Abstract
Objective
It is a major issue to diagnose and detect oropharyngeal dysphagia in the early stage of ALS in order to avoid pulmonary and nutritional complications. The aim of this study was to validate a simple clinical test, the Volume-Viscosity Swallow Test (V-VST), to detect oropharyngeal dysphagia in this population.
Patients and methods
Twenty patients were included in this study (mean age: 66.1 ± 8.13, six women). All patients had their swallowing function assessed by videofluoroscopy and V-VST.
Results
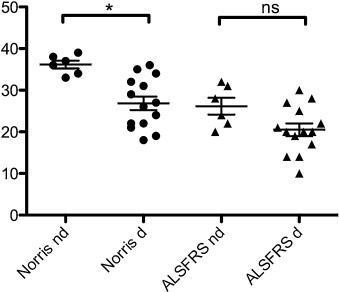
Among these 20 patients, 15 presented oropharyngeal dysphagia, diagnosed by videofluoroscopy, and five had normal swallowing. Norris score was lower in patients with oropharyngeal dysphagia compared to the patients with normal swallowing (27 ± 6 versus 36 ± 2; P = 0.003). Among the 15 patients with oropharyngeal dysphagia, 14 had abnormal V-VST, and only one had normal V-VST. The sensibility of V-VST to detect oropharyngeal dysphagia in these patients with ALS was of 93%, and the specificity was of 80% ( P = 0.007). There was no significant difference between the two populations for ALSFRS score (22 ± 6 versus 20 ± 6) and body mass index (BMI) (26 ± 6 versus 26 ± 6 kg/m 2 ).
Conclusion
The V-VST presented good sensibility and specificity. It may be interesting to use it systematically for the detection of oropharyngeal dysphagia in ALS, after confirming these results on a wider patient sample.
Résumé
Objectif
La dysphagie oropharyngée est fréquente aux cours de l’évolution de la SLA et nécessite un diagnostic et une prise en charge précoce, avant qu’elle ne se complique de dénutrition ou de pneumopathie d’inhalation. L’objectif de cette étude était de valider un test clinique simple, le Volume-Viscosity Swallow Test (V-VST), pour dépister et diagnostiquer la dysphagie oropharyngée dans cette population.
Patients et méthodes
Vingt patients ont été inclus dans cette étude (âge : 66,1 ± 8,13, six femmes) et ils ont tous eu une évaluation de leur déglutition par vidéofluoroscopie et par V-VST.
Résultats
Parmi les 20 patients inclus, 15 présentaient une dysphagie oropharyngée diagnostiquée par la vidéofluoroscopie et cinq avaient une déglutition normale. Les patients avec dysphagie oropharyngée avaient un score de Norris plus faible par rapport à ceux qui avaient une déglutition normale (27 ± 6 versus 36 ± 2 ; p = 0,003). Quatorze présentaient un V-VST anormal et un seul présentait un V-VST normal. La sensibilité du V-VST pour le dépistage des troubles de la déglutition chez les patients atteints de SLA était donc de 93 % et la spécificité de 80 % ( p = 0,007). Il n’y avait pas de différence significative entre les deux populations pour le score ALSFRS (22 ± 6 versus 20 ± 6) et l’indice de masse corporel (IMC) (26 ± 6 versus 26 ± 6 kg/m 2 ).
Conclusion
Le V-VST présentant une bonne sensibilité et spécificité, il pourrait être intéressant de le proposer pour le diagnostic précoce de la dysphagie oropharyngée chez les patients atteints de SLA, après avoir confirmé ces résultats sur un échantillon plus large.
1
English version
1.1
Introduction
Oropharyngeal dysphagia is very frequent during the course of amyotrophic lateral sclerosis, and especially in its bulbar form . In the early stages of oropharyngeal dysphagia, oral functions are mainly affected with an alteration of the forming and holding of the bolus . Early diagnosis and management of oropharyngeal dysphagia is important to avoid complications like undernourishment, dehydration, or aspiration pneumopathy. On the other hand, oropharyngeal dysphagia significantly impairs the patients’ quality of life, particularly during meals .
Initially, oropharyngeal dysphagia is clinically suspected in view of low specific signs and must be confirmed by videofluoroscopy or by nasofibroscopy . Videofluoroscopy is currently the reference examination for the study of swallowing disorders, and enables orienting their management by adapting at best food textures and rehabilitation . It is however a radiating examination, costly, and not very accessible. There is currently a clinical test, simple to carry out, the Volume-Viscosity Swallow Test (V-VST), validated for the screening of oropharyngeal dysphagia in general population, with good sensibility and specificity .
The objective of this study was to validate the V-VST, a simple, easy to carry out and accessible clinical test, for the systematic screening and early diagnosis of oropharyngeal dysphagia in patients with amyotrophic lateral sclerosis.
1.2
Patients and methods
1.2.1
Patients
Twenty patients were consecutively included during their systematic check-up performed every 3 months. ALS was diagnosed according to El Escorial criteria (clinical and paraclinical criteria).
The swallowing clinical evaluation was carried out using the V-VST test.
The V-VST was performed only if the patient had an efficient cough, saturation higher than 92%, voluntary swallowing, was able to maintain attention for more than 15 minutes, and presented neither drooling nor wet voice . V-VST and videofluoroscopy were realized at the same time, by two different operators. The operator realizing the V-VST was unaware of the results of the pharyngography. During the whole duration of the test and of the videofluoroscopy, the oxy-hemoglobin saturation was measured by pulse oxymetry (Nellcor OxiMax N-560, Coviden, Boulder, USA).
The V-VST was realized by a physician or a trained technician. The test consisted in the administration of increasing volumes of different textures and the evaluation during each swallowing of the presence of signs of efficacy or safety alteration. The test starts with a nectar texture (prepared with 4.5 g of food thickener in 100 ml of mineral water) by bolus of increasing volumes of 5, 10, and then 20 ml. If the patients presented no sign of choking, the test was continued with a liquid texture by bolus of 5, 10, and then 20 ml. Finally, the test ended with a bolus of 5, 10, and then 20 ml of a pudding texture (prepared with 9 g of food thickener in 100 ml of mineral water) .
If the patients presented signs of alteration of safety with the nectar texture, the liquids were not tested, and the pudding texture was directly used. As for consistency, the volumes were not increased in case of safety alteration. The V-VST was assessed as abnormal as soon as the patient presented a clinical sign of safety alteration, i.e. laryngeal aspiration or tracheal penetration (cough, desaturation greater than 3%, or wet voice) or of efficacy alteration (presence of an oral or pharyngeal residue during swallowing, need for repeated swallowing, and presence of drooling) during a single swallowing ( Fig. 2 ).
1.2.2
Videofluoroscopic evaluation of swallowing
Swallowing was assessed by videofluoroscopy to determine the presence or not of oropharyngeal dysphagia. Acquisition of images was realized by image intensifier (Flexiview 8800, General Electric, United Medical Technlogies Corp., Fort Myers, FL, USA) and was recorded on a computer at 20 images per second (MMS, Tubingen, The Netherlands). The upper incisors, the higher part of the palate, the upper cervical spine, and the lower part of the proximal esophagus were included in the field of projection.
The patients were comfortably seated in an armchair and were asked not to move during the video recording. They swallowed three barium boluses of respectively 5, 10, and 20 ml of nectar, then liquid, then pudding texture, following the same procedures of realization as those of V-VST. All boluses were measured with a 20-ml syringe and then given either in a glass or with a spoon.
Food choke was quantified through a validated 8-point scale . The diameter of a 5-centimes coin was used as a marker to assess the pharyngeal stasis and allowed its rating using a 5-point scale: 0 was absence of stasis whereas 4 was major stasis . The alterations of oral timing were also recorded by a 5-point score where 0 corresponded to the absence of temporal alteration, and 4 to the impossibility to control bolus formation . This reference examination enabled us to diagnose the presence of oropharyngeal dysphagia in case of stasis, food choking and temporal alteration.
1.2.3
Evaluation of nutritional status
The patients were weighed, which allowed calculating their body mass index (BMI). This enabled the assessment of undernourishment.
1.2.4
Norris bulbar scores and Amyotrophic Lateral Sclerosis Funtional Rating Scale (ALSFRS)
The bulbar Norris score allowed orienting towards a bulbar form of ALS. It was scored from 39 (normal status) to 0 (total dysfunction of bulbar form) . The ALSFRS score was used to assess the functional disability, taking into account 10 activities of daily life noted on five points each, where 0 corresponded to “impossibility to do it” and 4 to “normal activity” .
1.2.5
Statistics
The patients were divided in two groups: one group of patients presenting oropharyngeal dysphagia, and one group with normal swallowing, according to the results of the videofluoroscopy. The results of the V-VST were then analysed as being normal or abnormal (safety or efficacy altered). Sensibility and specificity of the V-VST for the diagnosis of oropharyngeal dysphagia were calculated using a test of the Chi 2 (StatView 5, SAS Institute, Cary, NC, USA).
The Norris and ALSFRS scores were analysed and compared between groups with the non parametric test of Mann-Whitney (StatView 5, SAS Institute, Cary, NC, USA). The differences were considered as significant if P ≤ 0.05.
1.3
Results
All patients had videofluoroscopy performed without any particular problem. Mean age was 66 ± 8 years and had a BMI of 26 ± 5 kg/m 2 ( Table 1 ). Among the twenty patients included, 15 presented oropharyngeal dysphagia at videofluoroscopy, 10 of them having moderate dysphagia, and five, severe. Norris score was significantly weaker in patients presenting oropharyngeal dysphagia compared those with normal swallowing ( P = 0.003), whereas there was no difference on the ALSFRS score ( Fig. 1 ).
| Patient | Weight | Height | BMI | Norris | ALSFRS |
|---|---|---|---|---|---|
| (kg) | (cm) | (kg/m 2 ) | |||
| #1 | 60 | 158 | 24 | 33 | 32 |
| #2 | 69 | 163 | 26 | 39 | 31 |
| #3 | 74 | 176 | 24 | 34 | 28 |
| #4 | 67 | 181 | 20 | 37 | 24 |
| #5 | 92 | 171 | 31 | 38 | 20 |
| #6 | 101 | 178 | 32 | 36 | 22 |
| m ± sd | 77 ± 15 | 171 ± 9 | 26 ± 5 | 36 ± 2 | 26 ± 5 |
| #7 (d) | 116 | 173 | 39 | 22 | 17 |
| #8 (d) | 49 | 167 | 18 | 27 | 25 |
| #9 (d) | 58 | 161 | 22 | 21 | 28 |
| #10 (d) | 78 | 180 | 24 | 36 | 20 |
| #11 (d) | 83 | 159 | 33 | 19 | 20 |
| #12 (d) | 52 | 163 | 20 | 18 | 19 |
| #13 (d) | 90 | 184 | 27 | 24 | 14 |
| #14 (d) | 79 | 169 | 28 | 22 | 14 |
| #15 (d) | 59 | 165 | 22 | 32 | 10 |
| #16 (d) | 69 | 169 | 24 | 35 | 22 |
| #17 (d) | 59 | 171 | 20 | 26 | 27 |
| #18 (d) | 87 | 167 | 31 | 34 | 20 |
| #19 (d) | 70 | 158 | 28 | 29 | 30 |
| #20 (d) | 67 | 167 | 24 | 31 | 21 |
| m ± sd | 73 ± 18 | 168 ± 7 | 26 ± 6 | 27 ± 6 | 21 ± 6 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







