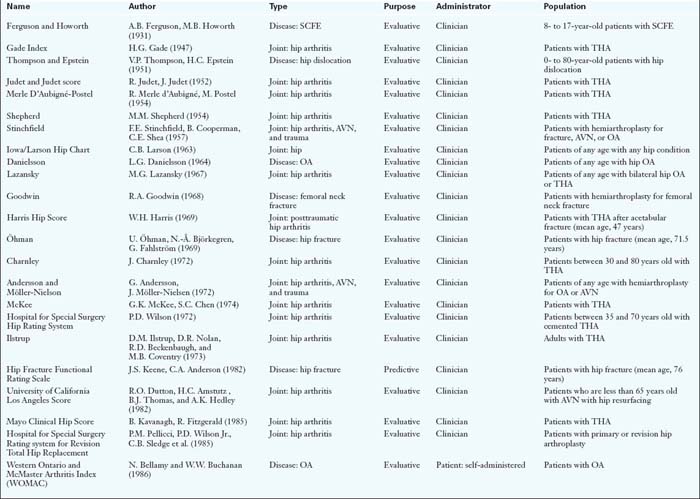
CHAPTER 8 Assessing Outcomes After Hip Surgery
Classification (Table 8-1)
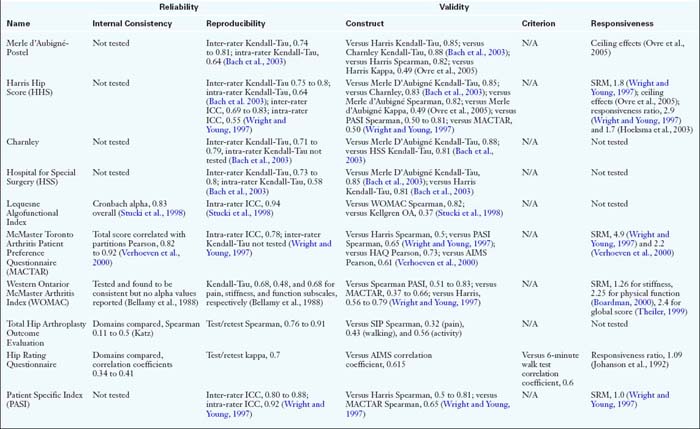
Psychometrics (Table 8-2)
Table 8-2 shows the evaluative tools that have been tested for reliability, validity, and responsiveness. Of the clinician-based tools, only the Harris Hip Score and Lequesne Index have been tested for reliability and shown to have internal consistency. Ten of the patient-based measures have demonstrated internal consistency. Two others—the Total Hip Arthroplasty Outcome Evaluation and the Hip Rating Questionnaire—have also been tested for internal consistency, but the results were poor. The majority of the questionnaires have demonstrated adequate reproducibility or test/retest reliability. All tools in Table 8-2 were presumed to have both face and content validity because patients and clinicians were involved in their creation or because they have been used by other surgeons in clinical practice or research. All have been tested for construct validity against other questionnaires. Only three tools have been tested for criterion validity: the Hip Rating Questionnaire was compared with the 6-minute walk test; the MFA was compared with stair climbing and walking speed; and the Lower-Extremity Measure was compared with the timed up-and-go test.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree