Chapter 64 Aloe vera (Cape Aloe)
Aloe vera (family: Liliaceous)
 General Description
General Description
More than 300 species of aloe plants exist, but the most popular medicinal variety is currently Aloe vera. The nomenclature of A. vera is somewhat confusing, because the plant has been known by various names, most notably A. barbadensis and A. vulgari. The geographic origination of the plant is unclear. Historical records indicate that it may have originated from Egypt or the Middle East. Aloe has been introduced and naturalized throughout most of the tropics and warmer regions of the world, including the Caribbean, southern United States, Mexico, Latin America, the Middle East, India, and Asia.1
The leaf is composed of three distinct layers: an outer layer of tough tissue; a corrugated lining just beneath the outer layer; and the major portion of the leaf, the inner layer consisting of parenchymal cells containing large vacuoles of a semisolid, gelatinous, transparent gel. The bitter latex of the corrugated layer protects the plants from predators. Should an animal bite the leaf, the sap causes irritation. The dried latex (juice) derived from the corrugated layer is the source of the laxative properties of aloe. The parenchymal tissue or gel is the portion of the aloe used in other applications.2
Aloe vera Terminology
• A. vera gel—naturally occurring, undiluted parenchymal tissue obtained from the decorticated leaves of A. vera
• A. vera concentrate—A. vera gel from which the water has been removed
• A. vera juice—an ingestible product containing a minimum of 50% A. vera gel
• A. vera latex—the bitter yellow liquid derived from the pericyclic tubules of the rind of A. vera, the primary constituent of which is aloin.
 Chemical Composition
Chemical Composition
The main feature of all aloe plant portions is a high water content. Aloe gel contains 99% water, whereas the skin and fillet fractions contain 90% and 98% water, respectively. A. vera contains numerous compounds possessing biological activity. Although many botanical medicines have substantial geographic variation in content, commercial aloe is quite consistent. One study found that the composition of the major compounds was remarkably invariable, with aloeresin A, aloesin, and aloin (both epimers A and B) contributing between 70% and 97% of total dry weight in a ratio of approximately 4:3:2, respectively. Minor compounds were less evenly distributed, with aloinoside A and aloinoside B found in higher concentrations in Western countries. The aloin content of the exudate varied, but there were no distinct geographic discontinuities.3
Anthraquinones
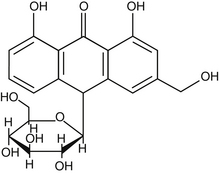
In 1851, the cathartic action of aloe was discovered to be due to aloin, a lemon yellow powder formed from drying of the bitter latex (Figure 64-1). From this material several anthracenes have been isolated, the major anthraquinone being barbaloin. Barbaloin and aloin are often referred to synonymously. Although aloe contains other anthraquinone derivatives, including the anthracene known as aloe-emodin, barbaloin is considered the most potent cathartic. As a whole, the anthraquinone compounds are water-soluble glycosides easily separated from the water-insoluble resinous material.1–5
Saccharides
Recent research on A. vera has focused on the glycoprotein, mucopolysaccharide, and polysaccharide constituents. Aloe contains the polysaccharides galactose, xylose, arabinose, and acetylated mannose. The latter, similar to guar and locust bean, has received considerable clinical research attention as an antiviral and immunopotentiating agent, especially in the treatment of acquired immunodeficiency syndrome (AIDS). Acemannan is a water-soluble, long-chain polydispersoid β(1,4)-linked mannan polymer interspersed with O-acetyl groups found mainly in aloe gel.6
Prostanoids
Several prostanoid compounds have been discovered in A. vera extracts.7 The conversion of essential fatty acids to prostanoids by the enzyme cyclooxygenase in a plant such as A. vera is rare. The major unsaturated fatty acid in the plant is γ-linolenic acid (C18:3), which can be converted to icosatrienoic acid, the precursor to prostaglandins of the 1 series. The 1 series prostaglandins are known to exert more favorable effects on inflammation, allergy, platelet aggregation, and wound healing. The presence of γ-linoleic acid or prostaglandins, or both, in a stable medium, along with inhibitors of thromboxane synthesis, may be another important chemical characteristic of aloe responsible for its antiinflammatory and wound-healing effects.
Superoxide Dismutase
Extracts from the parenchymatous leaf gel and the rind of aloe (A. barbadensis Miller) have been shown to contain seven electrophoretically identifiable superoxide dismutases (SODs). Two of these seven are mangano SODs, whereas the other five activities are cupro-zinc SODs.8
Other Constituents
Other biological active compounds found in A. vera include the following:
Box 64-1 provides a partial listing of the remarkably diverse range of compounds isolated from A. vera.2–5
BOX 64-1 Chemical Composition of Aloe Vera
Saccharides: Cellulose, glucose, mannose, L-rhamnose, aldopentose
Prostanoids: Gamma-linolenic acid
Enzymes: Oxidase, amylase, catalase, lipase, alkaline phosphatase
Amino acids: Lysine, threonine, valine, methionine, leucine, isoleucine, phenylalanine
Vitamins: Vitamins B1, B2, B6, C, and E; folic acid; choline; β-carotene
Minerals: Calcium, sodium, manganese, magnesium, zinc, copper, chromium
Data from Shelton RM. Int J Dermatol 1991;30:679-683.
 History and Folk Use
History and Folk Use
A. vera has a storied history of use. Mesopotamian clay tablets dated 1750 BC indicate that A. vera was used for medicinal purposes. Egyptian records from 550 BC also mentioned aloe for infections of the skin. The ancient Greeks were also aware of aloe’s medicinal effects, since both Pliny (23-79 AD) and Dioscorides (first century AD) wrote of aloe’s ability to treat wounds and heal infections of the skin. A. vera is still widely used in many traditional systems of medicine. In India, for example, in addition to external applications, aloe (whole leaves, the exudate, and the fresh gel) is used as a cathartic, stomachic, and anthelmintic. A. vera has been adopted into their materia medicas by many cultures of the world.1
In the United States, the history of aloe can be traced as far back as the United States Pharmacopoeia of 1820, where a number of aloe preparations were described. Most of these preparations were designed to take advantage of aloe’s laxative effects. By the early 1900s, more than 27 different aloe preparations were in popular use. In 1920, aloe began being cultivated for pharmaceutic use.4
A major development in the modern use of aloe occurred in 1935, when a group of physicians successfully used the fresh juice to treat a patient with facial burns due to radiographs.9 The relief offered by aloe in the topical treatment of burns, minor irritations, skin ulcers, and other skin disorders is a major reason why companies supplying dermatologic and cosmetic products have incorporated aloe into many of their formulations.
Although more and more of aloe’s medicinal effects are being confirmed, it is still predominantly administered without direct medical supervision. Therefore, the history and folk use of aloe are continuing to evolve.
 Pharmacology
Pharmacology
Gastrointestinal Effects
Laxative Effects
Although physicians have prescribed the whole aloe leaf as a cathartic for more than 2000 years, it was not until 1851 that the active principle aloin was discovered.1 In small doses, aloin acts as a tonic to the digestive system, giving tone to the intestinal muscle. At higher doses, it becomes a strong purgative. Its actions are most obvious on the large intestine, where it increases colonic secretions and peristaltic contractions. In combination with strychnine and belladonna, aloin became one of the most popular laxatives for chronic constipation for many years. Because aloin often causes painful contractions, other anthraquinone laxatives like cascara and senna are now much more popular.10,11
A substantial amount of research activity continues in an effort to understand the laxative effects of aloe. Research using the rat large intestine showed that the increase in water content of the large intestine induced by barbaloin preceded the stimulation of peristalsis, attended by diarrhea. Therefore, it was suggested that the increase in water content was a more important factor than the stimulation of peristalsis in the diarrhea induced by barbaloin.12 Further studies by the same researchers suggested that aloe-emodin-9-anthrone (AE-anthrone) produced from barbaloin in the rat large intestine might be the actual chemical mediator of this effect. AE-anthrone not only caused an increase in the intestinal water content but also stimulated mucus secretion.13
Bowel Detoxification
In 1985, Bland14 reported the effect of orally consumed A. vera juice on urinary indican, gastrointestinal pH, stool culture, and stool specific gravity in a semi-controlled study of 10 (5 men and 5 women) healthy human subjects.14 Urinary indican (see Chapter 30) is used as an indicator of the degree to which either dietary protein is malabsorbed or intestinal bacteria are engaged in putrefactive processes. After a full week of drinking 6 oz. of A. vera juice three times daily, urinary indican levels decreased one full unit. This suggests that regular A. vera juice consumption can lead to improved protein digestion and assimilation or reduced bacterial putrefaction, or both.
 Immune-Enhancing and Antimicrobial Activity
Immune-Enhancing and Antimicrobial Activity
Immunologic Effects
Antibacterial and Antifungal Activity
Aloe demonstrated activity against many common bacteria and fungi in several studies. In a detailed review of these studies, the researchers assayed the antimicrobial properties of an A. vera extract and reviewed the work of others.15–17 Both mean inhibitory and mean lethal concentrations were determined and compared with silver sulfadiazine (SSD), a potent antiseptic used in the treatment of extensive burns. As shown in Table 64-1,19 the antimicrobial effects of A. vera compare quite favorably with those of SSD. A 60% A. vera extract was found to be bactericidal against Pseudomonas aeruginosa, Klebsiella pneumoniae, Serratia marcescens, Citrobacter spp., Enterobacter cloacae, Streptococcus pyogenes, and S. agalactiae. Concentrations of 70% aloe were bactericidal for Staphylococcus aureus, 80% for E. coli, and 90% for S. faecalis and Candida albicans. Organisms inhibited in other studies include Mycobacterium tuberculosis, Trichophyton spp., and Bacillus subtilis.2,4,5 The antimicrobial activity against common skin pathogens of A. vera gel in a cream base was shown to be slightly better than SSD in agar well diffusion studies.19
TABLE 64-1 Antimicrobial Effects of Aloe Vera Extract in Cream Base Compared with Silver Sulfadiazine in Agar (AgSD) Well (6-mm) Diffusion
| ORGANISM | ALOE VERA | AgSD |
|---|---|---|
| Gram-negative | ||
| Escherichia coli | 16 | 12 |
| Enterobacter cloacae | 14 | 12 |
| Klebsiella pneumoniae | 14 | 6 |
| Pseudomonas aeruginosa | 17 | 12 |
| Gram-positive | ||
| Staphylococcus aureus | 18 | 12 |
| Streptococcus pyogenes | 16 | 12 |
| Streptococcus agalactiae | 16 | 12 |
| Streptococcus faecalis | 6 | 11 |
| Bacillus subtilis | 19 | 14 |
Inhibition zones measured in millimeters.
Data from Robson MC, Heggers JP, Hagstrom WJ. J Burn Care Rehabil 1982;3:157-162.
Antiviral Effects
Acemannan (acetylated mannose) in injectable form has been approved for veterinary use in fibrosarcomas and feline leukemia. Its action in feline leukemia is quite impressive. Feline leukemia, like AIDS, is caused by a retrovirus (feline leukemia virus). The virus is so lethal that once cats develop clinical symptoms, they are usually euthanized. Typically more than 70% of cats die within 8 weeks of the onset of clinical signs. In a study of 44 cats with clinically confirmed feline leukemia, acemannan was injected (2 mg/kg) weekly for 6 weeks and the cats were reexamined 6 weeks after termination of treatment.18 At the end of the 12-week study, 71% of the cats were alive and in good health.
Acemannan demonstrated significant antiviral activity against several viruses, including feline AIDS, human immunodeficiency virus type 1 (HIV-1), influenza virus, and measles virus.20–22
Immune Enhancement
Acemannan is a potent immunostimulant.18,23–25 Among the effects noted for acemannan are the enhancement of macrophage release of interleukin (IL)-1-α, cytokines, tumor necrosis factor, and nitric oxide release, as well as phagocytosis and nonspecific cytotoxicity. Acemannan also enhances T-cell function and interferon production, although these actions may also be due to enhanced macrophage function. Macrophage production of cytokines IL-6 and tumor necrosis factor-α were dependent on the dose of acemannan provided. These effects can be substantial. For example, in one study, acemannan was shown to enhance the macrophage respiratory burst (two-fold increase above the media controls), phagocytosis (45% compared with 25% in controls), and killing of C. albicans (38% killing of C. albicans compared with 0% to 5% killing in controls).26
Hematopoietic Effects
Several complex carbohydrates have been found to significantly stimulate hematopoiesis. CARN 750, a polydispersed β-(1,4)-linked acetylated mannan isolated from the A. vera plant, has been shown to have hemato-augmenting properties. Subcutaneous injections of 1 mg/mouse of CARN 750 optimally increased hematopoietic progenitors, measured as IL-3–supported colony forming units, culture (CFU-C) and high proliferative potential colony forming cell (HPP-CFC) assays in the spleen. Providing 2 mg/animal of CARN 750 optimally increased bone marrow cellularity, frequency, and absolute number of HPP-CFCs and CFU-Cs. The hematopoietic activity of CARN 750 increased with the frequency of administration. The greatest increase in activity occurred in mice myelosuppressed with radiation.27
Antiinflammatory Activity
A. vera has been shown to exert a number of antiinflammatory actions, including blocking of the generation of inflammatory mediators like thromboxanes and bradykinin, reducing neutrophil infiltration during inflammation and reducing edema.* Several compounds in aloe are responsible for these actions. The most important are glycoproteins, which inhibit and actually break down bradykinin, a major mediator of pain and inflammation; various anthraquinones; and salicylates. These antiinflammatory substances may be of significance in both topical and oral applications.
One comprehensive study evaluated the effects of aqueous, chloroform, and ethanol extracts of A. vera gel on carrageenan-induced edema in the rat paw and neutrophil migration into the peritoneal cavity stimulated by carrageenan. The capacity of the aqueous extract to inhibit cyclooxygenase activity was also evaluated. The aqueous and chloroform extracts decreased the edema induced in the hind paw and the number of neutrophils migrating into the peritoneal cavity, whereas the ethanol extract only decreased the number of neutrophils. The aqueous extract was also found to inhibit prostaglandin E2 production from arachidonic acid, demonstrating an inhibitory action on cyclooxygenase. The aqueous extract contained anthraglycosides, reductor sugars, and cardiotonic glycosides, whereas the ethanol extract contained saponins, carbohydrates, naphthoquinone, sterols, triterpenoids, and anthraquinones. The chloroform extract contained sterols and anthraquinones.32
Another useful aspect of aloe is its ability to inhibit lipid peroxidation and scavenge free radicals. One study measured the activity of seven anthraquinones and four anthrones against nonenzymatic and enzymatic lipid peroxidation in vitro and their ability to scavenge free radicals. Using rat hepatocytes exposed to strong oxidizing agents, dithranol and anthrone provided the strongest inhibition of nonenzymatic peroxidation. Rhein anthrone and aloe-emodin showed the highest inhibitory activity against peroxidation of linoleic acid catalyzed by lipoxygenase. Anthrone, dithranol, and rhein anthrone were the most effective free radical scavengers.33
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree