Congenital Mitral Valve Disease
Janette F. Strasburger
The left atrioventricular valve (mitral valve) includes the anterior and posterior mitral valve leaflets separated by their commissures, the chordae tendineae, and the anteromedial and posterolateral left ventricular papillary muscles. The annulus, or skeletal support of the mitral valve, is fibromuscular and contracts with the heart. The mitral valve permits egress of blood during diastole and atrial systole from the left atrium to the left ventricle and prevents reflux of blood into the left atrium during ventricular systole. Thus, closure of the mitral valve is the earliest component of the first heart sound. Abnormalities in the development of the mitral valve apparatus can result in hemodynamic alterations in blood flow, which can present with either congestive heart failure or pulmonary edema during fetal, neonatal, or later development.
Most abnormalities of the mitral valve are associated with other congenital cardiac defects, such as atrioventricular septal defects, and are not isolated mitral abnormalities. When isolated mitral abnormalities occur in the pediatric age group, they usually are acquired as the result of rheumatic carditis, myocardial ischemia or infarction, hypertension, Marfan syndrome, mitral valve prolapse syndrome, bacterial endocarditis, myocarditis, or cardiomyopathy. Congenital mitral valve abnormalities are much rarer. Because of the severity of obstruction of flow across the valve, valvular regurgitation, or associated cardiac defects, patients with congenital mitral abnormalities often present during infancy. Congenital lesions of the mitral valve are listed in Table 278.1.
Other abnormalities of the pulmonary veins or left atrium also can cause obstruction of left ventricular filling or pulmonary venous egress proximal to the mitral valve. They include the following: cor triatriatum, a perforated fibromuscular membrane that subdivides the left atrium; supravalvar stenosing mitral ring, a fibrous, shelflike ridge just above the mitral valve that encroaches on its orifice; left atrial tumor; and unilateral or common pulmonary venous stenosis or atresia. All these lesions can result in pulmonary edema and right-sided cardiac failure secondary to obstructed left-sided flow and pulmonary hypertension.
TABLE 278.1. CONGENITAL ABNORMALITIES OF THE MITRAL VALVE APPARATUS | ||||||||
|---|---|---|---|---|---|---|---|---|
|
CONGENITAL MITRAL STENOSIS
Mitral valve stenosis presents clinically with right-sided cardiac failure and pulmonary hypertension. The age at presentation depends on the degree of obstruction of left atrial emptying. Because exercise demands greater cardiac output, initial symptoms often are related to exercise. In infants, feeding requires increased cardiac output, and babies often present with dyspnea or cyanosis during feeding and with failure to grow. Because of pulmonary edema, infants and children are at risk for having recurring respiratory infections. Tachypnea, hemoptysis, respiratory distress, low cardiac output, and atrial fibrillation can be associated findings of mitral stenosis. Atrial fibrillation and left atrial thrombi are relatively uncommon occurrences in children; however, if atrial fibrillation is observed, the presence of intracardiac thrombi must be excluded before cardioversion.
The physical examination in mitral stenosis is characterized by a right ventricular lift at the left lower sternal border and by an increased pulmonary component of the second heart sound caused by pulmonary hypertension. A fourth heart sound sometimes is audible secondary to enhanced atrial systolic contraction. A long pandiastolic murmur often is audible
at the cardiac apex. The chest radiograph usually shows left atrial enlargement, with widening of the angle between the left and right main bronchi. In older children, a redistribution of blood flow can be seen, with increased flow to the upper lobes. Kerley B lines and pulmonary edema also are present. Generally, the electrocardiogram shows left atrial or biatrial enlargement during sinus rhythm, and, rarely, atrial fibrillation is present. Right ventricular hypertrophy with right axis deviation generally is seen. Two-dimensional and Doppler echocardiography studies determine the presence of mitral stenosis by measuring the cross-sectional area of the valve and its flow gradient, and they detect structural abnormalities of the mitral valve or supporting apparatus. The left atrial size often is enlarged, but the left ventricular volume usually is 70% to 100% of normal. Transesophageal echocardiography, which allows excellent imaging of the left atrium and mitral valve when the patient is under sedation or general anesthesia, frequently is used to provide specific anatomic and Doppler detail and can be an adjunct to cardiac catheterization and surgical valvuloplasty procedures or before cardioversion. Cardiac catheterization usually is reserved for situations in which the echocardiographic diagnosis is unclear or associated defects are present. Cardiac catheterization demonstrates elevation in pulmonary arterial pressure and right ventricular systolic pressure. A gradient between the left atrial A wave and the left ventricular end-diastolic pressure exists. Often, estimating the left atrial pressure using pulmonary capillary wedge pressure or entering the left atrium via transseptal puncture is necessary. Injections in the pulmonary artery or left atrium usually demonstrate abnormalities of the mitral valve or adjacent structures.
at the cardiac apex. The chest radiograph usually shows left atrial enlargement, with widening of the angle between the left and right main bronchi. In older children, a redistribution of blood flow can be seen, with increased flow to the upper lobes. Kerley B lines and pulmonary edema also are present. Generally, the electrocardiogram shows left atrial or biatrial enlargement during sinus rhythm, and, rarely, atrial fibrillation is present. Right ventricular hypertrophy with right axis deviation generally is seen. Two-dimensional and Doppler echocardiography studies determine the presence of mitral stenosis by measuring the cross-sectional area of the valve and its flow gradient, and they detect structural abnormalities of the mitral valve or supporting apparatus. The left atrial size often is enlarged, but the left ventricular volume usually is 70% to 100% of normal. Transesophageal echocardiography, which allows excellent imaging of the left atrium and mitral valve when the patient is under sedation or general anesthesia, frequently is used to provide specific anatomic and Doppler detail and can be an adjunct to cardiac catheterization and surgical valvuloplasty procedures or before cardioversion. Cardiac catheterization usually is reserved for situations in which the echocardiographic diagnosis is unclear or associated defects are present. Cardiac catheterization demonstrates elevation in pulmonary arterial pressure and right ventricular systolic pressure. A gradient between the left atrial A wave and the left ventricular end-diastolic pressure exists. Often, estimating the left atrial pressure using pulmonary capillary wedge pressure or entering the left atrium via transseptal puncture is necessary. Injections in the pulmonary artery or left atrium usually demonstrate abnormalities of the mitral valve or adjacent structures.
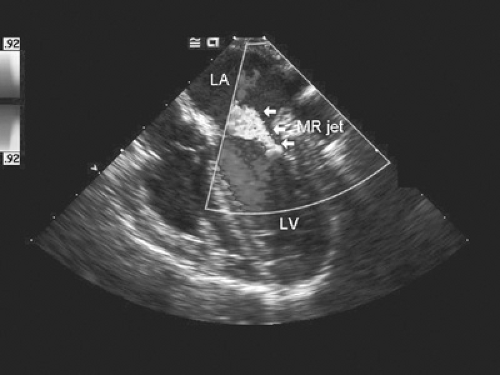 FIGURE 278.1. Mitral regurgitation. The mitral regurgitation jet (MR jet, arrow) is noted as a light colored flame directed into the left atrium (LA) from the left ventricle (LV) during systole.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|




