There has been a significant increase in the prevalence of obesity in the United States over the last 20 years, with the highest percentage in Mississippi. The percentage of obese patients undergoing total hip arthroplasty (THA) appears to be increasing at an even faster rate. Orthopedic surgeons performing hip arthroplasty need to be aware of potential issues to minimize complications associated with this population. This article outlines preoperative and postoperative care and describes current techniques and tools used by surgeons in obese patients to facilitate soft tissue dissection, exposure, implant placement, and closure.
Obesity in the United States and worldwide continues to grow. According to the Centers for Disease Control, obesity is defined as a body mass index (BMI, calculated as weight in kilograms divided by height in meters squared) greater than 30. There has been a significant increase in the prevalence of obesity in the United States over the last 20 years, with the highest percentage in Mississippi. The most recent data indicate that the prevalence of obesity now exceeds 30% in most sex and age groups. The percentage of obese patients undergoing total hip arthroplasty (THA) seems to be increasing at an even faster rate.
Many retrospective and prospective studies have evaluated whether obesity affects outcomes and complication rates after total hip replacement, with conflicting results. However, the increase in the number of obese patients requesting THA is certain, and orthopedic surgeons performing hip arthroplasty need to be aware of potential issues to minimize complications associated with this population. This article outlines preoperative and postoperative care and describes current techniques and tools used by surgeons in obese patients to facilitate soft tissue dissection, exposure, implant placement, and closure.
Preoperative planning
When considering any elective surgical intervention, detailed and thorough discussions are necessary between the patient and the surgeon. However, in the case of obese patients, preoperative counseling is even more critical before making the decision for elective THA. Obesity increases the risk of multiple medical problems, such as diabetes, hypertension, heart disease, obstructive sleep apnea, and osteoarthritis. Highly obese patients undergoing THA have an increased incidence of hypertension and diabetes mellitus. Each associated medical condition must be addressed before surgery; yet, in aggregate, managing multiple medical problems can be problematic and may lend themselves to increased perioperative complications. Preoperative medical clearance is mandatory to optimize the patient’s medical condition before surgery. Consideration should also be made for cardiology and pulmonary evaluations if there is any concern for coronary heart disease and sleep apnea.
Another factor associated with preoperative planning for the obese patients is age at the time of surgery. The obese patient set has been shown to be in need of surgical intervention at a young age. Furthermore, morbidly obese patients (BMI >40) have been found to be as much as 10 years younger than patients with a normal BMI at presentation for arthroplasty. Maximizing nonoperative management before elective joint replacement in young patients is encouraged. It is the responsibility of the surgeon considering THA for obese and morbidly obese patients that the patients understand the implications of earlier THA, and this discussion must be held within the context of the technical challenges associated with THA in obese patients.
A common belief, or possible excuse, among the obese population is that the pain associated with arthritis prevents exercise that is necessary for weight loss. Many obese patients understand that they are significantly overweight but are adamant that eliminating their pain through joint replacement will allow an increase in exercise and activity leading to weight loss; however, recent studies contradict these assertions. Several recent studies have shown that a higher percentage of obese and morbidly obese patients actually gain more than 5% of their preoperative weight after total knee arthroplasty and THA. Another prospective study of patients undergoing total joint replacement revealed postoperative weight gain in patients who underwent both hip and knee replacement and a significant amount of weight gain in youngpatients who underwent THA.
Therefore, when evaluating an obese patient for THA, it is crucial to encourage weight loss before surgery. Recommendations should include dietary changes with possible nutrition consultation, increased physical activity, and possible bariatric surgery. Physical activity is often difficult and painful for the morbidly obese, but aquatic therapy provides an alternative that both unloads the joints and allows for increased exercise ability. When considering recommendations for bariatric surgery, no specific levels are used, but patients with a BMI of more than 45 are likely to benefit, and the option should be mentioned. Results indicate that a patient can decrease their BMI significantly and undergo successful THA within an average of 2 years between bariatric surgery and arthroplasty.
Considering all the additional factors and the possibility of increased complication rates, preoperative planning and the final decision for surgery are of increased importance in the obese population. Surgery can be considered even if weight loss measures are unsuccessful, but both the surgeon and the patient need to carefully weigh all risks and benefits and proceed only after expectations are mutually understood.
Surgical technique
After the decision for surgery has been made, considerations must be made for surgical positioning, approach, and technique. As with all surgical interventions, the patient should receive the surgical technique and approach that is done best by their surgeon. The morbidly obese population has been found to require a significantly longer operating time for THA, and THA in obese patients tends to result in increased intraoperative blood loss. Soft tissue handling and exposure techniques are even more critical in obese patients because of the possibility of increased wound complications. Advantages and disadvantages exist for all surgical exposures, but the senior author (R.K.M) has found that the posterior approach in the lateral decubitus position ( Fig. 1 ) aids in improving visualization. No specific changes are necessary for the obese patient, but each step can prove more difficult. The obese patient typically needs a longer incision, more operative time devoted to exposure, and a full capsulotomy for acetabular exposure. In the lateral decubitus position, gravity aids in soft tissue retraction as the abdominal panniculus displaces anteriorly away from the operative field. The buttocks also fall away from the operative field posteriorly (see Fig. 1 ); however, the surgeon may face positioning difficulties. When placing the patient in the lateral decubitus position, it can be difficult to determine if the pelvis is positioned perpendicularly to the table because of the lack of visual and palpable landmarks. The difficulties with positioning can ultimately lead to issues with acetabular component position because of unrecognized pelvic obliquity. Therefore, more vigilance must be taken in positioning, and anatomic landmarks after acetabular exposure are necessary to obtain proper component version. The obese patient likely needs a longer incision to avoid tension on soft tissues. Although these patients may be interested in minimally invasive surgery, they are not ideal candidates for such techniques because of increased trauma to soft tissues. However, the push for minimally invasive surgery has led to better instrumentation that is compatible with obese patients, such as curved reamer handles and modified retractors.
The senior author prefers the posterior approach with complete posterior capsular and muscular repair as described by Hedley and colleagues for the obese population. The technique starts with an incision over the posterior half of the greater trochanter and extends proximally and distally, with two-thirds of the incision proximal to the greater trochanter and one-third distal. A straight-line incision is created, with the leg positioned at approximately 45° of hip flexion; this positioning creates a gentle posterior curve to the incision as the leg is extended. The greater trochanter can often be difficult to palpate in obese patients. It is recommended to palpate the greater trochanter while taking the extremity through a rotational range of motion to aid in proper orientation of the incision. Palpation of the trochanter is performed during dissection through the fatty layer to ensure the correct position before reaching the fascia. The proximal extent of the exposure is critical in the obese population because the increased amount of soft tissue can prevent proper access for femoral preparation. In addition, without proper exposure, the abductor musculature can be damaged during reaming and broaching.
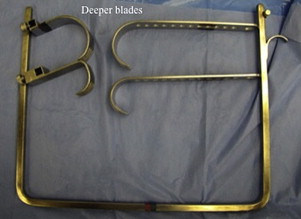
After the skin and subcutaneous fat dissection, the gluteus maximus muscle and iliotibial band are identified. The iliotibial band is split distally and extended proximally into a natural split in the gluteus maximus muscle. Allowing for an appropriate split in the muscle aids in minimizing the soft tissue trauma that can occur with a forced separation. A Charnley retractor is then placed to maintain exposure. In the obese population, the deeper blades for each side of the Charnley retractor need to be available and used ( Fig. 2 ). Richardson retractors are then used to sequentially retract the gluteus maximus muscle anteriorly, followed by identification and retraction of the posterior border of the gluteus medius muscle to identify the interval between the gluteus medius and gluteus minimus muscles. The piriformis muscle tendon is identified along the interval with the gluteus minimus muscle.
At this stage, a long Bovie electrocautery tip is used to ease deep dissection. The piriformis is clamped and released from its insertion on the piriformis fossa of the femur. This procedure allows access to the posterior border of the gluteus minimus, which is then dissected and elevated, off the capsule. The small Richardson retractor is then placed deep to the gluteus minimus between the muscle and the capsule. The capsule is then incised in line with the superior border of the piriformis. The capsule and short external rotator muscles are dissected off the posterior femur as one triangular flap, keeping this as long as possible for future repair.
An anterior superior capsulotomy is performed with a large curved scissors before dislocation of the femoral head. The femoral neck osteotomy is then performed at a level based on preoperative templating and intraoperative measurement from the proximal aspect of the lesser trochanter to a point representing the proposed center of the prosthetic head. The senior author has found that a full capsulotomy in this patient population is necessary to obtain proper acetabular exposure.
The second Charnley-type self-retaining retractor ( Fig. 3 ) is then placed with one side firmly seated in the capsule and the other in the posterior aspect of the greater trochanter. The seating in the capsule is facilitated by a making a 2-mm hole in the capsule with Bovie electrocautery before placement. The prong can then be placed securely in this opening in the capsule. A third Charnley-type self-retaining retractor is then placed with the 4-prong side in the gluteus minimus muscle and capsule and the 2-prong side in the inferior capsule (see Fig. 3 ). The Charnley-type retractors provide long handles and hinges between blades and arms to allow proper positioning even in deep wounds (DePuy Orthopaedics, Inc, Warsaw, IN, USA). The final retractor used is the anterior retractor, which allows further anterior translation of the femur. With proper placement of all retractors, sufficient visualization of the acetabulum can be achieved even in the obese population ( Fig. 4 ).






