Hip abnormalities affect most children with cerebral palsy. Dedicated surveillance programs have been shown to be effective means of identifying hips at risk and preventing pathologic dislocation. Patients who are ambulatory and correlate with Gross Motor Function Classification Score I and II experience deformities that affect mobility and gait, but rarely dislocations. Marginal and nonambulatory patients have an increasing risk of dislocation. Once subluxation has been identified, early surgical intervention is indicated. Long-term postoperative follow-up is needed to monitor for recurrence. Individuals who recur or who do not respond to initial soft tissue releases benefit from bony surgery. Comprehensive reconstruction of the hip has become the predominant treatment approach when acetabular and proximal femoral dysplasia is present. The painful arthritic dislocated hip has numerous treatment options. Hip arthroplasty procedures show promising results and may supplant other salvage options in the future.
The incidence and spectrum of hip abnormalities in children with cerebral palsy vary greatly. The reported incidence ranges from 2% to 75%. These reports include children who have significantly different degrees of neurologic involvement. The severity and pathology ranges from an alteration of gait or muscle contracture to painful neuromuscular dislocation. This wide spectrum raises several challenges for how best to identify the risk of hip deformities and how best to address their needs.
One of the major obstacles is having a reproducible system to allow comparison of different patient populations and different treatments. Currently, most common clinical descriptions of patients with cerebral palsy incorporate the movement abnormality (spastic vs athetoid) and a geographic description of the areas involved (diplegia or quadriplegia). However, children with the same diagnosis, such as spastic diplegia, do not necessarily have the same functional impairment or clinical course. Stratifying patients by functional capacity helps identify the risk relative to their level of independent function. Lonstein and Beck reported the incidence of hip abnormalities to be 7% in independent ambulators and up to 60% in nonindependent sitters. More recently, the Gross Motor Function Classification Score (GMFCS) categorizes youths and children with cerebral palsy. This system classifies patients into 5 levels based on self-initiated motor function. It is not intended to classify children’s best performance or potential for improvement; emphasis is paid to sitting, walking, and wheeled mobility in the community (ie, daily function). The classification has been updated to incorporate individuals in late adolescence. The full classification is available online at www.canchild.ca
Level I: walks without limitation
Level II: walks with limitations
Level III: walks using a hand-held mobility device
Level IV: self-mobility with limitations; may use power device
Level V: transported in manual wheelchair.
The GMFCS classification has gained clinical acceptance as a means of simplifying communication amongst researchers and as a means to guide treatment plans. Using the GMFCS, Soo identified the incidence of hip displacement as 0% for children with GMFCS level I and 90% for those with GMFCS level V. Compared with children with GMFCS level II, those with levels III, IV, and V had significantly higher relative risks of hip displacement (2.7, 4.6, and 5.9, respectively).
Natural history
In the normal hip, balanced muscle use promotes the symbiotic development of the acetabulum and femoral head. Upright posture and ambulation promotes remodeling of neonatal femoral anteversion. Children with cerebral palsy are born with normal hips. However, these hips are soon subjected to abnormal muscle forces that lead to hip abnormalities.
The ability to ambulate determines the fate of the hips. Children who become independent ambulators by age 5 years develop enough muscle balance to stabilize the hips; they may develop acetabular dysplasia or femoral head deformities but do not dislocate. Children who ambulate with crutches, walkers, or canes may develop silent and painless subluxation of hips that may not be a clinical issue for years. Nonambulators may begin to dislocate before the age of 7 years.
In a mathematical model of the spastic hip, the increased tone to the spastic muscles creates a hip-force magnitude 3 times that of the normal hip. It is thought that the main muscle deformers of the hip joint are the adductors, hip flexors, and hamstrings. The hip joint has a ball-and-socket configuration that presumably maximizes contact between the femoral head and the acetabulum throughout a wide range of different positions including flexion and extension. However, a computer model has demonstrated “very little ‘containment’ of the posterior and lateral surfaces of the femoral head” (p354) in the sitting position. The persistent femoral anteversion redirects the head away from the depth of the socket toward the rim.
The combination of spastic muscle activity and altered sitting posture redirects the femoral head to the superolateral and posterior aspects of the acetabulum. If the weak abductors and extensors are unable to offset the adductor spasticity, a contracture of the adductors and the inferomedial joint capsule develops in time. The femoral head is directed and restricted to the lateral rim of the socket. The abnormal forces on the chondroepiphysis of the acetabulum presumably lead to suppression of normal growth. Based on computed tomography (CT) scans, the deficiency is usually in the superolateral or posterior aspect of the acetabulum. It is unclear whether the acetabulum is dysplastic or is enlarging. Recent three-dimensional (3D) reconstruction study has shown that, once the hip dislocates, the acetabular deformity becomes global and the volume of the acetabulum decreases in much the same way that a saucer holds less volume than a cup. The greatest deformation of the acetabulum and femoral head occurs when the migration index is 52% to 68%. In cases in which the spasticity of the legs is asymmetric, a windblown deformity develops with the infrapelvic obliquity. The high side usually dislocates, although exceptions do occur. Subluxation and dislocation of the hip correlate with muscle imbalance and not pelvic obliquity.
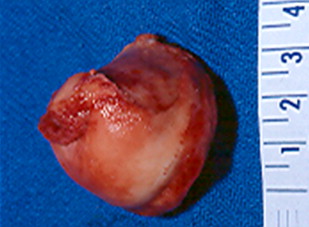
With progressive subluxation, the femoral head presses up to the lateral edge of the acetabulum. The lack of mobility and increased pressure on the medial aspect of the femoral head leads to flattening and a loss of sphericity. The superior portion of the femoral head remodels, resulting in the characteristic triangular-shaped femoral head, and the articular cartilage of the femoral head is denuded Fig. 1 . It is debatable whether the loss of articular cartilage is caused by degeneration caused by immobility and lack of contact with the opposing articular surface, pressure from the superior rim of the acetabulum, or from compression from the overlying soft tissues. There are no reports of mirror image articular cartilage lesions on the acetabular side. Regardless of the cause, the combination of remodeling and articular cartilage degeneration produces a femoral head that is not considered to be reconstructable.