FIGURE 4-1 Examples of dermatitis related to wet casts. A: A soiled hip spica cast. B: Upper extremity cast that was wet. (Property of UW Pediatric Orthopaedics.)
Thermal Injury
Plaster and fiberglass, the two most common casting materials, harden through exothermic chemical reactions. Plaster has a much higher setting temperature than fiberglass and therefore a higher risk for thermal injury when a cast is placed. Two factors strongly associated with thermal injuries are dip water temperature and the thickness of cast material. Several studies have shown that risk of thermal injury is significant if the dip water temperature is too hot (>50°C) or if the casts are too thick (>24 ply).39,46,61 Each plaster manufacturer has recommended dip water temperatures that should not be exceeded. Using warmer temperatures to “speed up” the setting time beyond those recommended should be avoided. Casts in excess of 24 ply are rarely encountered; however, increased amounts of casting material are often placed in the concavities of extremities (antecubital fossa and dorsum of the ankle) because of material overlap.46 Incorporating splints on the convexity thus decreasing overlap in the concavity can minimize this. Similarly, clinicians placing plaster splints of 10 to 15 ply on an extremity may breech safe thicknesses when the splint is too long and the edges are folded over thus creating a focal area of 20 to 30 ply, a thickness at which temperatures do become a risk.46 Studies have shown that temperatures high enough to cause significant thermal injuries can also be reached when the clinician places a curing cast on a pillow. 39,46 The practice of reinforcing a curing plaster cast with fiberglass may place the limb at significant risk because the synthetic overlap prevents heat from effectively dissipating, as well as an increased risk of case burns at removal in our experience. The plaster must be allowed to cure before setting the casted limb on a support or applying fiberglass reinforcement. Failure to wait may place the insulated portion of the limb at significant risk.46 Case reports demonstrating this potential complication do exist.9 Those patients undergoing regional or general anesthesia may be at increased risk as they will not report thermal injury.
Areas of Focal Pressure—Impending Pressure Sores
A key to preventing loss of fracture reduction is in the application of a well-molded cast. “Well molded” means casts should closely mimic the limb they are immobilizing. Cast padding should be applied between 3 and 5 layers thick over the limb being casted.71,88 Bony prominences and cast edges should be additionally padded to prevent irritation yet allow a cast to be molded to fit snugly without undue pressure. The heel, malleoli, patella, ASIS, and olecranon, are areas that may require additional padding. The use of foam padding in such areas may help decrease the incidence of pressure sores.35
If areas of increased pressure are formed, they may lead to foci of decreased perfusion and result in pressure sores. Similarly, great care should be taken in preventing a change in limb position between application of the cast padding and the casting material. A common example is a short leg cast applied in less than 90 degrees of ankle flexion; if the ankle is flexed to 90 degrees during the application or curing of the cast, the material will bunch up and will impinge on the dorsum of the ankle.
Families and patients should be instructed to refrain from placing anything between a cast and the patients’ skin. Often this is done to alleviate pruritus but should be avoided as inadvertent excoriation may occur. Despite these warnings, food, toys, writing utensils, money, and other items have been found down casts, and we have seen them erode through patients’ skin. Numerous case studies report problems from foreign bodies placed down casts.12,94 Any patient with a suspected foreign body down their cast should have the cast removed and skin inspected (Fig. 4-2).

FIGURE 4-2 Examples of foreign bodies found under splints/casts. A: A bracelet that was not removed prior to immobilization. B: A plastic knife which was found down a lower extremity cast. C: A coin found down a long-arm cast. D: A toy tank found under a cast. (Property of UW Pediatric Orthopaedics.)
A loose cast may result in a loss of reduction or skin sores as a result of shear forces repeatedly applied to the limb. One may rationalize that the best way to avoid pressure sores is to increase the amount of padding under the cast. Injudicious application of excessive padding can lead to a cast that is too loose and paradoxically increase the risk of skin irritation from sheer stress at the skin/padding interface. Loose-fitting casts can be further associated with fracture malunion because of loss of reduction.48 In such cases, the distal fingers or toes are often noted to “migrate” proximally when this occurs and should alert the parent and the clinician that there is a problem. This has been termed the “disappearing toes/fingers sign.”99 It is during this migration that pressure sores may occur as the limb migrates proximally in a fixed cast. This causes a mismatch in the shape of the cast and the shape of the limb. In a lower extremity cast, which migrates distally, the dorsum of the foot receives pressure from the anterior ankle crease of the cast, while the heel is pulled up and rests along the posterior calf portion of the cast. Prolonged positioning in such a manner may result in pressure sores.
Detecting Cast Complications
That “there are no hypochondriacs in casts” is an important aphorism to remember and every effort should be taken to resolve the source of complaint in an immobilized patient. Any reports of casts getting wet, soiled, or questionable foreign bodies being lost down casts should be taken seriously and the patient evaluated in a timely manner. A complication of casting should be considered whenever an immobilized patient has an unexplained increase in pain, irritability, or unexplained fevers.25
Some cast complications such as soiling and wetness can be detected on physical examination, whereas others may be more difficult to diagnose. A foul-smelling cast may be a sign of wound infection and the cast should be removed or windowed to be inspected the source of the smell. Pressure sores may be diagnosed if the patient can localize an area of discomfort away from the fracture or operative site. Complaints of pain in high-risk areas such as the heel, dorsum of the foot, popliteal fossa, patella, olecranon, must alert the clinician of an impending problem. However with pediatric patients, localization may not be possible. One must correlate history, the clinical examination findings, such as the “disappearing toes sign” with radiographs. These images can be used to critically evaluate not only the alignment of the fractured bone, but also the outline and contour of the cast padding and material, especially in the antecubital, the popliteal fossae, and over the dorsum of the foot. If there is a suspicion of a problem, the cast should be windowed or removed and the area inspected.
Certain pediatric patients may be at a higher risk for cast complications. These include patients with an inability to effectively communicate. The very young, developmentally delayed, or patients under anesthesia or sedation may have difficulty responding to noxious stimuli such as heat or pressure during the cast application. Discerning problems in this group may be quite difficult and cast sores can occur despite appropriate and careful application.
Similarly, patients with impaired sensation are at increased risk for injuries related to excessive heat and pressure. In this group are those with spinal cord injuries,80,89 myelomeningocele,66 and systemic disorders such as diabetes mellitus.43 Furthermore, prolonged immobilization in many of these marginally ambulatory patients will potentiate existing osteopenia, thus, increasing the risk of fractures and need for further immobilization.
Patients with spasticity are also at increased risk for complications. Often these patients have multiple risk factors including communication difficulties and poor nutrition in addition to their spasticity. These factors place them at particular risk for developing pressure sores.63,91
Treating Cast Complications
Dermatitis
The majority of dermatitis under casts has to do with maceration of the skin and continued contact with wetness including fluids such as urine or feces. Often removal of the cast, cleansing of the skin, and allowing the skin to “dry out” is all that is required. Some recommend applying over-the-counter skin moisturizers.27 If fungal infection is suspected, half-strength nystatin cream and 1% hydrocortisone cream may be applied followed by miconazole powder dusting twice daily.27 If unstable, the fracture may be managed by a newly applied dry split cast or splint allowing time for the skin to recover. In rare cases internal or external fixation may be chosen to manage the fracture and to allow treatment of the skin issues. Often the skin will improve dramatically after a few days and a new cast may be applied. If significant concern for cellulitis exists, such as induration or fevers, laboratory tests should be ordered and empiric oral antibiotics prescribed.
Pressure Sores
Pressure sores are the result of a focal area of pressure, which exceeds perfusion pressure. Although there may be initial pain associated with this pressure, this can be difficult to separate from the pain of the fracture or surgery. Any pain away from the injured area should be suspected to have a problem with focal pressure. The heel is the most common site. These sores may vary from areas of erythema, to black eschars, to full thickness soft tissue loss and exposed bone (Fig. 4-3). In the benign cases removal of the cast over the heel and either cessation or careful reapplication is all that is necessary. Typically black eschars imply partial to full thickness injuries. If they are intact, nonfluctuant, nondraining, and mobile from the underlying bone they may be treated as a biologic dressing with weekly wound checks. If any concern exists, a “Wound Team” and/or Plastic Surgery consult should be sought earlier rather than later. Often dressing changes utilizing topical enzymatic ointments and antibiotic ointments can be used to treat these wounds (Fig. 4-4). Whenever exposed bone is present, osteomyelitis is a concern requiring aggressive intervention and possible intravenous antibiotic therapy. In these severe cases vacuum-assisted closure (VAC) therapy, skin grafting, or flap coverage may be necessary.62
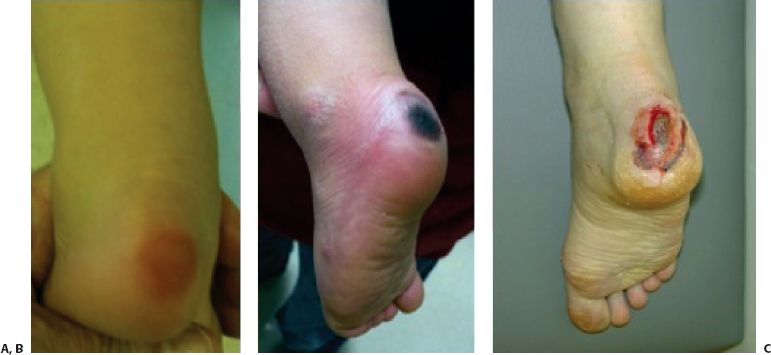
FIGURE 4-3 Examples of heel pressure sores. A: Mild erythema and superficial skin damage, (B) intact eschar, (C) partial/full thickness injury with exposed bone and fascia. (Property of UW Pediatric Orthopaedics.)

FIGURE 4-4 Picture of heel ulcer at clinical follow-up after operative debridement (A). After roughly 2 months of topical enzymatic and antibiotic treatment with dressing changes (B). (Property of UW Pediatric Orthopaedics.)
Joint Stiffness and Muscle Contractures
Determination of cast immobilization duration is often multifactorial; however, the clinician must recognize that unwanted physiologic changes occur. Although these changes are less pronounced in children than adults, excessive length of immobilization may lead to problems such as stiffness,33 muscle atrophy, cartilage degradation, ligament weakening, and osteoporosis.7,14,16,38,44,52,92 This must be weighed against the bony healing gained in prolonged immobilizations. Alternatives such as Pavlik harness bracing for infants with femur fractures,75 patellar tendon bearing casts versus long leg casts for tibial fractures, short-arm casts for distal forearm fractures, and other functional braces may minimize some of the risks of cast immobilization or at least decrease the duration of cast treatment.
The ankle, elbow, and fingers are often locations prone to stiffness. The duration of immobilization should be minimized if at all possible. In minimally displaced medial epicondyle and radial neck fractures, the limb should only be immobilized for 7 to 10 days until the patient is comfortable, but protected from further injury during activities such as contact sports for at least 3 to 6 weeks after the fracture. Similarly, once clearly established healing has occurred in supracondylar humerus fractures, the limb should be allowed motion after 3 to 4 weeks of casting. The position of immobilization is also important in the nearly skeletally mature. Placing the foot in plantar flexion, or failing to splint fingers in the safety position (70 degrees MCP flexion/IP extension) may result in joint contractures that persist long after fracture healing, though this is uncommon in young children.
Compartment Syndrome
Most limbs with fresh fractures are more comfortable after immobilization. Therefore, increasing pain or neurovascular change should be fully evaluated to detect above complications and possibly compartment syndrome. Fractures and surgery can result in progressive soft tissue swelling that might not have been present at the time of cast application and may lead to compartment syndrome. In this scenario,86 the first intervention should be relieving the circumferential pressure by splitting the cast and all underlying padding, as leaving the padding intact has been shown to not relieve compartment pressure. Should splitting the cast fail to alleviate symptoms, cast removal should be considered. Fractures of the tibia,34,42 forearm,42 and elbow have increased risk of compartment syndrome. High-energy fractures resulting from motor vehicle accidents,34 crush injuries,2 or two-level injuries such as a floating elbow, should raise the treating physician’s awareness to the possibility of an impending compartment syndrome. Any child unable to detect pain associated with compartment syndrome (a nerve injury or regional anesthesia)78 must be followed closely for the development of compartment syndrome.
Children do not usually exhibit the classical four Ps (pallor, paresthesias, pulseless, pain with passive stretch) associated with compartment syndrome until myonecrosis has occurred. Instead the three As of increased agitation, anxiety, and analgesic requirements have been documented as the earliest signs of compartment syndrome in children. Any child exhibiting these symptoms that are not relieved with cast splitting should have the cast removed and limb inspected with a high suspicion of compartment syndrome. One should be ready to take the child to the operating room for formal compartment evaluation and decompression if needed.
Fractures with associated neurovascular injuries are at significant risk of developing a compartment syndrome and require frequent neurovascular checks. These limbs may be stabilized with a splint as opposed to circumferential cast application; which could worsen the risk of compartment syndrome. These limbs are most often treated with operative stabilization using internal or external fixation and/or splint immobilization. This allows continued neurovascular assessment, palpation of compartments, and inspection of the limb. For instance, the child with a floating elbow fracture and associated nerve palsy (at high risk for compartment syndrome) is usually best treated with internal fixation of the fractures, and either a splint, bivalved cast that is easily opened, or cast with thick foam to allow for swelling, with the volar forearm exposed to assess the compartments as well as the pulses.
Disuse Osteopenia and Pathologic Fractures Adjacent to Cast
Patients with paralytic conditions or cerebral palsy patients and those taking anticonvulsants may experience further disuse osteopenia with immobilization.80,89 These patients are at significantly higher risk of pathologic fracture while casted or upon cast removal.3,63 Strategies to prevent this includes minimizing immobilization (<4 weeks), weight-bearing casts, and the use of less rigid immobilization such as Soft Cast (3M Healthcare Ltd, Loughborough, England) and splints and braces.
Delayed Diagnosis of Wound Infections
Many children are placed in postsurgical casts. The vast majority does well without incident. However, casts over wounds or pins may cause a delay in the diagnosis of a wound infection (Fig. 4-5). For instance, an estimated 1% to 4% of all pediatric supracondylar humerus fractures treated with pinning the elbow, will develop a postoperative pin tract inflammation or infection.5,33 Therefore, unexplained fever beyond the perioperative period, increase in pain at pin sites, foul smell, or discharge from a cast should be evaluated by a member of the orthopedic team. The wound should be examined either with cast windowing or cast removal. Laboratory tests including CBC, ESR, CRP are advisable. In cases of early pin site infection where the fracture is not yet healed, oral antibiotics may control the infection long enough to allow fracture healing. Infections of pins used for certain fractures may have a high chance of joint penetration (lateral condyle, distal femoral physeal, proximal humerus) and can lead to a septic joint. This is much more serious than simple pin site infections, and most often must be treated with surgical irrigation and debridement and pin removal should be considered.

FIGURE 4-5 After getting a postoperative cast wet, dermatitis and possible cellulitis were found at the incision following a gastrocnemius recession. (Property of UW Pediatric Orthopaedics.)
Types of Casting Materials
Before placing a cast, the limb must be inspected. Any dirt, operative skin prep, jewelry should be removed before the cast is applied. Often appropriate size stockinette or liner is applied against the skin, under the cast and cast padding. Although not essential, these liners minimize skin irritation; allow nice well padded and polished edges to the cast to be applied. They also minimize the tendency of some children to “pick out” their cast padding. These liners are made of cotton, water-friendly synthetic materials such as polyester, sliver-impregnated cotton (to minimize bacterial growth), and Gore-Tex (W.L. Gore & Associates; Newark, Delaware). Some in the care of children who require spica cast application favors water-permeable liners such as Gore-Tex. In addition to being more convenient for patients, these newer materials have been shown to minimize skin irritation.47,58,101
Cast Padding
Different materials are used to pad the extremity between the cast material and the patient’s skin. A thin layer (3 to 5 layers) of padding is applied to the portion of the extremity that is not prone to pressure sores and it is applied without wrinkles.71,88 Additional layers may be placed over bony prominences to minimize pressure in these areas. Cotton is the cheapest and is historically most commonly used. But casts with cotton padding cannot be made waterproof as the cotton padding retains water. Newer synthetic materials have variable water resistance and when paired with fiberglass can allow patients to bathe and swim. However, these materials are considerably more expensive than their cotton counterparts. In addition, some synthetic padding is less resistant to a cast saw. If one applies Gore-Tex (W.L. Gore & Associates; Newark, Delaware) padding, the blue DE FLEX safety strip (W.L. Gore & Associates; Newark, Delaware) can be placed along the path that the cast saw will take to remove the cast.
Cast edges are often a source of skin irritation and abrasion. This is especially true for fiberglass casts. When making a cast, applying the stockinette and cast padding at least 1 cm beyond the edge of the fiberglass, and folding the stockinette and padding back over the first layer of fiberglass, will make a cast with well-padded edges. Closed cell adhesive foam may also be applied to the edges of a cast and to pad bony prominences. It is important to recognize that some foam padding will accumulate moisture and will not be effectively wicked away from the liner and skin. Should difficulty be found in folding back the underlying stockinette or liner, the cast edges may be petaled with tape or moleskin adhesive. This involves placing a 1 to 2 in piece of tape on the inside of the liner and folding the taped liner over the opening of cast. Most commonly petaling is performed on hip spica casts, but may be performed on any cast.
Plaster of Paris
Plaster-impregnated cloth is the time-tested form of immobilization. It was first described in 1852 and has been the gold standard for cast immobilization for many years. This material is generally less expensive and is more moldable in comparison to the synthetic counterparts. The major advantages of plaster over synthetic materials in the prevention of cast sores and limb compression are its increase in pliability and its effective spreading after univalving. Inconveniences associated with plaster include its poor resistance to water and its lower strength-to-weight ratio resulting in heavier (thicker) casts.
Plaster of Paris combines with water in the following reaction:

In the process of setting up, the conversion to gypsum is an exothermic reaction with thermal energy as a by-product. In general the amount of heat produced is variable between each of the manufactured plasters. However, within each product line, faster “setting” plasters can be expected to produce more heat. As the speed of the reaction, amount of reactants, or temperature of the system (dip water and/or ambient temperature) increase; the amount of heat given off can cause significant thermal injury.39,46,61 The low strength-to-weight ratio may also increase risk of thermal injury as those unfamiliar with the amount (ply) of plaster to use may inadvertently use too much, resulting in a burn.
Fiberglass
More recently, synthetic fiberglass materials have been introduced. These materials have the benefit of being lightweight and strong. In addition these materials can be combined with waterproof liners to allow patients to bathe and swim in their casts. These materials are often more radiolucent allowing better imaging within the cast.
Risk of thermal injury is much lower and is a major advantage over plaster.46,76 However, because of the increased stiffness, some feel these casts are more difficult to mold, whereas others prefer fiberglass as the strength of the molded portion is greater. To prevent increased areas of pressure and constriction of the limb, special precautions are recommended when applying fiberglass rolls (see below).23 In addition, fiberglass is more expensive than plaster (2–2.5×). Finally, there may be a small long-term risk to those applying and removing these materials. Studies have disputed the carcinogenic risks in the manufacturing and use of fiberglass materials.37,93
Other Casting Materials
In addition to the standard rigid casting materials of plaster and fiberglass, a less rigid class of nonfiberglass synthetic casting material is available. Although less rigid than standard casting materials, this Soft Cast (3M Healthcare Ltd, Loughborough, England) has several potential advantages. Experimental studies have shown that this material is more accommodating to increases in pressure than the other casting materials.26 As this material is less rigid, it may be an ideal material to immobilize patients with severe osteopenia. Finally, this material can be removed without using a cast saw, which eliminates the risk of cast saw injury.10
Combination of Materials
Some combine plaster and fiberglass casting materials in hopes of obtaining the best features of both. One may reinforce a thin well-molded plaster cast by overwrapping it with fiberglass to increase its durability and minimize its weight. With this technique one must ensure that the plaster has set before overwrapping with the fiberglass. Failure to do so may result in a thermal injury.46 Shortcomings of this technique include the fact that the two layers of material may obscure fine radiographic detail. Finally, great care must be taken when removing such casts as it may be difficult to “feel” the depth of the cast saw blade and blade temperatures may be more elevated than usual. As a result of the increased risks of burns, it is especially important to use plastic protection strips under the cast when using a standard vibrating cast saw for cast removal. Yet despite these shortcomings, fiberglass has become the most popular casting material in most centers; this is because of the increased strength, decreased weight, improved radiographic quality, and ability to make water-friendly casts.
General Cast Application Principles
Optimal cast application in children requires cooperation, or at least compliance, an issue in younger children, or those with cognitive or behavioral issues, such as autistic-spectrum disorder, who often do not understand the rationale for cast application. Anxiety is further compounded by the presence of strangers, a chaotic environment, and, if applicable, pain. Controlling all of these factors increases the chances of an appropriately fitted cast.
While pain control and sedation are often required, other techniques are helpful for calming and distracting a child during cast application. Creating a calm environment begins with the first encounter with the child: Speak with a soft voice, sitting and placing oneself at a level at or below that of the child to present a less intimidating stature. Initial examination techniques should be soft and distant from the site of concern, progressing slowly to the area of concern. A less aggravated child prior to cast application more likely remains calm during cast application. Preparing casting materials outside of the room or out of direct visualization of the child during onset of sedation or distraction helps maintain a calm environment.
During cast application itself, a number of approaches may prove helpful, depending on the child. While some children are “attenders,” coping better when given more information and being talked through a procedure, others are “distractors” who do better with guided imagery and distraction techniques19,83; both types of children benefit from relaxation exercises. Talking to the child and his parents helps identify the best approach for an individual child, and use of child life specialists proves extremely helpful in implementing the preferred approach.17,84 Use of television/videos, games or interactive applications on a handheld device or tablet proves useful for most any age. For infants and toddlers, soft music, toys (especially those with lights or moving parts), and some interactive applications on handheld devices help with distraction and relaxation.65 When using a cast saw for cutting the cast or cast removal, ear protection helps decrease anxiety.13 For children with cognitive, behavioral, or autistic-spectrum disorders, discussion of possible approaches with the parents reaps rewards as they have the best sense of what will be calming, as well as stimulatory, for their child. Cast saws are now available that cut with a scissor-like mechanism that make very little noise and do not become hot. Use of these saws may reduce children’s anxiety.
In general, cast or splint application consists of several critical steps. (1) Understanding the injury and development of an appropriate treatment strategy. (2) Collection of all of the needed materials. (3) Assembling the team that is required to execute the process. (4) Education and preparation of the family and the patient. (5) Performing the reduction (if needed) and immobilization (cast or splint).
Once the treatment plan is identified; the key to successful cast application begins well before a cast or splint is applied. It is important to have ready and in easy access the needed padding (cast lining and stockinette); water (at appropriate temperature) cast material (plaster and fiberglass in rolls and reinforcing slabs) as well as needed instruments (C-arm imaging, scissors, cast saws, spreaders etc.). It is important that these are ready as cast application is a timely undertaking with materials that cure and harden in a short period and the application may depend on a short window of time available for comfort or sedation of the child. It is further recognized that all needed personnel need to be ready and this will ideally include sedation team and child life specialists in addition to the one to three people needed to apply a splint or cast.
Several important concepts need to be kept in mind when handling plaster of Paris. This material depends on excellent handling techniques to maximize the benefits of mold ability and fit and also to maximize strength. Each practitioner will have biases on how the art of cast application proceeds in their hands. Some like the plaster to be wet to mold better, others will like a drier roll to ease application (less slippery) and speed the curing process. Within these two extremes will be a consistency that is appropriate as the plaster roll is unrolled onto the limb. It is optimal to keep the plaster roll in contact to the limb to avoid wrapping the material too tight (Fig. 4-6). The plaster should be unrolled with overlaps of ½ to ¹∕³ the width of the roll and tucks are taken to avoid the tendency of pulling and stretching the material (thus increasing tightness) to get a good distribution and fit of the plaster around the difficult concave areas of the ankle, knee, elbow, and thumb. The optimal cast technique requires frequent rubbing and incorporation (termed: Initial molding) of the plaster rolls as the cast is being applied. Constantly rubbing the plaster as the cast is applied will improve the fit but will also flatten the tucks and incorporate the mineral portion of the plaster into the fiber mesh for optimal strength. Plaster splints should be dipped and vigorously molded together before applying to the convexity of the limb (back of elbow or ankle) or where additional strength is needed (anterior knee [long-leg cast] or posterior thigh [spica cast]).

FIGURE 4-6 Plaster roll is not lifted off of the cast but kept in contact during application as it is “rolled” up the extremity with an overlap of 30% to 50%. (Property of UW Pediatric Orthopaedics.)
Once the plaster cast is applied and the initial molding has been accomplished, the cast must be held in a manner that maximizes reduction and prevents possibility of pressure sores. For instance it is critical that a cast is supported by broad surfaces such as the palm of a hand; the thorax of the surgeon is an excellent broad surface to hold the plantar foot in neutral flexion and extension (Fig. 4-7). Holding a cast with the tips of fingers will leave indentations that can lead to pressure sores. If fingers are needed for molding, pressure should be applied and then withdrawn as the plaster reaches the final curing at which point “terminal” molding of the cast can be done. Terminal molding is that point at which the plaster is fairly firm and warm; yet can be gently deformed without cracking the plaster of Paris. This is the appropriate time to do the final mold and hold of fracture fragments. As the cast goes through the final curing process it can be supported on pillows, provided the cast is not too hot (the pillow prevents heat loss and will increase the temperature at the skin surface). A leg cast should be supported under the calf and allowing the heel to hang free (Fig. 4-8) and thus prevent a gradual deformation of the heel into a point of internal skin pressure.
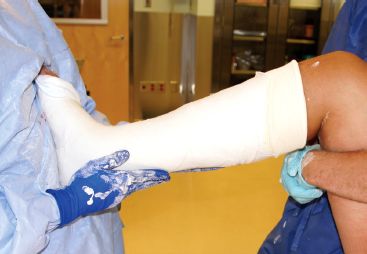
FIGURE 4-7 The foot is supported on the surgeon’s thorax and this holds the foot at 90 degrees while the rest of the cast is molded. (Property of UW Pediatric Orthopaedics.)

FIGURE 4-8 While the cooled cast is supported on the pillow, the heel is allowed to hang free and thus be at less risk for deformation and a heel sore. The cast is univalved with a cast saw that is supported by the surgeon’s index finger. (Property of UW Pediatric Orthopaedics.)
Fiberglass material is applied and molded in a slightly different manner than plaster of Paris. Although synthetic cast material has superior strength in comparison to plaster, some believe its material properties make it harder to apply and mold in comparison to plaster of Paris. Fiberglass material should be removed from its package and dipped in water just prior to application as it will cure and harden in the air. Fiberglass is often tacky in nature and therefore increased tension is needed to unroll the fiberglass, this tension can be inadvertently applied to the limb and result in a cast that is circumferentially too tight. To avoid this, fiberglass should be applied in a stretch relaxation manner23; the fiberglass roll is lifted off of the limb (in contradistinction to plaster which stays in contact); unrolled first then wrapped around the limb (Fig. 4-9). Difficulty exists when wrapping a wide roll into a concavity (anterior elbow or ankle) as the fiberglass can only lay flat if pulled too tight. Small relaxing cuts in the fiberglass may be needed, as fiberglass does not tuck as easily as plaster of Paris. Fiberglass is not as exothermic as plaster of Paris and risk of burns is lower, yet the other principles of holding the cast as the fiberglass cures is the same as in plaster of Paris.

FIGURE 4-9 The fiberglass is applied with stretch relaxation method. The fiberglass is unrolled first then placed over the body. (Property of UW Pediatric Orthopaedics.)
Cast Splitting
Casts are cut and split to decrease the pressure the limb experiences after trauma or surgery. In general, the more trauma (either from the trauma or the surgery performed) a limb experiences, the more edema that will ensue. Thus, minimally displaced fractures can often be managed without splitting a cast, while those requiring a closed or open reduction may initially need to be managed in a split cast or one padded with thick foam. Although splitting may be done prophylactically or as symptoms develop, the experienced clinician will often choose the former to avoid having to split the cast at a later time. Prophylactic cast splitting is often performed while the child is anesthetized or sedated and while this allows for a cooperative patient, great care should be taken when doing so. One must ensure that the plaster or fiberglass has set, that is hardened and cool, and that the blade temperature remains cool throughout the splitting process.
Decreased pressure in a limb can be obtained by cutting and spreading casts and after releasing the underlying padding. The effect of cast splitting depends on the material used, how it was applied, and whether or not the associated padding was split. Plaster cast cutting and spreading (univalve) can be expected to decrease 40% to 60% of the pressure and release of padding may increase this by 10% to 20%.8,23,40,69 Fiberglass casts applied without stretch relaxation are known to be two times tighter than those applied with plaster23 and in these cases bivalving the fiberglass cast would be needed to see similar decreases in pressure. Casts that are applied with the stretch relaxation method are among the least constrictive of fiberglass casts and therefore univalving may be sufficient as long as the cast can be spread and held open. However, many of these synthetic casts often spring back to their original position after simply cutting one side. Thus, it may be wise to use commercially available plastic cast wedges to help hold these split casts open.
Although splitting casts is the traditional means of relieving cast tightness and allowing for swelling, use of thick foam is gaining acceptance at many centers (Fig. 4-10A, B). One of the editors uses ½-in sterile foam on most postoperative casts when concern for swelling is present. In this technique the foam is placed directly on skin, to make sure circumferential pressure is not caused by cast padding. Stockinette and cast padding are then applied, followed by fiberglass. This type of cast is not used to hold a closed reduction with cast molding, but works well for casts with internal fixation. Advantages of this cast include the strength of a circumferential cast, while allowing for swelling similar to a split cast.

FIGURE 4-10 A and B: Foam padding is placed on skin, followed by cast padding, then fiberglass casting material. This allows for welling and provides strength, but does not hold fracture reduction. Ideally stockinette at the ends of the cast would make for better edges. (Image property of Children’s Hospital of Los Angeles.)
Cast Removal
Typically casts are removed using an oscillating cast saw. These saws are designed to cut the hard cast material and not soft material such as padding or skin. In one report the incidence of cast saw burns occurring with the removal of casting material was found to be 0.72%4 (Fig. 4-11). Cast removal may lead to significant morbidity and several precautions are needed. If a waterproof cast was applied using the Gore-Tex padding one must not forget to cut over the incorporated safety strips prior to removal of the fiberglass cast (Fig. 4-12A, B). These can assist in preventing injury from the saw as this type of padding is less heat resistant than the cotton padding.

FIGURE 4-11 Examples of cast saw burns. Initial injury photo (A) and after healing (B). C: A separate injury. Both of these injuries occurred when clubfoot casts were removed. (Property of UW Pediatric Orthopaedics.)

FIGURE 4-12 A: A cutaway picture showing the DE FLEX (W.L. Gore & Associates; Newark, Delaware) strip under the fiberglass casting tape. B: This strip will protect the skin from cast saw that has a propensity to cut easily through synthetic cast padding. (Property of UW Pediatric Orthopaedics.)
Studies have shown that increased cast thickness, decreased padding, and increased blade use result in higher blade temperatures.56 Thus, blades should be inspected and changed frequently as dull blades can increase the heat generated and potential for morbidity. Most importantly the technician who removes the cast must be well trained in the use of the saws. One common pitfall is to slide the oscillating saw along the cast thus increasing the chance of a cut or burn. Proper technique dictates that the blade be used by alternating firm pressure with relaxation into the material and then withdrawn before replacing it at a different location.88 Furthermore, the technician should intermittently feel the blade and pause during the removal process when necessary to allow the blade to cool. This is essential when cutting long casts (i.e., long leg plaster).
Cast removal may lead to significant morbidity and several precautions are needed. Various safety shields are available; which, at the time of cast removal may be slid between the skin and the padding to prevent saw injury. To protect the skin, the cast saw must cut directly over the shield. Often times, the safety shield cannot be slid up the entirety of the cast, so extreme care must be taken in these areas where the skin is not protected. Alternatively, safety strips may be incorporated into the cast at the time of cast application. If a waterproof cast was applied using the Gore-Tex padding one must not forget to cut over the incorporated safety strips prior to removal of the fiberglass cast (Fig. 4-12). These can assist in preventing injury from the saw, as this type of padding is less resistant than the cotton padding. Finally, new advances in differing types of saws may improve the safety of cast removal. For instance, some saws with a scissor-like do not become as hot. These saws are quieter and may reduce children’s anxiety.
Cast Wedging
In a fresh fracture (usually less than 2 weeks old and prior to significant callus formation) in which initial reduction was obtained and subsequently is found to have an unacceptable loss of reduction, cast wedging of a well-fitting cast may be attempted. Many techniques for cast wedging have been described; however, the most recent description by Bebbington6 appears to be easy to apply for simple angular deformities. The radiograph of the malaligned limb is used to trace the long axis of the bone onto a sheet of paper. The paper is then cut along this line. The cut edge of the paper is traced onto the cast, matching the position of the apex of the paper with the apex of the deformity. The cast is then cut, nearly circumferentially at this level, leaving a bridge of intact plaster only at the apex. Corks or cast wedges are applied opposite this bridge, until the line transferred on the cast is straight.
If this fails, the cast may need to be removed and the fracture either remanipulated or treated in some other fashion. Great care should be taken when performing cast wedging, especially in the tibia. The clinician needs to ensure that no excessive focal pressure is exerted at the bridge causing a pressure ulcer or nerve compression. Performing a “closing wedge” of a cast allows the bridge to be placed on the opposite side of the limb, which may be advantageous in certain circumstances, such as correcting a procurvatum or valgus deformity of the tibia. A disadvantage of a “closing wedge” is that it may pinch soft tissue. After performing a cast wedging, it is wise to observe the patient in the clinic long enough to reasonably ensure that any pain associated with the correction has abated and no pain because of focal pressure exists. If any concern exists, a new cast should be applied or a different treatment course taken.
Casting Over Surgical Wounds and Implants
Often casts are applied over surgical wounds. While the majority of these heal uneventfully, special attention should be given to casts applied over traumatic or surgical wounds. When applying a stockinette over a surgical wound, care should be taken to ensure the dressing is not “bunched up” under the liner. It is vitally important that wounds should not be dressed with circumferential cotton gauze as they may become constrictive with dried blood over time and act as a tourniquet. We prefer to use sterile cast padding, which is able to stretch with swelling and limit the gauze directly over the wound itself. Applying nonstick dressings directly to the wound aid in decreasing the anxiety of wound inspection during the cast removal process. Should unexplained pain, fevers, foul odors, drainage, or worsening pain occur; wounds should be inspected; however without these, routine inspection is not often necessary.
Bending the exposed ends of pins under a cast prevents excessive migration and allows for easy removal; however, migration of the bent end of the pin can occur. Sterile felt or antibiotic dressing may be placed at the pin site to help provide mechanical protection of soft tissue from migrating pins. Be aware that pin caps may become displaced and cause pressure sores. Cast padding should be placed over the pins to prevent them from sticking to the casting material as it hardens.
Although the technique of pins and plaster has largely disappeared from adult orthopedics, it can be used occasionally in pediatric orthopedics. In this technique, a fracture is reduced using pins that are placed percutaneously and incorporated into a cast to act essentially as an external fixator. The pin sites should be managed as any other exposed pin with an antibiotic dressing and/or sterile felt at the pin/skin interface. This technique allows the pins to be removed when callus formation is observed without removing the entire cast.
To inspect any area of concern under a cast, the cast can be removed, split, or windowed. The process of windowing involves localizing the area of concern and removing the overlying cast in this area without disrupting the alignment of the underlying bone. One may consider removing this window as a circular or oval piece to avoid creating any stress risers in the cast that may alter its structural integrity. However, attempting to cut “curves” with an oscillating saw places torque on the blade, increases blade temperature. These factors should be remembered when windowing a cast. Once the cast and padding materials are removed, the wound can be inspected. Once satisfied, equal depth of padding should be replaced over the wound and the window replaced. It may be taped in place if serial examinations are required or it may be overwrapped with casting tape. Failure to replace the window can lead to swelling through the window aperture.
Medical Comorbidities That Affect Cast Care
Even with application of a “perfect” cast, numerous medical issues may complicate tolerance of casting or lead to complications.45 Children with myelomeningocele are susceptible to a number of casting complications. Pressure sores commonly occur in insensate children who do not experience or exhibit discomfort when irritation arises under the cast. Caution should be taken to avoid areas of increased pressure or overmolding when casting. In addition, the many fractures in children with myelomeningocele result from casting used for immobilization following elective surgery.66 Iatrogenic fracture risk can be minimized by utilizing casting for as short a time frame as possible and/or use of a soft fiberglass casting material or a soft, bulky dressing that creates less of a stress riser on the bone.66 Children with cerebral palsy are also at increased risk for pressure sores.91 The contractures that likely contributed to the fracture may make casting or splinting difficult.77 Similar approaches may be considered in children with malnutrition, renal osteodystrophy or other bone fragility disorders. An additional consideration in cases of malnutrition and diminished bone health includes increased duration of fracture healing that may require longer periods of protection to prevent refracture.29
Children with obesity present their own complications. Although there are no studies documenting the outcomes of casting in obese children, studies on surgical treatment have demonstrated complications of refracture, wound infection, and failure of surgical fixation,64,98 issues that likely have nonoperative correlates. Loss of alignment when adequate molding cannot occur because of increased soft tissues can occur. When casting an obese child, inclusion of an extra joint above and/or below the fracture may be required to maintain cast position. Diligent monitoring of alignment allows intervention with recasting, wedging, or transition to surgical intervention. Obese patients are more likely to undergo surgical treatment, as opposed to closed reduction, although it is unclear whether this is related to fracture severity or concerns regarding fracture stabilization.81
Alterations in casting materials or approaches may also be necessary in children with behavioral issues. Children with autistic-spectrum disorder present additional complexity during cast application (see discussion on distraction techniques), but even prior to cast application considering their behavior guides decision making regarding the most appropriate immobilization. Children with violent tendencies pose even more risk once a cast is applied, not only to others but also themselves. Administration of behavioral medications may improve tolerance of casting.18 Soft splinting may be preferable, accepting some risk of malunion over likely secondary injury. Discussion and shared decision making with the parents result in the best management for an individual child and her family.
Children with dermatologic conditions require other considerations when deciding on best methods of immobilization. Children with atopic dermatitis may react to synthetic padding, so cotton may be more preferable. Splinting allows for better skin management, but when casting is required, minimizing duration or performing frequent cast changes allows for monitoring of skin conditions or early transition to splinting. Soft casting material contains diisocyanate which has been suspected, but not proven, as a skin irritant in isolated cases60; avoiding such material in children with significant skin sensitivity or disorders seems prudent. Windowing the cast over an area of skin breakdown or infection allows for monitoring of the area. Varicella presents an even more complex issue as widespread skin breakdown occurs predisposing to superinfection. Casting helps prevent skin breakdown by covering itchy lesions, but monitoring lesions is not possible. Again, splinting may be preferable to allow for monitoring if it does not compromise maintenance of fracture reduction; otherwise, windowing, or frequent cast changes may allow for skin monitoring. There should be a low threshold for removal of the cast if the child complains of pain to assess for not only compartment syndrome or infection, but also necrotizing fasciitis.20,25
LOCATION-SPECIFIC IMMOBILIZATION
Sugar-Tong Splint Immobilization
Sugar-tong splints provide effective temporary support to the wrist and forearm until definitive reduction and casting or internal fixation, while allowing for swelling. Sugar-tong splints can be used for definitive treatment provided the splint is comfortable and is retightened after 3 to 5 days to accommodate the decrease in swelling. At that point reapplication of an elastic bandage or overwrapping with fiberglass is appropriate.
Before treating, the contralateral uninjured limb may be used as a template to measure and prepare an appropriate slab of casting material which should be wide enough to fully support the volar and dorsal surfaces of the arm (without radial and ulnar overlap) and long enough to span the arm from the volar MP flexion crease in the hand, around the elbow (flexed at 90 degrees), and dorsally to the metacarpal heads (Fig. 4-13). It is important that plaster splints are no more than 10 layers thick and of appropriate length so that edges do not have to be folded over (increasing thickness and the heat from curing). The slab is further customized to cut out material around the thumb base and tuck cuts are made at the elbow to prevent bunching of the material during the application.

FIGURE 4-13 The plaster roll for the sugar-tong splint is measured and is chosen to be wider than the arm without allowing for overlapping once the plaster slab is dipped and applied. (Property of UW Pediatric Orthopaedics.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


