Dynamic stabilization of the spine has applications in cervical and lumbar degenerative disease and in thoracolumbar trauma. There is little evidence to support the use of dynamic cervical plates rather than rigid anterior cervical fixation. Evidence to support the use of dynamic constructs for fusion in the lumbar spine is also limited. Fusion rates, implant loosening, and failure are significant concerns that limit the adoption of current devices. This article provides a synopsis of the literature on human subjects. There is a need for high-quality evidence for interventions for spinal pathology. An evidence-based approach to the management of spinal disorders will require ongoing assessment of clinical outcomes and comparison of effectiveness between alternatives.
Arthrodesis of the spine is an important and useful technique for the management of spinal disorders including deformity, trauma, segmental instability, and symptomatic disc degeneration. Rigid stabilization of the spine with segmental fixation, fixed axis screws, and large diameter rods creates a mechanical environment that is associated with higher fusion rates than noninstrumented or semirigid constructs. However, rigid segmental fixation may have significant adverse effects including an increase in the stress on adjacent mobile segments, and stress shielding the bone graft material within the regenerate. Dynamic stabilization of a painful motion segment is an alternative to rigid internal fixation that may be useful in improving rates of fusion, or in providing an alternative approach to the surgical management of a painful motion segment without arthrodesis. Techniques of dynamic stabilization have been developed and evaluated for the treatment of degenerative conditions of the cervical and lumbar spine, and for thoracolumbar trauma and deformity. The purpose of this article is to review and assess the evidence in the literature on the efficacy of dynamic stabilization techniques in the management of spinal disorders.
Dynamic stabilization of the spine is a mechanical constraint of spinal motion that allows selective motion of the functional spinal unit. Dynamic stabilization in the cervical spine with a dynamic plating system is intended to limit motion to compression without translation. Selective compression may improve interbody healing and fusion mass formation. In the lumbar spine, posterior dynamic stabilization devices may provide segmental distraction without fusion, or may limit the motion of an unstable motion segment. When not used for fusion, these devices are designed to be load sharing with the spinal segment, selectively reducing translatory stresses and potentially modifying axial pain. Dynamic stabilization encompasses motion-sparing options for spinal instrumentation. Total disc arthroplasty devices have limited constraint in flexion, extension, and rotation compared with the normal motion segment. Rigid fixation of a motion segment causes changes in motion segment kinematics in the adjacent segments and increases in the area of center axis of rotation and intradiscal pressure. Less constrained motion-sparing options, including total disc arthroplasty in the cervical and lumbar spine, may reduce the effect of instrumentation on adjacent segments. The association of adjacent segment degeneration and disease with altered segmental kinematics remains controversial. The efficacy of restoring kinemetics of the adjacent segment with motion-sparing devices on reducing adjacent segment degeneration and pathology has yet to be reported in long-term follow-up.
This article is a systematic review of the evidence for dynamic stabilization devices used for cervical fusion and lumbar posterior dynamic stabilization for degenerative disease and trauma. Selection of devices for discussion was limited to dynamic stabilization options with published clinical outcome studies, and including objective patient-based health-related quality of life outcomes. All devices included have been approved by the US Food and Drug Administration (FDA) through 510k regulatory provision. The studies of lumbar and thoracolumbar posterior dynamic stabilization devices include physician-directed, or off-label uses of the devices without fusion. The quality of the evidence is graded using the technique of the Center for Evidence-based Medicine. The article is intended to provide the reader with an overview of published evidence of efficacy for dynamic stabilization devices in the cervical and lumbar spine.
Cervical spine
Anterior cervical plating is associated with decreased rates of graft dislodgement, kyphosis, and endplate fracture, and increased rates of fusion following multilevel anterior cervical discectomy and fusion. Rigid plating of multilevel constructs is believed to increase fusion rates by minimizing micromotion at the interbody spaces. With more than 2 treated levels, however, reported pseudarthrosis rates have been similar for instrumented and noninstrumented constructs. The rigid anterior cervical plate may prevent segmental subsidence, and loading of the interbody graft, allowing for gap formation and leading to nonunion. Dynamic cervical fusion plates are designed to compress the graft axially while preventing translation. There are 3 main types marketed and studied that are designed to load the interbody graft with variable axis of screws or axial compression capacity in the plate design. The first allows load sharing through screws that may toggle within the plate, allowing for compression through the graft. A second allows for graft compression through sliding screws within the plate, as the screw holes are oblong ( Fig. 1 ). A third design allows for rigid fixation through the screw holes, and allows for shortening of the plate itself through a telescoping design.
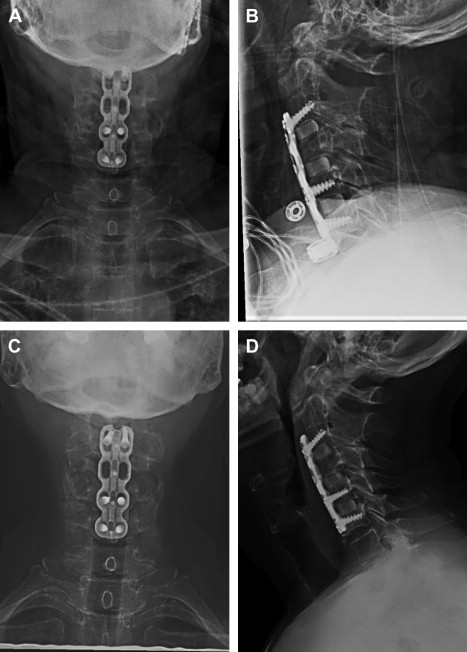
The biomechanical advantages of a dynamic cervical plate have been validated in basic scientific investigations. In a cadaveric C5 corpectomy model, Reidy and colleagues compared compressive forces borne by rigid and dynamic cervical plates. With optimally sized grafts, the rigid plate bore 23% of the load, versus 9% for the dynamic plate. The interbody graft handled 23% more force with the dynamic plate, which supports the intent of loading the interbody graft. With an undersized graft, a situation similar to graft subsidence or contact osteolysis, the dynamic plate allowed for more force transmission through the graft, although the greatest increases in forces were seen in the posterior elements. Brodke and colleagues, in a subsequent C5 corpectomy model, showed a significant increase in the load borne by the rigid plate with graft subsidence. In this model, graft subsidence did not affect the load-sharing properties of a dynamic cervical plate.
Clinical efficacy of dynamic cervical plates has been studied in several retrospective and prospective studies including prospective randomized controlled trials. Epstein reported on 42 patients undergoing single-level anterior cervical disc fusion (ACDF) with a dynamic plate. The results confirmed excellent fusion rates, and documented compression of the graft construct beneath the plate. However, the plate failure rate was 9.5%. Similar results were reported by Casha and Fehlings in their study of dynamic plating for cervical fusion. The cases reviewed were not limited to single-level ACDF, however, and included nearly equal numbers of single- and multilevel ACDF and single- and multilevel corpectomy. They reported an overall fusion rate of 93.8% at 2 years follow-up, with an implant complication rate of 8.2%. Implant failure correlated with an increasing length of construct. Radiographic measurements confirmed the dynamic properties of the plate.
Pitzen and colleagues presented level I data from a trial of 132 patients, comparing rigid with dynamic cervical plating for 1- and 2-level ACDF for degenerative disease or cervical trauma. The outcomes assessed were implant-related complication rates, time to radiographic fusion, loss of lordosis, and outcomes as assessed by the Visual Analog Scale (VAS) and the Neck Disability Index (NDI). The rigid plating group experienced a significantly higher rate of implant complications including plate loosening and screw breakage ( P = .045) The rigid plating group did have better preservation of cervical lordosis at 2 years follow-up ( P = .003). There were no significant differences in the clinical outcomes assessments. Because of the difference in complication rates, and despite the differences in cervical lordosis, the investigators concluded that dynamic plates are the preferable method of fixation for 1- and 2-level ACDF.
Nunley and colleagues performed a randomized controlled trial of a heterogeneous mix of patients undergoing single- or multilevel ACDF with rigid or dynamic fixation. They found no difference in outcomes for the groups undergoing single-level ACDF, but did find an advantage to dynamic instrumentation for multilevel ACDF. In contrast, DuBois and colleagues reviewed 52 patients undergoing 2- and 3-level ACDF, comparing rigid with dynamic anterior cervical plating. They found an increase in the rate of nonunion when using the dynamic cervical plate ( P = .05). They measured the amount of construct settling over 1 to 2 years, and found no difference between the plating systems, thus questioning the compressive properties of the plate in vivo. Clinical outcomes were similar among the groups, which led the investigators to conclude that the more expensive dynamic plates do not offer any clear benefit compared with rigid plates.
Anterior cervical plating is associated with adjacent-level ossification which may be due to impingement from the plate on the adjacent level disc space ( Fig. 2 ). Although comparative series have shown no difference in incidence of this complication when comparing rigid with dynamic cervical plating, special attention must be paid to technique when using a dynamic plate. Park and colleagues noted that the incidence of moderate to severe adjacent-level ossification was increased with less than 5 mm of space between the adjacent disc and plate. The implication for those using dynamic plates is that the subsidence of the bodies and graft must be accounted for at the time of surgery, as the plates may encroach on the adjacent levels in follow-up, as the graft is compressed. This problem requires the surgeon to know the amount of subsidence allowed by the plate, and to understand the method of dynamization to optimize plate and screw placement.
Conclusion
The clinical evidence for cervical dynamic plating remains mixed. The literature supports a compressive role of the dynamic cervical plate ( Table 1 ). However, there is little evidence for improvement of fusion rates or clinical outcomes compared with rigid fixation. The loss of segmental lordosis and potential for adjacent segment impingement is a significant limitation of cervical dynamic stabilization.
| Authors | Year | Study Design | Indications | Results | Grade of Evidence |
|---|---|---|---|---|---|
| Epstein | 2003 | Retrospective cohort | Degenerative disk disease (DDD), ossification of the posterior longitudinal ligament (OPLL), spondylosis | Mean Nurick score improved 2.5 points; 90.5% fusion rate | C |
| Casha and Fehlings | 2003 | Prospective cohort | Spondylosis, herniated nucleus pulposus (HNP), trauma, tumor, reactive arthritis (RA) | 68.7% neurologic improvement; 76.6% pain improvement; 93.8% fusion rate | C |
| DuBois et al | 2007 | Retrospective, case control | Degenerative disease | Odom ratings similar; dynamic group with 16% nonunion vs 5% rigid | B |
| Saphier et al | 2007 | Prospective cohort | Degenerative disease | Fusion rates and patient satisfaction similar | C |
| Goldberg et al | 2007 | Retrospective, case control | 2-level degenerative disease | Fusion rates similar between rigid and dynamic plates | B |
| Pitzen et al | 2009 | Prospective, randomized, controlled | Trauma, single- and 2-level DDD | Fusion rates similar; dynamic lost 3.6° lordosis vs static plate; VAS/ODI similar | A |
| Nunley et al | 2009 | Prospective, randomized, controlled | Degenerative disease | Fusion rates similar; single-level procedure VAS/ODI scores similar; double level VAS/ODI improved with dynamic plate | A |
Lumbar spine
The advent of rigid spinal instrumentation was accompanied by higher fusion rates in the treatment of degenerative lumbar disease without clear improvements in clinical outcomes. Rigid instrumentation does result in increased forces at the adjacent segments of the spine as measured by intradiscal pressure. The role of increased forces at the adjacent segments in causing adjacent segment degeneration and disease remains undetermined. The rates of adjacent segment disease are as high as 36%. The concern for adjacent segment degeneration and disease has driven the development of dynamic, or semirigid, constructs for lumbar spine instrumentation. As with cervical spine instrumentation, the dynamic instrumentation for the lumbar spine is designed to be a load-sharing device, allowing for fusion without excessive rigidity leading to adjacent segment complications. Some dynamic constructs have also been used without fusion. Preclinical evidence to support less rigid stabilization as a mechanism for improving fusion rates in the spine is limited. In the United States, the FDA has approved lumbar dynamic stabilization devices through the 510k regulatory pathway. A new technology that is substantially equivalent to existing devices that have been in use since before 1976 may be approved by the FDA under the process of 510(k) approval. The US FDA 510(k) regulatory process specifically applies to devices and technologies for which there was a predicate device in existence before 1976. The level of clinical evidence required for 510k approval is variable and approval may be based on mechanical and preclinical studies alone. Dynamic stabilization devices without fusion have been applied in a physician-directed use, or off-label application. Therefore, the literature on lumbar dynamic stabilization without fusion is limited to a few prospective studies. This section reviews the evidence for these devices as instruments for spinal fusion, and discusses the use of fusion devices for dynamic stabilization. For a broader review of the recent data, the reader is referred to the recent publication by Bono and colleagues.
The dynamic systems approved for spinal fusion under the FDA 510k provision are pedicle screw–based constructs that are semirigid, or allow constrained motion in compression or flexion and extension. The rigidity of these constructs is affected by the choice of material and design of the rods connecting pedicle screws. Although solid stainless steel and titanium are commonly used in spinal fusion constructs, the semirigid constructs include polyetheretherketone (PEEK) rods, nitinol rods, specially cut rods (eg, Accuflex), articulated rods, and polyethylene terephthalate cords (Dynesys). The optimal mechanical properties of a semirigid fixation system have not been determined.
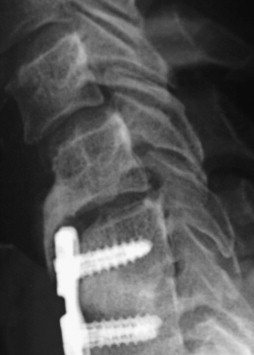
PEEK is a polymer that has been studied in spinal fusion. The material properties of PEEK make it popular for several reasons. It is a biocompatible polymer, with excellent strength, virtually no reactivity, and it is radiolucent ( Fig. 3 ). Ponnappan and colleagues compared the biomechanical properties of 5.5-mm PEEK rods with those of 5.5-mm titanium rods for single-level posterolateral fusion (PLF), and when paired with posterior lumbar interbody fusion (PLIF). They found no significant difference in stiffness between the PLF constructs in flexion/extension, lateral bending, or axial rotation. The PLIF constructs were significantly stiffer than the PLF constructs in all 3 planes. Again, there were no differences between the titanium and PEEK constructs with PLIF. The PEEK constructs with interbody graft did show increased load sharing with the interbody graft compared with the titanium posterior instrumentation. A PEEK posterior rod with an interbody graft may improve load sharing with interbody fusions, thereby encouraging compression of the interbody graft. The PEEK constructs also showed reduced stress at the pedicle screw to bone interface, which may reduce the risk of pedicle screw loosening. The ability to visualize the fusion mass is also a noted advantage of PEEK rods. There are no published clinical data that support improved outcome regarding fusion rates or screw loosening.
Nitinol is a nickel and titanium memory alloy. The flexibility and rigidity of the alloy vary with the temperature of the surrounding environment. These material properties allow the alloy to be contoured at room temperatures, and to return to a precontoured position at body temperature. The Bio-Flex System (Bio-Spine; Korea) consists of titanium pedicle screws and coiled 4-mm Nitinol rods. Kim and colleagues described the use of this system in a heterogeneous cohort of patients and treatment modalities for degenerative disease of the lumbar spine. Used in combination with PLIF, the fusion rate achieved was 90%, and the overall success rate was 90.7%. The investigators reported that adjacent segment motion was increased at levels adjacent to the Bio-Flex system alone and at combined Bio-Flex/PLIF levels, and concluded that the Bio-Flex system allows for more physiologic movement at the adjacent segments. The effect of increased motion at segments adjacent to instrumented levels on degeneration will require long-term follow-up. Further evaluation of nitinol semirigid fixation will require matched comparison with rigid fixation systems.
The AccuFlex System (Globus Medical Inc; Audubon, PA, USA) is a semirigid rod designed for use with a standard pedicle screw instrumentation system. Through a proprietary technique, helical cuts are made in a 6.5-mm rod, making the rod less rigid. This system is limited to single-level use, and because the orientation of the helical cuts is fixed, the rod is not amenable to contouring. The results for a randomized controlled trial of single-level posterior spinal fusion (PSF) with interbody fusion with standard 6.5-mm rods versus AccuFlex rods were reported by Mandigo and colleagues. At 1 year of follow-up, results with respect to Short Form 36 (SF-36) scores, VAS scores, and fusion rates did not differ between the 2 groups. The investigators were careful to note that more follow-up is needed to determine whether rates of adjacent segment disease are different between the groups.
The Twinflex system (Eurosurgical; Beaurains, France) is a flexible system, based on 2.5-mm stainless steel rods, and pedicle screw fixation. The smaller diameter rods allow for less rigid fixation, again with the hypothesis that load sharing will allow for high fusion rates with less adjacent segment disease. A well-designed study by Korovessis and colleagues compared this system with rigid and semirigid pedicle screw systems. With 15 patients per group and an average of 4 years follow-up, no differences in clinical results were observed. Three patients in the dynamic Twinflex group sustained broken implants, but fusion rates were similar within all 3 groups. Adjacent segment disease was not observed in any of the groups. These investigators concluded that, as the results were similar among all groups, no clear recommendations may be made. In this case, further follow-up and cost analyses may help clarify the usefulness of these different instrumentation systems.
The Dynesys (Centerpulse/Zimmer, Winterthur, Switzerland) system is marketed as a fusion device, despite a lack of peer-reviewed reports available to assess its utility for this purpose. Dynamic stabilization of the spine without fusion remains a controversial strategy in the management of spinal disorders. The Dynesys dynamic stabilization system is a pedicle screw–based construct, with polyethylene terephthalate cords and polyurethane sleeves bridging the pedicle screws. The cord acts to stabilize the motion segment in flexion, whereas the sleeve acts to stabilize in extension, and this effect has been shown in cadaveric studies. As with other dynamic devices, the intention of instrumentation with this device is to minimize the effect of stabilization on the adjacent segments, thereby lowering the incidence of adjacent segment disease. The designers of the device reported good results at 3-year follow-up in 73 patients undergoing dynamic stabilization for degenerative disease with the Dynesys system. Eleven patients suffered “complications related to the implant,” with 2 requiring reoperation. An additional 11 patients underwent additional surgery for persistent pain or adjacent segment disease. Despite these high complication rates (30%), the trial investigators concluded that the implant was a success for management of degenerative lumbar disease. Statistically significant changes were observed in VAS and Oswestry Disability Index (ODI) scores. Comparison with a matched cohort treated with rigid stabilization will be useful in an assessment of the Dynesys system for treatment of degenerative lumbar pathology without fusion.
Dynesys instrumentation has been reported with variable outcomes in recent publications. Beastall and colleagues used positional magnetic resonance imaging (MRI) to compare instrumented segment and adjacent segment motion following rigid instrumentation and Dynesys instrumentation. The investigators confirmed the motion-sparing and stabilizing properties of Dynesys compared with rigid instrumentation, as the dynamic stabilization group had a greater, although still restricted, range of motion (ROM) at the instrumented level. Their results, however, were opposite to the in vitro results of Schmoelz and colleagues, as extension was limited, rather than flexion. With only 9 months follow-up, Beastall and colleagues did confirm that adjacent segment motion was unchanged following Dynesys instrumentation. However, this same group found MRI evidence of progressive degenerative disease at Dynesys instrumented levels and at adjacent levels. Whether this is a result of the natural history of degenerative disease, as suggested by Hilibrand and colleagues in the cervical spine, or a result of the intervention is unknown and will require further follow-up. In a separate investigation comparing adjacent segment ROM after Dynesys and rigid instrumentation, Cakir and colleagues found no difference in ROM from the preoperative and postoperative periods. They conclude that Dynesys shows no beneficial effect on the adjacent segment.
Patient-based outcome measures are an important tool for assessing device efficacy, and represent the most important measure of implant performance. Grob and colleagues presented results in their report of 2 years follow-up of a heterogeneous group of lumbar degenerative disease patients who underwent dynamic stabilization. Their results show that only 50% of patients reported that the procedure helped or helped a lot. When comparing their results with historical controls treated with fusion procedures for similar indications, these results were inferior. They note that 19% of the patients studied required reoperation within the short follow-up period. They conclude that there is no evidence to support that dynamic stabilization is superior to fusion regarding clinical outcome or need for revision surgery at the same or an adjacent level. Clinical results were also reported by Bothmann and colleagues in a review of 40 patients with an average of 16 months follow-up. Subjective improvements in pain and quality of life were reported in 73% of the patients studied. These clinical improvements were similar to results from traditional fusion surgery. The investigators conclude that dynamic stabilization alone is not a successful procedure, and stabilization should be accompanied by decompression of the neural elements. An alarming reoperation rate of 27.5% was reported, with 17.5% of patients suffering from loosening of the pedicle screws. Implant loosening and high reoperation rates are important limitations in the published efficacy of dynamic stabilization systems without fusion.
Conclusion
Semirigid instrumentation of the spine may be applied with the intent to fuse the spine, or to stabilize the affected motion segment without fusion. The optimal rigidity of a posterior instrumentation system for fusion remains undetermined. Preclinical data support semirigid fixation improving the load on the interbody graft. There is little evidence that semirigid fixation may improve PLF rates ( Table 2 ). Long-term follow-up of the effect of semirigid fixation on adjacent segment pathology will permit an evaluation of the technology as a strategy for preventing adjacent segment degeneration.




