2 The Hand
S. Rehart, S. Sell, B. Kurosch, J. Richard
2.1 General
The assessment of treatment indications for the rheumatic hand is easily one of the most difficult topics in orthopaedic rheumatology.
Determining an optimal course of treatment for the patient requires simultaneous consideration of many factors. The hand’s current functional limitations need to be evaluated within the context of the underlying destruction and dysfunction of the hand structures, as well as the patient’s overall disease-related limitations. An in-depth knowledge of the different courses of specific rheumatic illness is essential for determining an indication for treatment. For example, does the patient have psoriatic arthritis that is more prone to ankyloses, or destabilizing arthritis that leads to instability?
The level of destruction plays only a limited role in determining the extent of surgical intervention. The best functional improvement is achieved by arthrodesis of the thumb carpometacarpal joint. Consequently, this type of intervention paves the way for and creates the necessary confidence in additional and potentially more major procedures. For it to be possible to give patients a timeline for surgical improvement of their hand, a therapeutic plan is often essential:
Stabilization of the wrist joint.
Swanson prosthesis of the metacarpophalangeal (MCP) joint.
Arthrodesis of the proximal interphalangeal (PIP) joint.
The importance of functional aftercare must be discussed with the patient from the outset because it is one of the keys to success.
It is relatively easy to determine indications for treatment of the hand in urgent or emergent situations. First and foremost among these are tendon ruptures. However, even these can be tolerated by some patients for months or years. The goal is to treat flexor or extensor tendon ruptures as quickly as possible. From both technical and functional standpoints, the more time that elapses after the initial event, the more difficult treatment of these ruptures becomes.
An end-to-end suture repair is only rarely feasible because the tissue is usually too damaged and the tendons have retracted too far. Side-to-side repair is possible for extensive ruptures, and a free transplant (for example, using the palmaris longus tendon) is an option for large defects. In these situations functional aftercare and, ultimately, outcomes are clearly more challenging.
A rupture of the tendon of the extensor pollicis longus (EPL) muscle, the most common tendon rupture of the hand, represents a special situation. It typically involves performing a surgical transposition of the tendon of the extensor indicis proprius muscle, although this requires lengthy follow-up treatment. Arthrodesis of the interphalangeal joint of the thumb presents an alternative and should be considered depending upon the amount of hand involvement and level of overall disease. Functionality should also be discussed with the patient.
The indications are much more obvious if there is medial nerve compression accompanied by significant inflammatory symptoms. Here patients usually seek medical care themselves due to pain. In addition to decompression of the median nerve, it is crucial to perform an extensive synovectomy of the flexor tendons.
Treatment indications for tenosynovitis, in contrast, are often more difficult to recognize and not as easy for patients to accept. Here the swelling in the hand is painless and, as long as tendon rupture has not occurred, does not impair the patient.
As a general rule for surgical correction of the hand: Start proximal, move distal!
For example, a soft tissue repair of an ulnar deviation of the MCP joint seems futile if the wrist has a severe axial deviation located more proximally. The repair inevitably results in recurrence.
According to the Schulthess classification of rheumatic wrist disease, there are three different progressive forms:
Arthritic.
Ankylosing.
Destabilizing.
The destabilizing progressive form, which leads to ulnar dislocation, usually originates from scapholunate (SL) ligament disruption. It must be recognized early in order to perform a radiolunate arthrodesis as this type of arthrodesis requires an intact distal wrist joint.
It is often difficult to determine indications for soft tissue repairs on MCP joints or swan neck/boutonnière deformities. There cannot be too much bone damage and the soft tissues must still be amenable to repair through a release. At the same time, there must still be sufficient long-term stability of the soft tissues after they are surgically repaired or transposed. Accurate assessment requires many years of experience treating rheumatic hands.
Clearly, it is much harder to determine the correct treatment indications than to perform the operative intervention itself.
2.2 The Wrist
2.2.1 Arthroscopic Synovectomy of the Wrist
Indication
Therapy resistant Larsen 0–II/III synovitis after optimization of medication therapy and cortisone injections.
Extensor tendon synovitis, which is frequently present, requires an open procedure.
Specific disclosures for patient consent
Recurrence. Infection. Radiosynoviorthesis or chemosynoviorthesis may be necessary 6 weeks postoperatively.
Instruments
Standard small joint arthroscope. Camera. Shaver system. Electrocautery.
Position
Supine. Tourniquet on the proximal upper arm. The arm is suspended using a wrist traction device with the elbow joint in 90° of flexion. The suspension device is draped in a sterile fashion (Fig. 2‑2). Weights (ca. 3 kg each) are hung on both sides.
Approach
See Fig. 2‑1.


Specifics
See Fig. 2‑3, Fig. 2‑4, Fig. 2‑5, Fig. 2‑6 . Prior to insertion of the trocar, the radiocarpal joint is insufflated through the 3/4 (radiocarpal) portal using a syringe. The probe and shaver are initially inserted through the 4/5 portal, and then later switched. Finally, the midcarpal joint is accessed via the midcarpal radial (MCR) and midcarpal ulnar (MCU) portals.




Key steps
Arthroscopy should be performed carefully in the small spaces to avoid iatrogenic cartilage injuries.
Operative technique


Specific complications
Recurrence. Progression of destruction. Development of a supination deformity.
2.2.2 Radiolunate Arthrodesis
Indication
Larsen III–IV destruction with significant clinical symptoms. Radiocarpal joint supination deformity with ulnar drift and palmar subluxation. Radiologically progressive destabilizing form. Impending extensor tendon rupture.
Note that there should be no more than moderate midcarpal destruction.
Consider performing a radioscapholunate arthrodesis if there is pronounced radioscaphoid joint destruction. A Mannerfelt arthrodesis or a prosthesis is indicated for midcarpal destruction.
Specific disclosures for patient consent
Loosening, breakage, or dislocation of staples. Tendon rupture (also secondary). Perioperative impact on flexor tendons and median nerve. Loss of wrist function. Pseudarthrosis. Bone fracture/perforation. Damage to sensory cutaneous nerve branches. Resection of the ipsilateral ulnar head is often necessary and cancellous bone is harvested to place into the radiolunate (RL) arthrodesis site.
Instruments
Stapler with 10 × 15-mm or 16 × 15-mm staples. Standard hand surgery set.
Position
Supine. Hand table. Arrange for perioperative mobile radiography.
Approach
See Fig. 2‑9.

Specifics
Preoperatively, fit a palmar plaster splint that is to be applied immediately postoperatively.
A residual midcarpal range of motion of 30–0–30° extension–flexion can be expected postoperatively.
Key steps
Precisely match the resection surfaces of the distal radius lunate fossa and the decorticated proximal lunate surfaces. Firmly reduce and hold the surfaces together during staple insertion. Resect the interosseous branch of the radial nerve on the floor of the fourth extensor tendon compartment.
Surgical technique
See Fig. 2‑10, Fig. 2‑11, Fig. 2‑12, Fig. 2‑13, Fig. 2‑14, Fig. 2‑15, Fig. 2‑16, Fig. 2‑17, Fig. 2‑18, Fig. 2‑19.










Specific complications
Fracture and dislocation of staples. Pseudarthrosis (often asymptomatic).
Postoperative aftercare
Radiographic imaging at 2 and 6 weeks postoperatively.
Immobilization in the plaster splint (palmar plaster splint, with fingers freely mobile at the MCP joints) until stitches are removed 14 days postoperatively. Then an additional 2 to 4 weeks of immobilization in a forearm circular cast. Cast removal is dependent upon follow-up radiographic findings. See Fig. 2‑20 for an 8-year follow-up.

2.2.3 Ulnar Head Resection
Indication
Larsen II–III destruction of the radioulnar joint with instability and pain that limits forearm rotational movement. Synovitis. (Pseudo-)Prominence of the ulnar head with skin breakdown imminent or impending rupture of the fourth or fifth digit extensor tendons.
Specific disclosures for patient consent
Wrist joint extension/flexion range of motion may be reduced by as much as 30%. Reduced distal radioulnar joint (DRUJ) range of motion for pronation and supination.
Instruments
Standard hand surgery set. Oscillating saw.
Position
Supine. Hand table.
Specifics
A tenosynovectomy of the entire wrist and extensor tendons is also typically performed. Ulnar head resection is frequently combined with a partial radiocarpal arthrodesis (radiolunate or radioscapholunate) due to anticipated instability. Alternatively, a split tendon transfer using the extensor carpi radialis brevis (ECRB) tendon or a Sauvé–Kapandji procedure (distal ulnar segment resection and radioulnar fusion) can be performed.
Approach
A dorsal longitudinal incision is made over the wrist and continued over the DRUJ. A lateral incision over the distal end of the ulna is used only for isolated ulnar head resection. See Fig. 2‑21, Fig. 2‑22, Fig. 2‑23.



Key steps
Meticulous joint tenosynovectomy, capsule reconstruction, and repositioning of the extensor carpi ulnaris muscle tendon over the ulnar head.
Surgical technique
See Fig. 2‑24, Fig. 2‑25, Fig. 2‑26, Fig. 2‑27, Fig. 2‑28.





Specific complications
Progressive ulnar translocation of the carpus may occur if only an isolated ulnar head resection is performed without carpal fixation.
Postoperative aftercare
Postoperative radiography. Immobilize the joint in a palmar forearm plaster splint until wound healing is complete. Administer active and passive physical exercise therapy.
2.2.4 Wrist Prosthesis
Indication
Larsen III–V destruction with significant clinical symptoms. Absence of severe axial deformities. No wrist instability (function-sparing procedures such as radiolunate arthrodesis are no longer possible).
Specific disclosures for patient consent
Prosthesis loosening or dislocation. Tendon rupture (also secondary). Loss of wrist joint function. Bone fracture/perforation. Damage to sensory nerve branches.
Instruments
Prosthesis system from the manufacturer of choice. Standard hand surgery set.
Position
Supine. Hand table. The hand should be extended as far as possible onto the hand table. A radiograph may be needed.
Approach


Wrist prosthesis system (Maestro, Biomet):
Carpal plates in eight sizes; capitate stems in three different lengths; carpal heads in three different heights to allow for wrist balancing.
Scaphoid augments in various sizes.
Anatomically contoured radial plates in two sizes with four different radial stem sizes.
Surgical technique
See Fig. 2‑29, Fig. 2‑30, Fig. 2‑31, Fig. 2‑32, Fig. 2‑33, Fig. 2‑34, Fig. 2‑35, Fig. 2‑36, Fig. 2‑37, Fig. 2‑38, Fig. 2‑39, Fig. 2‑40, Fig. 2‑41, Fig. 2‑42, Fig. 2‑43, Fig. 2‑44, Fig. 2‑45, Fig. 2‑46, Fig. 2‑47.









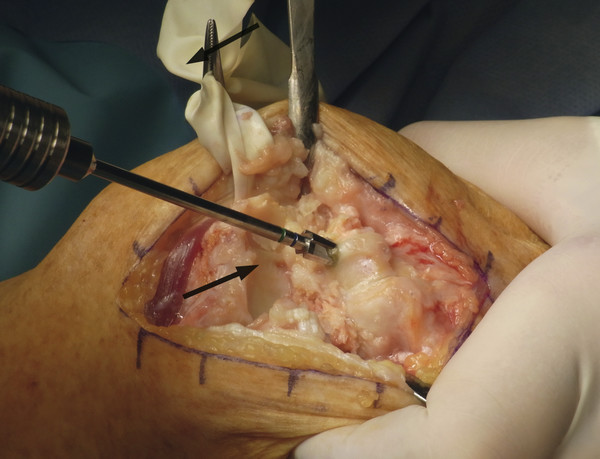







Postoperative aftercare
See Fig. 2‑48, Fig. 2‑49 . Immediate full range of motion mobilization (caveat: no shoulder immobilization!). Early finger exercises. Palmar splint for 1 to 3 weeks.


2.2.5 Mannerfelt Wrist Arthrodesis
Indication
Advanced Larsen IV–V radiocarpal and midcarpal destruction. Simmen type III advanced instability with ulnar drift and palmar subluxation. This is particularly appropriate for fixing the dominant hand in 10 to 20° extension. If needed, the contralateral hand can then be fixed in a neutral position or fitted for a prosthesis.
Specific disclosures for patient consent
Postoperative wrist joint function. Delayed or failed bone healing. Hardware dislocation or breakage. Fracture. Damage to sensory nerve branches. Tendon rupture (also secondary).
Instruments
Standard hand surgery set; intramedullary hook-end nail (Rush pin). Alternative: plate fixation arthrodesis. Fluoroscopy equipment.
Position
Supine. Hand table. The hand should be extended as far as possible onto the hand table. A radiograph may be needed.
Specifics
The bones are frequently very osteoporotic.
Approach
A dorsal longitudinal incision is made starting over the third metacarpal and extending to the wrist along the ulnar axis.
Key steps
Reposition the wrist joint. Completely decorticate the joint surfaces. Prebend the hook-end nail to ca. 50° at the level of the wrist (clinically there will still be 20° of extension left postoperatively). Insert the nail on the ulnar side of the base of the third metacarpal via a bone window.
Surgical technique
See Fig. 2‑50, Fig. 2‑51, Fig. 2‑52, Fig. 2‑53, Fig. 2‑54, Fig. 2‑55, Fig. 2‑56, Fig. 2‑57, Fig. 2‑58, Fig. 2‑59, Fig. 2‑60, Fig. 2‑61.












Postoperative aftercare
Postoperative radiography. A palmar forearm plaster splint should be applied until wound healing is complete, then circular forearm cast for an additional 4 weeks.
Alternative
Plate fixation arthrodesis (Fig. 2‑62, Fig. 2‑63 ).


Specific disclosures for patient consent
Extensor tendon problems in the rheumatoid wrist.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








