Chapter objectives
- •
Recognize and describe methods of assessing and measuring range of motion and flexibility.
- •
Identify the principles associated with stretching of connective tissue structures.
- •
Explain the principles and techniques for active, active assisted, passive, and resistive stretching.
- •
Identify the basic principles of proprioceptive neuromuscular facilitation and recognize its benefits for the rehabilitation of athletes.
- •
Identify key principles of, indications for, and contraindications to joint mobilization.
Range of motion is the available amount of movement of a joint, whereas flexibility is the ability of soft tissue structures, such as muscle, tendon, and connective tissue, to elongate through the available range of joint motion. Whether it is undergoing therapeutic stretching during postinjury rehabilitation or during a routine flexibility program, connective tissue is the most important physical focus of range-of-motion exercises. For favorable physiologic potentials to exist, both range of motion and range of flexibility need to be optimized. The connective tissue involved in the body’s reparative process after trauma or surgery often limits normal joint motion. Therefore, understanding the biophysical factors of connective tissue is important for determining optimal ways to increase range of motion because histologic evidence has shown that fibrosis can occur within 4 days of the onset of immobility. To effectively maintain and improve range of motion and flexibility, knowledge of both the related tissue structures and the various techniques used to facilitate extensibility of these structures is imperative.
Reasons for limitations in range of motion
The physiologic conditions associated with limitations in range of motion may vary. Often, a single structural component may be the cause of restricted movement. However, it is not uncommon to have related concurrent limitations from more than one structure. Structures that play a role in limiting one’s range of motion are summarized in Box 6-1 . Limitations as a result of structural involvement may be caused by a traumatic incident, such as surgery, or may develop over time from disuse, such as a lack of stretching. Furthermore, the pain associated with disruption of tissue or caused by joint swelling that becomes a space-occupying lesion and compresses against joint receptors and cutaneous nerves may inhibit one’s ability to actively and passively generate joint movement.
Joint capsule tightness
Ligamentous adhesions
Muscular spasm
Muscular tightness
Myofascial tightness
Pain
Joint effusion
Bony blocks
Stretching
Biophysical Considerations
Properties of Connective Tissue
Connective tissue is composed of collagen and other fibers within a ground substance—a protein-polysaccharide complex. A thorough discussion of the composition of connective tissue is presented in Chapter 2 . Connective tissue has viscoelastic properties, defined as two components of stretch that allow elongation of the tissue. The viscous component permits a plastic stretch that results in permanent tissue elongation after the load is removed. Conversely, the elastic component allows an elastic stretch, or temporary elongation, with the tissue returning to its previous length when the stress is removed. Range-of-motion exercise techniques should be designed to primarily produce plastic deformation. Repetitive intervention that incorporates sustained tissue elongation with low loads of stress versus shorter-duration aggressive loads may be more beneficial in achieving the clinical outcome of plastic deformational changes.
Neurophysiology
All stretching techniques are based on the premise of the stretch reflex, which involves two muscle receptors—the Golgi tendon organ (GTO) and the muscle spindle—that are sensitive to changes in muscle length. The GTO is also affected by changes in muscle tension. These receptors must be considered in the process of selecting any stretching procedure. The intrafusal muscle spindle responds to rapid stretch by initiating a reflexive contraction of the muscle being stretched. If a stretch is held long enough (at least 6 seconds), this protective mechanism can be negated by the action of the GTO, which can override the impulses from the muscle spindle. The reflexive relaxation that results is referred to as autogenic inhibition , and it allows effective stretching of the muscle tissue. Additionally, isotonic contraction of an agonist muscle causes reflexive relaxation of the antagonist muscle, which allows it to stretch. This phenomenon is referred to as reciprocal inhibition . Conversely, a quick stretch of the antagonist muscle will cause a contraction of the agonist muscle. For example, when the quadriceps muscle contracts, reflexive relaxation of the hamstring muscles occurs. In other words, when a tight muscle or muscles have been identified, an isotonic contraction of its antagonist will result in relaxation of the tight muscles and an improved range of motion. Autogenic inhibition and reciprocal inhibition are two components on which proprioceptive neuromuscular facilitation (PNF) stretching is based.
Duration
The amount and duration of the force applied during performance of the stretch are some of the principal factors determining how much elastic or plastic stretch occurs when connective tissue is stretched. Elastic stretch is enhanced by high-force, short-duration stretching, whereas plastic stretch results from low-force, long-duration stretching. Numerous studies representing decades of research have noted the effectiveness of prolonged stretching at low to moderate levels of tension. , A precise time frame for holding a static stretch has not been determined. Research has suggested that static stretches be held between 6 and 60 seconds, with 15- to 30-second holds most commonly being advocated. Some authors have proposed that a single static stretch of 15 to 30 seconds one time each day is sufficient for most people.
Temperature of Connective Tissue
Research has shown that temperature has a significant influence on the mechanical behavior of connective tissue under tensile stretch. Because connective tissue is composed of collagen, which is resistant to stretch at normal body temperature, the effect of increased tissue temperature on stretch has been studied. Synthesis of the body of research shows that higher therapeutic temperatures at low loads produce the greatest plastic tissue elongation with the least damage. Lentell et al reported greater increases in the range of motion of healthy shoulders after the application of heat.
Increased connective tissue temperature decreases the resistance of connective tissue to stretch and promotes increased soft tissue extensibility. It has been reported that collagen is very pliable when heated to a range between 102°F and 110°F. The use of ultrasound before joint mobilization has proved effective in elevating deep tissue temperature and extensibility. Draper and Ricard demonstrated the presence of a “stretching window” after a 3-MHz ultrasound application. This window indicates that for optimal tissue elongation, stretching should be performed during ultrasound treatment or within 3.3 minutes after termination of the treatment. In a follow-up study, Rose et al reported that after a 1-MHz ultrasound application, the deeper tissues cooled at a slower rate than did the superficial tissues; thus, the stretching window was open longer for deeper structures than for superficial ones. Although superior stretching results have been reported with the application of heat before and during stretching, other studies have found greater increases in flexibility after the application of cold packs. Brodowicz et al reported improved hamstring flexibility in healthy subjects after 20 minutes of hamstring stretching with an ice pack applied to the posterior aspect of the thigh when compared with subjects who received heat or who performed stretching without the application of any therapeutic agent. Kottke et al have also shown that greater plastic stretch results if the tissue is allowed to cool before tension is released, whereas others have reported that the use of cold during the end stages of stretching diminishes the cumulative gains in flexibility that occurred after the application of heat. Moreover, it appears that the use of either a superficial heat or a cold modality in conjunction with stretching results in greater improvements in flexibility than does stretching alone. It remains to be seen whether increased extensibility is the sole result of a single structure or a combination of structural changes perhaps related to musculotendinous, capsuloligamentous, or fascial tissue.
Objectivity of Range-of-Motion and Flexibility Assessments
Range of motion and flexibility are measured in a number of different ways. Typically, the type of tissue being assessed will dictate the method of assessment, although some methods may be used for various tissues. The primary movements that are assessed are termed as being physiologic or accessory . Physiologic movement accounts for the major portion of the range and can be measured with a goniometer (see Chapter 5 ). Physiologic joint movements occur in the cardinal movement planes and include flexion-extension, abduction-adduction, and rotation. Accessory motion, also referred to as arthrokinematics , is necessary for normal physiologic range of motion; it occurs simultaneously with physiologic motion and cannot be measured precisely.
The ability to accurately assess and measure physiologic range of motion appears to be dependent on the joint. These findings are detailed in Chapter 5 , and the reader is encouraged to be innovative in developing improved methods of measurement to enhance those that currently exist. Devices, such as a sit-and-reach tool, can be used to assess excursion of the hamstring muscles ( Fig. 6-1 ).

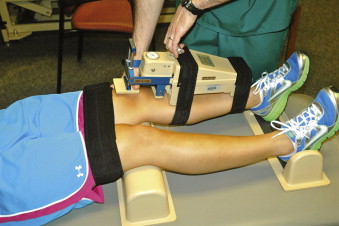
Accessory range of motion is much more difficult to assess and measure because it is often measured in units of millimeters. Experience in assessing both normal and abnormal joint accessory movement plays a critical role in one’s ability to accurately process such movement. Studies have shown a clear difference between novice and expert clinicians in determining accessory range of motion. Equipment can also be used to assess accessory joint motion, such as that seen when one is measuring the amount of anterior translation of the knee as a result of injury to the anterior cruciate ligament ( Fig. 6-2 ).
Types of Stretching Techniques
The limited joint range of motion caused by soft tissue restriction often inhibits initiation or completion of the rehabilitative process. Conservative treatment of contractures is only moderately successful, and overly aggressive stretching may result in undesired adverse effects. Optimal stretching is achieved only when voluntary and reflexive muscle resistance is overcome or eliminated and tissue elongation is facilitated. The main types of tissue that are stretched include musculotendinous, capsuloligamentous, and myofascial.
Three types of stretching techniques are generally recognized to facilitate musculotendinous flexibility: ballistic, static, and PNF. Ballistic stretching consists of repetitive bouncing movements that stretch a muscle group. Ballistic stretching has not been advocated because forces could be applied to a muscle that exceed its extensibility or that activate the muscle spindles described previously, with resultant microtrauma to the muscle fibers. However, it has been reported that because many physical activities involve dynamic movement, ballistic stretching should follow a static stretching routine. Static stretching involves stretching a muscle to a point of discomfort and holding the stretch for a length of time, followed by a return to normal resting muscle length. PNF involves alternating muscle contractions and stretching. The efficacy of all three techniques has been evaluated, and it appears that each technique has the capacity to increase flexibility, with static stretching being the safest of the three. . In some cases static stretching has been advocated over PNF because it is easier to teach and perform. Some clinicians prefer PNF stretching because it allows stretching to occur in functional planes of movement that more closely simulate activities. Each of the techniques should be performed with a prescribed set of repetitions while taking care to avoid overstretching. Contraindications to general stretching are indicated in Box 6-2 .
Limitation of joint motion by a bony block
Recent fracture
Evidence of an acute inflammatory or infectious process (heat and swelling) in or around joints
Sharp, acute pain with joint movement or muscle elongation
Hematoma or other indications of tissue trauma
Contractures or shortened soft tissues providing increased joint stability in lieu of normal structural stability or muscle strength
Contractures or shortened soft tissues forming the basis for increased functional abilities, particularly in individuals with paralysis or severe muscle weakness
Passive and Active Assisted Stretching Techniques
Various mechanical passive and active assisted techniques augment manual passive stretching. Methods of achieving the desired outcome are often limited only by creativity and improvisational skills. After the soft tissue restriction has been assessed, the clinician should analyze appropriate and effective ways of carrying out the treatment and rehabilitation plan. Several methods of stretching can be used, but a clinician should be careful to consider joint positioning when assessing extensibility and use standardized and consistent approaches to most accurately reflect reliable and valid measurements.
Spray and stretch
This technique has been described in detail by Travell and Simons. Spraying of Fluori-Methane *
* Available from Gebauer Chemical Co., Cleveland, OH.
or ethyl chloride * cools taut muscle fibers and desensitizes palpable myofascial trigger points, thereby facilitating stretching of the muscle to its full length. Passive stretch remains the central component in this technique. Concerns about the use of both vapocoolants have been documented. Travell and Simmons advocated the use of Fluori-Methane spray. However, because Fluori-Methane is a chlorofluorocarbon, which destroys the atmospheric ozone layer, its use has been questioned. Conversely, although ethyl chloride is not a chlorofluorocarbon, it is colder than Fluori-Methane, flammable, and explosive in a critical concentration with air. It is also a potent, readily acting general anesthesic (see Chapter 8 for additional information on vapocoolants). Ice stroking has been advocated as an alternative to the use of vapocoolants.Prolonged weighted stretch
The rationale for a prolonged-duration, low-load stretch has been discussed. Figure 6-3 illustrates a method of prolonged weighted stretching for the knee in which a small cuff weight is placed distally on the lower part of the leg to provide gentle passive stretching of the hamstring muscle group. Similar types of stretches can be performed for the upper extremity, as seen in Figure 6-4 . The key to success with prolonged-duration, low-load types of stretches is to allow muscle relaxation and gentle overpressure. If not comfortable, an athlete will contract the muscles surrounding the joint and resist the overpressure, which results in no short- or long-term gains in flexibility.


Assistive devices
These appliances aid in gaining and maintaining end range of motion. Assistive devices include pulleys, extremity traction, T-bars or wands, and continuous passive range-of-motion units. Pulleys are commonly used for restriction of the shoulder ( Fig. 6-5 ) and knee joints. Wands, T-bars, towels, sport sticks ( Fig. 6-6 ), or other similar apparatus may be used for individual active assisted stretching of the upper extremities.


Continuous passive range-of-motion units are often valuable mechanical devices that can benefit various joints. They can provide constant movement of a joint after surgical intervention and are most helpful because longer durations of passive movement can be implemented. Postoperatively, most continuous passive range-of-motion units are not set within a range of motion that provides tissue stretching beyond even the slightest level of discomfort. Rather, movement is facilitated within the range of motion that currently exists, thereby allowing the device to serve as more of a passive component to maintain range of motion and promote joint nutrition. As joint range of motion gradually increases, the controls can be adjusted to allow movement within a larger range of motion. A passive mode can be used on other equipment, including isokinetic units, to permit controlled passive range of motion with a pause to provide a stretch at the end range of motion ( Fig. 6-7 ). Some clinicians and patients alike do not promote the use of continuous passive range-of-motion and isokinetic units as a mechanism to maintain and gain joint range of motion for fear of the patient not being able to understand how to control the unit should any increase in pain be felt during use.

Adjustable dynamic splints can produce prolonged-duration, low-load force. The construction of these devices offers a lower progressive load that can be self-adjusted and graduated as orthotic tolerance time increases ( Fig. 6-8 ). Dynamic splints have been used successfully for the treatment of restrictions in knee and elbow motion.

Proprioceptive Neuromuscular Facilitation Techniques
PNF can be defined as a method of promoting or hastening the response of neuromuscular mechanisms through stimulation of mechanoreceptors. PNF stretching techniques are based on a reduction in sensory activity through the spinal reflexes to cause relaxation of the muscle to be stretched. Sherrington’s principle of reciprocal inhibition demonstrates relaxation of the muscle being stretched (agonist) through voluntary concentric contraction of its opposite (antagonist) muscle. Many studies , support the efficacy of PNF and show greater increases in flexibility when PNF is used rather than static or dynamic stretching techniques. Other investigations have found PNF to be at least as effective as other types of stretching. Originally, PNF was described as a rehabilitation technique for those recovering from neurologic disorders, but the technique has the capability of being used for various orthopedic conditions as well.
PNF patterns can be performed in a single plane, such as flexion-extension, or in rotational and diagonal patterns that incorporate multiple planes and synergistic patterns ( Table 6-1 ). PNF techniques generally consist of five 5-second trials of passive stretching followed by a 5- to 10-second maximal voluntary contraction, as indicated by the technique used. The work of Cornelius et al has shown that significant increases in systolic blood pressure occur after three trials consisting of a protocol of 5 seconds of passive stretching, followed by a 6-second maximal voluntary antagonist contraction. Thus, caution is warranted when one works with populations who have a predisposition to cardiovascular conditions.
| Extremity | Diagonal 1 | Diagonal 2 | ||
|---|---|---|---|---|
| Flexion | Extension | Flexion | Extension | |
| Upper | ||||
| Scapula | Elevation | Depression | Elevation | Depression |
| Shoulder | Flexion | Extension | Flexion | Extension |
| Adduction | Abduction | Abduction | Adduction | |
| External rotation | Internal rotation | External rotation | Internal rotation | |
| Elbow | Flexion | Extension | Flexion | Extension |
| Forearm | Supination | Pronation | Supination | Pronation |
| Wrist | Radial deviation | Ulnar deviation | Radial deviation | Ulnar deviation |
| Fingers | Flexion | Extension | Extension | Flexion |
| Lower | ||||
| Pelvis | Elevation | Depression | Elevation | Depression |
| Hip | Flexion | Extension | Flexion | Extension |
| Adduction | Abduction | Abduction | Adduction | |
| External rotation | Internal rotation | Internal rotation | External rotation | |
| Knee | Flexion | Extension | Flexion | Extension |
| Ankle | Dorsiflexion | Plantar flexion | Dorsiflexion | Plantar flexion |
| Foot | Inversion | Eversion | Eversion | Inversion |
| Toes | Extension | Flexion | Extension | Flexion |
Contract-relax
The contract-relax technique produces increased range of motion in the agonist pattern by using consecutive isotonic contractions of the antagonist. Box 6-3 outlines how this technique is performed.
- 1.
The body part to be stretched is moved passively into the agonist pattern until limitation of range of motion is felt.
- 2.
The athlete contracts isotonically into the antagonist pattern against strong manual resistance.
- 3.
When the clinician realizes that relaxation has occurred, the body part is again moved passively into as much range of motion as possible until limitation is again felt.
The procedure is repeated several times, followed by the athlete moving actively through the obtained range ( Fig. 6-9 ). When performing the contract-relax technique, the clinician must maintain proper stabilization to ensure that an isometric contraction occurs.

Hold-relax
Hold-relax is a PNF technique used to increase joint range of motion that is based on an isometric contraction of the antagonist performed against maximal resistance. This technique is done in the same sequence as the contract-relax technique, but because no motion is allowed on isometric contraction, this is the method of choice when joint restriction is accompanied by muscle spasm and pain. The intensity of each contraction is gradually increased with each successive repetition ( Fig. 6-10 ).

Slow reversal hold-relax
The slow reversal hold-relax technique uses reciprocal inhibition, as does the hold-relax technique. Box 6-4 outlines how this technique is performed. The technique is good for increasing range of motion when the primary limiting factor is the antagonist muscle group ( Fig. 6-11 ).
- 1.
The body part is moved actively into the agonist pattern to the point of pain-free limitation.
- 2.
An isometric contraction is performed in the antagonist pattern for a 5- to 10-second hold.
- 3.
The agonist muscle group actively brings the body part into a greater range of motion in the agonist pattern.
- 4.
The process is repeated several times.

Special Considerations for Proprioceptive Neuromuscular Facilitation
Proprioceptive neuromuscular feedback depends not only on the performance of an athlete but also on the ability of the clinician to provide appropriate and timely verbal and tactile commands. Verbal commands, such as “contract” and “relax,” must be made clear and at the precise moment to enhance gains in range of motion and minimize any associated discomfort. Hand placement by the clinician also provides tactile feedback and serves to inform the athlete into what direction a joint should be moving and with how much resistance. The limitations that exist will help dictate which PNF pattern is appropriate and how much resistance should be applied during performance of the technique.
Although specific patterns and techniques have been identified, it is also important for the athlete to progress through increasing levels of difficulty if one chooses to use a PNF technique to increase range of motion and muscle strength. Figure 6-12 demonstrates an upper extremity diagonal pattern that has been modified from the traditional supine position. Although not in accordance with standard teachings of true PNF techniques, use of the PNF upper extremity diagonal “2” extension pattern in a seated position not only applies similar resistance as when it is performed supine but also requires the athlete to develop trunk control without the assistance of gravity or a table. This modification more closely resembles an individual who may be preparing to throw a baseball or football.
Consider the activity and position when choosing PNF techniques for athletes in an attempt to closely simulate sport-specific function, proprioception, and gains in strength; clear and concise verbal commands will assist in optimal performance of an athlete during PNF exercises. To closely simulate sport performance, patterns and positioning may be modified.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








