Patients with Legg-Calvé-Perthes disease can often be successfully treated with femoral head–preserving measures, such as bracing, or containment procedures with osteotomies. However, in some cases, after resolution of the disease, the femoral head may proceed to collapse or progress to severe arthritis at a young age. If nonoperative methods have failed, the only treatment options available for these adolescents or young adults may be a total hip resurfacing or a total hip arthroplasty (THA). This article focuses on the results and unique technical considerations of resurfacing and THA for patients who have severe hip osteoarthritis after resolved Legg-Calvé-Perthes disease.
Patients with Legg-Calvé-Perthes disease can often be successfully treated with femoral head–preserving measures, such as bracing, or containment procedures with osteotomies. However, in some cases, after resolution of the disease, the femoral head may proceed to collapse or progress to severe arthritis at a young age. If nonoperative methods have failed, the only treatment options available for these adolescents or young adults may be a total hip resurfacing or a total hip arthroplasty (THA). A study of the Danish registry of 135 patients (156 hips) treated for Legg-Calvé-Perthes disease found that 13% of patients required a THA procedure as opposed to none in an age-matched cohort of healthy patients after a mean follow-up of 47 years (range, 37–58 years). This article focuses on the results and unique technical considerations of resurfacing and THA for patients who have severe hip osteoarthritis after resolved Legg-Calvé-Perthes disease.
Total hip resurfacing
Because of younger age and higher activity levels seen in patients who have severe hip osteoarthritis after resolved Legg-Calvé-Perthes disease, total hip resurfacing may provide a more attractive alternative to conventional THA. Resurfacing is performed by replacing the hip joint with a metal cup in the acetabulum that articulates with a bearing that is capped on the prepared femoral head. Typically, the cap has a small stem that goes down the neck of the femur, and the procedure does not involve the placement of a stem down the shaft of the femoral diaphysis. This feature allows for easier component placement in those who have deformities associated with Perthes disease of the proximal femur from prior surgeries, such as coxa vara or coxa valga. These metal-on-metal designs are usually larger in diameter than most THA components, which have the potential to decrease the risk of dislocation rates that may occur more frequently in these younger, more-active patients. In addition, this procedure is more bone conserving than a THA because it preserves the proximal femur, which may allow for an easier revision to a THA, if necessary.
Several reports on resurfacings have shown excellent results in patients younger than 40 years with reported survivorships of 93% or greater. Boyd and colleagues reported on 18 patients (19 hips) who underwent total hip resurfacing for Legg-Calvé-Perthes disease; they observed a 100% survivorship at a mean follow-up of 51 months (range, 26–72 months) and noted that 18 of the 19 hips had good to excellent clinical results as evidenced by Harris hip scores of 80 points or more. The investigators concluded that their results for resurfacing compared similarly to other studies using standard THA. Amstutz and colleagues studied 21 patients (25 hips) who had a mean age of 38 years (range, 18–57 years) and underwent resurfacing for Legg-Calvé-Perthes disease (14 hips) or slipped capital femoral epiphysis (11 hips). At a mean follow-up of 4.7 years (range, 2.7–8.1 years), they observed a 92% survivorship.
There are a few contraindications to total hip resurfacing. Although wear rates seen with metal-on-metal bearings are extremely low, there have been reports of increased metal ion concentrations in these patients. Therefore, renal dysfunction is an absolute contraindication to this procedure because metal ions are excreted by the kidneys. In addition, because the effect of increased metal ions is mostly unknown, the US Food and Drug Administration recommends that women of childbearing age should not undergo this procedure. Other relative contraindications to this procedure are the presence of extensive cystic damage of the femoral head or severe osteoporosis because a healthy bone stock is important for good component fixation and sizing. Intraoperative assessment should be made of the femoral head, and the authors recommend that if less than 75% of the bone is viable, a standard THA should be performed. A report from the Australian Orthopaedic Association National Joint Replacement registry noted a higher failure rate in total hip resurfacing than in THA in patients with acetabular cup sizes less than 50 mm, which may have implications for smaller patients who have had Perthes disease. Complications that have been reported with this procedure include local adverse tissue reactions such as pseudotumor and aseptic lymphocytic vasculitis–associated lesions, although symptomatic lesions seem to occur in less than 1% of all patients undergoing the procedure. The true incidence and cause of these complications is unknown.
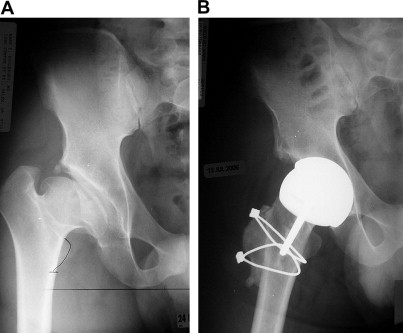
Total hip resurfacing is a technically demanding procedure, and it is recommended that it be performed only by an experienced surgeon. Patients who had Legg-Calvé-Perthes disease may have unique deformities that necessitate variations in the surgical approach. These patients often have overgrowth of bone around the femoral head (coxa magna) or flattening of the femoral head (coxa plana) and thus are at an increased risk for limb length shortening and femoral neck impingement after the procedure. One must focus on not notching the femoral neck when preparing these hips with deformed femoral heads. Trochanteric advancement is a useful variation to this procedure, described by Boyd and colleagues, to prevent these complications. The greater trochanter is cut and advanced over the femoral neck under the vastus lateralis muscle. The bone is then fixed with 2 cables, one placed over the greater trochanter and the other through 2 drill holes in the cortex of the femoral neck to aid in compression ( Fig. 1 ). This mode of fixing adds length to the femoral neck to counter limb length discrepancies and tightens the abductor muscle group for later increased strength.
THA
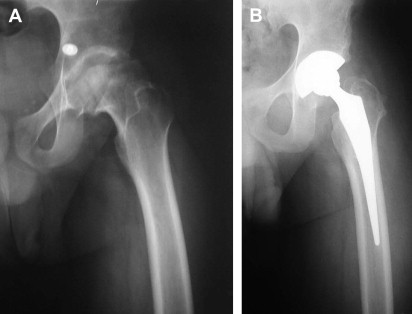
In patients who are poor candidates for a resurfacing, a standard THA may be performed ( Fig. 2 ). There are only a few published reports on exclusive cohorts of patients undergoing THA for residual arthritis from Legg-Calvé-Perthes disease. However, survivorship of this procedure in young adults has ranged from 51% to 94% at midterm follow-up in reports, including patients who have diagnoses of Legg-Calvé-Perthes disease. Since the publication of these articles, advancements in polyethylene bearings and femoral stems have further increased THA implant survivorship and durability, making these procedures even more palatable to younger patients. One recent study of the Danish Hip Registry found in 361 patients (404 hips) who had Legg-Calvé-Perthes disease and had undergone THA, a revision rate of only 6% (24 of 404 hips) at a mean follow-up of 4.6 years (range, 1 day–12 years). It was noted that patients undergoing THA who previously had Legg-Calvé-Perthes disease were at no increased risk for revision when matched to other patient cohorts. Another study from the Norwegian Arthroplasty Registry of patients who underwent THA for either Legg-Calvé-Perthes disease or epiphysiolysis derived a Kaplan-Meier 10-year survivorship of 92% (55 revisions in 708 hips). The mean age at the time of surgery was 52 years (range, 15–88 years).