FIGURE 21-1 Clinical photographs of a preadolescent child with atraumatic multidirectional instability. A: Anterior view demonstrates obvious anteroinferior position of the humeral head. B: View of the lateral aspect depicts inferior humeral head position and the “sulcus” sign.
Finally, there are some pediatric patients who sustain glenohumeral joint dislocation due to neuromuscular pathology. In cases of arthrogryposis, brachial plexus birth palsy, stroke, or cerebral palsy, muscle imbalance with or without glenohumeral joint dysplasia can lead to atraumatic dislocations, even in neonates or young children.13,77,148,152,411,451,458 These situations must be distinguished from neonatal pseudodislocation, in which a traumatic displaced physeal fracture and radiographically unossified proximal humeral epiphysis may give the radiographic appearance of glenohumeral dislocation.
Associated Injuries with Shoulder Dislocations
The axillary nerve is commonly injured in association with shoulder dislocations. Because of its circuitous course around the proximal humerus and inferior to the glenohumeral joint, as well as its relative tethering at the quadrilateral space, the axillary nerve is usually stretched at the time of humeral head dislocation. As these are neuropraxic injuries, spontaneous recovery is typically seen, though recovery may take many months. In the event of complete axillary nerve injuries without spontaneous recovery after the expected period of time, the axillary nerve may be explored, repaired, grafted, or neurotized to provide return of deltoid motor function.18,37,79,87,118,268 Similarly, injuries to the axillary artery, though rare, have been reported in association with shoulder dislocation.18,87,301 Prompt fracture reduction with or without arterial reconstitution should be performed in cases of vascular insufficiency and ischemia.
While less common than in adults, concomitant fractures of the proximal humerus (e.g., lesser tuberosity, greater tuberosity) or scapula (e.g., coracoid process, glenoid) may be seen with shoulder dislocation.76,109,355,436 (Fig. 21-2). Careful inspection of plain radiographs is needed to assess for associated bony injuries. While nondisplaced fractures may be effectively treated nonoperatively, displaced fractures may predispose to recurrent instability.239
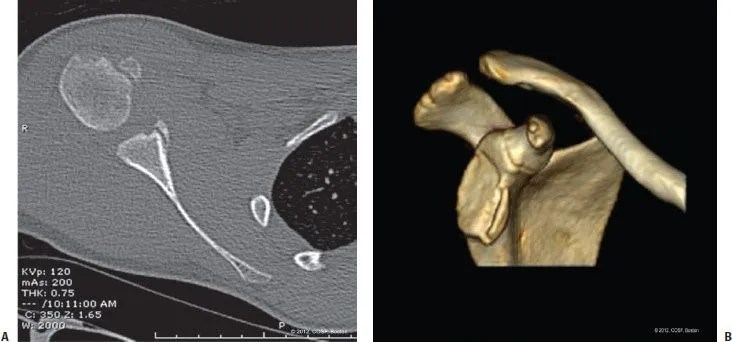
FIGURE 21-2 Computed tomography (CT) images of a 13-year-old male after traumatic anterior shoulder dislocation. Axial images (A) and three-dimensional reconstruction with subtraction of the humeral head (B) depict an anterior glenoid fracture (bony Bankart lesion).
Signs and Symptoms of Shoulder Dislocations
In cases of traumatic anterior glenohumeral joint dislocations, patients will present with pain, swelling, and limited shoulder motion. Typically the limb is held in slight abduction and external rotation, and often the patient will support the affected extremity with the contralateral hand. Careful inspection will reveal abnormal contour of the shoulder, with a prominent acromion, flattened or concavity to the posterolateral shoulder girdle, and obvious prominence or fullness anteriorly in the area of the dislocated humeral head. Careful and comprehensive physical examination is critical to rule out concomitant neurologic injury. The axillary nerve is most commonly affected; sensation over the lateral aspect of the shoulder and deltoid muscle function is checked to assess axillary nerve function (Fig. 21-3). In cases in which there has been spontaneous reduction after an anterior instability event, the shoulder appears more normal in contour and glenohumeral motion is typically preserved. Patients will be guarded in active motion especially above the shoulder line, resist extremes of abduction and external rotation, and the apprehension test will be positive.122,263,368,427

FIGURE 21-3 A: Sensory distribution for the axillary nerve important in anterior dislocation. B: Deltoid muscle can be tested in acute anterior dislocation by grabbing the muscle belly with the right hand while supporting the elbow with the left. The patient then can actively contract the deltoid by pushing the elbow against the examiner’s hand while the examiner feels the muscle contraction.
Conversely, patients with traumatic posterior dislocations will present with a painful adducted and internally rotated shoulder. There is often flattening or concavity to the anterior aspect of the shoulder girdle, with palpable fullness posteriorly. Prominence of the superomedial scapular angle (the so-called Putti sign) is often seen, and patients will resist attempts at passive shoulder motion. Inability to passively externally rotate the shoulder or supinate the forearm should alert the examiner to the possibility of a posterior glenohumeral joint dislocation. Again, a comprehensive examination is performed to evaluate for associated neurovascular deficits.
In neonates and infants, pseudodislocation may similarly present with pain, reluctance to move the affected upper limb, swelling, and asymmetric contour of the shoulder girdle. Occasionally crepitus due to motion at the fracture site may be appreciated with gentle, small arc range of motion.
Children and adolescents with atraumatic and/or multidirectional instability present quite differently. In addition to the lack of causative or antecedent trauma, these patients may not have pain with joint subluxation or dislocation (Fig. 21-1). Even with discomfort, patients will frequently report rapid resolution of pain after reduction. Examination will often elicit diffuse signs of ligamentous laxity, including hyperextension of the elbow, knee, and metacarpophalangeal joints.307 Abnormally hyperelasticity and striae of the skin may be seen. Focused examination of the shoulder will demonstrate a positive sulcus sign and increased translation with anterior and posterior load-and-shift testing.419 The sulcus sign refers to a concavity or indentation noted of the skin inferior to the acromion with manual longitudinal traction applied to the adducted arm (Fig. 21-4). Anterior and posterior load-and-shift tests are performed with the examiner standing behind or alongside the patient. While stabilizing the scapula with one hand, the humeral head is grasped and translated anteriorly and/or posteriorly with the examiner’s other hand; translation of greater than 5 mm from center is thought to be an indicator of multidirectional instability. Though some patients are truly unstable in all directions, posterior-inferior dislocations are most common. This pattern may be elicited with forward flexion and slight adduction, with joint reduction achieved with abduction. Patients with voluntary instability may demonstrate their condition by contracting the anterior deltoid and internal rotators while inhibiting the antagonistic muscles.

FIGURE 21-4 Dramatic demonstration of inferior subluxation of the glenohumeral joint in a patient with multidirectional instability. The clinical correlate is the sulcus sign.
Imaging and Other Diagnostic Studies for Shoulder Dislocation
Radiographic evaluation should include orthogonal views of the shoulder to assess for direction of dislocation, congruency of subsequent joint reduction, and presence of associated bony injuries. Anteroposterior (AP) and axillary views are preferred (Fig. 21-5). In the acutely injured or anxious, uncomfortable child, alternative views including the transthoracic scapular Y, West Point lateral, or apical oblique projections may be performed.69,144,156,400 AP views with the shoulder in internal rotation are not routinely required, but may allow for visualization of Hill–Sachs lesions of the humeral head.

FIGURE 21-5 Anterior dislocation of the right shoulder in a 15-year-old girl. A: Note the typical subcoracoid position on the AP film. B: On a true scapular lateral film, note the anterior displacement of the humeral head. C: Postreduction film demonstrates a Hill–Sachs compression fracture in the posterolateral aspect of the humeral head. D: On the postreduction axillary film, note the posterolateral compression fracture of the humeral head.
In patients with recurrent instability or in whom the extent of injury needs to be assessed after the initial traumatic dislocation, advanced imaging may be performed. Magnetic resonance imaging (MRI) will provide visualization of chondral, labral, capsular, and musculotendinous pathology. The addition of intra-articular contrast improves sensitivity for labral pathology and provides more detailed information regarding capsular patulousness; this is particularly helpful in patients with persistent, functionally limiting multidirectional instability in whom surgical treatment is being considered (Fig. 21-6). While computed tomography (CT) and CT-arthrography are less helpful for soft tissue evaluation, they do provide the best modality to identify and quantify bony defects in the glenoid and humeral head.75,101,227 (Fig. 21-7). In children and adolescents in whom a large portion of the glenoid is incompletely ossified, careful inspection of the glenoid contour is needed to avoid missing bony lesions. Loss of the normal sclerotic margin of the glenoid has been proposed as a sign of bony defects of the anterior glenoid rim.210
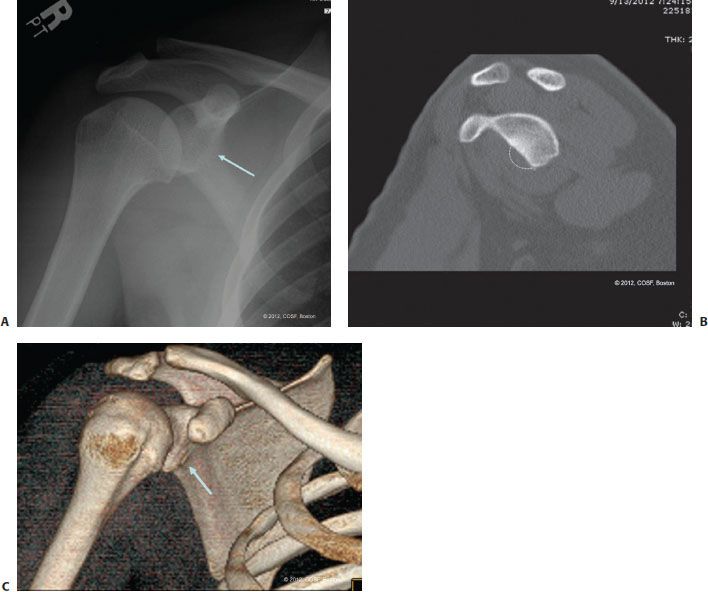
FIGURE 21-7 Bony glenoid deficiency in the setting of recurrent anterior instability in a 16-year-old male. A: AP radiograph depicts loss of the sclerotic margin of the anterior glenoid. B: Sagittal CT scan demonstrates loss of the anterior-inferior glenoid. C: Three-dimensional reconstruction further highlights the loss of anteroinferior glenoid bone.

FIGURE 21-6 MRI arthrogram of the left shoulder in a 14-year-old female with multidirectional instability. Axial (A) and coronal (B) images depict an intact labrum with a patulous capsule.
Radiographic evaluation of patients with atraumatic multidirectional instability is similar, though a few points deserve mention. Though plain radiographs are typically normal, patients with congenital glenoid hypoplasia will have subtle rounding or convexity to the glenoid fossa, with or without scapular neck dysplasia.77,85,88,334 As cited above, MRI-arthrography is a useful tool in assessing the capsular laxity and presence of pathologic lesions of the labrum in these patients.
Classification of Shoulder Dislocations
In general, shoulder dislocations in children and adolescents are described according to the association with trauma, direction of instability, chronicity, and presence of underlying local or systemic disorders (Table 21-1). Characterizing shoulder dislocations according to these categories is important and influences treatment decision making.11
TABLE 21-1 Classification of Shoulder Instability

As noted in Table 21-1, shoulder dislocations may be traumatic or atraumatic in etiology. Direction of humeral instability may be anterior, posterior, inferior (luxatio erecta), or multidirectional. As in adults, perhaps 90% of traumatic dislocations in children and adults is anterior, with posterior dislocations occurring much less commonly and luxatio erecta described in case reports.44,130,132,179,246,283,286,356 Furthermore, pathologic instability may include both subluxation or true dislocation. Dislocation refers to situations in which the humeral head moves completely out of the glenoid fossa, with no articular contact and often with locking of the humeral head on the anterior or medial rim of the glenoid. Subluxation is defined as an incomplete dislocation characterized by pain, a feel of “looseness” or “slipping,” and/or a “dead” feeling to the affected limb. Even traumatic subluxations have been associated with structural injury to the glenoid labrum and Hill–Sachs lesions of the humeral head.327 These conditions must be distinguished from ligamentous laxity, which is typically asymptomatic.
Chronicity is generally classified as being acute, recurrent, or chronic. While a single episode of dislocation denotes acute instability, recurrent instability refers to multiple episodes. Chronic instability refers to unrecognized or untreated shoulder dislocations in which the humeral head is not reduced, and may be seen with congenital or neuromuscular conditions in children.
The presence or absence of associated systemic conditions—including collagen disorders such as Ehlers–Danlos syndrome, or congenital/neuromuscular syndromes such as cerebral palsy—is also a key consideration in diagnosis and management.
PATHOANATOMY AND APPLIED ANATOMY RELATING TO SHOULDER DISLOCATION
The anatomic development, structure, and growth of the proximal humerus are described in the section on proximal humerus fracture. The glenoid is a shallow, concave fossa with which the humeral head articulates. The radius of curvature of the humeral head is approximately three times that of the glenoid. As the glenohumeral articulation lacks substantial bony constraint, the shoulder is afforded near global range of motion, facilitating placement of the hand in space and upper limb function.
Given the relatively unconstrained bony architecture, the glenohumeral joint relies primarily on soft tissue capsuloligamentous structures for stability. The cartilaginous labrum runs along the rim of the glenoid, deepening the concavity and conferring stability. The glenohumeral ligaments are confluent with the labrum and are thickenings of the joint capsule. The inferior glenohumeral ligament has both anterior and posterior components. The anteroinferior glenohumeral ligament is taught and biomechanically contributes most stability in shoulder abduction and external rotation. Disruptions of the anteroinferior glenohumeral ligament or anteroinferior labrum (Bankart lesion) are most commonly seen with anterior traumatic instability (Fig. 21-8). Furthermore, traumatic instability may also cause elevation of the anterior labrum with the periosteum of the anterior glenoid neck, resulting in the so-called anterior labroligamentous periosteal sleeve avulsion (ALPSA).309 The middle glenohumeral ligament is primarily responsible for stability in midabduction and external rotation, whereas the superior glenohumeral ligament resists inferior translation of the humeral head.

FIGURE 21-8 A: The tight anteroinferior glenohumeral ligament complex with the arm abducted and externally rotated. This ligament sling is the primary restraint against anterior instability of the shoulder. B: A cross section in the transverse plane through the glenohumeral joint demonstrates the common lesions associated with anterior instability of the shoulder: Hill–Sachs lesion, Perthes–Bankart lesion, and redundant anteroinferior glenohumeral ligaments. (HH, humeral head; P, posterior.)
On the humeral side, the joint capsule inserts along the anatomic neck of the humerus, except for medially where the insertion lies more inferiorly along the proximal humeral metaphysis. Thus the proximal humeral physis is predominantly extracapsular, with exception of the very medial extent. Shoulder dislocation may result in detachment of the capsule from its humeral insertion, resulting in the so-called humeral avulsion of the glenohumeral ligament (HAGL) lesions.463 Failure of recognition and repair of these HAGL lesions is a common cause of recurrent instability after surgical treatment.341
The glenohumeral joint is surrounded by the rotator cuff muscles, comprising the supraspinatus, infraspinatus, teres minor, and subscapularis. While rotator cuff tears are uncommon in children, these musculotendinous units form a force couple with the larger surrounding shoulder girdle muscles (deltoid, pectoralis major, teres major, and latissimus dorsi) and serve as important dynamic secondary stabilizers of the shoulder. The dynamic stabilizing effects of the rotator cuff muscles are largely the focus of nonoperative rehabilitative programs for young patients with glenohumeral instability.52
TREATMENT OPTIONS FOR SHOULDER DISLOCATIONS
Nonoperative Treatment of Shoulder Dislocations
Indications/Contraindications
Treatment options continue to evolve for shoulder instability in children and adolescents, though remain based upon the classification system and considerations described above. Nonoperative treatment is typically recommended for acute traumatic dislocations as well as atraumatic multidirectional instability.
Closed reduction is performed for acute traumatic dislocations, and a host of reduction maneuvers have been described. Adequate analgesia and relaxation facilitates closed reduction, and both conscious sedation and intra-articular anesthetic injection have been advocated. Multiple reports have suggested that intra-articular lidocaine injection is as safe and effective as intravenous sedation, with less cost and shorter length of stays.73,281,295,299,444 The method of traction–countertraction is advocated by many (Fig. 21-9). In this method, a bedsheet is looped around the axilla of the affected shoulder and passed superiorly and laterally to the contralateral shoulder. Longitudinal traction is applied to the affected upper extremity in line with the deformity, with countertraction provided by pull of the bedsheet. Steady, continuous traction will ultimately overcome the spasm of the shoulder girdle muscles, and the humeral head may be disimpacted and reduced. Others advocate modifications of the Milch maneuver.96,292,293,317,399 In this technique, the patient is positioned supine and the affected limb supported. Gradual abduction and external rotation is used to achieve glenohumeral reduction. As this technique does not employ traction to overcome muscle spasm, it may be successfully performed without sedation.237,366 Still others utilize the Stimson technique of reduction (Fig. 21-10).413 With the patient in prone position and the affected limb hanging free over the edge of the stretcher, longitudinal traction is applied to the extremity by means of a weight attached to the wrist. As the spasm of the shoulder girdle muscles fatigues and is overcome, reduction is achieved spontaneously and relatively atraumatically. Additional scapular mobilization may assist with reduction using the Stimson technique 231,285

FIGURE 21-9 Techniques for closed shoulder reduction. A modification of the Hippocratic method uses a handheld sheet around the thorax to provide countertraction.

FIGURE 21-10 The Stimson technique for closed shoulder reduction. With the patient in prone position, weight is hung from the wrist to distract the shoulder joint. Eventually, with sufficient fatigue in the shoulder musculature, the joint can be easily reduced.
Posterior dislocations may be similarly reduced with traction–countertraction maneuvers. Furthermore, the addition of a laterally directed force on the proximal humeral diaphysis may assist in achieving reduction.297 In the rare inferior dislocations (or luxatio erecta), a two-step closed reduction maneuver has been advocated.310 An anterior-directed force is applied to the humeral shaft, converting the inferior dislocation to an anterior one. Subsequent external rotation will then achieve glenohumeral reduction. Closed reduction is the definitive management of luxatio erecta in the majority of cases.329
Outcomes
Following closed reduction, patients are typically immobilized with a sling for comfort. There is no evidence that longer duration of sling immobilization with the shoulder in internal rotation reduces the risk of recurrent instability.330 Recent work, however, has raised the question of whether immobilization with the shoulder in adduction and external rotation is preferred. Anatomically, 30 degrees or more of external rotation of the shoulder may tension the anterior soft tissues and “reduce” the torn anterior capsulolabral structures to a more anatomic position on the glenoid.206,294 Dynamic MRI have demonstrated improved position of the displaced labrum with external rotation.207,378,384,398 Subsequent clinical studies have demonstrated up to a 40% reduction in recurrent instability rates when external rotation bracing was utilized for 4 or more weeks.204,205,418 These findings have not been universally reproducible; however, other investigators have failed to demonstrate reduction in recurrent instability with external rotation immobilization.126,255,259,330,417 Regardless of the type or time of immobilization after reduction of acute dislocation, physical therapy is typically recommended to improve the dynamic stability conferred by the rotator cuff and adjacent shoulder girdle muscles.52
Despite successful closed reduction and subsequent rehabilitation, there is a high risk of recurrent instability, particularly in young, active patients.284 The available literature, however, is limited in quantifying the true recurrent dislocation rates in children and adolescents. Much of the previously published information consists of retrospective case series of both adult and pediatric patients with limited follow-up.
Rowe361 previously reported recurrent anterior instability in 100% of children less than 10 years of age and 94% of patients between 11 and 20 years. Marans et al.276 similarly reported universal recurrent instability in their series of 21 children following traumatic dislocations. Wagner and Lyne443 reported an 80% recurrence in 10 patients with open physes. In a series of nine patients who sustained traumatic instability at a mean age of 12.3 years, Elbaum et al.118 similarly reported recurrent instability in 71%. In their review of 154 traumatic dislocations, Vermeiren et al.435 found a 68% recurrence rate in patients less than 20 years of age. Higher rates of recurrent instability have been reported in higher-energy injuries as well as those associated with bony glenoid injuries.291,349,354 Younger patients involved in overhead or contact sports have similarly been noted to have higher recurrent instability rates.367
Other reports, however, cite lower recurrence rates in younger patients. Rockwood356 documented a 50% recurrence rate in patients between 13.8 and 15.8 years of age. Cordischi et al.83 published their study of 14 patients between 10.9 and 13.1 years of age and reported that only three patients (21%) went on to surgical treatment for recurrent instability. In perhaps the largest study with the longest follow-up, Hovelius et al.189 reported 25-year follow-up on 229 shoulder in 227 patients who sustained their first traumatic dislocation between 12 and 40 years of age. Of the 58 patients who sustained their primary dislocation between 12 and 19 years of age, 26% reported a single recurrence, and an additional 16% of shoulders stabilized over time (defined as no instability events in the last 10 years). Only 43% of patients underwent surgical stabilization procedures. Additional case reports and small case series exist of young patients without recurrent instability at midterm follow-up (Table 21-2).121,171
TABLE 21-2 Classification of Non-Operative Treatment for Shoulder Instability

Operative Treatment of Shoulder Dislocations: Arthroscopic Bankart Repair
Indications/Contraindications
Surgical treatment is considered in patients with functionally limiting recurrent instability as well as in high-demand, overhead or contact athletes in whom the risk of recurrent instability after their primary event is unacceptably high. In general, patients considered for surgery should have failed attempts at physical therapy and rehabilitation. In patients with traumatic anterior shoulder dislocations, recurrent instability is due to injury to the anterior-inferior labrum and adjacent glenohumeral joint capsule and ligaments. Surgical treatment is focused on repairing the torn labrum to its anatomic location on the glenoid rim.
Surgical Procedure
Preoperative Planning. Presently, arthroscopic labral repair is the standard treatment for posttraumatic shoulder instability. Preoperative imaging should include plain radiographs of the affected shoulder to rule out associated bony lesions (e.g., glenoid fractures, Hill–Sachs lesions). MRI, with or without intra-articular contrast, is also helpful in determining the extent of labral injury and assessing for concomitant soft tissue injuries. Typical equipment required includes a standard 4-mm 30-degree arthroscope, arthroscopic cannulae, and surgical instruments used to mobilize and prepare the capsulolabral tissue (e.g., arthroscopic shavers, elevators, rasps, and suture passing devices). While a host of commercially available instruments are available, all provide the same fundamental arthroscopic capabilities. Suture anchors are also invaluable for arthroscopic labral repairs, and increasing the standard is to use bioabsorbable suture anchors for intra-articular procedures (Table 21-3).
TABLE 21-3 Bankart Repair for Shoulder Instability

Positioning. In general arthroscopic stabilization may be performed in either the beach chair or lateral decubitus position (Fig. 21-11). Advantages of lateral decubitus position include ease of longitudinal and lateral distraction to assist in visualization and access to the axillary recess of the glenohumeral joint. Patients are placed with the unaffected shoulder down, allowing the thorax to fall posteriorly about 10 degrees, which will place the glenoid parallel to the ground. Care is taken to place an axillary roll and pad all bony prominences (e.g., contralateral fibular head) to avoid excessive or prolonged compression of the peripheral nerves. The entire affected limb and shoulder girdle are prepped and draped into the surgical field. The limb is placed in balanced suspension with about 40 degrees of abduction and 10 to 20 degrees of forward flexion, typically with 7 to 10 lb of longitudinal and lateral distraction with the assistance of a limb holder. This allows for circumferential access to the shoulder girdle. Furthermore, additional abduction–adduction and internal–external rotation may be employed during surgery for selective access and tensioning of soft tissues.

FIGURE 21-11 Patient positioning for surgical procedures. A, B: Beach chair positioning allows for near circumferential access to the shoulder girdle. C: Lateral decubitus positioning with assistance of a bean bag. D: Use of longitudinal and/or lateral distraction will facilitate arthroscopic visualization.
The modified beach chair position is also effective and commonly utilized. After placement of a roll or bump behind the patient between the scapulae, patients may be positioned with the affected limb and shoulder girdle off the edge of the table to allow circumferential access. The use of commercially available beach chairs, limb holders, and/or bean bags will assist with positioning.
Surgical Approach(es). The procedure begins with examination under anesthesia to assess pathologic instability anteriorly, posteriorly, and inferiorly. After glenohumeral joint is insufflated with sterile saline solution, a standard posterosuperior, anterosuperior, and anteroinferior arthroscopy portals are established. Viewing is traditionally performed from the posterosuperior portal, but moving the camera to the anterosuperior portal will allow for improved visualization of the anterior glenoid neck and anterior soft tissues, particularly in cases of long-standing instability where the labral and capsule have scarred in a more medial position.
Technique. Arthroscopic survey is performed to assess the extent of labral, capsular, and/or bony injury (Fig. 21-12). After confirmation of labral pathology, the capsulolabral complex is mobilized from its typical medial position using arthroscopic elevators. The glenoid rim and medial glenoid neck in the region of the labral tear is similarly prepared with arthroscopic rasps or shavers in efforts to debride fibrinous tissue and prepare a bleeding bony bed for biologic healing. In a sequential fashion, arthroscopic suture anchors are placed from inferior to superior and sutures are shuttled through the capsulolabral complex.346,385,431 Knots are tied in a sequential fashion, reapproximating the labrum to its anatomic location and retensioning the soft tissues. While a host of commercially available devices and techniques may be utilized, all conform to the standard principles of soft tissue mobilization, glenoid preparation, and repair of the soft tissue to the glenoid rim, thus tensioning the anteroinferior capsule (Table 21-4).
TABLE 21-4 Bankart Repair for Shoulder Instability


FIGURE 21-12 Arthroscopic Bankart repair. A: Arthroscopic image of an anterior labral tear in the right shoulder of a 16-year-old male. The patient is positioned in the lateral decubitus position. B: Arthroscopic appearance after anterior labral repair, demonstrating reapproximation of the labral tissue to the glenoid rim.
Operative Treatment of Shoulder Dislocations: Latarjet Reconstruction
Indications/Contraindications
In patients with traumatic anterior shoulder dislocations, recurrent instability may also be due to bony fracture or bony insufficiency of the anteroinferior glenoid.291,354 In these cases, soft tissue procedures alone may not address the underlying pathoanatomy and are prone to failure. Surgical treatment in these situations typically involves restoring or augmenting the bony deficit of the glenoid. While several techniques have been advocated, transferring the coracoid process with its soft tissue attachments to the glenoid (the so-called Latarjet procedure) has increasingly become the standard of care.331,336 Bony reconstructions such as the Latarjet procedure have also been advocated in patients with recurrent instability after prior failed soft tissue reconstruction.
In addition to providing additional bony support for the articulating humeral head, the Latarjet procedure also stabilizes the glenohumeral joint by virtue of the fact that the conjoined tendon remains attached to the tip of the coracoid during transfer. These soft tissues act as a “sling” and provide additional anteroinferior stability. Stability is further conferred by preservation of the musculotendinous fibers of the subscapularis. This “triple effect” has been touted by Patte and Debeyre.99,331,445
Surgical Procedure
Preoperative Planning. Though MRI is helpful in identifying and qualitatively assessing the extent of labral injury, Latarjet reconstructions are typically reserved for recurrent posttraumatic instability with associated glenoid loss; or, in those patients who have failed prior soft tissue stabilizations. In these situations, assessment of glenoid bone loss and possible engaging Hill–Sachs lesions is best done with CT with three-dimensional reconstructions (Fig. 21-7).
Most Latarjet reconstructions are performed via open deltopectoral approaches. Aside from the standard instruments and retractors used for open shoulder surgery, a few additional items are useful. A 90-degree oscillating saw blade will facilitate accurate and efficient coracoid osteotomy. Appropriate-sized cannulated screws—typically 4 mm in diameter and 34 to 40 mm in length—are used for fixation of the coracoid process to the anterior glenoid (Table 21-5).
TABLE 21-5 Latarjet Reconstruction for Shoulder Instability

Positioning. The modified beach chair position is effective and commonly utilized. A roll or bump is placed behind the patient between the scapulae, to allow for scapular positioning and improved access to the glenoid neck. Patients are positioned with the affected limb and shoulder girdle off the edge of the table to allow circumferential access. The use of commercially available beach chairs, limb holders, and/or bean bags assist with positioning.
Surgical Approach(es). A standard deltopectoral approach is utilized. The incision is placed slightly more medial and superior than traditional deltopectoral approaches to the shoulder, because of the need to expose the coracoid and medial glenoid neck. A vertical incision in Langer skin lines will maximize the aesthetics of the resultant scar. Superficial dissection will allow visualization of the deltopectoral interval, which is developed taking the cephalic vein laterally with the deltoid. Deep dissection will allow visualization of the coracoid process, conjoined tendon, clavipectoral fascia, and subscapularis muscles.
Technique. After initial dissection is performed, a spike Hohmann retractor is placed superiorly over the coracoid process, with its tip just anterior to the origin of the coracoclavicular (CC) ligaments. The shoulder is abducted and externally rotated, placing the coracoacromial (CA) ligament under tension. The CA ligament is then divided approximately 1 to 2 cm from the coracoid, leaving a cuff of tissue which will be used later for capsular reconstruction. The shoulder is then adducted and internally rotated. The pectoralis minor insertion is then released off the coracoid process, being careful to protect the brachial plexus which lies deep to the pectoralis minor. Following this, the coracoid is osteotomized at its flexure, or “knee,” from medial to lateral. The use of commercially available 90-degree microsagittal saws will facilitate coracoid osteotomy. The coracoid is then freed from the remaining surrounding soft tissue attachments, including the deep coracohumeral ligament, and mobilized while protecting the origin of the conjoined tendon. The undersurface of the coracoid is decorticated to expose bleeding cancellous bone. Two drill holes (typically 3.5 to 4 mm) are made in the coracoid to facilitate subsequent screw placement. Overzealous mobilization or retraction of the freed coracoid process is avoided, as the musculocutaneous nerve enters the coracobrachialis approximately 4 to 5 cm distal.
Direction is then turned to glenoid preparation. With the shoulder in adduction and external rotation, the subscapularis is split in line with its muscle fibers between the superior two-thirds and inferior one-third. This muscle splitting technique preserves subscapularis integrity, contributing stability and minimizing iatrogenic injury to the axillary nerve. The plane between the subscapularis and underlying capsule is developed bluntly, and the glenohumeral joint line is identified. With the shoulder in neutral rotation, a vertical capsulotomy is made in the glenohumeral joint; this may be extended with a medial horizontal incision (in the shape of a sideways “T”) for improved exposure of the anterior-inferior glenoid. With the shoulder internally rotated, a Fukuda or humeral head retractor is then placed into the glenohumeral joint. Exposure of the anterior-inferior glenoid neck is then performed via subperiosteal elevation or debridement of the scar tissue and prior bony Bankart fragments. The recipient bed on the glenoid is then decorticated until punctate bleeding is seen.
The coracoid process is then passed through the subscapularis split and its previously decorticated deep surface is approximated to the anterior-inferior glenoid neck. Care is made to position the coracoid bone block precisely; lateral overhang may result in joint incongruity and subsequent degenerative arthrosis or pain. After the coracoid is positioned, the previously placed drill holes are identified. Through these holes, the glenoid neck is drilled anterior to posteriorly in the path of anticipated screw passage. Measurements are taken, and screw fixation of the coracoid process to the glenoid is achieved with 3.5- or 4-mm screws (Fig. 21-13). Screws are typically 34 to 36 mm in older adolescents, though the size will vary according from patient to patient. The lateral portion of the glenohumeral capsule is then reapproximated to the cuff of prior CA ligament still attached to the coracoid, completing a capsular reconstruction. Wound closure is performed in layers including pectoralis major repair, though the subscapularis split need not be closed. Patients are placed in a sling and swathe postoperatively (Table 21-6).
TABLE 21-6 Latarjet Reconstruction for Shoulder Instability


FIGURE 21-13 Intraoperative fluoroscopy images of the left shoulder following Latarjet reconstruction. A: Anteroposterior and (B) axillary projections depict screw fixation of the coracoid process, with care made not to lateralize the bone block.
Operative Treatment of Shoulder Dislocations: Arthroscopic Capsulorrhaphy
Indications/Contraindications
In patients with multidirectional instability which is painful and/or functionally limiting and has failed nonoperative treatment, arthroscopic capsulorrhaphy may be considered. As cited above, careful patient selection and preoperative counseling is critical, given the risk of recurrent instability and importance of postoperative therapy. Relative contraindications include patients with poorly controlled neuromuscular conditions, or those with cognitive or developmental delays limiting understanding and compliance with postoperative care.
Surgical Procedure
Preoperative Planning. Preoperative planning and equipment is similar to arthroscopic Bankart repair, as described above. MRI-arthrography is particularly useful, as it may demonstrate areas of capsular redundancy and guide selective capsulorrhaphy (Table 21-7).
TABLE 21-7 Arthroscopic Capsulorrhaphy for Shoulder Instability

Positioning. Arthroscopic capsulorrhaphy may be performed either in the lateral decubitus or modified beach chair positions. Given the need for circumferential access around the glenoid and glenohumeral joint, the addition of laterally directed distraction is useful. This may be facilitated with the use of lateral traction, commercially available arm holders, or placement of a bump beneath the axilla.
Surgical Approach(es). Similar to arthroscopic Bankart repairs, the procedure begins with examination under anesthesia to assess pathologic instability anteriorly, posteriorly, and inferiorly. After glenohumeral joint is insufflated with sterile saline solution, standard posterosuperior, anterosuperior, and anteroinferior arthroscopy portals are established. Viewing is traditionally performed from the posterosuperior portal, but moving the camera to the anterosuperior portal and establishing a posterior working portal will allow for improved visualization and circumferential access to the glenohumeral joint capsule.
Technique. Arthroscopic survey is performed to assess the extent of capsular patulousness and rule out unrecognized labral and/or bony pathology (Fig. 21-14). As plication of the posterior capsule is typically more challenging, direction is first turned to the posterior aspect of the shoulder. The arthroscope is placed in the anterosuperior portal and a working portal established posteriorly. The redundant capsule adjacent to the glenoid rim is prepared using arthroscopic rasps or shavers until punctate bleeding is seen, in efforts to stimulate a healing response; care is made to avoid overzealous tissue preparation, as the tissue is thin and undesirable rents in the capsule may be created. Following this, imbricating sutures may be placed, beginning in the most inferior aspect of the joint. Typically this is performed by passing a suture through capsular tissue approximately 1 cm from the labrum, and then passing the suture a second time from the capsule through the chondrolabral junction. (Prior biomechanical studies have demonstrated that sutures passed through the chondrolabral junction of patients with an intact labrum is as strong as suture anchors).342 This “pinch-tuck” suture will plicate the capsule when tied, reducing overall capsular volume. If knots are tied as the sutures are passed, the reduced capsular volume will often make subsequent suture placement more difficult; for this reason, consideration is made to pass all posterior sutures first before tying. After all posterior sutures are placed, they may be tied in sequential fashion from inferior to superior, completing the posterior capsulorrhaphy.


FIGURE 21-14 Arthroscopic capsulorrhaphy for multidirectional instability. A: Arthroscopic images depict redundant capsule (arrows), falling away from the glenoid rim and labrum. B: Tissue preparation may be performed with either rasps, shavers, or other devices to stimulate a bleeding response (C). D: Suture passing devices are used in a “pinch-tuck” fashion to imbricate the redundant tissue. E: Arthroscopic view after posterior plication sutures have been passed. F: After sutures have been tied, note is made of plication of the capsule and loss of the capsular redundancy.
The arthroscope is then repositioned posteriorly and an accessory portal reestablished anterosuperiorly. The anteroinferior capsule is similarly prepared with rasps, shavers, or other instruments until punctate bleedings is seen. Plicating sutures are again passed in a “pinch-tuck” fashion, imbricating the redundant capsule to the intact glenoid labrum. These may be tied in series, completing the circumferential repair (Table 21-8).
TABLE 21-8 Arthroscopic Capsulorrhaphy for Shoulder Instability

Operative Treatment of Shoulder Dislocations: Open Capsulorrhaphy
Indications/Contraindications
Despite advances in arthroscopic surgical techniques, open soft tissue procedures may still be performed. Relative indications for open capsulorrhaphy include failed prior arthroscopic procedures, multidirectional instability in setting of capsular laxity without labral tear, and surgeon preference and/or experience. The principles of these procedures are similar to arthroscopic plication: Stability is conferred by tightening the redundant capsule, thus reducing joint volume and conferring stability.
Surgical Procedure
Preoperative Planning. Preoperative planning similar to procedures described above (Table 21-9).
TABLE 21-9 Open Capsulorrhaphy for Shoulder Instability

Positioning. The modified beach chair position is utilized. Intraoperative positioning is aided by a limb holder.
Surgical Approach(es). A standard deltopectoral approach is utilized, with the skin incision beginning just lateral to the coracoid process and extending within Langer skin lines toward the axillary crease. The cephalic vein is typically retracted laterally with the deltoid. After the clavipectoral fascia is excised, the conjoined tendon is carefully retracted medially to avoid excessive traction to the musculocutaneous nerve. This will allow direct visualization of the subscapularis and underlying glenohumeral joint capsule.
Technique. After the subscapularis is exposed, the limb is placed in adduction and external rotation. The lesser tuberosity is palpated and identified. A subscapularis tenotomy may then be performed 2 to 3 cm medial to its insertion on the lesser tuberosity, leaving a cuff of tissue laterally to allow for subsequent repair. Traction sutures are placed on the subscapularis tendon, which may then be mobilized and separated from the underlying glenohumeral joint capsule. (In some situations, the upper two-thirds of the subscapularis may be divided, leaving a portion of the inferior musculotendinous unit intact.) Following this, T-shaped capsulotomy is created; a vertical incision is made laterally, with a subsequent transverse extension medially. The superomedial and inferomedial capsular flaps are then mobilized with suture tags. With the limb in the desired position of slight abduction and external rotation, the inferomedial limb is advanced and shifted superolaterally, repaired to the lateral capsule with multiple interrupted nonabsorbable sutures. The superomedial limb is then similarly advanced inferomedially and sewn to the lateral capsule, completing the capsulorrhaphy. Meticulous repair of the subscapularis tenotomy is performed with multiple braided nonabsorbable sutures. The subcutaneous tissues and skin are closed in layers, followed by application of a sling and swathe (Table 21-10).
TABLE 21-10 Open Capsulorrhaphy for Shoulder Instability

AUTHOR’S PREFERRED TREATMENT OF SHOULDER DISLOCATIONS
Children and adolescents with traumatic, anterior shoulder dislocations are treated with prompt closed reduction and sling immobilization. Radiographs are obtained to confirm adequacy of glenohumeral reduction and evaluate for possible bony glenoid fractures. In the majority of patients with purely soft tissue injuries—likely anterior-inferior labral tears—physical therapy is initiated following brief immobilization. Return to sports is limited until patients have restoration of motion, strength, and proprioception.8
Early in the post injury period, patients and families are counseled regarding the risk of recurrent instability. In high-risk patients (e.g., contact or overhead athletes) or patients for whom the risk of recurrent instability is judged to be unacceptable, arthroscopic Bankart repair may be performed after primary dislocation. In rare circumstances where patients wish to continue with high-risk activities despite known risk of recurrent instability (e.g., in-season contact athlete), functional bracing with orthoses limiting abduction and external rotation may be utilized.
Patients with bony Bankart lesions are further assessed with CT, and quantification is made of glenoid deficiency. Given the high risk of recurrent instability in the setting of glenoid bone loss, patients with small marginal lesions are offered arthroscopic repair. Patients with larger bony glenoid lesions are treated with open reduction and internal fixation (ORIF) versus Latarjet reconstruction, depending upon the integrity of the bony fragment.
Surgical stabilization of adolescents with recurrent unidirectional instability is typically performed via arthroscopic capsulolabral repair. Preoperative imaging with MRI-arthrography will better define the extent of labral injury and rule out unrecognized or attritional glenoid insufficiency. Latarjet reconstructions are performed in cases of glenoid bone loss or recurrent instability failing prior arthroscopic stabilizations.
Patients with atraumatic multidirectional instability in the setting of ligamentous laxity or other systemic conditions (e.g., hypermobility, Ehlers–Danlos, etc.) are treated with physical therapy, emphasizing strength, proprioception, biofeedback, and neuromuscular retraining of the entire shoulder girdle. In select patients where there is persistent, painful or functionally limiting instability refractory to or precluding physical therapy, surgical treatment is considered. MRI-arthrography is obtained to characterize the extent and magnitude of capsular redundancy. Stabilization is performed via arthroscopic capsulorrhaphy, with appropriate postoperative immobilization and therapy (Fig. 21-15).

FIGURE 21-15 Proposed treatment algorithm for shoulder dislocation.
Postoperative Care
Postoperatively, patients are sling immobilized for 4-week postoperatively. During the third and fourth postoperative weeks, patients initiate pendulum exercises only. Formal supervised physical therapy is begun after the fourth postoperative week, limiting forward flexion and lateral abduction in the plane of the scapula to 90 degrees and external rotation to 30 degrees. After the sixth postoperative week, motion and strengthening are advanced as tolerated. Sports participation is generally limited for 6 months postoperatively, provided full motion and strength has been restored.
Potential Pitfalls and Preventative Measures
Potential pitfalls in the diagnosis and management of shoulder dislocations are described above. In general, early recurrent instability after nonoperative or surgical treatment is generally due to failure to recognize the pertinent pathoanatomy. Careful radiographic evaluation after primary or recurrent instability events is needed to recognize bony glenoid deficiency and guide appropriate management. Early recurrent instability after arthroscopic soft tissue procedures may be due to unrecognized glenoid deficiency, suboptimal mobilization and preparation of the capsulolabral tissue, untreated HAGL lesions, or technical errors in suture passage and knot security. Finally, recurrent instability after capsulorrhaphy for multidirectional instability may be due to unrecognized systemic connective tissue disorders, suboptimal tissue preparation and plication, or inappropriate patient selection (Table 21-11).
TABLE 21-11 Potential Pitfalls and Strategies for Prevention

Treatment-Specific Outcomes
As noted above, there is limited published information regarding the results of surgical stabilization for glenohumeral instability in children and adolescents. Much of the current understanding of the treatment outcomes is derived from applications of the adult experiences. A number of general observations may be gleaned from review of the existing retrospective case series. First, there has been an increase in the incidence of glenohumeral instability in younger patients, perhaps because of increasing activities and younger age of first sports participation, with expectation for high recurrence rates with nonoperative treatment alone.100,149,189,420 Second, arthroscopic repairs have become increasingly common and preferred over open stabilization procedures.275,349 Third, surgical stabilization of Bankart lesions safely and effectively improves shoulder stability, with the risk of recurrence reduced to 5% to 20%.1,61,247 Castagna et al.61 reported the results of 65 patients between 13 and 18 years of age, treated with arthroscopic capsulolabral repair, all of whom were overhead or contact athletes. At mean 5-year follow-up, shoulder motion was restored and 81% had returned to their preinjury level of sports participation. Recurrent instability was reported in 21%, and recurrence was associated with choice of sports participation. In a report of 32 arthroscopic stabilizations in 30 patients under 18 years of age, Jones et al.214 similarly reported high functional outcomes, though recurrent instability was noted in 12% to 19% of patients. Finally, bony procedures including the Latarjet coracoid transfer is safe and effective, with low risk of recurrent instability.21,191,193
MANAGEMENT OF ADVERSE OUTCOMES AND UNEXPECTED COMPLICATIONS RELATED TO SHOULDER DISLOCATIONS
Adverse outcomes and complications occur infrequently with glenohumeral instability. As noted above, vascular injury is exceedingly rare, and the majority of neurologic injuries associated with traumatic dislocations represent neurapraxic traction injuries to the axillary nerve or brachial plexus, with expectation of spontaneous resolution over time. Nerve repairs or reconstructions are rarely needed and reserved for patients who fail to demonstrate progressive spontaneous recovery.
Chondrolysis has been increasingly reported in patients undergoing arthroscopic stabilizations for glenohumeral instability. Recent reports suggest that use of intra-articular analgesics (e.g., indwelling intra-articular pain catheters) are associated with chondrolysis, and for this reason are currently contraindicated.377,382,403,457 Similarly, unexpected joint degeneration has been reported after thermal capsulorrhaphy and loose metallic suture anchors, likely related to thermal injury and third body wear of the articular cartilage, respectively.82,107,150,216 Cartilage loss in a young, skeletally immature shoulder is a disastrous and yet unsolved complication. Avoidance of excessive heat and proper placement of bioabsorbable suture anchors may minimize these adverse events. Judicious placement of bone grafts and internal fixation, such as in the Latarjet procedure, is also critically important to minimize risk of early arthrosis (Table 21-12).192
TABLE 21-12 Shoulder Dislocations

SUMMARY, CONTROVERSIES, AND FUTURE DIRECTIONS RELATED TO SHOULDER DISLOCATIONS
In summary, glenohumeral instability is common in children and adolescents. While closed reduction is easily performed after acute dislocations, there is a high risk of recurrent instability. In appropriately selected patients, arthroscopic or open soft tissue and/or bony stabilization procedures are safe and effective.
There is ongoing debate and controversy surrounding the indications for surgical stabilization after primary traumatic dislocation in the child or adolescent. Proponents of primary surgery point to the safety and efficacy of predominantly arthroscopic procedures in reducing recurrence risk and restoring stability and return of function. Furthermore, there is some evidence suggesting recurrent dislocations may lead to more extensive labral tears, development of glenoid insufficiency, and even arthrosis.190,219 Many argue that surgical stabilization should be performed in higher-risk patients (e.g., young athletes involved in contact sports).67,233 A recent expected-value decision analysis supports primary arthroscopic stabilization if recurrence risk above 32% and utility value of surgical intervention remains above 6.6.33 Further investigation of the natural history of recurrent glenohumeral instability as well as prospective randomized trials of surgical versus nonoperative treatment is needed in the pediatric patient population.
Finally, as more information regarding the frequency and clinical significance of bony glenoid and humeral head defects becomes available, clarification of the indications for bony augmentation procedures (e.g., coracoid transfer, bone grafting) is needed. This is particularly relevant given the persistent risks of recurrent instability after arthroscopic Bankart repairs and the promising longer-term studies regarding the results of bony procedures.75,191,193,210,227
INTRODUCTION TO PROXIMAL HUMERUS FRACTURES
Proximal humeral fractures are relatively uncommon injuries, with an estimated annual incidence of 1.2 to 4.4 per 1,000, and representing less than 5% of all childhood fractures.26,182,203,240,241,358,464 Given the metaphyseal location, thick periosteum, and proximity to the proximal humeral physis, there is tremendous healing and remodeling potential of proximal humerus fractures. Furthermore, given the robust, near universal motion about the glenohumeral joint, little functional impairment may be seen even in cases of considerable bony malalignment. For these reasons, most proximal humeral fractures are amenable to nonoperative treatment.
ASSESSMENT OF PROXIMAL HUMERUS FRACTURES
Mechanisms of Injury for Proximal Humerus Fractures
Proximal humerus fractures occur through a number of characteristic injury mechanisms. Birth-related fractures of the proximal humerus are not uncommon.250,397 In general, hyperextension and/or rotational forces imparted on the upper limb during labor and delivery result in failure through the proximal humeral physis or metaphysis (Fig. 21-16).95,155,163,167,250,272,397 Risk factors include difficult delivery, macrosomia, and breech presentation, but are not entirely predictive.56,136,212,397 Indeed, proximal humerus fractures may occur during vaginal delivery of infants of all weights and sizes, implicating other maternal and perinatal factors.

FIGURE 21-16 Hyperextension or rotation of the ipsilateral arm may result in a proximal humeral or physeal injury during birth.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


