Revision surgery of the proximal femur with bone loss secondary to failed cephalomedullary nails is problematic and becoming more prevalent as their use grows. This article presents a technique of deformity correction, bone graft techniques that reconstitute residual defects, and definitive fixation using load-sharing devices that provide immediate stability for bone healing and early rehabilitation. Preoperative planning and the potential advantages and disadvantages of newer fixed-angled plates versus established implants are discussed. With proper planning, surgical execution with proved techniques, augmented by the addition of newer graft harvesting techniques, anatomic restoration, and bone reconstitution with healing, has invariably been the result.
Fractures of the peritrochanteric and subtrochanteric region of the femur can represent a significant problem in the primary setting. In the revision setting, dealing with bone loss and correcting deformity increases the difficulty. These fractures have large mechanical forces exerted over very short bone segments. Koch described the forces acting on the proximal femur and observed that a 100-lb force could create 1250 lb/in 2 of compression on the medial side of the femur and 1000 lb/in 2 of tension on the lateral side of the femur. These forces have a significant impact on the treatment of proximal femur fractures and, to overcome them, durable implants that attain reliable fixation are needed. Current primary treatment of these factures has shifted from plate osteosynthesis to that of intramedullary splinting. Several intramedullary devices have been developed with enlarged proximal bodies and large screws that insert into the femoral head to overcome the deforming forces of these fractures, sometimes referred to as cephalomedullary nails. Some studies suggest these larger implants can provide increased initial stability. A study by Roberts and colleagues found that the fracture site motion was decreased in unstable subtrochanteric fractures with implants designed as cephalomedullary nails have large proximal bodies. Although the development of new implants has lead to improved stability over older extramedullary implants, it is not without cost. The amount of bone removed from the proximal femur is significantly increased when compared with plate fixation and can lead to problems of implant dependency and bone voids and problems during revision of these implants in ununited or malunited fractures. The tremendous forces acting on the proximal femur are compounded when there is little bone for implants to obtain purchase. In the setting of nonunions and malunions of the proximal femur, the bone defects typically need to be addressed.
Despite these drawbacks, the prevailing treatment has shifted to intramedullary nails with cephalic locking options. Biomechanical studies comparing intramedullary fixation and plate fixation are conflicting. A study by Tencer and coworkers found an advantage in intramedullary nailing with respect to combined bending and compression, although plates and intramedullary constructs were able to support at least 100% of a human’s body weight. A more recent biomechanical study showed increase displacement in an unstable subtrochanteric fracture model with use of the gamma nail (Stryker, Kalamazoo, Michigan) compared with a 95° angle blade plate (Synthes, Paoli, Pennsylvania).
Initial treatment of these fractures is difficult, regardless of the implant chosen for fixation. Forces on the proximal femur tend to externally rotate, flex, and abduct the proximal fragment, and correction of these forces is critical for the initial treatment of these fractures to be successful. Anatomic reduction is the best way to insure appropriate healing of these fractures at the initial time of surgery and affords patients the best opportunity to gain full recovery. Anatomic reduction is imperative for normal hip kinematics and to promote rapid union. A durable implant, like a cephalomedullary implant, placed poorly that can induce malreduction cannot always be relied on to attain final union. If union is attained, then a residual deformity may leave a patient with a deformed extremity, altered gait, or limp
The rate of symptomatic malunion is rarely reported in the literature. Wiss and Brien defined malunion as shortening greater than 1 cm, 10° of angulation in any plane, or rotational malalignment greater than 15°. They reported six malunions out of 98 subtrochanteric femur fractures treated with intramedullary nailing. Malunion can be severely disabling with shortening of the affected extremity or persistent limp that does not improve without surgical intervention.
Despite the reported increased biomechanical favorability of intramedullary implants used to treat proximal femur fractures, the affect of these large implants has not been studied. The enlarged proximal body implants remove a significant amount of cancellous bone in the head, neck, and peritrochanteric region of the femur that is difficult to replace in revision surgery. Volumetric analysis of three popular cephalomedullary implants ranges from 21 to 27 cm 3 ( Table 1 ). Subsequent removal of these implants, therefore, exemplifies the problem surgeons must anticipate when dealing with these large defects. Not only is the bone loss large but also it is directly in the region of the compression and tension trabeculae of the proximal femur, which are of utmost importance in hip structural integrity.
| Nail Description | Nail Volume (cm 3 ) | Blade/screw Description | Blade/screw Volume (cm 3 ) | Sleeve (cm 3 ) | Total Volume (cm 3 ) | |
|---|---|---|---|---|---|---|
| TFN | 11 mm × 130°, 170-mm long | 15.96 | 110 mm long | 6.65 | n/a | 22.61 |
| Gamma | 11 mm × 130°, 180-mm long | 15.84 | 75 mm long | 3.86 | n/a | 19.70 |
| IMHS | 12 mm × 130°, 210-mm long | 19.91 | 105 mm long | 4.83 | 2.30 | 27.04 |
The rate of nonunion of the subtrochanteric femur fracture healing is reported as between 1% to 20% in the orthopedic literature. Few studies have been done looking at revision surgery of subtrochanteric nonunions. Options include revision to a larger intramedullary implant, fixation with a plate, or hip arthroplasty with typically a calcar replacing implants in older patients with severely diminished bone stock. Haidukewych and Berry reported on 23 nonunions that underwent revision using a variety of implants, including cephalomedullary nails and blade plates. Twenty of the 21 nonunions healed and two were lost to follow-up. Eighteen of the 23 required additional bone grafting. The investigators concluded that different implants can be used successfully depending on fracture location and bone quality; however, statistically significant differences could not be found with the limited numbers of patients.
de Vries and colleagues evaluated results of subtrochanteric nonunions treated with blade plating techniques. Thirty-two of 33 nonunions healed with this technique. They thought that blade plates were more suited for nonunions with deformity, as anatomic correction and compression with the plate is reliable whereas use of intramedullary implants is challenging and limited. They also emphasized key steps in treating these nonunions: correction of malalignment, bone grafting when necessary, and internal fixation with compression. Barquet and colleagues reported on a series of 26 patients with subtrochanteric nonunion treated with revision surgery with a long cephalomedullary nail. Their results were good, with 88% going on to union after one procedure and 25 of 26 uniting after additional procedures, including nail dynamization and bone grafting. They chose to use a gamma nail due to the biomechanical advantage, allowing immediate postoperative weight bearing, and because of the large proximal body that filled the proximal bone defects. They reported six patients with continued varus deformity greater than 5° postoperatively, three of whom had a pre-existing varus deformity that was not corrected. Correction of deformity and compression across the nonunion site are difficult to attain with a cephalomedullary nail during revision surgery. In the authors’ experience, the majority of proximal femoral nonunions have residual deformity that typically needs to be addressed at the time of revision to assure union and restoration of normal gait.
The revision of intramedullary fixation of the proximal femur is a technically demanding surgery, which requires significant preoperative planning. Surgical tactics must allow for contingency plans for problems typically encountered during the procedure. In addition to bridging large cavitary bone defects with biomechanically stable fixation, surgeons must promote reconstitution of bone loss to allow later implant removal. Recent advances in reaming techniques and harvesting of osteoinductive, autogenous cancellous grafts combined with established uses of structural, osteoconductive allografts allow consistent management of these two problems.
In the authors’ experience, proximal femoral fracture nonunions and malunions with bone loss are best treated with four typical steps: first, removal of previous hardware; second, bone grafting of defects; third, controlled osteotomy to correct deformity and restore normal anatomy; and fourth, and finally, attaining a stable, load-sharing construct by tensioning the implant and using Association for the Study of Internal Fixation (ASIF) techniques, thereby compressing the osteotomy and allowing early weight bearing and rapid bone consolidation.
Preoperative planning is required to deal with proximal femoral fractures with bone loss. Included in this planning are identification of the previous implant and having any special equipment required for removal, the need for and degree of osteotomy, having structural allograft and the ability to obtain autogenous bone graft for osteoindution, and, finally, the ideal implant for controlled reduction and definitive stabilization. A preoperative workup for infection is also important. This usually consists of erythrocyte sedimentation rate, C-reactive protein, and a white blood cell count. A preoperative plan with templating of the corrective osteotomy level, including the degree and the steps of the procedure, should be visible to the entire operating room team. This helps prevent confusion and allows everyone to know the current step and next step in the operative plan by reviewing the surgical tactic.
In most situations, an extensile approach to the hip is used through a lateral approach. The tensor fascia lata aponeurosis is split longitudinally and the vastus lateralis is freed laterally and transversely at the inferior aspect of the vastus ridge and elevated anteriorly with a posterior based L-shaped incision. Only the lateral side of the femur is dissected free; preserving the vascular supply to medially based fragments is paramount. In cases of atrophic nonunions, the nonunion site is débrided until punctuate bleeding from both ends is encountered. In this case, more extensive exposure of medial based structures may be needed. In hypertrophic nonunions where stability at the fracture site is the main cause of nonunion, a thorough débridement is not necessary.
Removal of failed hardware is usually the first step in dealing with these revision surgeries. Correction of deformities is impossible without removing the failed previous implants. Prevention of further bone loss is important in these difficult fractures. Having the proper equipment available can help to remove implants in an efficient and atraumatic manner. Most implants have removal devices that minimize further iatrogenic injury and should be made available. A broken screw removal set aids in removal of broken hardware. In the most difficult situations, a metal cutting burr can be beneficial in freeing and extracting incarcerated hardware. The time required for this initial part of the procedure should not be minimized.
The authors’ technique of managing the resultant bone defects is multifaceted. Bone grafting depends on the size and extent of the bone loss. In general, use of structural allograft is imperative for increasing strength of the fixation in the head and blocking loss of cancellous graft from the large peritrochanteric defects. The authors typically use preshaped allograft cortical bone dowels stacked sequentially into the screw/head defect and then dowels that block egress of cancellous graft from the holes left by the nail in the trochanter, lateral femur, and subtrochanteric canal ( Fig. 1 ). Alternatively, cortical struts or matchsticks can sometimes be used in the screw/head defect. Cancellous graft is liberally impacted into the open proximal femur and around the interstices of the allograft.
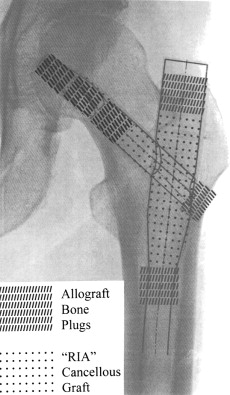
The large cancellous defects left in the peritrochanteric region require generous amounts of osteoinductive, cancellous autograft. Traditionally, autogenous graft was harvested from the ipsilateral iliac crest through a separate incision and then morselized and impacted into the defects. This requires an additional incision and has been associated with additional complications, including prolonged pain, infection, hematoma, and even lateral femoral cutaneous nerve palsey. Iliac crest bone graft can provide limited volumes from some crests that can be insufficient for the large defects encountered. The authors use the Reamer-Irrigator-Aspirator System (RIA, Synthes) to harvest morselized bone graft from the ipsilateral femoral canal after the previous hardware is removed. Recent studies suggest the advantage of this system in that it is a negative pressure system that minimizes embolic phenomena and irrigates the canal, minimizing thermal injury that may be induced with standard reamers and reaming techniques. The aspirated graft shares many of the growth factors and delivers comparable amount of osteoconductive and inductive tissue compared with iliac crest grafting techniques with less morbidity. This technique allows obtaining large volumes, in excess of 30 cm 3 , of rich cancellous graft typically in excess of what is required with little or no added morbidity or surgical time. The reamer head selected is at least 2 mm larger than the implant removed. A guide rod is bent and the advanced down, alternating sides of the distal femur passing the RIA after the guide rod has been repositioned. Fibular strut allografts have been shown to provide a reliable, biologic structural support in the postoperative period and, over time, partially incorporates with the surrounding native bone. First, a fibular strut allograft or cortical dowels are used to fill in the hole left in the head from the cephalic screw. Secondly a dowel or plug is used to block the femoral canal at the level of the lesser trochanter; thirdly dowel is placed in the superior greater trochanter defect. Filling the holes allows having an impact the copious amounts of morselized autograft obtained with the RIA. The lateral hole left from the entrance of the cephalic screw can then be blocked with another dowel or with the blade plate itself to keep the autograft from displacing. The authors’ technique, as depicted in Fig. 1 , has afforded a reliable way to improve fixation in the femoral head of the definitive implant while at the same time restoring the large volumes of bone stock destroyed by the previous enlarged proximal body of the cephalomedullary device. Residual graft can also be placed around the nonunion or osteotomy site before final closure.
Although replacing existing bone defects is an important part of a successful plan in treating peri- and subtrochanteric nonunions, it cannot be overemphasized that correction of the typical biomechanical and biologically unfavorable varus and shortened deformity is paramount for success. Having multiple implants available to obtain fixation, while allowing correction of deformity in these fractures, can be useful. The use of revision reconstruction nailing provides satisfactory results, but there are several drawbacks to using them. It is difficult to obtain correction of the deformity of the previous fracture with an intramedullary nail. As discussed previously, correction of the deformity is an essential step in revision surgery of the proximal femur and, in some cases, correcting this deformity and changing the biomechanical forces is enough to provide an ideal biologic environment for healing. The nail is also not as amendable to intraoperative contouring to optimize correction as the blade plate. Intramedullary nailing can also makes future surgery of the proximal femur even more difficult as additional bone is removed to seat the implant or a new hole is created to correct malalignment.
The question of whether or not to débride the nonunion site, complete the osteotomy through the nonunion, or fish scale the area is purely academic. The questions are, at which level is the osteotomy done and which angle is more relevant. Typically, the authors bypass the nonunion site and complete the controlled osteotomy at a lower level for several reasons. First, most nonunions of this area are due to poor stability or poor biomechanics and deformity, leading to hypertrophic or oligotrophic nonunions. Oligotrophic nonunion is rare and may suggest infection, osteonecrosis secondary to thermal necrosis from overzealous reaming, or significant devascularization. Secondly, nonunions lack distinct sharp edges and dense cortical bone that when compressed with the plate store energy well and impart stability. Thirdly, bypassing the nonunion avoids causing further devascularization of the nonunion. Finally, a controlled osteotomy at a lower level allows for longer proximal segment that can be more easily controlled and compressed.
The orientation of the osteotomy must take into consideration restoration of normal anatomy and leg length. Sometimes a double-level osteotomy is anticipated if greater than 2 cm of lengthening is required ( Fig. 2 ). Typically, the osteotomy is short and oblique, allowing easy correction of the common malrotation while also allowing the more simple correction of flexion, extension or varus, or valgus deformities. Lengthening of 1 cm can typically be obtained through a single-level osteotomy (discussed later). The sharp short edges are ideal for obtaining excellent stability in multiple planes once the plate is tensioned.









