The number of individuals with disabilities participating in athletics, either in competition or for recreation, continues to increase, as technology improves to allow participation. As of 2014, it is estimated that about 2 million individuals with disabilities participate in recreational sports [1]. The growth of the Paralympic Games, from 16 participants in 1948 to greater than 4000 in 2012, reflects the larger overall growth in participation [2]. As participation continues to increase, it is important that medical providers become comfortable managing the acutely injured adaptive athlete on the field and in a medical setting. These athletes incur many of the same emergent injuries that other athletes suffer from, such as overuse musculoskeletal injuries, extremity fractures, traumatic brain injury, heat illness, and cardiac disease. There are also unique injuries to these athletes based on their disability and their sport of competition. The provider caring for these individuals must be comfortable with the basic principles of evaluation and management of acutely injured individuals. They need to also be mindful of the unique injuries and factors that should be considered when managing the individual athlete, with their specific disabilities. This chapter will discuss a basic approach to emergency care, placing special emphasis on the aspects of care that make these individuals unique.
Emergency Department Care
The initial approach to any patient evaluated in the emergency department starts with the assessment of the patient’s airway, breathing, and circulation (A, B, Cs). The remainder of this chapter will go through the specifics of evaluating each one of these systems. Using this systematic approach reminds the provider to pay particular attention to the critical life-enabling systems initially, without being distracted by more peripheral injuries that may not carry the same immediate mortality risk. Any disorder detected during this primary survey should be immediately addressed before proceeding forward with the survey. Assessment of the A, B, Cs is followed, naturally, by D—evaluation of neurologic disability—and E exposing the patient. This initial primary evaluation of the patient should be followed by a systematic and thorough secondary head-to-toe evaluation, looking for signs of injuries that may not be immediately apparent on the primary survey.
After establishing the stability of the patient, it is important to gain as much information about the mechanism of injury as possible. This information alerts the provider to have a higher index of suspicion for certain injuries that follow a certain mechanism of injury. Family, coaches, and EMS who were at the scene may be great additional resources to get an understanding of the injury. This history should also include general health information such as comorbid conditions, medications, prior injuries, extent of prior disability, and allergies, as this will affect your work-up and treatment plan.
It is important to get an initial set of vital signs to assess for the stability of the cardiopulmonary and thermoregulatory status of the injured or ill athlete. Many of these will be part of the primary survey—respiratory rate (RR) and oxygen saturation during the assessment of the patient’s breathing and blood pressure and heart rate during the circulatory evaluation. It is important to obtain the injured athlete’s temperature, including a rectal temperature if the athlete is altered or you have a high suspicion for heat-related or cold-related illness. According to a 2002 review, rectal temperature remains the most accurate way of measuring core temperature in the athlete [3]. Especially in the altered or confused patient, consider finger-stick glucose as an additional vital sign. Failure to recognize and respond to hypo- or hyperglycemia may cause poor outcomes for the patient. Remember to get a new set of vital signs if there is any change in clinical condition or any significant intervention was done.
In any acutely injured patient, it is important to obtain intravenous (IV) access for laboratory testing, administration of intravenous contrast for imaging, medication administration, and intravenous fluid rehydration. While a single IV may be sufficient in many patients, in a hypotensive patient or one who is acutely ill, two large bore IVs may be required for adequate resuscitation. If unable to provide access via an IV line, intraosseous access is an alternative method to provide medication and resuscitation fluids to patients.
Airway
The assessment of an acutely ill or injured individual should begin with the determination if the patient has a patent and protected airway. A patent-protected airway is necessary for oxygenation and ventilation, as well as to prevent aspiration of gastric contents. It is important to first observe for anatomic deviations that may cause mechanical obstruction of the airway, such as a large neck hematoma or posterior displacement of a fractured maxilla and midface. Further evaluation should be completed to assess the functionality of the airway. A quick approach that is recommended to determine if the airway is patent is to have the patient verbally respond to a question. This simple response informs the provider that the patient (1) has no upper airway obstruction, allowing them to transmit air through the vocal cords, and (2) has a high enough level of consciousness to listen, integrate data, and give an appropriate response. This approach is not appropriate for the hearing impaired or individuals who are nonverbal at baseline secondary to a previous stroke or intellectual/social impairment. Another reliable indicator of a patent airway is the patient’s ability to swallow their own secretions. A patient with pooling secretions in the airway, copious drooling, or gurgling respirations is not maintaining a patent airway and may need urgent intervention to establish one. Additionally, the provider can listen for stridor, which may indicate an upper airway obstruction or vocal cord dysfunction. Historically, the absence of a gag reflex has been described as an indicator of someone failing to maintain an airway. However, 12–25% of normal adults have an absent gag reflex, making this technique less useful than the other’s previously discussed [4].
Patients with cerebral palsy, or other neurologic disorders affecting the brainstem, may have diminished airway reflexes at baseline. It is important to keep this in mind and minimize any aspiration risks [5]. With cerebral palsy affecting muscles of movement, posture, and swallowing, approximately 90% of patients with CP have some degree of oropharyngeal dysphagia. This inability to consume sufficient food and fluids safely can lead to respiratory complications and has a direct correlation with the severity of gross motor skill function [6].
The first step in helping to keep the airway patent is to have the patient in a neutral airway position, such as the “sniffing position.” Lifting the chin superiorly places the neck in a slightly extended position placing the upper airway into a more neutral open alignment (Fig. 6.1) [7].


Fig. 6.1
Lifting chin to place in sniffing position and open airway
In the past for helmeted and padded athletes, the recommendations were always to leave equipment on for transport and to access the chest or face by removing only the front of the pads or face mask, respectively [8]. Recently, recommendations have advised that prehospital providers or sideline physicians can and in some cases should remove helmets and other protective equipment prior to transport to a primary emergency facility [9]. Recent research has demonstrated basic life-support skills including chest compressions and ventilations may be compromised in the setting of athletic equipment [10]. However, this is still a very controversial topic, and equipment removal needs to be done in the hands of an experienced provider. If there are ample prehospital and experienced physician providers on the sideline and the equipment can be safely removed, then this would be the recommendation. Otherwise, waiting until after transport, especially if there are no life-threatening injuries, should be considered.
The jaw thrust maneuver helps to prevent posterior deviation of the tongue into an obstructing position in the oropharynx. Moving the angle of the mandible anteriorly lifts the base of the tongue forward and away from the posterior oropharynx, without the manipulation of the cervical spine that can occur with the head tilt-chin lift. The helmet has been cited as complicating jaw thrust maneuvers or providing bag-valve mask placement for ventilations, along with the chin strap obstructing a proper seal for the mask [11].
In addition to opening the airway with jaw thrust, it is important to look into the airway for any source of obstruction: a mouth guard, gum, a displaced tooth, etc. It is no longer recommended to perform a blind sweep of the oropharynx; but if an obstructing object is visually identified, using a finger sweep or forceps to remove an obstructing object is definitely indicated.
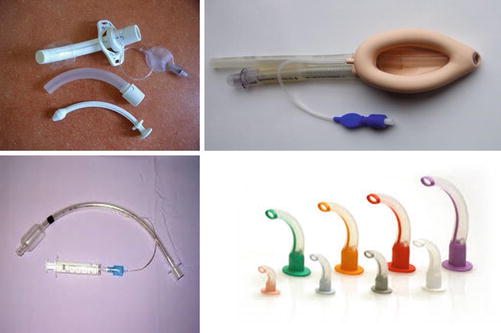
If these maneuvers are not sufficient to maintain a patent airway, or the provider suspects that the patient’s clinical condition may continue to deteriorate, it may be necessary to provide an airway adjunct to maintain patency. A nasopharyngeal airway may be placed in a sedated or awake/alert patient to allow oxygenation/ventilation past an oropharyngeal obstruction. Note that this technique is contraindicated for a patient with a suspected midface fracture. An oropharyngeal airway can also be used in this matter but will not be tolerated in the awake patient. Ultimately these techniques are temporizing maneuvers. Patients that require this level of intervention will likely need to have an advanced airway placed that is secured allowing oxygenation/ventilation while protecting the patient from aspiration of gastric contents. Supraglottic airway devices can be placed quickly using a blind technique. These devices provide an airway until a definitive secure airway can be established safely. Placement of an endotracheal tube using a rapid sequence intubation (RSI) technique should be attempted when it is clear that the patient will need prolonged airway or ventilatory support. The patient’s hemodynamic and oxygenation level should be optimized prior to any intubation attempt, unless the patient is acutely declining and not able to be oxygenated or ventilated with bag-valve mask and adjunct airway ventilation (Fig. 6.2) [12].