Fig. 10.1
Female sport participation increased from 7 % in 1972 to 41 % in 2009 as a result of Title IX
However, many athletes remained undiagnosed according to the 1992 definition of the Triad because they did not meet the classic Triad criteria. For example, many young female athletes did not fit the classic “eating disorder” definition but had amenorrhea. By the time they were diagnosed with a stress fracture, treatment options for the Triad became more limited because females can only accrue BMD up until 20–25 years of age. After this time frame, athletes can only try to maintain BMD.
In 2007, the definition transitioned into a spectrum disorder of low energy availability, irregular menstruation, and decreased BMD. The updated definition can also be described as an athlete falling under the “umbrella” of the spectrum of the Triad so that not all three components need to be present for the athlete to suffer from some of the long-term, negative consequences (Fig. 10.2). For example, an athlete may present with only one component of the Triad, such as low energy availability, which makes early interventions possible to prevent progression to the second (irregular menstruation) and third (decreased BMD) components of the Triad.
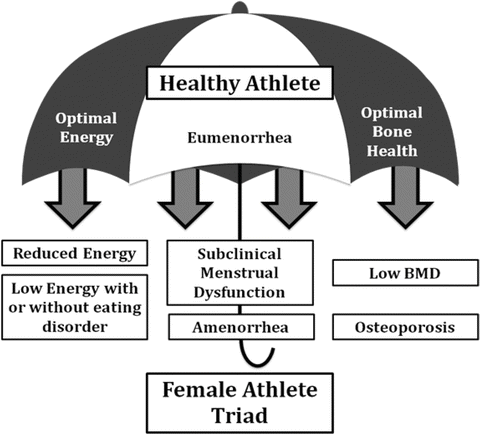

Fig. 10.2
The Female Athlete Triad is now defined as a spectrum disorder, so many female athletes may fit under the umbrella of the Triad without having all three features of the Triad concomitantly
The true Triad prevalence is unknown for a variety of reasons, including patient population heterogeneity, lack of prospective studies, and lack of studies evaluating all three components of the Triad under the new definition formulated in 2007. The literature reports that disordered eating can affect up to 70 % of athletes compared to 10 % in the general population, that secondary amenorrhea has a 65–69 % prevalence in female ballet dancers, and that there is a 2–4× higher prevalence of low BMD among athletes compared to the general population when disordered eating and amenorrhea is present [2–4, 6, 9, 10, 12]. In contrast, studies done evaluating the Triad under the criteria prior to 2007 report a Triad prevalence of 1.2 % in high school athletes, 2.7 % in collegiate athletes, and 4.3 % in elite athletes [13–15]. Such contrasting numbers suggest that the prevalence of the Triad as defined as a spectrum disorder is likely much higher than previously reported in the literature.
Bone Formation
Epidemiology
BMD Accrual, Sex Differences, and Affected Athletes
Ninety percent of BMD is accrued by adolescence and a net peak in bone mass usually occurs around 26 years of age [16]. Normal females gain approximately 2 % of bone mass per year while amenorrheic females lose 2 % per year. Once females reach their late twenties, they can no longer increase their bone mass—only lose or maintain what they have.
In general, athletes have been found to have a 5–15 % greater BMD level compared to the general population [17]. However, athletes with disordered eating and amenorrhea have shown a 2–4 times higher prevalence of low BMD compared to the general population [6, 12].
Males tend to have higher peak BMD after puberty compared to females [18]. Further, 40 % of women and 25 % of men aged 50 years and older will sustain an osteoporotic fracture. While both sexes will lose BMD over time, females undergo menopause that results in an accelerated bone loss [19].
Among females there are specific sport types that increase a female athlete’s risk of developing the Female Athlete Triad and subsequent reduced BMD. Aesthetic/weight-dependent sports, such as figure skating, gymnastics, endurance running, lightweight rowing, cycling, and dance leave athletes at a greater risk since there is often incredible pressure from coaches and peers to maintain a certain weight and physique.
Predispositions to Reduced BMD
There are also certain medical conditions and therapies associated with reduced BMD, including metabolic disorders, such as estrogen deficiency, excess parathyroid and thyroid hormone, osteogenesis imperfecta, long-term glucocorticoid or anticonvulsant use, smoking, vitamin D deficiency, rheumatoid arthritis, and conditions that prevent nutrient uptake, such as Celiac disease (sprue) or Crohn’s disease (Table 10.1). Identification of secondary causes of low bone mass is important to potentially reverse or treat the underlying cause of low bone density and osteoporosis.
Table 10.1
There are many medical conditions outside of the Female Athlete Triad that leave patients at a greater risk of reduced BMD. Some examples are highlighted below
Conditions associated with increased risk of low BMD |
|---|
• Hormone abnormalities (estrogen deficiency, excess parathyroid and thyroid) |
• Osteogenesis imperfecta |
• Long-term glucocorticoid use |
• Long-term anticonvulsant use |
• Smoking |
• Vitamin D deficiency |
• Conditions that require prolonged limb immobilization |
• Conditions that prevent nutrient uptake (e.g., Celiac disease and Crohn’s disease) |
Stress Fractures from an Orthopaedic Surgeon’s Perspective
Stress fractures are the result of bone not being able to handle the stress introduced to it. This is due to both intrinsic and extrinsic factors that result in microdamage to the bones structure and integrity. Intrinsic factors include bone structure and density, vascularity, metabolism, menstrual cycle, anatomic alignment, endurance, and initial fitness level. Extrinsic factors include nutrition, exercise surface, shoe wear, and changes in training regimen such as increasing the amount of time or intensity of the exercise.
If bone is weak prior to seeing these “stresses,” it is at higher risk of having a stress injury. Bone is a living tissue and responds to stress if it is introduced slowly. When bone undergoes too much impact too quickly, it will result in a stress reaction and if the impact persists, the end result will be a stress fracture. Certain stress fractures may be more resistant to healing or more likely to require surgical intervention. These include—navicular, anterior tibia and fifth metatarsal fractures [20].
A detailed patient history can often lead to the diagnosis of a stress fracture. Pain with activity over a few weeks getting progressively worse until unable to continue with activity is a common scenario. Clinical exam demonstrates tenderness over the area of the stress fracture. Radiographs may demonstrate the injury, but an MRI is most sensitive and specific to understanding the extent of bone and soft tissue injury. Once a female athlete presents with a stress fracture—it is paramount that the clinician considers the Female Athlete Triad as a cause.
Most stress fractures will heal with symptomatic treatment—rest the affected bone and allow it to heal. The location of the fracture and the extent of injury dictate the treatment. Most stress fractures will take 3 months to completely heal. Certain fractures and situations in competitive athletes may warrant more aggressive surgical intervention. Other modalities to speed the healing process are available but none have demonstrated any clear advantages—future research is promising. These include—bisphosphonates, teriparatide, pulsed ultrasound, and extracorporeal shock wave therapy. The most important thing to consider when seeing an athlete with a stress fracture is making sure there is not an underlying cause or any other components of the Female Athlete Triad.
Awareness of the Female Athlete Triad
Prior Studies
The first Female Athlete Triad awareness study was published in 2006, which assessed the awareness of athletic trainers, coaches, medical students, physical therapists, and physicians concerning this disorder [21]. According to surveys of 240 health care professionals, only 48 % of physicians and 32 % of medical students were able to identify the Female Athlete Triad and only 9 % of physicians felt comfortable treating a patient with this disorder; only 36 % of pediatricians could identify the Triad components and 4 % were comfortable treating the disorder. This study was limited by sample size and did not assess knowledge of the new Female Athlete Triad definition [22].
Another study subsequently examined the awareness of coaches about the Female Athlete Triad [22]. While about 43 % of coaches properly identified the three components of the Triad, only 8 % of coaches assessed menstrual function prior to sport participation. This study had several limitations, including: a sample size (91 coaches), minimal 30 % response rate, and a predominant response from female coaches, which is not indicative of the demographic of athletic coaches [22].
Current Awareness Study
In a recent study conducted at three prominent academic institutions, awareness of the Triad by physicians was also surprisingly low. Among 931 physicians surveyed, only 37 % had heard about the Triad (Fig. 10.3). Of the physicians surveyed, 51 % felt comfortable treating or referring a patient with the Triad, while 49 % did not. Orthopaedic surgery had the highest level of awareness (80.3 %) and anesthesiology (9 %) had the lowest levels of awareness (Fig. 10.4). On average, only 2.1 out of the three components could be properly identified. This initial study demonstrated that there is a need to educate physicians about the Triad spectrum so that they can diagnose those at risk for this disorder, discuss treatment interventions, and/or refer affected patients to the appropriate health professionals.
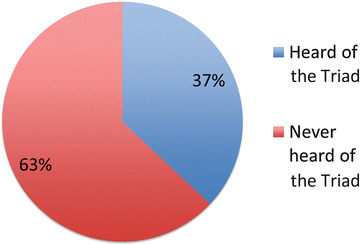
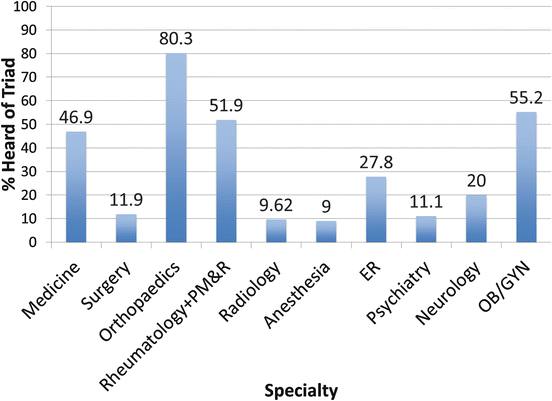

Fig. 10.3
Overall percentage of people who have heard of the Triad compared to those who have not heard of the Triad

Fig. 10.4
The percentage of respondents that have heard of the Female Athlete Triad based on specialty
Strategies to Promote Identification of Patients with Female Athlete Triad
The best approach to identifying patients who have or who are at risk for developing the Female Athlete Triad centers on obtaining a comprehensive history. In the Orthopaedist’s office, this includes taking a proper history of calcium and vitamin D intake, menstruation history and frequency, a history of stress reactions, stress fractures or fractures, exercise habits, and an assessment of energy availability. An open dialogue about the Triad components allows the clinician to gain the pertinent data, while also reviewing the importance of these issues to the patient.
Earlier chapters in this guide detailed these patient history themes; however, it is important to emphasize how incorporation of medical history that focuses on the factors that contribute athlete Triad will promote bone health in the female athlete. A verbal or written screening measure can be used to obtain nutritional, exercise and menstrual history. Multiple screening tools exist and each clinician must determine the best measure for his/her practice [23]. Based on these screening questions, if the athlete is determined to be at risk, further evaluation in all three components of the Triad should be initiated. This investigation should include a multidisciplinary approach, necessitating referral to other specialists.
During the patient evaluation, particular attention should be placed on identifying risk factors and warning signs. There are several nutritional, exercise-based and psychological behaviors known to be associated with increased risk of the Triad, such as participation in lean sports, menstrual irregularities, or stress fractures [24–28]. However, other warning signs may include a history of frequent injuries, mood changes, or a decrease in athletic performance.
As clinicians, we must also remember that components of the Triad occur in women participating in sport at all levels, including recreational and club athletes. We must have a low threshold to delve deeper into an area of concern.
Strategies to Increase Awareness of the Female Athlete Triad
Patient-Based Strategies
Increasing awareness of the Female Athlete Triad ought to be done at the patient and community-based level. Patient-based strategies focus on educating the athlete about the Triad, its components, and its impact on the athlete’s body. Miller et al. [29] found 45 % of female athletes surveyed did not identify a relationship between menstrual dysfunction and poor bone health, highlighting a disconcerting lack of awareness with the Triad. Even more troubling, 22 % of athletes participating in lean sports would not seek treatment for amenorrhea [29].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





