prolonged bisphosphonate therapy. The potential pathogenic mechanisms are discussed to identify gaps in our knowledge that warrant further research. A management approach is also provided to help guide orthopedic surgeons in the treatment of these fractures.
The emergence of atypical femoral fractures
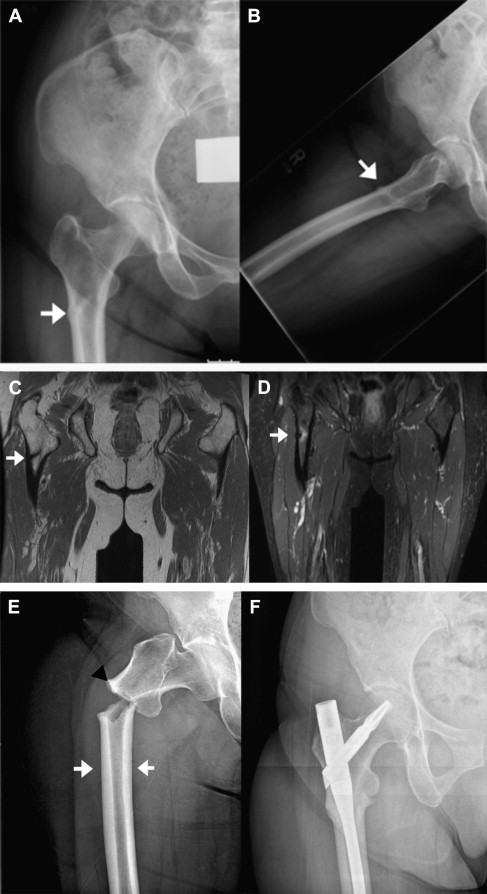
When the early reports raised concerns regarding the possible link between bisphosphonate therapy and atypical fractures, most case series described a low-energy subtrochanteric or femoral shaft fracture in patients on prolonged bisphosphonate therapy. On further histologic examination, these patients seemed to have severely suppressed bone turnover. Subsequent retrospective reports identified an atypical radiographic pattern as a simple transverse or oblique, noncomminuted fracture configuration with a medial spike, and cortical thickening ( Fig. 1 E ). This pattern was found to be particularly associated with prolonged bisphosphonate use. Furthermore, prodromal pain and a periosteal stress reaction preceding the complete fracture were reported; these findings were consistent with stress fracture propagation (see Fig. 1 A–D).
The American Society for Bone and Mineral Research (ASBMR) soon recognized the occurrence of atypical femoral fractures, often in the setting of bisphosphonate use, and sought to provide diagnostic criteria to facilitate the proper identification of such fractures. In 2010, a task force of multidisciplinary experts reviewed available clinical evidence and defined major and minor features of atypical fractures ( Table 1 ). According to this definition, for a fracture to be considered atypical, all major features must be present, whereas minor features are not required to make the diagnosis. However, this definition remains subject to change and revision as more data become available.
| Major features | Location: anywhere distal to lesser trochanter down to the supracondylar flare Configuration: transverse or short oblique No trauma or low-energy trauma Noncomminuted Medial spike in complete fracture Incomplete fracture only in the lateral cortex |
| Minor features | Localized periosteal reaction in the lateral cortex beaking Generalized cortical thickening Prodromal thigh pain or discomfort Bilaterality Delayed healing Bisphosphonate or glucocorticoid use |
Epidemiology: reasons for controversy
Atypical femoral fractures and their association with bisphosphonate therapy continue to be a controversial subject. Low level of evidence, controversial defining features, the use of diagnostic codes rather than radiographic adjudication, inadequate power, and short duration of the original trials are some of the limitations that impede accurate reporting and identification of a true association between bisphosphonate therapy and atypical fractures. In this section of the article, the authors discuss the epidemiologic evidence from larger cohort studies and clinical trials in light of these limitations.
Low Level of Evidence
The available evidence regarding the incidence of atypical femoral fractures and their association with prolonged bisphosphonate therapy comes from several case-control studies and several large retrospective cohort studies using national registries. Therefore, the available level of evidence of this particular type of fracture is largely limited to levels III and IV. Although prospective studies are required to properly answer the question of incidence and association, the rarity of these fractures calls for a large multicenter effort to achieve sufficient statistical power.
A Debatable Definition: What is Major and What is Minor?
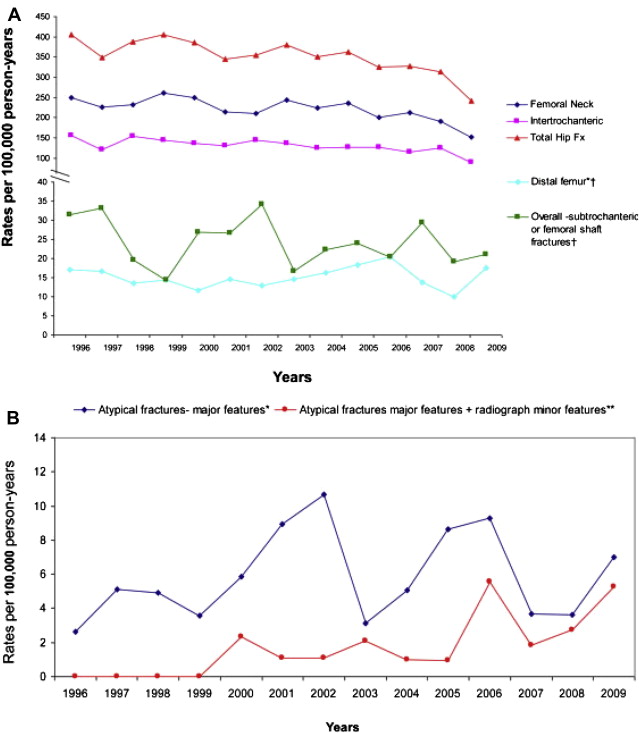
Although the definition set forth by the ASBMR task force does not require minor features for the diagnosis of atypical femoral fractures, this definition may have to be revised in light of recent work by Feldstein and colleagues. This study reviewed both electronic medical records and radiographs of women older than 50 years and men older than 65 years between 1996 and 2009 at Kaiser Permanente Northwest to describe incidence rates and characteristics of atypical fractures. By using the ASBMR major and minor radiographic criteria, they subdivided atypical femoral fractures into those with major features only and those with both major and minor features (localized periosteal reaction of the lateral cortex [beaking] and generalized cortical thickness). According to this definition, the incidence of typical femoral fractures and atypical fractures with major features only remained flat over the study period (cumulative incidence: 18.2 per 100 000 person-years and 5.9 per 100 000 person-years, respectively), whereas the proportion of atypical fractures with both major and minor features increased over time ( Fig. 2 ). Moreover, patients with atypical fractures with only major features had a lower frequency of prolonged bisphosphonate use (2%) and prodromal pain (0%) compared with those with both major and minor features (29% and 27%, respectively). This study serves to create a more precise case definition of atypical femoral fractures and suggests that future research should evaluate fractures with minor features (localized periosteal reaction and cortical thickness) separately. Making this distinction not only affects incidence rates and association with bisphosphonate therapy but also advances our understanding of these fractures and has pathophysiological implications.
According to the ASBMR case definition, the minor criteria consist of either a localized periosteal reaction on the lateral cortex (beaking) or a generalized increase in cortical thickness of the diaphysis (see Fig. 1 ). Because a higher proportion of patients with minor features had a history of bisphosphonate use, the study by Feldstein and colleagues revisits the association between bisphosphonate therapy and cortical thickening. However, it is important to make the distinction between the localized cortical thickening caused by the periosteal reaction and generalized cortical thickening. In a retrospective radiological study of complete subtrochanteric and femoral shaft fractures, cortical stress reaction (localized cortical thickness or beaking) had the highest odds ratio for predicting prior bisphosphonate use among other atypical features. On the other hand, generalized cortical thickening, as assessed from the subtrochanteric region using dual-energy x-ray absorptiometry, did not seem to be common in long-term bisphosphonate users. Although it remains to be determined whether generalized cortical thickening serves as a marker for propensity to sustain atypical fractures, a recent large population-based cohort of bisphosphonate-naïve women showed that subtrochanteric cortical thickening does not increase the risk of subtrochanteric, femoral shaft, or typical hip fractures. Collectively, these findings emphasize our incomplete understanding of these features and the need for a revised definition of atypical femoral fractures.
The Use of Diagnostic Codes in Large National Registries Without Radiographic Adjudication
Large health databases provide advantages in power, real-world validity, and longer follow-up durations over clinical trials for assessing the harms and benefits of preventive medications. However, with regard to atypical femoral fractures, large health databases are not without limitations. Registers use diagnostic codes to capture patients with subtrochanteric and femoral shaft fractures. It is important to realize that not every subtrochanteric fracture is an atypical fracture. Typical subtrochanteric and femoral shaft fractures usually occur with high-energy trauma, are comminuted, and have a spiral configuration as opposed to the atypical fractures defined by the ASBMR. As of yet, no diagnostic code has been assigned to atypical fractures; therefore, registers using diagnostic codes cannot distinguish between an atypical subtrochanteric fracture and a typical, osteoporotic subtrochanteric fracture. Previous studies that examined individual radiographs of patients with subtrochanteric or femoral shaft fractures reported that 2.3% to 34.0% of atypical fractures were miscoded by International Classification of Diseases codes. Furthermore, information on trauma mechanism (low-energy trauma being one of the major features of atypical fractures) may be missing or uncertain. Therefore, studies that individually examined radiographs of patients with subtrochanteric and femoral shaft fractures are more valid for drawing conclusions regarding trends, risk factors, and associations.
With careful radiographic identification in large databases, atypical fractures seem to be uncommon ( Table 2 ). In the Kaiser Permanente Northwest study, as described earlier, the rate of atypical femoral fractures with major and minor criteria seem to have increased from no events in the period between 1996 and 1999 to 5 per 100 0000 patient-years in 2009, along with a decline in classical hip fractures (see Fig. 2 ). In another study using the National Swedish Patients Register, probably the largest database of patients who sustained femoral fractures, Schilcher and colleagues performed a nationwide cohort analysis in 12 777 women aged 55 years and older who sustained a femoral fracture in Sweden in 2008. They reviewed radiographs of 1234 subtrochanteric fractures of which 59 were identified as atypical, with an overall rate of 4 per 100 000 person-years and 55 per 100 000 among bisphosphonate users. Giusti and colleagues also reviewed the radiographs of 906 consecutive patients admitted into a single center with femoral fractures and showed a low prevalence of atypical fractures (1.1% of all femoral fractures and 10.4% of all subtrochanteric or femoral shaft fractures).
| Study | Data Source | Number of Fractures | Prevalence of Atypical Fractures |
|---|---|---|---|
| Feldstein et al, 2012 | Kaiser Permanente Northwest | 5034 Femoral fractures 122 ST/FS 75 Atypical | 5.9 per 100 000 person-years |
| Schilcher et al, 2011 | National Swedish Patient Register | 12 777 Femoral fractures 263 ST/FS 59 Atypical | 4 per 100 000 person-years |
| Giusti et al, 2011 | Single center in the Netherlands | 906 Femoral fractures 53 ST/FS 10 Atypical | 1.1% of all femoral fractures and 10.4% of ST/FS fractures |
In large databases without radiographic adjudication, it remains possible to examine whether there is a shift from classical hip fractures to other femur fractures since the introduction of bisphosphonates in 1996. Wang and Bhattacharyya analyzed national trends in hip and femur fractures between 1996 and 2007 by retrospectively using the National Inpatient Sample, Medical Expenditure Panel Surgery, and National Hospital Discharge Survey (NHDS) databases. The results showed that during this period, rates for typical fractures decreased by 32% in women and 20% in men, whereas the overall trends in subtrochanteric fractures remained unchanged in men and increased by 20% in women. Another study by Nieves and colleagues using the NHDS also analyzed the trends for distinct subtypes of femoral fractures over a similar time period (1996–2006) and found a significant decline in incidence rates of hip fractures but not in subtrochanteric fractures, which remained stable at 20 per 100 000 person-years in women. Collectively, studies with and without radiograph adjudication clearly show that atypical femoral fractures constitute a small subset of subtrochanteric and femoral shaft fractures, which in turn account for only 3% to 5% of all femoral fractures.
Several cohort and matched case-control studies were conducted to identify the risk of developing atypical femoral fractures in bisphosphonate users ( Table 3 ). Again, most of these studies did not have radiograph adjudication to identify atypical fractures as such. Studies relying on large databases without reviewing radiographs have largely failed to demonstrate an increased risk of atypical fractures in bisphosphonate users. Three studies used the Danish National Hospital Discharge database. The first study did not find a greater frequency of these fractures in bisphosphonate users ; the second one from the same group did demonstrate an increased risk, but not a dose-response relationship ; and the third study concluded that the risk of fracture was already present before the drugs were started and there was no dose-response relationship present. However, one large Canadian, population-based, nested case-control study used data from the Ontario Public Drug Program database and showed that the risk of atypical fractures only increased in those who received bisphosphonates for longer than 5 years. As mentioned earlier, the biggest study to specifically look at the risk of atypical fractures using radiographs was by Schilcher and colleagues ; it demonstrated an increased relative risk (RR) in the cohort analysis (RR 47.3; 95% confidence interval [CI], 25.6–87.3) and an increased odds ratio (OR) of 33.3 (95% CI, 14.3–77.8). Even more interesting, the investigators were able to demonstrate a 70% reduction in the RR per year after drug withdrawal (OR 0.28; 95% CI, 0.21–0.38). The fact that radiographs were individually examined in this study grants more validity to the results over other registry-based studies.
| Study | Data Source | Risk of ST/FS in Bisphosphonate Users | Conclusions |
|---|---|---|---|
| Abrahamsen et al, 2009 | Danish National Hospital Discharge database | HR = 1.46 (95% CI, 0.91–2.35) | ST/FS fractures share the epidemiology and treatment response of classical hip fractures and are best classified as osteoporotic fractures. |
| Abrahamsen et al, 2010 | HR = 2.66 (95% CI, 2.35–3.02) |
| |
| Vestergaard et al, 2011 | HR = 2.41 (95% CI, 1.78–3.27) |
| |
| Black et al, 2010 | Post hoc analysis of 3 randomized clinical trials |
| There was no significant increase in risk, but the study was underpowered for a definitive diagnosis. |
| Kim et al, 2011 | Medicare beneficiaries in Pennsylvania and New Jersey | HR = 1.03 (95% CI, 0.70–1.52) compared with raloxifene/calcitonin |
|
| Park-Wyllie et al, 2011 | Ontario Public Drug Program database | OR = 2.74 (95% CI, 1.25–6.05) >5 y of BP therapy | Treatment with BP for more than 5-y increased the risk of ST/FS fracture. |
| Schilcher et al, 2011 | National Swedish Patient Register | OR = 33.3 (95% CI, 14.3–77.8) for atypical fractures |
|
The Inherent Limitations of the Original Trials
Randomized clinical trials are efficacy trials by design and are not powered to look at adverse effects, especially rare adverse effects, such as atypical fractures. In addition to having too few participants, follow-up times are often short; and in some populations, comorbidities and additional drug interactions may not be adequately represented in earlier phases of clinical testing. The true safety profile of any medication is really only understood after the medication has been on the market for a sufficiently long period of time and has been used by a large number of patients. This point is especially true in the case of atypical fractures because the pathogenesis involves time-dependent processes (see pathogenesis section later) rather than a dose-dependent adverse effect. Therefore, it was certainly difficult to anticipate a potential long-term complication when most phase trials were conducted for shorter durations.
Black and colleagues performed secondary analyses using the results of 3 large randomized controlled trials: the Fracture Intervention Trial (FIT), the FIT Long-Term Extension (FLEX) trial, and the Health Outcomes and Reduced Incidence with Zoledronic Acid Once Yearly Pivotal Fracture Trial (HORIZON-PFT). The investigators showed that the relative hazard was not significant; but the 95% confidence intervals were wide, and original radiographs were generally unavailable at the time of the analysis. Furthermore, the 2 placebo-controlled trials (FIT and HORIZON-PFT) lasted only 3.0 to 4.5 years and, thus, could not assess whether the risk of fracture increased with treatment duration. Even in the FLEX trial, which included women who were treated up to 10 years, only 186 patients received more than 8 years of treatment, making the study strongly underpowered.
The lack of long-term exposure is a major problem when examining long-term outcomes, such as atypical fractures. Studies with access to a substantial number of femur radiographs from fracture patients have been limited by short-term drug history data. For example, although the study by Schilcher and colleagues from Sweden used radiograph adjudication, it was constrained by having access to less than 3 years of medication history. What makes this more troublesome is that patients on bisphosphonates often have substantial treatment gaps and varying compliance rates, so that what would seem to be a bisphosphonate-naïve patient could be in fact a patient who had used bisphosphonate for many years but done so at a time when prescriptions were not yet captured.
It is clear that atypical femoral fractures are not common. An association with bisphosphonate therapy seems to exist based on studies that identified those fractures radiographically. Large observation studies had to rely on diagnosis codes, resulting in incidence rates that are too high and odds ratios that are too low because they include fractures that may not be atypical. Yet the fact that many patients with skeletal malignancies receiving massive doses of bisphosphonate never develop these fractures, and that some patients with atypical fractures have not used bisphosphonates, adds to the controversy. Longer-term drug exposure data linked to radiographs are required to elucidate an accurate association and optimal duration of bisphosphonate therapy.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





